Diabetes and Canker Sores: Complete Guide

Key Takeaways
- Living with diabetes means managing various aspects of your health, often extending beyond blood sugar levels to encompass areas you might not immediately consider – like your oral health. Did you know that individuals with diabetes are more susceptible to a range of oral issues, including the commo
Diabetes and Canker Sores: Complete Guide
Living with diabetes means managing various aspects of your health, often extending beyond blood sugar levels to encompass areas you might not immediately consider – like your oral health. Did you know that individuals with diabetes are more susceptible to a range of oral issues, including the common and often painful canker sore? Approximately 37 million Americans live with diabetes, and a significant portion will experience oral complications. Understanding the intricate link between diabetes and canker sores isn't just about managing discomfort; it's about safeguarding your overall well-being and maintaining effective diabetes control.

Canker sores, also known as aphthous ulcers, are small, shallow lesions that develop on the soft tissues inside your mouth or at the base of your gums. While typically harmless and self-healing, they can be excruciating, making eating, drinking, and speaking a challenge. For someone with diabetes, these sores can be more frequent, severe, and slower to heal due to the systemic effects of the condition. This comprehensive guide will delve into the complex relationship between diabetes and canker sores, exploring their causes, various types, effective treatment options, prevention strategies, and how to manage them while living with diabetes. We'll equip you with the knowledge to identify, treat, and potentially prevent these unwelcome oral visitors, helping you maintain a healthier mouth and a better quality of life.
Key Takeaways:
- Elevated Risk: Individuals with diabetes, particularly those with uncontrolled blood glucose, face a higher risk of developing more frequent, severe, and slow-healing canker sores due to compromised immune function and altered healing processes.
- Types & Duration: Canker sores primarily manifest as minor (most common, 1-10mm, heal in 1-2 weeks), major (larger, deeper, >10mm, can take weeks to months, may scar), or herpetiform (clusters of tiny ulcers).
- Treatment Varies: Treatment ranges from over-the-counter (OTC) numbing gels ($5-$30) and protective pastes to prescription topical corticosteroids ($20-$200) and in-office laser therapy ($50-$250 per session), depending on severity.
- Blood Glucose Control is Key: Effective management of blood glucose levels is the most critical preventative and supportive measure for reducing the incidence and severity of canker sores in diabetic patients.
- Prevention Strategies: Include avoiding triggers, maintaining excellent oral hygiene with non-irritating products, addressing nutritional deficiencies, and stress management.
- Insurance Coverage: Most dental insurance plans do not directly cover canker sore treatment unless it's a symptom of a broader issue requiring a covered procedure. Medical insurance might cover prescription medications.
- When to Seek Professional Help: Consult a dentist if sores are larger than 1/2 inch, persist for more than 2-3 weeks, are unusually painful, reoccur frequently, or are accompanied by fever, fatigue, or difficulty swallowing.
What It Is / Overview
Canker sores, medically known as aphthous ulcers, are among the most common lesions affecting the oral cavity. They are small, round or oval sores that appear on the soft tissues inside your mouth, such as the inside of the lips, cheeks, tongue, soft palate, or at the base of the gums. Unlike cold sores, which are caused by the herpes simplex virus and appear on the outside of the lips, canker sores are not contagious and are not caused by a virus. They are essentially a break in the oral mucosa, exposing sensitive underlying tissue.
For the general population, canker sores are often a nuisance, healing within a week or two without intervention. However, for individuals living with diabetes, the picture can be significantly different. Diabetes, a chronic metabolic disorder characterized by high blood glucose levels, impacts various bodily systems, including the oral cavity and the body's ability to heal and fight infection.
Diabetes and Canker Sores: The Connection
The link between diabetes and canker sores primarily stems from several physiological changes that diabetes can induce:
- Compromised Immune System: High blood glucose levels can weaken the immune system's ability to respond effectively to irritations and minor injuries. This makes individuals with diabetes more susceptible to developing sores from minor trauma (like biting the cheek) and prolongs the healing process.
- Impaired Healing: Diabetes can affect the body's microcirculation, reducing blood flow to tissues, including those in the mouth. Adequate blood flow is crucial for delivering nutrients and immune cells necessary for tissue repair. Slower healing means canker sores can persist longer and be more prone to secondary infections.
- Increased Inflammation: Chronic low-grade inflammation is a hallmark of diabetes. This heightened inflammatory state throughout the body can predispose oral tissues to respond more intensely to minor irritants, potentially leading to more severe or frequent aphthous ulcers.
- Changes in Oral Microbiome: Diabetes can alter the balance of bacteria and fungi in the mouth, creating an environment that is less resilient and more prone to inflammatory conditions.
Therefore, while the specific triggers for canker sores may be the same for everyone (stress, trauma, certain foods), individuals with diabetes may experience them with greater frequency, increased severity, and a significantly longer healing time. This can lead to considerable discomfort, interfere with nutrition, and impact overall quality of life. Understanding this systemic connection is the first step toward effective management.
Types / Variations of Canker Sores
Canker sores are not a monolithic entity; they appear in a few distinct forms, each with characteristic features. While the underlying causes and treatments often overlap, recognizing the type can help in diagnosis and predicting their course. In individuals with diabetes, any of these types can occur, but they may present with increased severity or prolonged healing.
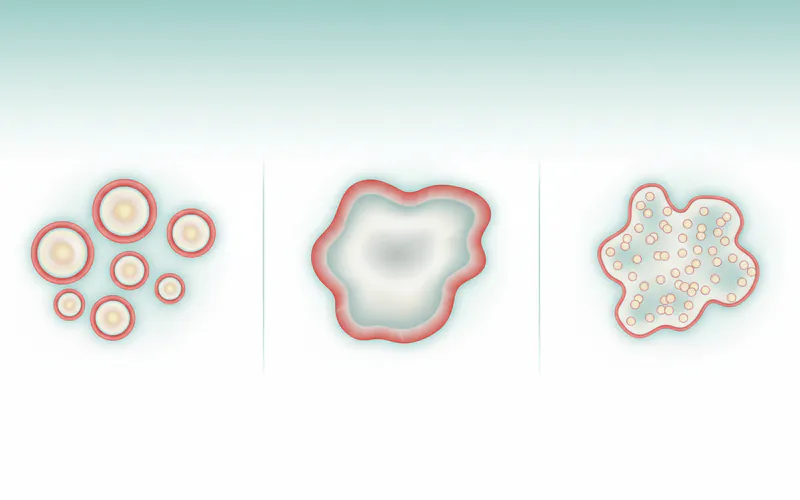
Minor Aphthous Ulcers (MiAUs)
- Description: These are the most common type of canker sore, accounting for 80-85% of all cases. They are typically small, round or oval, and have a distinct white or yellowish center surrounded by a bright red halo of inflammation.
- Size: Usually less than 1 centimeter (about 1/2 inch) in diameter, often ranging from 1 to 10 millimeters.
- Location: Primarily found on the non-keratinized movable oral mucosa, such as the inside of the lips and cheeks, floor of the mouth, underside of the tongue, and soft palate.
- Symptoms: Painful, especially when eating or speaking.
- Healing Time: Typically heal within 1 to 2 weeks without scarring.
- Recurrence: Can recur frequently, often in cycles.
Major Aphthous Ulcers (MaAUs)
- Description: Less common but far more severe than minor canker sores. These are larger, deeper, and often more irregularly shaped. They also present with a white/yellowish center and a red inflammatory border.
- Size: Greater than 1 centimeter (often 1/2 inch to 1 inch or more) in diameter.
- Location: Can occur in the same areas as minor ulcers but often extend deeper into the tissue.
- Symptoms: Extremely painful, often interfering significantly with eating, drinking, and speaking. They can cause a general feeling of malaise.
- Healing Time: Can take anywhere from 2 weeks to several months to heal. Due to their depth, they often result in scarring.
- Recurrence: Less frequent than minor ulcers but can be debilitating when they do occur. These may be more indicative of underlying systemic issues in non-diabetic individuals, and certainly in those with diabetes, their presence could signal compromised health.
Herpetiform Aphthous Ulcers (HAUs)
- Description: Despite the name, "herpetiform" (meaning herpes-like), these are not caused by the herpes virus and are not contagious. They are characterized by multiple, pinpoint-sized ulcers that occur in clusters, often coalescing to form larger, irregular lesions.
- Size: Each individual ulcer is very small, typically 1 to 3 millimeters. However, the clusters can cover a significant area.
- Location: Can appear anywhere in the mouth, but often on the tongue.
- Symptoms: Can be intensely painful due to the sheer number of lesions.
- Healing Time: Usually heal within 1 to 2 weeks without scarring, similar to minor aphthous ulcers.
- Recurrence: Tend to recur frequently.
In the context of diabetes, the distinction between these types is important because major aphthous ulcers, in particular, can be significantly more challenging to manage, leading to prolonged discomfort and potential nutritional deficiencies if eating becomes too painful. Slower healing in diabetic patients means even minor ulcers can behave more like major ones in terms of duration.
Causes / Why It Happens
The exact cause of canker sores remains somewhat elusive, as they are not contagious and not directly caused by bacteria or viruses (though bacteria can secondarily infect them). However, a combination of factors is believed to contribute to their development, often involving an aberrant immune response. For individuals with diabetes, these factors are frequently amplified or complicated by their underlying condition.
General Contributing Factors to Canker Sores
- Oral Trauma: Minor injury to the mouth from biting the cheek or tongue, aggressive tooth brushing, dental work, or ill-fitting dentures.
- Stress: Emotional stress is a well-known trigger.
- Acidic or Abrasive Foods: Foods like citrus fruits, pineapples, apples, figs, cheese, coffee, nuts, and spicy foods can irritate the oral mucosa in susceptible individuals.
- Nutritional Deficiencies: Lack of vitamin B12, folate (folic acid), iron, or zinc can predispose individuals to canker sores.
- Hormonal Shifts: Some women report a correlation with their menstrual cycle.
- Certain Toothpastes and Mouthwashes: Products containing sodium lauryl sulfate (SLS), a foaming agent, can irritate oral tissues in some people.
- Genetics: A family history of canker sores increases your likelihood of developing them.
- Immune System Dysfunction: Canker sores are often considered an autoimmune-like response where the body's immune system mistakenly attacks healthy oral cells.
- Systemic Conditions: Beyond diabetes, conditions like Celiac disease, Crohn's disease, Behcet's disease, and HIV/AIDS can be associated with recurrent aphthous ulcers.
Diabetes-Specific Links to Canker Sores
For individuals managing diabetes, several physiological changes can exacerbate the general factors above and introduce new ones, leading to more frequent, severe, or persistent canker sores:
- Impaired Immune Response: High blood glucose levels (hyperglycemia) can compromise various aspects of the immune system. Neutrophils, key immune cells, may function less efficiently, and antibody production can be altered. This reduces the body's ability to protect oral tissues from minor irritations or fight off potential secondary infections, making canker sores more likely to form and harder to heal.
- Microvascular Changes: Diabetes damages small blood vessels (microangiopathy), which can reduce blood flow to the oral tissues. This diminished circulation hinders the delivery of oxygen, nutrients, and immune cells essential for tissue repair and healing, directly contributing to prolonged canker sore duration.
- Increased Inflammation and Oxidative Stress: Diabetes is characterized by chronic low-grade systemic inflammation and increased oxidative stress. This heightened inflammatory state can make oral mucosa more sensitive and reactive to triggers, potentially initiating or worsening the inflammatory response associated with canker sore formation.
- Glycemic Control: Poorly controlled diabetes is a significant risk factor. When blood glucose levels are consistently high, the oral environment can become more acidic or sugar-rich, which might favor certain microbial imbalances or directly irritate tissues. Good glycemic control is paramount in reducing the frequency and severity of oral complications, including canker sores.
- Medication Side Effects: While generally not a primary cause, some medications can have oral side effects. It's crucial for your dental professional to be aware of all medications you are taking, especially if you experience recurrent oral lesions.
- Nutritional Deficiencies: Diabetics, particularly those with Type 1 or poorly managed Type 2, might have specific dietary restrictions or absorption issues that could lead to deficiencies in B vitamins, iron, or zinc, all of which are linked to canker sore development.
Addressing Specific Keywords: "Oral Osteoporosis Drugs" and "Oil Pulling Inflammation"
While "diabetes and canker sores" is the primary focus, it's essential to address related keywords like "oral osteoporosis drugs" and "oil pulling inflammation" with medical accuracy and relevance to our target audience.
Oral Osteoporosis Drugs (Bisphosphonates)
Oral osteoporosis drugs, specifically bisphosphonates, are crucial for managing bone density. However, it is vital to clarify that these medications are not a direct cause of typical canker sores. Bisphosphonates are primarily associated with a rare but serious oral health complication known as osteonecrosis of the jaw (ONJ), particularly after invasive dental procedures like tooth extractions.
Important Note for Diabetics: Individuals with diabetes are already at a higher risk for various oral complications and slower healing. If a diabetic patient is also taking oral bisphosphonates, the combined effect of compromised healing from diabetes and the ONJ risk from bisphosphonates means that any invasive dental procedure requires meticulous planning and communication between the patient, their dentist, and their endocrinologist/physician. While ONJ is distinct from canker sores, it underscores the importance of a comprehensive medical history for your dental team. Your dentist needs to be aware of all your medications to provide the safest and most effective care, ensuring the best outcomes for your oral health.
Oil Pulling Inflammation
Oil pulling is an ancient Ayurvedic practice involving swishing oil (like coconut or sesame oil) in the mouth for an extended period. Proponents claim it can improve oral hygiene, reduce bacteria, and decrease inflammation.
Regarding oil pulling inflammation in the context of canker sores and diabetes:
- Limited Scientific Evidence: There is limited robust scientific evidence to support oil pulling as an effective treatment or preventative measure specifically for canker sores. Most claims are anecdotal.
- Potential for Irritation: While generally considered safe for most, some individuals may experience oral irritation or even inflammation from oil pulling, especially if they have sensitive oral tissues or an underlying condition like diabetes. The prolonged contact with certain oils or vigorous swishing could potentially exacerbate existing oral lesions or trigger new ones in a susceptible mouth.
- Allergic Reactions: Though rare, allergic reactions to specific oils (e.g., coconut oil) are possible, leading to oral inflammation or discomfort.
- Recommendation: For individuals with diabetes, whose oral tissues may be more fragile or prone to delayed healing, it's essential to exercise caution with unproven remedies. Focusing on evidence-based oral hygiene practices and effective diabetes management is paramount. If you choose to try oil pulling, discontinue immediately if any irritation or worsening of canker sores occurs. Always discuss alternative therapies with your dentist or physician, especially when managing a chronic condition like diabetes.
Signs and Symptoms
Identifying canker sores is usually straightforward due to their distinct appearance and the characteristic pain they cause. For individuals with diabetes, while the signs are similar, the intensity and duration of symptoms might be amplified.
Primary Signs and Symptoms:
- Painful Sores: The hallmark symptom. Canker sores are typically very painful, often described as a burning, stinging, or tingling sensation that precedes the visible sore by a day or two. The pain can range from mild discomfort to severe agony, especially when eating, drinking, or speaking.
- Location: Most commonly found on the soft, movable tissues of the mouth, including:
- Inside the lips and cheeks
- Tongue (sides, tip, or underside)
- Soft palate (the back, soft part of the roof of your mouth)
- Floor of the mouth
- Base of the gums (but not usually on the attached gum tissue around the teeth, which is more common for cold sores or herpes)
- Appearance:
- Small, Round or Oval: Typically well-defined, with a distinct shape.
- White or Yellowish Center: This is the fibrin membrane covering the ulcer base.
- Red, Inflamed Border: A characteristic halo of redness surrounds the central white/yellow area.
- Single or Multiple: You might have one sore or several appearing simultaneously, or in clusters (as with herpetiform aphthae).
- Difficulty with Oral Functions: Due to pain, you might experience:
- Trouble eating, leading to reduced food intake.
- Difficulty speaking clearly.
- Discomfort when swallowing.
- General irritability due to persistent pain.
Less Common Symptoms (More often associated with major aphthous ulcers or systemic involvement):
- Fever: While rare for typical canker sores, a low-grade fever can accompany particularly severe or extensive outbreaks.
- Swollen Lymph Nodes: Lymph nodes under the jaw or in the neck may swell, indicating an immune response to the inflammation.
- General Malaise: A feeling of being unwell or fatigued.
Specific Considerations for Diabetics:
- Increased Severity: The pain and discomfort might be more pronounced due to heightened inflammatory responses.
- Prolonged Duration: As discussed, impaired healing mechanisms in diabetes can mean sores last significantly longer than the typical 1-2 weeks. Minor sores might persist for 3-4 weeks, and major ones could linger for months.
- Higher Frequency: Diabetics may experience more frequent recurrences of canker sores due to chronic immune system modulation.
- Secondary Infection Risk: Slower healing and compromised immunity increase the risk of the open sore becoming secondarily infected by bacteria or fungi, which can complicate treatment and extend healing time.
Recognizing these signs early, especially if you have diabetes, allows for prompt intervention and better management to alleviate discomfort and prevent complications.
Treatment Options
Treating canker sores, especially for individuals with diabetes, focuses on pain relief, accelerating healing, preventing secondary infection, and addressing underlying systemic factors. A multi-pronged approach often yields the best results.
Over-the-Counter (OTC) Remedies
These are often the first line of defense for minor canker sores.
- Topical Numbing Agents:
- Description: Gels or liquids containing benzocaine (e.g., Orajel, Anbesol) or lidocaine. They temporarily numb the area, providing immediate pain relief.
- Pros: Readily available, provides quick relief.
- Cons: Short-acting, doesn't promote healing, can alter taste.
- Typical Cost: $5 - $15.
- Protective Pastes/Patches:
- Description: Adherent pastes (e.g., Orabase, Zilactin-B) or dissolvable patches that cover the sore, protecting it from irritation from food, drink, and saliva.
- Pros: Creates a physical barrier, allows healing underneath, lasts longer than numbing agents.
- Cons: Can be challenging to apply in certain areas, may not adhere well in a moist environment.
- Typical Cost: $10 - $20.
- Oral Rinses:
- Saltwater Rinse: Dissolve 1 teaspoon of salt in 8 ounces of warm water. Swish gently for 30 seconds, then spit.
- Pros: Reduces inflammation, cleanses the area, very inexpensive.
- Cons: Can sting initially.
- Baking Soda Rinse: Dissolve 1 teaspoon of baking soda in 8 ounces of warm water.
- Pros: Soothes, neutralizes acids, helps cleanse.
- Cons: Chalky taste.
- Diluted Hydrogen Peroxide Rinse: Mix 1 part 3% hydrogen peroxide with 1 part water. Use as a rinse, then rinse with plain water. Use sparingly, no more than twice daily.
- Pros: Antiseptic, helps clean the lesion.
- Cons: Can be irritating if not properly diluted, should not be swallowed.
- Typical Cost: Minimal for ingredients (pennies).
- Saltwater Rinse: Dissolve 1 teaspoon of salt in 8 ounces of warm water. Swish gently for 30 seconds, then spit.
Prescription Medications
For more severe, frequent, or persistent canker sores, especially in diabetic patients, a dentist or physician may prescribe stronger treatments.
- Topical Corticosteroids:
- Description: Gels, creams, or pastes containing corticosteroids (e.g., fluocinonide, clobetasol, triamcinolone acetonide). These reduce inflammation and pain, promoting faster healing.
- Pros: Highly effective for reducing inflammation and accelerating healing.
- Cons: Requires prescription, proper application technique is crucial, long-term use can thin oral tissues or lead to fungal overgrowth (thrush), especially in diabetics.
- Typical Cost: $20 - $100 (generic) to $200+ (brand name), varies by insurance.
- Corticosteroid Oral Rinses:
- Description: Dexamethasone elixir or prednisolone solution can be used as a rinse for multiple or hard-to-reach sores.
- Pros: Covers a wider area, effective for multiple lesions.
- Cons: Same potential side effects as topical steroids, should not be swallowed.
- Typical Cost: $30 - $150, varies by insurance.
- Antibiotic or Antimicrobial Rinses:
- Description: Chlorhexidine gluconate rinse or doxycycline syrup (swished and spit) might be prescribed if there's concern for secondary bacterial infection or to promote healing.
- Pros: Helps prevent/treat secondary infections, some have anti-inflammatory properties.
- Cons: Chlorhexidine can stain teeth with prolonged use, can alter taste.
- Typical Cost: $20 - $50.
- Systemic Medications (Rare):
- Description: For very severe, recurrent, or debilitating major aphthous ulcers, oral medications like colchicine, thalidomide, or corticosteroids may be considered. These are generally reserved for extreme cases due to potential significant side effects.
- Pros: Can provide systemic relief for severe cases.
- Cons: Significant side effects, requires close medical supervision, often not the first choice for typical canker sores.
- Typical Cost: Varies widely, potentially $100-$1000s depending on medication and duration.
Dental Procedures
- Chemical Cautery (Silver Nitrate):
- Description: Application of a chemical agent (like silver nitrate stick) directly to the sore to destroy nerve endings and cauterize the lesion.
- Pros: Provides immediate pain relief, can accelerate healing for some.
- Cons: Can be painful during application, may cause temporary black staining, not suitable for all sores.
- Typical Cost: $50 - $150 (often part of a dental visit fee).
- Low-Level Laser Therapy (LLLT):
- Description: Application of a therapeutic laser directly to the canker sore.
- Pros: Reduces pain, inflammation, and accelerates healing by stimulating cellular activity. It's quick, non-invasive, and well-tolerated.
- Cons: Requires a dental visit, not always covered by insurance.
- Typical Cost: $50 - $250 per session.
Nutritional Supplements
If nutritional deficiencies (B12, folate, iron, zinc) are identified, supplementation can be crucial, especially as diabetics can have unique dietary needs or absorption challenges.
- Pros: Addresses underlying causes, promotes overall health.
- Cons: Only effective if a deficiency exists, requires diagnosis.
- Typical Cost: $10 - $50 for a bottle of supplements.
Pro Tip: For individuals with diabetes, it's paramount to inform your dentist about your condition and all medications you're taking before starting any new treatment for canker sores. This ensures that selected treatments are safe and won't interfere with your diabetes management. Strict blood glucose control remains a foundational "treatment" that can significantly improve your body's ability to heal and prevent future sores.
Step-by-Step Process for Professional Canker Sore Treatment (e.g., Laser Therapy)
While many canker sores are managed with home remedies, seeking professional dental care, especially for recurrent, severe, or persistent sores in diabetic patients, is often beneficial. Here's what you can expect if your dentist recommends a professional treatment like laser therapy:
Step 1: Initial Consultation and Diagnosis
- Scheduling: You'll schedule an appointment with your dentist or an oral medicine specialist.
- Medical History Review: Your dental professional will meticulously review your medical history, paying close attention to your diabetes diagnosis, current glycemic control (e.g., recent HbA1c levels), and all medications you are taking, including any oral osteoporosis drugs or insulin. This is crucial for understanding your systemic health and potential healing capabilities.
- Oral Examination: The dentist will perform a thorough intraoral examination to visually inspect the canker sore(s), noting their size, location, appearance, and any signs of infection. They will differentiate it from other oral lesions (like cold sores, fungal infections, or more serious conditions).
- Discussion of Symptoms: You'll discuss the duration of the sore, the level of pain, and how it impacts your daily activities (eating, speaking).
- Treatment Recommendation: Based on the assessment, the dentist will recommend the most appropriate treatment option, explaining the benefits and potential considerations, especially given your diabetes. If laser therapy is chosen, they will explain the procedure.
Step 2: Preparing for Treatment
- Informed Consent: You will be provided with information about the treatment and asked to sign a consent form.
- Anesthesia (Optional): For highly sensitive sores or very painful areas, the dentist might apply a topical anesthetic gel to numb the area slightly before laser application. Most laser treatments for canker sores are comfortable enough not to require injectible anesthesia.
- Protective Eyewear: Both you and the dental professional will wear protective eyewear to shield your eyes from the laser light.
Step 3: The Laser Treatment Procedure
- Patient Positioning: You will be comfortably seated in the dental chair.
- Laser Application: The dentist will use a small, handheld soft-tissue laser device. The laser tip will be gently placed near or lightly brushed over the canker sore.
- Duration: The treatment is very quick, usually lasting only 1-5 minutes per sore, depending on its size. You might feel a mild warming sensation or nothing at all. There is typically no pain during the procedure.
- Mechanism: The low-level laser light energy penetrates the tissue, reducing inflammation, decreasing pain by desensitizing nerve endings, and stimulating cellular regeneration to accelerate healing.
Step 4: Immediate Post-Treatment
- Immediate Relief: Many patients report immediate or significant pain relief shortly after the laser treatment.
- No Downtime: There is no "downtime" required. You can typically resume normal activities immediately.
- Post-Treatment Instructions: The dentist will provide specific aftercare instructions, which may include avoiding irritating foods for a short period, continuing gentle oral hygiene, and monitoring the healing process.
Step 5: Recovery and Follow-up
- Healing Progression: The sore should start to heal noticeably faster than it would without treatment. Pain relief often lasts for several hours to days, allowing for more comfortable eating and speaking.
- Follow-up (If Needed): For very large or persistent sores, or if you have frequent recurrences due to your diabetes, your dentist might recommend a follow-up visit or additional laser sessions. They may also discuss strategies for diabetes control and nutritional support.
- Continued Diabetes Management: Emphasize the importance of maintaining optimal blood glucose control to prevent future outbreaks and support overall oral healing.
This structured approach ensures that individuals with diabetes receive tailored, effective, and safe treatment for their canker sores, minimizing discomfort and promoting quicker recovery.
Cost and Insurance
Understanding the financial aspect of canker sore treatment, particularly for individuals with diabetes who may face more frequent or complex issues, is essential. Costs can vary significantly based on the type of treatment, the provider, and geographic location within the US. Insurance coverage is also a crucial factor.
Cost Ranges for Canker Sore Treatments (USA)
Costs listed are typical out-of-pocket expenses without insurance, though insurance may reduce them.
- Over-the-Counter (OTC) Remedies:
- Numbing gels (e.g., Orajel, Anbesol): $5 - $15 per tube
- Protective pastes/patches (e.g., Orabase): $10 - $20 per tube/pack
- Saltwater/Baking Soda Ingredients: Less than $5 for a supply
- Total for basic self-care: $5 - $30
- Prescription Medications (Topical/Rinses):
- Topical Corticosteroid Gels (e.g., Triamcinolone acetonide): $20 - $100 (generic) / $100 - $200+ (brand name) per tube.
- Corticosteroid Oral Rinses (e.g., Dexamethasone elixir): $30 - $150 per bottle.
- Antibiotic/Antimicrobial Rinses (e.g., Chlorhexidine): $20 - $50 per bottle.
- Costs vary significantly based on pharmacy, generic vs. brand, and dosage.
- Professional Dental Procedures:
- Dental Consultation/Examination (for diagnosis): $50 - $150 (if not part of a routine check-up).
- Chemical Cautery (Silver Nitrate): $50 - $150 per sore (often in addition to consultation fee).
- Low-Level Laser Therapy (LLLT): $50 - $250 per session, per sore (some clinics may offer package deals for multiple sores or sessions).
- Total for professional treatment: $100 - $400+ depending on complexity.
Insurance Coverage Details
Navigating insurance for canker sores can be complex, as coverage depends on whether the treatment is considered medical or dental, and the specific plan's terms.
- Dental Insurance:
- Generally limited: Most standard dental insurance plans (PPO, HMO, DHMO) do not directly cover the treatment of canker sores as a stand-alone procedure. They are often considered elective or minor cosmetic/symptomatic relief, not a restorative dental procedure.
- Exceptions: If the canker sore is a symptom of a larger, covered dental issue (e.g., an ulcer caused by an ill-fitting crown requiring adjustment, or a lesion requiring biopsy for diagnosis), some aspects of the visit or procedure might be covered.
- Diagnostic Visits: The initial examination and diagnosis might be covered under your preventative or basic dental care benefits, depending on your plan's deductible and co-pay structure.
- PPO vs. HMO: PPO plans offer more flexibility in choosing providers and may cover a small percentage of specialized treatments after deductibles are met. HMO/DHMO plans typically require you to see an in-network provider and may have higher restrictions on what's covered.
- Medical Insurance:
- Prescription Medications: If your physician or dentist prescribes oral medications or strong topical prescriptions for recurrent or severe canker sores, your medical insurance plan (e.g., employer-sponsored, ACA marketplace, Medicare Part D, Medicaid) will typically cover these under your prescription drug benefits. This usually involves a co-pay, and the cost contributes to your annual deductible and out-of-pocket maximum.
- Systemic Conditions: If the canker sores are diagnosed as a manifestation of an underlying systemic medical condition (beyond general diabetes management, e.g., inflammatory bowel disease), then diagnostics and treatments related to that medical condition may be covered under your medical plan.
- Medicare/Medicaid: Coverage varies widely. Medicare Part B might cover some physician visits, and Part D covers prescriptions. Medicaid typically has broad coverage for necessary medical care and prescriptions, but dental coverage can be limited for adults.
Pro Tip: Always call your dental and medical insurance providers before receiving treatment to confirm coverage details. Ask for the specific procedure codes (CADA codes for dental, CPT codes for medical) for the recommended treatment and inquire about your benefits, deductibles, co-pays, and out-of-pocket maximums. For diabetics, clearly explain that you have diabetes and are inquiring about treatment for a related oral complication, as this might influence how the claim is processed.
Recovery and Aftercare
Effective recovery and aftercare are crucial for minimizing discomfort, promoting healing, and preventing recurrence of canker sores, especially for individuals with diabetes. Your body's ability to heal is directly linked to your overall health and diligent management of your condition.
Immediate Aftercare Post-Treatment
Whether you've used OTC remedies, prescription medications, or undergone professional treatment like laser therapy, these steps will support healing:
- Pain Management:
- Continue OTC pain relievers: If pain persists after treatment, acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) can help. Always check with your doctor if these are safe with your diabetes medications.
- Topical agents: Continue using prescribed topical numbing gels or protective pastes as directed for ongoing comfort.
- Dietary Adjustments:
- Soft, Bland Foods: Stick to soft, non-acidic, non-spicy, and non-abrasive foods for several days. Think yogurt, mashed potatoes, cooked vegetables, soft fruits, soups, and oatmeal.
- Avoid Triggers: Steer clear of foods known to irritate canker sores, such as citrus fruits, tomatoes, coffee, chocolate, nuts, pretzels, and very hot or cold items.
- Hydration: Drink plenty of water to keep your mouth moist and aid in healing. Avoid sugary drinks which can worsen oral health for diabetics.
- Oral Hygiene:
- Gentle Brushing: Continue to brush your teeth twice daily with a soft-bristled toothbrush. Be extra gentle around the sore to avoid further irritation.
- Non-SLS Toothpaste: Consider using a toothpaste that does not contain sodium lauryl sulfate (SLS), as it can be an irritant for some people and potentially exacerbate canker sores. Brands like Sensodyne Pronamel or Boka often offer SLS-free options.
- Mild Rinses: Continue using lukewarm saltwater rinses or a mild, alcohol-free mouthwash as recommended by your dentist. Avoid harsh, alcohol-based mouthwashes that can sting and irritate the sore.
- Monitoring Healing:
- Observe the sore daily. It should gradually decrease in size, and the redness around it should subside. The pain should lessen progressively.
- For minor sores, expect improvement within a few days and full healing in 1-2 weeks. Major sores, especially in diabetics, will take longer.
Long-Term Aftercare and Prevention
Beyond the immediate healing phase, long-term strategies are crucial for preventing recurrence, particularly when managing diabetes.
- Strict Blood Glucose Control: This is the single most important aftercare and preventative measure for diabetics. Well-managed blood sugar levels directly support immune function, improve circulation, and enhance the body's natural healing capabilities, reducing both the frequency and severity of canker sores. Work closely with your endocrinologist or primary care physician to maintain your target HbA1c and daily blood glucose levels.
- Nutritional Support:
- Ensure a balanced diet rich in vitamins and minerals. If a deficiency was identified (B12, folate, iron, zinc), continue with supplements as advised by your healthcare provider.
- Consult a registered dietitian specializing in diabetes for personalized dietary advice to manage both your diabetes and nutritional needs, which can impact oral health.
- Stress Management: Identify and implement strategies to reduce stress, such as exercise, meditation, yoga, hobbies, or adequate sleep. Stress is a significant trigger for canker sores.
- Avoid Known Triggers: Once you identify specific foods or habits that trigger your canker sores, consistently avoid them.
- Regular Dental Check-ups: Maintain a schedule of professional dental cleanings and examinations, ideally every 3-6 months for individuals with diabetes, as recommended by the American Dental Association (ADA). Your dentist can identify potential issues early and provide guidance on oral hygiene specific to your needs.
- Address Dental Issues: Ensure any ill-fitting dentures, sharp tooth edges, or orthodontic appliances that might cause trauma are addressed promptly by your dentist.
- Consider Oral Osteoporosis Drugs Disclosure: If you are prescribed oral osteoporosis drugs (bisphosphonates) at any point, inform your dentist immediately. While not a cause of canker sores, these medications require careful consideration for any invasive dental procedures due to the risk of osteonecrosis of the jaw, especially for diabetic patients with compromised healing. Your dentist will coordinate with your physician to ensure optimal safety.
- **Re-evaluate Oil Pulling: If you were attempting oil pulling and experienced any irritation or worsening of symptoms, discontinue it. Focus on scientifically proven oral hygiene practices. If considering it again, consult your dentist first.
By diligently following these recovery and aftercare instructions, and critically by maintaining optimal diabetes management, you can significantly reduce the impact of canker sores on your oral health and overall well-being.
Prevention
Preventing canker sores, especially for individuals with diabetes, involves a combination of general oral health practices, managing specific triggers, and crucially, maintaining excellent control over blood glucose levels. Proactive measures are often more effective and comfortable than reactive treatments.
Primary Prevention Strategies
- Optimal Diabetes Management: This is the cornerstone of prevention for diabetics.
- Strict Blood Glucose Control: Consistent management of blood glucose levels through diet, exercise, and medication adherence is vital. Stable blood sugar reduces inflammation, supports immune function, and improves healing capacity, significantly lowering the risk of canker sores and other oral complications.
- Regular Monitoring: Routinely monitor your blood glucose and HbA1c levels and work closely with your healthcare team to keep them within target ranges.
- Identify and Avoid Triggers:
- Dietary Triggers: Keep a food diary to identify specific foods that seem to precipitate canker sores. Common culprits include acidic foods (citrus fruits, tomatoes, pineapple), spicy foods, very hot beverages, chocolate, coffee, nuts, and abrasive foods (pretzels, chips). Once identified, limit or avoid these foods.
- Stress Management: Implement stress-reduction techniques such as meditation, yoga, regular exercise, adequate sleep (7-9 hours per night), or spending time on hobbies. Stress is a powerful trigger for canker sores.
- Excellent Oral Hygiene:
- Gentle Brushing: Use a soft-bristled toothbrush and brush gently twice a day. Avoid aggressive brushing that can cause micro-trauma to the oral tissues.
- Non-SLS Toothpaste: Many individuals find relief by switching to toothpastes free of sodium lauryl sulfate (SLS), a foaming agent that can irritate the oral lining. Look for "SLS-free" on the label.
- Flossing: Floss daily to remove food particles and plaque, preventing gum irritation and maintaining overall oral health.
- Mild Mouthwash: Use an alcohol-free, mild mouthwash if desired. Avoid harsh, alcohol-containing rinses that can dry and irritate the mouth.
- Regular Dental Check-ups: Schedule professional cleanings and examinations at least twice a year, or more frequently (every 3-4 months) if recommended by your dentist due to your diabetic status.
- Prevent Oral Trauma:
- Chewing Carefully: Be mindful while eating to avoid accidentally biting your cheeks, lips, or tongue.
- Check Dental Appliances: Ensure dentures, braces, or retainers fit properly and don't rub or create sharp spots. Report any irritation to your dentist or orthodontist promptly.
- Avoid Harsh Oral Products: Be cautious with new toothpastes, mouthwashes, or dental tools that might cause irritation.
- Address Nutritional Deficiencies:
- Ensure your diet is balanced and rich in essential vitamins and minerals.
- If you experience recurrent canker sores, ask your doctor to test for deficiencies in vitamin B12, folate, iron, and zinc. Supplement only if a deficiency is confirmed and under medical guidance. This is particularly important for diabetics who may have specific dietary considerations.
- Hydration: Keep your mouth moist by drinking plenty of water throughout the day. A dry mouth can increase susceptibility to irritation.
Clarifying "Oil Pulling Inflammation" in Prevention
While oil pulling is sometimes promoted as a preventive measure for various oral ailments, it's essential to approach it with a critical perspective, especially for individuals with diabetes.
- Limited Evidence for Canker Sores: There is currently insufficient scientific evidence to support oil pulling as an effective preventative strategy specifically for canker sores.
- Potential for Irritation: For some, particularly those with sensitive oral mucosa or underlying conditions like diabetes which can make tissues more fragile, oil pulling can potentially cause irritation or even inflammation if done vigorously or with oils that are not well-tolerated. This can ironically contribute to canker sore formation rather than prevent it.
- Focus on Evidence-Based Practices: Given the limited evidence and potential for irritation, it's generally recommended for individuals with diabetes to prioritize evidence-based oral hygiene practices (brushing, flossing, regular dental visits) and strict blood glucose control over unproven alternative therapies for canker sore prevention. If you wish to try oil pulling, discuss it with your dentist first and discontinue immediately if any adverse effects occur.
By integrating meticulous diabetes management with conscious oral care and trigger avoidance, you can significantly reduce the likelihood and severity of canker sores, contributing to better oral health and overall well-being.
Risks and Complications
While often considered minor inconveniences, canker sores, particularly when persistent or severe in individuals with diabetes, can lead to several risks and complications. Understanding these can help in deciding when to seek professional help and emphasizes the importance of diligent management.
General Risks and Complications:
- Severe Pain and Discomfort: The most immediate and common complication. Canker sores can be excruciatingly painful, making basic functions like eating, drinking, and speaking very difficult. This can significantly impact quality of life.
- Nutritional Deficiencies and Weight Loss: Prolonged pain can deter individuals from eating adequately, leading to reduced calorie intake, weight loss, and potential nutritional deficiencies, which can further impede healing.
- Difficulty Swallowing (Dysphagia): Large or numerous sores, especially in the throat area, can make swallowing painful or challenging.
- Secondary Infection: The open wound of a canker sore is susceptible to bacterial or fungal infections. This can prolong healing, increase pain, and potentially spread. Signs include increased redness, pus, fever, or swelling.
- Scarring: Major aphthous ulcers, due to their depth and prolonged healing time, often leave noticeable scars on the oral mucosa.
- Recurrence: For many individuals, canker sores are a recurrent problem, leading to chronic discomfort and frustration.
Specific Risks and Complications for Diabetics:
For individuals living with diabetes, these general risks are often heightened, and new, diabetes-specific complications can arise:
- Prolonged Healing: As discussed, impaired immune function and microvascular changes in diabetes mean canker sores take significantly longer to heal. A sore that might resolve in a week for a non-diabetic could linger for 3-4 weeks or even months in a diabetic patient. This prolongs discomfort and increases the window for secondary infection.
- Increased Risk of Secondary Infection: The compromised immune system in poorly controlled diabetes makes individuals more vulnerable to secondary bacterial or fungal infections within the canker sore. This can complicate treatment and further delay healing.
- Impact on Blood Glucose Control: Severe canker sores can indirectly affect diabetes management:
- Dietary Changes: Pain may lead to avoidance of healthy, complex carbohydrates and preference for soft, often higher-sugar foods, potentially spiking blood glucose.
- Stress: Chronic pain and discomfort are significant stressors, which can elevate blood glucose levels in diabetics.
- Reduced Activity: Pain might limit physical activity, impacting glucose utilization.
- Medication Adherence: Discomfort might make it difficult to adhere to regular meal schedules, potentially affecting medication timing (e.g., insulin doses).
- Misdiagnosis of Serious Conditions: While rare, persistent or unusual oral lesions could be signs of more serious conditions, including oral cancer or other autoimmune diseases. For diabetics with a higher baseline risk for various health issues, it is crucial not to dismiss unusual oral lesions and to have them evaluated by a dental professional.
- Systemic Spread of Infection: In extremely rare and severe cases of unchecked secondary infection, there is a theoretical risk of localized oral infection spreading systemically, which can be particularly dangerous for immunocompromised individuals like diabetics.
Therefore, for anyone with diabetes, vigilance regarding oral health and prompt attention to canker sores is not just about comfort but a critical component of overall diabetes management and preventing more serious health consequences.
Comparison Tables
To help visualize the differences between types of canker sores and their treatment options, here are two comparison tables:
Table 1: Canker Sore Types Comparison
| Feature | Minor Aphthous Ulcers (MiAUs) | Major Aphthous Ulcers (MaAUs) | Herpetiform Aphthous Ulcers (HAUs) |
|---|---|---|---|
| Prevalence | Most common (80-85%) | Less common (10-15%) | Least common (5-10%) |
| Size | Small (1-10 mm, typically <1 cm) | Large (>10 mm, often 1-3 cm or more) | Very small (1-3 mm), appear in clusters |
| Appearance | Round/oval, white/yellow center, red halo | Deep, irregular, white/yellow center, red halo | Numerous tiny ulcers, often coalesce, resemble herpes |
| Location | Movable oral mucosa (lips, cheeks, tongue, soft palate) | Any oral mucosa, often deeper tissues | Any oral mucosa, frequently tongue |
| Pain Level | Moderate to significant pain | Severe, debilitating pain | Intense pain due to multiple lesions |
| Healing Time | 1-2 weeks | 2 weeks to several months (can be much longer in diabetics) | 1-2 weeks |
| Scarring | No | Yes, often | No |
| Recurrence | Frequent | Less frequent, but debilitating when they occur | Frequent |
| Diabetic Impact | May be more frequent and slower healing | Increased severity and significantly prolonged healing, higher risk of scarring | May be more frequent and slower healing |
Table 2: Canker Sore Treatment Options Comparison
| Treatment Option | Method | Pros | Cons | Typical Cost Range (USD) |
|---|---|---|---|---|
| OTC Numbing Gels | Apply gel directly to sore | Quick, temporary pain relief, readily available | Short-acting, doesn't promote healing | $5 - $15 |
| Protective Pastes | Apply paste to cover sore | Forms protective barrier, aids healing, longer lasting | Can be hard to apply/adhere, doesn't treat underlying cause | $10 - $20 |
| Saltwater Rinse | Swish warm salt water | Reduces inflammation, cleanses, very inexpensive | Can sting initially, doesn't target specific pain | < $5 |
| Topical Steroids | Prescription gel/paste applied to sore | Effectively reduces inflammation, accelerates healing | Requires prescription, potential for side effects with long-term use | $20 - $200 (generic to brand) |
| Oral Steroid Rinse | Prescription liquid swished and spit | Good for multiple/hard-to-reach sores, reduces inflammation | Requires prescription, potential side effects, shouldn't be swallowed | $30 - $150 |
| Laser Therapy (LLLT) | Dental laser applied to sore | Immediate pain relief, accelerates healing, non-invasive | Requires dental visit, may not be insurance covered | $50 - $250 per session |
| Chemical Cautery | Chemical (e.g., silver nitrate) applied to sore | Immediate pain relief (by nerve destruction) | Can be painful during application, temporary staining, not for all sores | $50 - $150 |
| Nutritional Supp. | Oral supplements (B12, Iron, Zinc) | Addresses underlying deficiency | Only effective if deficiency exists, requires diagnosis | $10 - $50 (per bottle) |
| Diabetes Control | Diet, exercise, medication | Fundamental for prevention and healing (systemic benefit) | Ongoing effort, requires discipline and medical supervision | Ongoing (cost of meds, monitoring) |
Children / Pediatric Considerations
Canker sores are common in children, just as they are in adults, and can be particularly distressing for young ones due to the pain and difficulty eating. When a child also has diabetes (most commonly Type 1, though Type 2 is increasing in adolescents), the management and considerations become even more critical.

Prevalence and Presentation in Children
- Common Occurrence: Canker sores frequently appear in children, often starting around ages 10-20, but can occur younger. Minor aphthous ulcers are the most common type.
- Triggers: Similar to adults, common triggers include minor trauma (biting the cheek, aggressive brushing), stress (e.g., school exams, family changes), acidic foods, and sometimes nutritional deficiencies.
- Symptoms: Children may express pain by crying, refusing to eat or drink, becoming irritable, or pointing to their mouth. They may drool more due to pain when swallowing.
Diabetes in Children and Canker Sores
- Increased Vulnerability: Children with diabetes, particularly those with fluctuating or poorly controlled blood sugar, are more susceptible to canker sores due to their developing immune systems and the systemic effects of diabetes. Their healing might also be slower than non-diabetic children.
- Impact on Nutrition: For diabetic children, refusal to eat due to painful canker sores can be particularly problematic, potentially affecting blood glucose stability and making diabetes management more challenging. It's crucial to ensure they continue to receive adequate nutrition to prevent hypoglycemia or hyperglycemia.
- Differentiating from Other Conditions: It's vital to differentiate canker sores from other common oral lesions in children, such as:
- Herpetic Gingivostomatitis: Caused by the herpes virus, presents with widespread ulcers, fever, and swollen gums. These are contagious.
- Hand-Foot-and-Mouth Disease: Caused by coxsackievirus, presents with sores in the mouth and rashes on hands and feet.
- Thrush (Oral Candidiasis): More common in diabetic children, appears as white patches that can be scraped off, sometimes leaving red, irritated areas underneath.
Management Strategies for Children with Diabetes
- Prioritize Diabetes Management: Above all, maintaining tight blood glucose control is the most critical preventative and healing measure for a diabetic child. Work closely with their endocrinologist and pediatrician.
- Pain Relief:
- Topical Numbing Gels: Child-safe numbing gels (e.g., those with benzocaine, ensure appropriate age and dosage) can provide temporary relief. Always consult a pediatrician or dentist before use.
- OTC Pain Relievers: Acetaminophen (Tylenol) or ibuprofen (Motrin, Advil) can help with pain and fever, adhering to age- and weight-appropriate dosing.
- Dietary Modifications:
- Soft, Bland, Non-Acidic Foods: Offer soft foods like yogurt, applesauce, mashed potatoes, well-cooked pasta, and smoothies. Avoid acidic, spicy, or crunchy foods.
- Hydration: Ensure the child drinks plenty of water to prevent dehydration, especially if they have a fever. Offer diluted, sugar-free juices or electrolyte solutions, carefully monitoring blood sugar.
- Nutritional Focus: If eating is very difficult, discuss with your child's diabetes care team about alternative nutritional strategies to maintain blood glucose stability and prevent deficiencies.
- Gentle Oral Hygiene:
- Use a very soft-bristled toothbrush and a mild, SLS-free toothpaste.
- Encourage gentle saltwater rinses if the child is old enough to swish and spit without swallowing.
- Identify Triggers: Help your child identify potential triggers, such as specific foods or stress factors, and work to minimize exposure.
- When to See a Dentist/Pediatrician:
- Sores that are large, extremely painful, or interfere significantly with eating/drinking.
- Sores that don't start to heal within a week or persist for more than 2 weeks.
- Frequent recurrence of sores.
- Any signs of secondary infection (fever, spreading redness, pus).
- If you suspect the lesion is not a typical canker sore.
- If the child's blood glucose control becomes erratic due to pain or inability to eat.
Pro Tip for Parents: Maintaining open communication with your child's diabetes care team and their dentist is essential. Inform all healthcare providers about oral health issues, as they can sometimes be an indicator of overall diabetes control. Early intervention for canker sores in diabetic children can prevent greater discomfort and ensure continuity in their diabetes management plan.
Cost Breakdown
A detailed breakdown of costs for canker sore treatments in the US helps readers understand potential expenses and navigate their healthcare options. For individuals with diabetes, the potential for more frequent or severe issues means these costs can add up.
Average US Costs (Low, Mid, High) for Canker Sore Treatment
Costs are estimates and can vary by region (e.g., urban vs. rural), provider's specialty, and specific clinic pricing.
- Self-Care / Over-the-Counter (OTC) Remedies:
- Low: $5 - $10 (e.g., store-brand numbing gel, baking soda for rinse)
- Mid: $10 - $30 (e.g., brand-name numbing gel + protective paste/patch)
- High: $30 - $50+ (e.g., combination of multiple OTC products, specialty SLS-free toothpaste)
- Frequency Impact: If recurring monthly, annual cost can be $60 - $600.
- Prescription Medications (Topical/Rinses):
- Low: $20 - $50 (generic topical corticosteroid cream/gel with good insurance co-pay)
- Mid: $50 - $150 (generic corticosteroid rinse or brand-name topical with average insurance)
- High: $150 - $300+ (brand-name prescription without good insurance, or specialized systemic medication for severe cases)
- Note: These prices are per prescription; recurring sores mean recurring costs.
- Professional Dental Procedures:
- Dental Consultation / Examination (Code D0120/D0140):
- Low: $50 - $80 (new patient promo, in-network with basic insurance coverage)
- Mid: $80 - $120 (typical visit without insurance, or with deductible)
- High: $120 - $180+ (specialist visit, out-of-network)
- Chemical Cautery (e.g., Silver Nitrate, often D9910):
- Low: $50 - $80 (in addition to exam fee)
- Mid: $80 - $120
- High: $120 - $150+
- Low-Level Laser Therapy (LLLT - often D9999/D7999, non-specific code):
- Low: $50 - $100 (per sore, often introductory offer or smaller lesion)
- Mid: $100 - $180 (per sore, typical for most clinics)
- High: $180 - $250+ (per sore, for larger lesions or premium clinics)
- Note: LLLT is often considered elective and may not have a specific ADA code, making insurance coverage less likely.
- Dental Consultation / Examination (Code D0120/D0140):
With vs. Without Insurance
- Without Insurance (Cash Pay): You will be responsible for 100% of the listed costs. Some dental offices offer cash discounts or in-house membership plans for uninsured patients, which can provide a small percentage off services.
- With Dental Insurance:
- Initial Exam: Often covered at 80-100% after deductible, especially if part of a routine check-up.
- Treatment: Coverage for specific canker sore treatments (cautery, laser) is generally very limited or non-existent. Many plans consider them non-covered services. You might pay 100% out-of-pocket for these.
- Deductibles & Co-pays: You'll typically pay a deductible ($50-$150) annually before coverage kicks in, and then a co-pay (e.g., 20-50%) for covered services.
- With Medical Insurance (for prescriptions):
- Prescription Drugs: Most medical plans (e.g., PPO, HMO, Medicare Part D, Medicaid) include prescription drug benefits.
- Co-pays: You'll pay a co-pay (often $10-$60, depending on generic/brand and tier) per prescription. This can significantly reduce the cost of prescription topical steroids or rinses.
- Deductibles: If your medical plan has a high deductible, you might pay the full cash price for prescriptions until your deductible is met.
Payment Plans and Financing Options
For higher-cost treatments or frequent visits, especially if insurance coverage is limited, consider these options:
- CareCredit: A popular healthcare credit card that offers promotional financing options (e.g., 6 or 12 months with no interest if paid in full). Accepted by many dental and medical offices.
- In-Office Payment Plans: Some dental practices offer their own installment plans, allowing you to pay the cost over a few months, often without interest.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer, you can use these tax-advantaged accounts to pay for qualified medical and dental expenses, including canker sore treatments and prescriptions.
Cost-Saving Tips
- Start with OTC: For minor sores, try inexpensive OTC remedies first.
- Maintain Excellent Diabetes Control: This is the best long-term cost-saving strategy by reducing the frequency and severity of canker sores.
- Preventative Care: Regular dental check-ups can identify issues early and prevent severe complications.
- Discuss Generics: Always ask your doctor or pharmacist if a generic version of a prescribed medication is available, as it's typically much cheaper.
- Shop Around for Prescriptions: Compare prices at different pharmacies or use discount cards (e.g., GoodRx) if paying out-of-pocket.
- Verify Insurance: Always contact your dental and medical insurance providers beforehand to understand exactly what is covered and what your out-of-pocket expenses will be.
Frequently Asked Questions
Here are some common questions patients with diabetes have about canker sores:
Is there a direct link between uncontrolled diabetes and canker sores?
Yes, there is a significant link. Uncontrolled or poorly managed diabetes can weaken your immune system, impair your body's healing capabilities, and increase inflammation throughout your body, including your oral tissues. These factors can lead to more frequent, severe, and slower-healing canker sores compared to individuals with well-managed blood glucose levels.
How long do canker sores typically last in someone with diabetes?
While minor canker sores typically heal within 1-2 weeks for the general population, individuals with diabetes may experience significantly prolonged healing times. Even minor sores can persist for 2-4 weeks, and major aphthous ulcers might take several weeks to months to resolve, often accompanied by increased pain and risk of complications.
Can specific foods trigger canker sores in diabetics, and what should be avoided?
Yes, certain foods can act as triggers. Acidic foods (citrus fruits, tomatoes, pineapples), spicy foods, very hot beverages, and abrasive items (chips, pretzels) can irritate oral tissues. Diabetics should also be mindful of sugary and processed foods that can negatively impact blood glucose and overall oral health. Keeping a food diary can help identify personal triggers.
Is laser treatment effective for canker sores in diabetic patients?
Yes, low-level laser therapy (LLLT) is generally considered an effective and safe treatment for canker sores, including in diabetic patients. It can provide immediate pain relief, reduce inflammation, and accelerate the healing process by stimulating cellular activity. It's non-invasive and typically well-tolerated, making it a good option for diabetics who may have prolonged healing otherwise.
Are canker sores contagious?
No, canker sores (aphthous ulcers) are not contagious. They are not caused by a virus like cold sores (herpes simplex) and cannot be spread through kissing, sharing utensils, or other close contact. Their origin is often linked to immune system responses, trauma, stress, or nutritional deficiencies.
What's the difference between a canker sore and a cold sore?
Canker sores occur inside the mouth on soft tissues (cheeks, tongue, soft palate), are not contagious, and are not caused by a virus. Cold sores (fever blisters) are caused by the herpes simplex virus, are highly contagious, and typically appear outside the mouth on the lips or around the nostrils.
When should a diabetic person see a dentist for a canker sore?
You should see a dentist if a canker sore is unusually large (>1/2 inch), extremely painful, lasts longer than 2-3 weeks, recurs frequently, is accompanied by fever, fatigue, or difficulty swallowing, or if you suspect it's not a typical canker sore. For diabetics, any persistent oral lesion warrants prompt professional evaluation due to compromised healing.
Are there natural remedies for canker sores that are safe for diabetics?
While some natural remedies like saltwater rinses, baking soda rinses, and aloe vera are generally safe and can provide symptomatic relief, their effectiveness for treating canker sores in diabetics is primarily supportive. Oil pulling, for example, has limited scientific evidence for canker sores and can potentially cause irritation in sensitive diabetic oral tissues. Always consult your dentist or physician before trying new natural remedies, especially with diabetes.
Can diabetes medications cause canker sores as a side effect?
While some medications can have oral side effects, it's uncommon for standard diabetes medications (like metformin, insulin, GLP-1 agonists) to directly cause canker sores. However, poor glucose control from unmanaged diabetes or a medication regimen not working optimally is a more likely contributor. Always discuss any new oral symptoms with your prescribing doctor and dentist.
Does frequent occurrence of canker sores mean my diabetes is poorly controlled?
Frequent or severe canker sores can be an indicator of compromised immune function and slower healing, which are often associated with suboptimal blood glucose control in diabetic individuals. While not a definitive diagnostic, increased incidence of canker sores should prompt a discussion with your healthcare team about reviewing your diabetes management plan and HbA1c levels.
When to See a Dentist
Given the increased risks and potential for complications in individuals with diabetes, it's crucial to know when a canker sore warrants a visit to your dental professional or physician. Don't simply wait for it to go away if you have diabetes.
You should schedule an appointment with your dentist or doctor if you experience any of the following:
- Sores Lasting Longer Than 2-3 Weeks: For anyone, but especially for diabetics whose healing is often compromised, a sore that persists beyond this timeframe needs professional evaluation to rule out other conditions and ensure proper healing.
- Unusually Large or Deep Sores: Canker sores larger than 1/2 inch (major aphthous ulcers) or those that appear particularly deep require professional attention, as they are often more painful, slower to heal, and can lead to scarring.
- Intense, Debilitating Pain: If the pain is so severe that it interferes significantly with your ability to eat, drink, speak, or get adequate sleep, professional treatment for pain relief and accelerated healing is necessary.
- Frequent or Recurrent Sores: If you experience frequent outbreaks of canker sores (e.g., several times a year, or multiple sores at once), it suggests an underlying issue that needs to be identified and addressed. This is a common concern for diabetics.
- New Sores Developing Before Old Ones Heal: This indicates a chronic problem that requires a comprehensive assessment.
- Signs of Infection: If you notice increased redness spreading beyond the sore, pus, swelling, fever, or swollen lymph nodes, the sore may be secondarily infected, requiring immediate medical attention.
- Accompanying Systemic Symptoms: If canker sores are accompanied by other general symptoms like unexplained fever, skin lesions, eye irritation, chronic fatigue, or gastrointestinal problems, it could indicate an underlying systemic condition that needs diagnosis and management.
- Uncertainty of Diagnosis: If you are unsure whether the lesion is a canker sore or something else (like a cold sore, fungal infection, or a more serious lesion), it's always best to have a dental professional examine it.
- Difficulty Managing Blood Glucose: If the pain or discomfort from canker sores is impacting your ability to follow your diet or medication schedule, leading to erratic blood glucose levels, inform your healthcare team immediately.
Red Flags vs. Routine Care Guidance:
- Routine Care: Minor, infrequent canker sores that heal quickly (within a week) and cause minimal discomfort can often be managed with OTC remedies.
- Red Flags (Seek Prompt Attention): Any of the above points, especially for individuals with diabetes, constitute a red flag and warrant prompt professional medical or dental advice. Do not delay seeking care, as early intervention can prevent complications and improve your quality of life.
When in doubt, always err on the side of caution and consult your dental professional. They can provide an accurate diagnosis, recommend appropriate treatment, and ensure your oral health is integrated with your overall diabetes management plan.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026