How to Get Rid of a Cold Sore in 24 Hours
Key Takeaways
- You've felt that familiar tingle. That tell-tale itch on your lip that signals the unwelcome arrival of a cold sore. For the more than 50% of American adults who carry the herpes simplex virus type 1 (HSV-1), this scenario is all too common, and the desire to banish these painful, unsightly lesi
You've felt that familiar tingle. That tell-tale itch on your lip that signals the unwelcome arrival of a cold sore. For the more than 50% of American adults who carry the herpes simplex virus type 1 (HSV-1), this scenario is all too common, and the desire to banish these painful, unsightly lesions quickly is universal. Imagine waking up with a burgeoning cold sore, knowing you have a big event tomorrow. Your immediate thought? "How to get rid of a cold sore in 24 hours!" While completely eliminating a cold sore in such a short timeframe isn't always possible once it's fully formed, there are highly effective strategies and treatments that, when applied at the very first sign, can significantly shorten its duration, reduce its severity, and in some cases, prevent it from fully erupting.
This comprehensive guide from SmilePedia.net is designed to equip you with the knowledge and actionable steps to tackle cold sores with speed and efficacy. We'll delve into the science behind these pesky blisters, explore the most potent treatment options—from prescription antivirals to advanced laser therapy—and provide practical advice on prevention and long-term management. By understanding the lifecycle of a cold sore and acting decisively, you can dramatically improve your chances of minimizing its impact, helping you return to a confident, comfortable smile sooner.
Key Takeaways:
- Early Action is Crucial: To have the best chance of significantly reducing a cold sore in 24 hours, start treatment at the very first sign (tingling, itching) during the prodromal stage.
- Prescription Antivirals are Most Effective: Oral medications like valacyclovir (Valtrex), acyclovir, or famciclovir, and topical creams like acyclovir or penciclovir, can shorten healing time by days, especially when used early. A typical prescription can cost $30 - $150 without insurance.
- Laser Treatment Offers Rapid Healing: Dental laser therapy can reduce pain, viral activity, and dramatically speed up healing, often resolving symptoms within 24-48 hours. Costs typically range from $75 - $300 per session.
- OTC Options Provide Relief: Docosanol (Abreva) can shorten healing by about a day if applied early. Pain relievers and protective creams help manage symptoms. OTC treatments range from $10 - $30.
- Prevention is Key: Identify and avoid triggers (stress, sun exposure, fever), practice good hygiene, and consider prophylactic antiviral medication for frequent outbreaks.
- Cold Sores are NOT Canker Sores: They are distinct oral conditions caused by different factors, requiring different treatment approaches.
What It Is / Overview
A cold sore, medically known as herpes labialis, is a common viral infection caused primarily by the herpes simplex virus type 1 (HSV-1). Less commonly, it can be caused by HSV-2, which is more typically associated with genital herpes but can affect the mouth. These painful, fluid-filled blisters typically appear on or around the lips, though they can occasionally occur on other areas of the face. Once you're infected with HSV-1, the virus remains dormant in your nerve cells for life. It can reactivate periodically, leading to outbreaks.

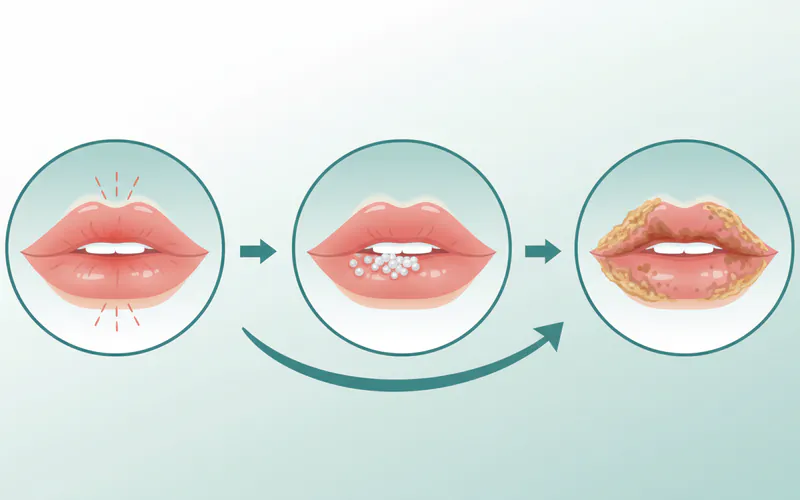
Cold sores progress through several distinct stages:
- Prodromal Stage (Day 1): This is the crucial stage for intervention. You might feel a tingling, itching, burning, or numb sensation on or around the lips, often accompanied by redness and slight swelling. This typically lasts a few hours to a day.
- Blister Stage (Day 2-3): Small, painful, fluid-filled blisters erupt, usually in a cluster. The fluid inside these blisters is highly contagious, containing millions of active virus particles.
- Weeping/Ulcer Stage (Day 4): The blisters burst, releasing the fluid, and leave behind shallow, open sores or ulcers. This is often the most painful and highly contagious stage.
- Crusting Stage (Day 5-8): The sores begin to dry out and form a yellowish or brownish crust (scab). This scab protects the healing skin underneath.
- Healing Stage (Day 9-14): The scab eventually falls off, revealing new skin. It usually heals without scarring, though hyperpigmentation (a dark spot) might temporarily remain.
The entire process can take anywhere from 7 to 14 days without treatment. The goal of "how to get rid of a cold sore in 24 hours" is to disrupt this cycle, ideally preventing the blister stage or at least dramatically shortening the weeping and crusting phases.
Types / Variations
While cold sores are primarily caused by HSV-1 and manifest similarly, the 'variations' often relate to the frequency, severity, and location of outbreaks, as well as their distinction from other oral lesions.
Recurrent Herpes Labialis
This is the most common form, characterized by repeated outbreaks on the lips or surrounding skin. The triggers for recurrence vary widely among individuals.
Primary Herpetic Gingivostomatitis
This is the initial infection with HSV-1, often occurring in young children. It can be much more severe than recurrent cold sores, causing widespread painful sores inside the mouth, on the gums, tongue, and throat, often accompanied by fever, swollen lymph nodes, and general malaise. This is not what people typically refer to when asking "how to get rid of a cold sore in 24 hours" but is the starting point for developing recurrent cold sores.
Ocular Herpes
If the HSV-1 virus spreads to the eye, it can cause herpes keratitis, a serious infection that can lead to scarring of the cornea and potentially vision loss. This highlights the importance of preventing self-transmission.
Herpetic Whitlow
This is an HSV infection of the finger, typically occurring when the virus enters through a break in the skin, often from touching a cold sore. Dental professionals are at a higher risk without proper barrier protection.
Cold Sores vs. Canker Sores (Aphthous Ulcers)
It's crucial to distinguish cold sores from canker sores, a common point of confusion for many.
- Cold Sores (Herpes Labialis): Caused by a virus (HSV-1). Appear on the outside of the mouth, usually on or around the lips. They are contagious.
- Canker Sores (Aphthous Ulcers): Not caused by a virus and are not contagious. They appear inside the mouth, on soft tissues like the tongue, inside of the cheeks, or gums. While their exact cause is unknown, triggers include stress, injury, acidic foods, vitamin deficiencies, and certain toothpastes. While this article focuses on how to get rid of a cold sore in 24 hours, understanding this distinction is vital for proper self-care. If you're looking for "how to get rid of canker sores," the treatment approaches are entirely different, often involving topical steroids, pain-relieving rinses, or laser therapy, as opposed to antiviral medications.
Causes / Why It Happens
Cold sores are caused by the herpes simplex virus type 1 (HSV-1), an extremely common virus. Once infected, the virus resides dormant in the sensory nerve ganglia (specifically the trigeminal ganglion for facial outbreaks). It never leaves your body, but various triggers can reactivate it, causing an outbreak.
Common triggers include:
- Stress: Emotional or physical stress is a major trigger for many individuals.
- Sunlight Exposure: UV radiation from the sun can weaken the immune system in the skin, allowing the virus to reactivate. This is why cold sores are common after beach trips or skiing.
- Fever or Illness: Any condition that taxes your immune system, such as a cold, flu, or fever (hence "cold sore"), can lead to an outbreak.
- Hormonal Changes: Menstrual cycles, pregnancy, or hormonal fluctuations can trigger cold sores in some women.
- Physical Trauma: Injury to the lip or mouth area, dental work, or even intense lip balm application can sometimes initiate an outbreak.
- Weakened Immune System: Conditions like HIV/AIDS, chemotherapy, or immunosuppressant medications significantly increase the risk and severity of outbreaks.
- Fatigue: Lack of sleep can weaken the immune response, making an outbreak more likely.
Understanding your specific triggers is a key component of prevention.
Signs and Symptoms
Recognizing the earliest signs is paramount to effectively addressing the question of how to get rid of a cold sore in 24 hours. The quicker you act, the better your chances of minimizing its impact.
The progression of symptoms usually follows these stages:
-
Prodromal Stage (The Warning Signs - Crucial for 24-hour intervention):
- Tingling, Itching, or Burning: This is the most common and definitive early symptom. You might feel a distinct tingling or itching sensation on or around your lip, often in the exact spot where previous cold sores have appeared. This can last from a few hours to a full day.
- Redness and Swelling: The affected area may become slightly red and tender, indicating inflammation.
- Numbness: Some people report a feeling of numbness in the area.
-
Blister Stage:
- Small, Fluid-Filled Blisters: Within 1-2 days of the prodromal stage, small, often painful, fluid-filled blisters erupt, usually in a cluster. They are typically red at the base.
- Pain and Tenderness: The area becomes increasingly sensitive and painful.
-
Weeping/Ulcer Stage:
- Bursting Blisters: The blisters rupture, leaking clear fluid. This leaves behind shallow, often painful, open sores or ulcers.
- High Contagion: This is the most contagious stage, as the viral load in the fluid is at its peak.
-
Crusting/Scabbing Stage:
- Formation of a Scab: The open sores dry out and form a yellowish or brownish crust (scab). The scab provides a protective layer over the healing skin.
- Itching and Cracking: The scab can be itchy and might crack, especially if the mouth moves, which can be painful and delay healing.
-
Healing Stage:
- Scab Falls Off: The scab eventually detaches, revealing newly healed skin underneath.
- No Scarring (Usually): Most cold sores heal without leaving a scar, though a temporary dark spot (hyperpigmentation) might remain for a while.
Pro Tip: Pay close attention to the prodromal stage. If you experience the characteristic tingling, itching, or burning, consider it your immediate call to action for rapid treatment.
Treatment Options
When it comes to how to get rid of a cold sore in 24 hours, or at least dramatically shorten its course, a multi-pronged approach initiated at the first sign of symptoms is your best bet.
1. Prescription Antiviral Medications (Most Effective)
These medications work by inhibiting the virus's ability to replicate, thereby reducing the severity and duration of the outbreak. They are most effective when taken during the prodromal stage.
-
Oral Antivirals:
- Valacyclovir (Valtrex): Often considered the most effective for rapid treatment. A common regimen for cold sores is a single high dose (e.g., 2 grams) taken twice a day for one day, or a lower dose for several days. Can significantly reduce healing time, sometimes by several days.
- Acyclovir (Zovirax): One of the oldest antivirals. Typically prescribed in a multi-day regimen (e.g., 400 mg three times a day for 5 days or 200 mg five times a day for 5 days).
- Famciclovir (Famvir): Similar to valacyclovir, often prescribed as a single high dose or over a shorter period.
- Pros: Highly effective at shortening duration, reducing pain, and preventing blister formation if taken early. Can reduce the frequency of future outbreaks when used prophylactically.
- Cons: Requires a prescription. May cause mild side effects like headache, nausea. Effectiveness diminishes significantly if started after blisters have formed.
- Cost: Without insurance, a course of valacyclovir can range from $50 to $150, acyclovir from $30 to $100, and famciclovir from $80 to $200, depending on dosage and pharmacy. Many insurance plans cover generic versions.
-
Topical Antivirals:
- Acyclovir Cream (Zovirax Cream): Applied 5 times a day for 4 days. Can reduce healing time by about half a day to a day if used early.
- Penciclovir Cream (Denavir): Applied every 2 hours while awake for 4 days. Can shorten healing time and reduce pain.
- Pros: Applied directly to the affected area, minimizing systemic side effects. No prescription needed for some versions.
- Cons: Less effective than oral antivirals for rapid resolution, especially for severe outbreaks. Requires frequent application.
- Cost: Over-the-counter acyclovir cream can cost $15-$30. Prescription penciclovir cream can be $30-$70.
2. Over-the-Counter (OTC) Treatments
These options focus more on symptom management and providing a protective barrier, though some can aid healing.
-
Docosanol (Abreva): A 10% cream applied at the first sign of tingling. It works by preventing the virus from entering healthy cells.
- Pros: Non-prescription, readily available. Can shorten healing time by about a day if applied 5 times a day from the prodromal stage.
- Cons: Less potent than prescription antivirals.
- Cost: Around $15-$25 per tube.
-
Pain Relievers and Topical Anesthetics:
- Lidocaine or Benzocaine Creams: Provide temporary numbing relief from pain and itching. Brands like Orajel Cold Sore.
- Oral Pain Relievers: Ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can help manage discomfort.
- Pros: Immediate symptomatic relief.
- Cons: Do not treat the underlying viral infection or shorten duration.
- Cost: $5-$15 for topical anesthetics, $5-$20 for oral pain relievers.
-
Protective Balms and Patches:
- Zinc Oxide Creams: Can provide a physical barrier and may have some antiviral properties.
- Hydrocolloid Patches (e.g., Compeed): Cover the cold sore, protect it from contamination, reduce pain, and create an optimal healing environment.
- Pros: Protects the sore, reduces irritation, can make it less noticeable.
- Cons: Don't kill the virus directly.
- Cost: $10-$20 for patches or zinc creams.
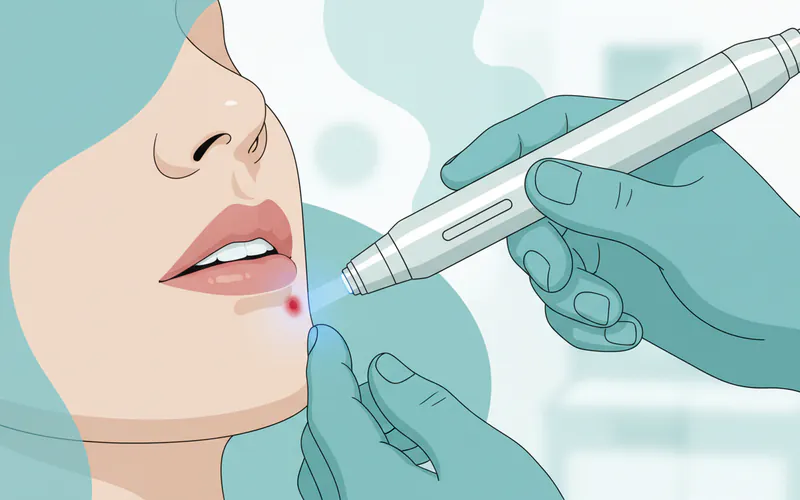
3. Laser Treatment (Dental Laser Therapy)
Administered by a dentist, specific dental lasers (like soft tissue diode lasers) can be highly effective, especially when used early.
- Mechanism: The laser energy targets the virus particles and inflamed tissue, reducing viral load, stimulating cellular healing, and alleviating pain.
- Pros: Often provides immediate pain relief and can prevent blister formation if treated in the prodromal stage. Can significantly speed up healing (often within 24-48 hours), potentially halting the progression of the sore. May reduce the frequency and intensity of future outbreaks in the treated area. No drugs required.
- Cons: Requires an office visit to a dental professional. Not always covered by insurance.
- Cost: A single laser treatment typically costs between $75 and $300 per session, depending on the clinic and region. Some dental plans may offer partial coverage, but it's often considered elective.
4. Home Remedies and Natural Approaches
While scientific evidence for some of these is limited or anecdotal, many people find them helpful for symptom relief or mild cases.
- L-Lysine: An amino acid available as an oral supplement or topical cream. Some studies suggest it may help prevent or reduce the severity of outbreaks by inhibiting arginine, which HSV-1 needs to replicate.
- Pro Tip: For acute outbreaks, many recommend taking 1,000-3,000 mg daily during the prodromal stage.
- Lemon Balm (Melissa officinalis): A topical cream or diluted essential oil. Studies suggest it may have antiviral properties and can reduce healing time.
- Propolis: A resinous substance collected by bees. Available as a cream or ointment, it may have antiviral and anti-inflammatory effects.
- Ice: Applying an ice pack directly to the tingling area for 10-15 minutes can reduce inflammation and numb the area, potentially slowing progression.
- Aloe Vera Gel: Known for its soothing and healing properties, it can provide comfort and aid in skin repair.
- Zinc Oxide: Besides being a physical barrier, zinc may also have antiviral properties.
- Pros: Natural, readily available.
- Cons: Efficacy varies widely, and scientific backing is often weaker than for prescription medications. Unlikely to "get rid of a cold sore in 24 hours" on its own if blisters have already formed.
- Cost: Varies, but generally inexpensive ($5-$20).
Step-by-Step Process: How to Tackle a Cold Sore in 24 Hours
To achieve the best possible outcome within a 24-hour window, rapid recognition and immediate action are critical. This process assumes you've caught the cold sore at the very first sign (prodromal stage).
Step 1: Recognize the Prodromal Stage (0-6 Hours)
- Identify the warning signs: As soon as you feel that familiar tingling, itching, burning, or numbness on your lip, act immediately. This is your narrow window of opportunity.
Step 2: Initiate Potent Antiviral Treatment (Immediately upon recognition)
- Prescription Oral Antiviral: If you have a standing prescription for valacyclovir, acyclovir, or famciclovir, take the prescribed dose now. This is often your most powerful tool for rapid suppression.
- Example: For valacyclovir, this might mean taking 2 grams orally twice, 12 hours apart.
- Prescription Topical Antiviral (if oral isn't an option): If you only have topical acyclovir or penciclovir cream, apply it generously to the tingling area. Follow package instructions carefully for frequency (e.g., 5 times a day for acyclovir, every 2 hours while awake for penciclovir).
- Over-the-Counter Docosanol (Abreva): If you don't have a prescription, apply docosanol cream as directed (typically 5 times a day). While less potent than oral antivirals, it's the best OTC option for shortening duration.
Step 3: Consider Dental Laser Treatment (Within 6-12 Hours)
- Contact your dentist: If your dental office offers laser cold sore treatment, call them immediately. Many dentists prioritize same-day appointments for cold sore flare-ups, especially during the prodromal stage.
- Benefits: A single laser session can often stop the progression of the sore, reduce pain, and accelerate healing, sometimes resolving symptoms within 24-48 hours.
Step 4: Symptom Management and Prevention of Spread (Ongoing)
- Ice Application: Apply an ice pack wrapped in a cloth to the affected area for 10-15 minutes at a time, several times a day. This can reduce swelling and discomfort.
- Pain Relief: Take over-the-counter pain relievers like ibuprofen or acetaminophen if you experience pain.
- Protective Barrier: Apply a thin layer of petroleum jelly or a hydrocolloid patch to protect the area, keep it moist, and prevent cracking. This also helps contain the virus.
- Avoid Touching: Do not pick, squeeze, or unnecessarily touch the cold sore. This can spread the virus to other parts of your body (e.g., eyes, genitals, fingers) or to other people. Wash your hands thoroughly if you do touch it.
- Hygiene: Avoid sharing utensils, cups, towels, or lip products.
Step 5: Continue Treatment and Monitor (Beyond 24 Hours)
- Maintain Antiviral Regimen: Continue your prescribed oral or topical antiviral medication as directed for the full course, even if symptoms improve. This ensures the virus is suppressed effectively.
- Hydration: Maintain good overall oral health by staying well-hydrated. While not directly treating the cold sore, it supports your body's healing process. This is particularly important if you're experiencing xerostomia (dry mouth) due to other medications or conditions, as a healthy oral environment can aid recovery.
- Sun Protection: If outdoors, use a lip balm with SPF 30 or higher, as UV exposure can trigger future outbreaks and irritate existing ones.
By following these steps, you significantly increase your chances of preventing a full-blown cold sore or at least reducing its severity and duration within the crucial 24-hour window and beyond.
Cost and Insurance
The cost of cold sore treatments in the US can vary significantly based on the type of treatment, whether it's prescription or OTC, and your insurance coverage.
Prescription Medications:
- Oral Antivirals (Valacyclovir, Acyclovir, Famciclovir):
- Without Insurance: A single course can range from $30 to $200, with generics being at the lower end. Valacyclovir tends to be more expensive than acyclovir.
- With Insurance: Most dental and medical insurance plans cover generic antiviral medications for cold sores. You'll typically pay your copay (e.g., $10-$50), or a percentage of the cost if you have a high deductible plan. It's usually covered under your medical pharmacy benefits.
- Topical Antivirals (Penciclovir Cream):
- Without Insurance: A small tube can cost $30 to $70.
- With Insurance: Often covered, with a typical copay of $10-$40.
Over-the-Counter (OTC) Treatments:
- Docosanol (Abreva): Generally $15 to $25 per tube. Not typically covered by insurance, but FSA/HSA eligible.
- Lidocaine/Benzocaine Creams, Patches, Lip Balms: Ranging from $5 to $20. Not covered by insurance, but FSA/HSA eligible.
Dental Laser Treatment:
- Cost Per Session: Typically ranges from $75 to $300 per session. This can vary based on the dental practice's location, technology used, and the dentist's fees.
- Insurance Coverage: Many medical and dental insurance plans consider laser cold sore treatment as elective or aesthetic and may not cover it. Some plans might cover a portion if it's coded as a therapeutic treatment for pain or infection. It's essential to check with your specific provider before undergoing treatment.
- Payment Plans: Some dental offices offer in-house payment plans or third-party financing options like CareCredit for larger treatment costs.
Pro Tip: Always call your insurance provider directly to confirm coverage for prescription medications and specifically ask about laser cold sore treatment before your appointment. Many pharmacies also offer discount programs for cash payments on generic drugs.
Recovery and Aftercare
Even with the most aggressive "how to get rid of a cold sore in 24 hours" strategy, proper recovery and aftercare are essential to ensure complete healing, prevent complications, and reduce the risk of future outbreaks.
Immediate Aftercare (Post-Treatment):
- Continue Medication: If prescribed oral antivirals, complete the full course as directed by your doctor, even if your symptoms improve rapidly. For topical creams, continue applying as instructed.
- Keep it Clean: Gently clean the area with mild soap and water, then pat dry. Avoid harsh scrubbing or picking at scabs, as this can lead to scarring or secondary bacterial infection.
- Moisturize: Apply a thin layer of petroleum jelly or a healing balm to keep the area moist and prevent cracking, especially during the scabbing phase. This can promote faster healing and reduce discomfort.
- Avoid Irritants: Steer clear of acidic or spicy foods, alcohol, and very hot beverages that can irritate the healing skin.
- Protect from Sun: Continue to use a lip balm with SPF 30 or higher, even after the sore has healed. Sun exposure is a major trigger for recurrence.
Long-Term Aftercare and Prevention:
- Identify and Manage Triggers: Keep a journal to identify your personal cold sore triggers (stress, sun, illness, specific foods). Once identified, actively work to mitigate them.
- Stress Management: Incorporate stress-reducing activities into your routine, such as exercise, meditation, yoga, or hobbies.
- Sun Protection: Always use lip balm with broad-spectrum SPF 30+ when outdoors, even on cloudy days. A wide-brimmed hat can also provide protection.
- Boost Immune System: Maintain a healthy lifestyle with a balanced diet rich in fruits and vegetables, regular exercise, and adequate sleep. Consider supplements like L-Lysine or Vitamin C after consulting your doctor.
- Good Hygiene: Avoid touching your face unnecessarily. Wash your hands frequently. Do not share personal items like lip balm, razors, or towels.
- Replace Contaminated Items: Discard old toothbrushes, lip balms, or makeup applicators that may have come into contact with the active cold sore to prevent reinfection or spreading.
- Prophylactic Antivirals: For individuals with very frequent or severe outbreaks (e.g., more than 6 times a year), your doctor may prescribe a daily low-dose antiviral medication to suppress the virus and prevent outbreaks. This is a long-term strategy for severe cases.
Prevention
Preventing cold sores is ultimately more effective than trying to eliminate them in 24 hours. Given that HSV-1 is a lifelong infection, prevention focuses on avoiding triggers and minimizing transmission.
1. Identify and Avoid Triggers:
- Sun Exposure: Use lip balm with SPF 30 or higher daily, especially when outdoors. Wear a wide-brimmed hat.
- Stress: Practice stress-reduction techniques like meditation, yoga, regular exercise, or hobbies. Ensure adequate sleep.
- Illness/Fever: While hard to avoid, maintaining a strong immune system through a healthy lifestyle can help.
- Physical Trauma: Be gentle with your lips. Avoid excessive picking or biting. Inform your dentist if you are prone to cold sores before dental work, as they might suggest prophylactic antivirals.
- Hormonal Changes: If you notice a pattern with your menstrual cycle, discuss it with your doctor.
2. Boost Your Immune System:
- Healthy Diet: Eat a balanced diet rich in vitamins and minerals, especially Vitamin C and Zinc.
- Regular Exercise: Helps reduce stress and improve overall immune function.
- Adequate Sleep: Aim for 7-9 hours of quality sleep per night.
- Hydration: Drink plenty of water to maintain overall health and oral moisture. This is especially relevant if you suffer from xerostomia (dry mouth), as a chronically dry mouth can impair your body's natural defenses against pathogens.

3. Practice Good Hygiene and Prevent Transmission:
- Avoid Direct Contact: Do not kiss others or engage in intimate contact when you have an active cold sore.
- Do Not Share Items: This includes eating utensils, drinking glasses, towels, razors, toothbrushes, and lip balms.
- Wash Hands Frequently: Especially after touching your cold sore. Avoid touching your eyes or other parts of your body after touching the sore.
- Discard Contaminated Items: Replace your toothbrush after a cold sore outbreak to prevent reinfection.
4. Prophylactic Antiviral Therapy:
- For individuals experiencing frequent, severe, or debilitating cold sore outbreaks (e.g., more than six times a year), a doctor may prescribe daily low-dose oral antiviral medication (e.g., acyclovir, valacyclovir). This long-term suppressive therapy can significantly reduce the frequency and severity of outbreaks.
5. L-Lysine Supplementation:
- Some individuals find taking daily L-Lysine supplements (e.g., 500-1000 mg) helpful for prevention. Lysine is thought to interfere with the virus's replication process. Consult your doctor before starting any new supplement regimen.
Risks and Complications
While cold sores are generally benign, they can lead to complications, especially in individuals with compromised immune systems or if the virus spreads to other areas.
- Spread to Other Body Parts: The most common complication is autoinoculation, where you spread the virus to other areas of your own body by touching the cold sore and then touching other susceptible areas.
- Herpes Keratitis (Ocular Herpes): Infection of the eye, which can cause pain, redness, sensitivity to light, and potentially lead to corneal scarring and permanent vision loss.
- Herpetic Whitlow: Infection of the fingers, resulting in painful blisters.
- Genital Herpes: While HSV-1 is typically oral, it can cause genital herpes through oral-genital contact, and vice-versa (HSV-2 can cause oral cold sores).
- Secondary Bacterial Infections: Open sores can become infected by bacteria, leading to increased pain, swelling, pus, and delayed healing. Signs include increasing redness, warmth, pus, and fever.
- Severe Outbreaks in Immunocompromised Individuals: People with weakened immune systems (e.g., HIV/AIDS, organ transplant recipients, chemotherapy patients) can experience more severe, widespread, and persistent cold sores that may spread to internal organs.
- Eczema Herpeticum: A rare but severe complication in individuals with eczema, where HSV spreads rapidly across large areas of the skin, causing widespread painful blisters and skin erosion. This is a medical emergency.
- Psychological Impact: Frequent or severe cold sores can cause significant emotional distress, self-consciousness, and social anxiety.
Comparison Tables
To help you decide on the best "how to get rid of a cold sore in 24 hours" strategy, here's a comparison of common treatment options:
Table 1: Cold Sore Treatment Options Comparison
| Treatment Type | Primary Mechanism | Effectiveness (for 24hr goal) | Typical Cost Range (USD) | Key Pros | Key Cons |
|---|---|---|---|---|---|
| Oral Antivirals | Inhibits viral replication | High (if started early) | $30 - $200 (Rx) | Most effective for rapid shortening/prevention of outbreak; systemic action | Requires prescription; less effective if blisters already formed; potential mild side effects |
| Topical Antivirals | Inhibits viral replication (localized) | Moderate (if started early) | $15 - $70 (OTC/Rx) | Localized application, fewer systemic side effects; OTC options available | Less potent than oral antivirals; requires frequent application; less effective for severe outbreaks |
| Dental Laser Therapy | Reduces viral load, stimulates healing | High (especially if started early) | $75 - $300 (per session) | Immediate pain relief; often prevents blister, dramatically speeds healing; no drugs; reduces recurrences | Requires dental visit; often not covered by insurance; cost per session can add up for frequent use |
| Docosanol (Abreva) | Prevents virus entry into healthy cells | Low-Moderate (if started early) | $15 - $25 (OTC) | Readily available, no prescription; can shorten duration by ~1 day | Less potent than antivirals; requires frequent application; not effective if blisters fully formed |
| Home Remedies | Symptom relief, minor antiviral support | Low (anecdotal) | $5 - $20 | Natural, inexpensive, accessible | Limited scientific evidence; unlikely to "cure" in 24 hours; inconsistent results |
Table 2: US Cost of Prescription Oral Antivirals (Without Insurance)
| Medication Name | Generic Name | Typical Dosage for Cold Sores | Estimated Cost Range (Without Insurance, Per Course) |
|---|---|---|---|
| Valtrex | Valacyclovir | 2g twice daily for 1 day | $50 - $150 |
| Zovirax | Acyclovir | 400mg three times daily for 5 days | $30 - $100 |
| Famvir | Famciclovir | 1500mg as a single dose | $80 - $200 |
| Acyclovir Topical Cream | Acyclovir cream 5% | Apply 5 times daily for 4 days | $15 - $30 |
| Denavir | Penciclovir cream 1% | Apply every 2 hours while awake for 4 days | $30 - $70 |
(Costs are estimates and can vary based on pharmacy, location, and discount programs.)
Children / Pediatric Considerations
Cold sores in children, especially toddlers and infants, require careful attention due to their developing immune systems and propensity for touching their faces.
Primary Infection (Primary Herpetic Gingivostomatitis):
- Young children often experience their first HSV-1 infection (primary herpetic gingivostomatitis) between 6 months and 5 years of age.
- Symptoms: This can be severe, involving painful sores inside the mouth, on the gums, tongue, and throat, making eating and drinking difficult. Fever, swollen lymph nodes, irritability, and dehydration are common.
- Treatment: A pediatrician will often prescribe oral antiviral medications (like acyclovir suspension) to reduce the severity and duration. Pain relief (acetaminophen or ibuprofen, age-appropriate) and ensuring hydration are critical.
- When to See a Dentist/Pediatrician: Always seek medical attention for a child experiencing a suspected primary HSV-1 infection, especially if they are refusing to drink or showing signs of dehydration.
Recurrent Cold Sores in Children:
- Once a child has had the primary infection, they may experience recurrent cold sores similar to adults.
- Triggers: Similar to adults, triggers include fever, illness (e.g., common cold, flu), sun exposure, stress, or even minor trauma. Parents should monitor for these.
- Treatment:
- Early Intervention: As with adults, starting treatment at the very first tingle is crucial.
- Topical Antivirals: Acyclovir or penciclovir creams can be used, but ensure the child doesn't lick it off. Docosanol (Abreva) is also an option for children 12 and older.
- Oral Antivirals: For frequent or severe recurrent outbreaks, a pediatrician might prescribe a short course of oral antivirals (e.g., acyclovir, valacyclovir) for children.
- Pain Relief: OTC pain relievers (like children's acetaminophen or ibuprofen) can manage discomfort.
- Prevention:
- Sun Protection: Use child-safe lip balm with SPF 30+.
- Hygiene: Teach children not to touch their cold sores and to wash their hands frequently. Emphasize not sharing cups, utensils, or towels.
- Avoid Contact: Do not let adults with active cold sores kiss young children.
- Risks: Children are at higher risk for autoinoculation (spreading the virus to their eyes or fingers) due to frequent touching. Parents should monitor for signs of eye redness, irritation, or new blisters elsewhere. Pro Tip for Parents: Keep a watchful eye for any changes in your child's behavior, especially irritability or refusal to eat/drink, which could signal a cold sore that they can't articulate.
Cost Breakdown
A detailed breakdown of cold sore treatment costs in the US, considering various scenarios:
Average US Costs (Without Insurance):
- Low-End Scenario ($10-$30): Relying solely on OTC topical treatments like Docosanol (Abreva) or generic acyclovir cream, plus OTC pain relievers. This is generally for mild cases caught very early.
- Mid-Range Scenario ($30-$150): Accessing generic prescription oral antivirals (e.g., acyclovir or valacyclovir, depending on dosage) via a primary care visit (PCP visit fee could be $75-$200 if no insurance) or a telemedicine consultation (telemedicine fee usually $40-$75).
- High-End Scenario ($150-$500+): This might involve a more expensive brand-name oral antiviral prescription, or a combination of prescription medication and a single dental laser treatment session. If primary herpetic gingivostomatitis requires multiple doctor visits or emergency care, costs could be higher.
With Insurance:
- PCP/Telemedicine Visit: Your copay typically ranges from $20-$75.
- Prescription Oral Antivirals: Your pharmacy copay for generic versions is usually $10-$50. Brand-name drugs might have a higher copay or require a deductible to be met.
- Prescription Topical Antivirals: Pharmacy copay typically $10-$40.
- Dental Laser Treatment: As mentioned, coverage is variable. If covered, you might pay a copay or a percentage of the cost after your deductible, ranging from $0 (rare) to $200+.
Payment Plans and Financing Options:
- Dental Offices: For laser treatment, some dental practices offer in-house payment plans, allowing you to pay the cost over several months without interest.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options if paid off within a promotional period.
- Pharmacy Discount Cards: Programs like GoodRx or SingleCare can offer significant discounts on prescription medications for those without insurance or with high deductibles.
Cost-Saving Tips:
- Generic Medications: Always ask your doctor if a generic version of a prescription antiviral is available, as they are significantly cheaper.
- Telemedicine: For initial consultations or prescription refills, telemedicine services can be a cost-effective way to get a prescription without a full in-person doctor's visit.
- Pharmacy Shopping: Prices for medications can vary widely between pharmacies. Use online tools or call around to compare prices.
- FSA/HSA Funds: Utilize Flexible Spending Accounts (FSA) or Health Savings Accounts (HSA) for eligible prescription, OTC, and dental expenses to save on taxes.
- Prophylactic Treatment: If you suffer from frequent outbreaks, discuss prophylactic antiviral therapy with your doctor. While it's an ongoing cost, it can prevent acute outbreaks which might lead to more expensive reactive treatments or missed work/social engagements.

Frequently Asked Questions
### What is the fastest way to get rid of a cold sore in 24 hours?
The absolute fastest way to potentially get rid of or significantly reduce a cold sore in 24 hours is to apply a prescription oral antiviral (like valacyclovir) at the very first sign of tingling, combined with a dental laser treatment performed by a dentist. Oral antivirals suppress the virus systemically, while the laser targets the lesion locally, often providing immediate pain relief and accelerating healing.
### Are cold sores contagious, and for how long?
Yes, cold sores are highly contagious, primarily from the moment you feel the first tingle until the sore is completely healed and the scab has fallen off. The fluid in the blisters is packed with virus particles. Avoid kissing, sharing food/drinks, or intimate contact during this period.
### What is the difference between a cold sore and a canker sore?
Cold sores (herpes labialis) are caused by the herpes simplex virus (HSV-1), appear outside the mouth on or around the lips, and are contagious. Canker sores (aphthous ulcers) are not viral, appear inside the mouth on soft tissues, and are not contagious. Treatments for each are entirely different.
### Can dry mouth (xerostomia) make cold sores worse?
While xerostomia (dry mouth) isn't a direct cause of cold sores, maintaining good oral health, including adequate saliva flow, supports the body's natural defenses and healing processes. Severe dry mouth can make the oral environment more susceptible to various issues, potentially prolonging healing or increasing discomfort of any oral lesion, including a cold sore on the lip.
### How do I prevent cold sores from recurring?
Prevention involves identifying and avoiding your triggers (stress, sun, illness), maintaining a strong immune system, using SPF lip balm, practicing good hygiene, and sometimes taking daily antiviral medication (prophylactic therapy) if outbreaks are frequent or severe.
### Is laser treatment painful?
Most patients report that dental laser treatment for cold sores is not painful and often provides immediate relief from the itching or burning sensation. It typically takes only a few minutes, and some dentists apply a topical anesthetic beforehand for added comfort.
### Can I use makeup to cover a cold sore?
While you can use specific cold sore patches (like hydrocolloid patches) that allow makeup application, applying makeup directly to an open cold sore is generally not recommended. It can trap bacteria, irritate the sore, delay healing, and contaminate your makeup products. Wait until it has scabbed over.
### How long do cold sores typically last without treatment?
Without any treatment, a cold sore typically runs its full course in 7 to 14 days, progressing through the tingling, blistering, weeping, crusting, and healing stages.
### Are there specific foods I should avoid or eat during an outbreak?
Avoid acidic, spicy, or very salty foods, as they can irritate the sore. Some people find that foods high in L-arginine (like nuts, chocolate, and oats) can trigger outbreaks, while foods high in L-lysine (like dairy, fish, and chicken) may help. However, scientific evidence for dietary impact is mixed.
### When should I see a dentist or doctor for a cold sore?
You should see a dentist or doctor if your cold sore is unusually large or severe, doesn't start to heal within 7-10 days, spreads to your eyes or other body parts, is accompanied by fever or swollen glands, or if you have a weakened immune system.
When to See a Dentist
While many cold sores can be managed at home or with over-the-counter remedies, certain situations warrant a visit to your dentist or a medical professional. Prompt professional evaluation can prevent complications and ensure effective treatment.
See a Dentist or Doctor If:
- The cold sore does not heal within 7-10 days: If the lesion persists beyond two weeks, it should be evaluated to rule out secondary infection or other oral conditions.
- You have a weakened immune system: Individuals with compromised immune systems (e.g., due to HIV/AIDS, cancer treatment, organ transplant medications) are at higher risk for severe and widespread outbreaks. They should seek professional help at the first sign of a cold sore.
- The cold sore is unusually large, painful, or accompanied by fever or swollen glands: These could indicate a more severe infection or a primary HSV-1 outbreak.
- The infection spreads to your eyes: Any redness, irritation, sensitivity to light, or changes in vision in the eye, especially after touching a cold sore, is an emergency. HSV-1 can cause serious eye infections (herpes keratitis) that can lead to permanent vision damage. See an ophthalmologist immediately.
- Outbreaks are frequent or severe: If you experience cold sores regularly (e.g., more than 6 times a year), a healthcare provider can discuss prophylactic antiviral therapy to reduce the frequency and intensity of future outbreaks.
- Signs of secondary bacterial infection appear: These include increasing redness, swelling, warmth, severe pain, or the presence of pus in the cold sore.
- The cold sore recurs in the same exact spot after laser treatment: While rare, if a cold sore consistently returns to a previously laser-treated site, your dentist might need to re-evaluate the treatment plan or investigate underlying factors.
Red Flags vs. Routine Care: While routine cold sores can often be addressed with early intervention, any deviation from the typical healing process or spread to other areas should be considered a red flag. Your dental professional at SmilePedia.net can provide guidance, prescribe appropriate medications, and offer advanced treatments like laser therapy to help you manage and prevent cold sores effectively.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026