Tmj Specialist Near Me: Complete Guide
Key Takeaways
- Experiencing persistent jaw pain, clicking sounds, or difficulty opening your mouth can be incredibly disruptive, affecting everything from eating and speaking to your overall quality of life. If you're searching for a tmj specialist near me, it likely means you're tired of discomfort and ready
Tmj Specialist Near Me: Complete Guide
Experiencing persistent jaw pain, clicking sounds, or difficulty opening your mouth can be incredibly disruptive, affecting everything from eating and speaking to your overall quality of life. If you're searching for a tmj specialist near me, it likely means you're tired of discomfort and ready to find a lasting solution for your temporomandibular joint (TMJ) disorder. An estimated 10 million Americans are affected by TMJ disorders (TMDs) at any given time, making it a common yet often misunderstood condition. This comprehensive guide from SmilePedia.net will demystify TMDs, help you understand what causes TMJ issues, outline various treatment options, and provide crucial information on finding the right specialist to restore your jaw health and comfort. We'll cover everything from symptoms and diagnosis to advanced therapies and what to expect regarding costs and recovery, ensuring you have the knowledge to make informed decisions about your oral health.

Key Takeaways:
- TMJ disorders affect an estimated 10 million Americans, primarily women aged 20-40.
- Common causes include teeth grinding (bruxism), trauma, arthritis, stress, and bite issues.
- A TMJ specialist can be an oral surgeon, prosthodontist, orthodontist, or pain management specialist with advanced training.
- Initial conservative treatments often cost $200 - $1,500 (e.g., splints, physical therapy).
- Advanced treatments like surgery can range from $5,000 to over $50,000, with recovery times varying from weeks to several months.
- Insurance coverage for TMJ disorders varies widely; many plans consider it a medical issue rather than purely dental.
- Seek a specialist if you have persistent jaw pain, clicking/locking, or difficulty chewing/speaking.
What It Is / Overview: Understanding Your Temporomandibular Joint
The temporomandibular joint (TMJ) is one of the most complex joints in your body, acting like a sliding hinge connecting your jawbone (mandible) to your skull (temporal bone) on each side of your face. These two joints, located just in front of your ears, are responsible for all jaw movements, including chewing, speaking, yawning, and swallowing.
A temporomandibular disorder (TMD), often referred to simply as "TMJ," refers to a range of conditions that cause pain and dysfunction in the jaw joint and the muscles that control jaw movement. It's important to differentiate: "TMJ" is the joint itself, while "TMD" is the disorder. TMDs can manifest in various ways, from mild discomfort to severe, debilitating pain, significantly impacting a person's quality of life. The condition is more prevalent in women, particularly those between the ages of 20 and 40.
The TMJ consists of several key components:
- Mandibular condyle: The rounded end of the jawbone.
- Temporal bone: The socket in the skull where the condyle sits.
- Articular disc: A small, oval-shaped piece of cartilage that acts as a shock absorber between the condyle and the temporal bone, allowing for smooth movement.
- Ligaments, tendons, and muscles: These structures support the joint and facilitate its movement.
When any of these components are compromised or become dysfunctional, a TMD can develop, leading to a host of uncomfortable symptoms.
Types / Variations of TMJ Disorders
TMJ disorders are broadly categorized into three main types, though it's common for patients to experience a combination of these:
1. Myofascial Pain
This is the most common type of TMD, characterized by pain in the muscles that control jaw function (masseter, temporalis, pterygoids) and often extends to the neck and shoulders. It's frequently associated with clenching, grinding (bruxism), or stress. The pain is usually dull, aching, and persistent, often accompanied by tenderness when touching the muscles.
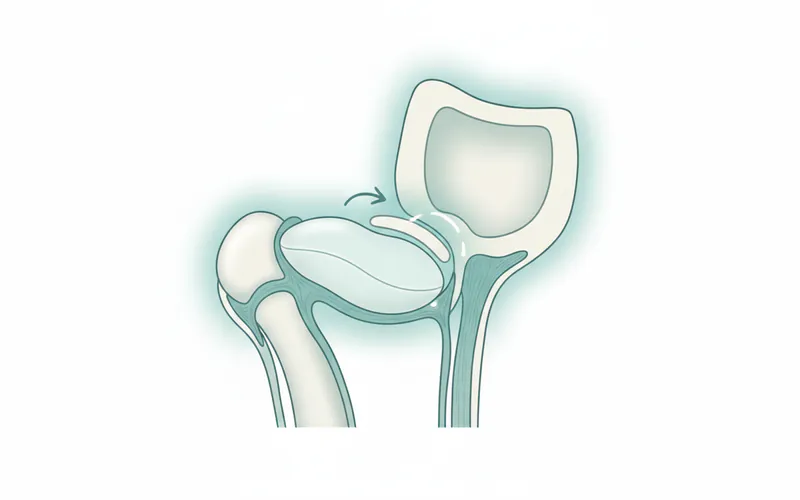
2. Internal Derangement of the Joint
This category refers to structural problems within the TMJ itself, most commonly involving the articular disc.
- Disc Displacement with Reduction: The disc slips out of its normal position when the jaw is at rest but snaps back into place when the mouth opens, often causing a clicking, popping, or clunking sound.
- Disc Displacement Without Reduction: The disc remains displaced even when the mouth opens fully, leading to limited jaw movement (e.g., "locked jaw") and pain, usually without the clicking sound.
- Subluxation: The condyle moves too far forward in the joint, past the articular eminence, and gets temporarily stuck before snapping back.
3. Degenerative Joint Disease (Arthritis)
This involves inflammatory or degenerative changes to the joint surfaces, similar to arthritis in other joints.
- Osteoarthritis: Caused by the breakdown of cartilage and bone within the joint, leading to pain, stiffness, and crepitus (grating sounds). This often affects older adults.
- Rheumatoid Arthritis: An autoimmune disease that can affect the TMJ, causing inflammation, pain, and potentially bone erosion.
Other Less Common Types:
- Traumatic TMJ Injury: Fractures, dislocations, or direct blows to the jaw.
- Infection: Although rare, infections can affect the joint.
- Developmental Abnormalities: Congenital issues with jaw development.
- Neoplasia: Tumors, though extremely rare, can affect the TMJ.
Causes / Why It Happens: Unraveling the Roots of TMJ Disorders
Understanding what causes TMJ problems is crucial for effective diagnosis and treatment. TMDs often arise from a combination of factors rather than a single cause.
1. Trauma or Injury
A direct blow to the jaw, head, or neck, a whiplash injury, or even a dental procedure requiring the mouth to be open for extended periods can cause or exacerbate TMD. These injuries can damage the joint, disc, or surrounding muscles.
2. Bruxism (Teeth Grinding and Clenching)
Chronic grinding or clenching of the teeth, especially during sleep (sleep bruxism) or unknowingly during the day, puts immense pressure on the TMJ and surrounding muscles. This can lead to muscle fatigue, inflammation, and eventual damage to the joint structures. Many people are unaware they brux until symptoms appear.
3. Stress and Psychological Factors
Emotional stress, anxiety, and tension can lead to increased muscle activity, including clenching and grinding. Stress can also lower a person's pain threshold, making existing discomfort more pronounced.
4. Arthritis and Degenerative Joint Disease
As mentioned, osteoarthritis can wear down the cartilage within the TMJ, leading to pain and reduced function. Inflammatory conditions like rheumatoid arthritis can also attack the joint, causing inflammation and bone destruction.
5. Malocclusion (Bad Bite)
While historically considered a primary cause, modern research suggests that malocclusion alone is rarely the sole cause of TMD. However, a significant discrepancy in how the upper and lower teeth meet can place uneven stress on the TMJ over time, especially in conjunction with other factors.
6. Connective Tissue Diseases
Conditions like Ehlers-Danlos syndrome, which affect collagen and connective tissues, can lead to joint hypermobility and instability, making the TMJ more susceptible to injury and dysfunction.
7. Hormonal Factors
The higher prevalence of TMDs in women, particularly during reproductive years, suggests a potential hormonal influence, though the exact mechanism is not fully understood. Estrogen receptors are present in the TMJ, and hormonal fluctuations may play a role in pain perception and inflammation.
8. Osteonecrosis of the Jaw (ONJ)
While not a direct cause of typical TMJ dysfunction, osteonecrosis of the jaw (ONJ) is a severe and distinct condition that can lead to jaw pain and dysfunction, sometimes mimicking TMD symptoms or occurring concurrently. ONJ involves the death of bone tissue in the jaw due to a lack of blood supply.
-
Causes of ONJ:
- Bisphosphonate Medications: Most commonly associated with long-term use of bisphosphonates (e.g., for osteoporosis or cancer treatments like multiple myeloma, breast cancer, prostate cancer). This is termed Medication-Related Osteonecrosis of the Jaw (MRONJ).
- Radiation Therapy: High doses of radiation to the head and neck for cancer treatment can damage blood vessels in the jaw, leading to ONJ (Osteoradionecrosis - ORN).
- Trauma: Severe local trauma or infection in the jawbone.
- Systemic Diseases: Rarely, conditions like sickle cell anemia, Gaucher disease, or steroid use can contribute.
-
Connection to TMJ: Patients with ONJ can experience severe jaw pain, swelling, numbness, and limited jaw mobility, symptoms that can overlap with TMD. A TMJ specialist evaluating jaw pain will need to consider ONJ, especially in patients with a history of bisphosphonate use or radiation therapy, as the diagnostic and treatment approaches are vastly different and ONJ requires specialized medical management. It's a critical differential diagnosis for any persistent, severe jaw pain, particularly if accompanied by exposed bone in the mouth.
Signs and Symptoms: What to Look For
TMD symptoms can vary widely in severity and presentation. Recognizing these signs early can help you seek timely intervention.
Common Signs and Symptoms:
- Pain or Tenderness: Often felt in the jaw joint, ears, face, neck, and shoulders. This pain can be dull, aching, or sharp, and may worsen with chewing, speaking, or yawning.
- Clicking, Popping, or Grating Sounds: Audible sounds when opening or closing the mouth. While occasional clicks without pain might not be problematic, persistent, painful, or loud sounds are concerning. A grating sound (crepitus) often indicates degenerative changes.
- Limited Jaw Movement: Difficulty opening the mouth wide, or a feeling that the jaw is "stuck" or "locked" in an open or closed position.
- Fatigue in Jaw Muscles: Feeling tired or sore in the jaw, especially after eating or speaking.
- Headaches: Frequent tension-type headaches, often radiating from the temples or behind the eyes.
- Ear-related Symptoms: Earaches, ringing in the ears (tinnitus), dizziness, or a feeling of fullness in the ear, often mistaken for an ear infection.
- Facial Swelling: Occasional swelling on the affected side of the face.
- Changes in Bite: A sudden change in how your upper and lower teeth fit together, or a feeling that your bite is "off."
- Neck and Shoulder Pain: Referred pain from the jaw muscles can manifest in the neck and shoulders.
Pro Tip: Keep a symptom journal. Note when symptoms occur, their intensity, what makes them better or worse, and any associated activities (e.g., stress, specific foods). This information is invaluable for your TMJ specialist during diagnosis.
Treatment Options: A Spectrum of Solutions
Treatment for TMDs is highly individualized and often involves a multidisciplinary approach, starting with conservative, non-invasive therapies and progressing to more advanced interventions if necessary. The goal is always to reduce pain, restore normal jaw function, and improve quality of life.
1. Conservative Treatments (Most Common First Approach)
These are typically the first line of defense and are highly effective for many patients.
- Pain Management:
- Over-the-counter (OTC) pain relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can reduce pain and inflammation.
- Heat/Cold Therapy: Applying moist heat or cold packs to the jaw area can relieve muscle pain and inflammation.
- Soft Diet: Avoiding hard, chewy, or crunchy foods to rest the jaw muscles.
- Physical Therapy:
- Exercises: Gentle stretching and strengthening exercises to improve jaw mobility and muscle function.
- Massage: Techniques to relax tight jaw muscles.
- Posture Correction: Addressing poor head and neck posture that contributes to jaw strain.
- Ultrasound/TENS: Therapeutic ultrasound or transcutaneous electrical nerve stimulation (TENS) can sometimes be used to alleviate pain.
- Splints or Oral Appliances (Occlusal Guards):
- Stabilization Splints (Mouthguards): Custom-fitted acrylic appliances worn over the upper or lower teeth, primarily at night. They prevent teeth grinding/clenching, distribute bite forces evenly, and help reposition the jaw.
- Repositioning Splints: Designed to temporarily reposition the jaw to a more comfortable position, particularly for disc displacement issues.
- Pros: Non-invasive, reversible, often effective in reducing muscle strain and protecting teeth.
- Cons: Can be uncomfortable initially, requires consistent wear, may need adjustments, doesn't always resolve underlying issues.
- Lifestyle Modifications:
- Stress Management: Techniques like meditation, yoga, or counseling to reduce clenching/grinding due to stress.
- Avoid Extreme Jaw Movements: Limiting wide yawning, singing, or chewing gum.
- Good Posture: Maintaining proper alignment of the head, neck, and shoulders.
- Counseling/Biofeedback: Learning to be aware of and control muscle tension, especially habitual clenching or grinding.
2. Pharmacological Treatments
- Muscle Relaxants: Prescription medications like cyclobenzaprine can relieve muscle spasms and pain, often used short-term.
- Anti-inflammatory Drugs: Prescription-strength NSAIDs for more severe inflammation.
- Tricyclic Antidepressants: Low doses, often taken at bedtime, can help with pain control, muscle relaxation, and improve sleep quality, even in non-depressed individuals.
- Corticosteroids: Oral steroids for short-term inflammation relief, or injections directly into the joint.
3. Minimally Invasive Procedures
If conservative treatments are insufficient, a specialist may consider these options:
- Arthrocentesis: A procedure where two needles are inserted into the joint. Fluid (often saline) is irrigated through the joint to wash out inflammatory byproducts and free up disc adhesions. Sometimes hyaluronic acid (lubricant) is injected.
- Pros: Minimally invasive, relatively quick recovery, can provide significant relief for certain types of TMD.
- Cons: Not a permanent solution for structural issues, potential for infection or nerve damage.
- Corticosteroid Injections: Directly into the joint to reduce inflammation and pain. Effects are temporary.
- Botulinum Toxin (Botox) Injections: Injected into the jaw muscles (e.g., masseter, temporalis) to relax them, reduce clenching/grinding, and alleviate pain. Effects last 3-6 months.
- Pros: Effective for myofascial pain, relatively quick procedure.
- Cons: Temporary, can be costly, potential for temporary facial weakness or asymmetry.

4. Surgical Treatments (Last Resort)
Surgery is generally considered only when conservative and minimally invasive treatments have failed, or when there are severe structural problems within the joint.
- TMJ Arthroscopy: A small incision is made, and a thin, lighted scope (arthroscope) is inserted into the joint. Small surgical instruments can then be used to remove inflamed tissue, wash out the joint, reposition the disc, or remove adhesions.
- Pros: Less invasive than open-joint surgery, shorter recovery.
- Cons: Limited visibility, not suitable for all structural problems.
- Open-Joint Surgery (Arthroplasty): Involves a larger incision in front of the ear to directly access the joint. This allows for more extensive repairs, such as:
- Disc Repair/Repositioning: Repairing tears or repositioning a severely displaced disc.
- Condylectomy: Removal of part of the condyle.
- Eminectomy: Reshaping the bone to prevent locking.
- Pros: Allows for comprehensive repair of complex structural issues.
- Cons: More invasive, longer recovery, higher risks (nerve damage, scarring, infection).
- Total Joint Replacement: In severe cases of joint degeneration or ankylosis (fusion), the entire TMJ may be replaced with an artificial prosthetic joint.
- Pros: Can restore significant function and relieve severe pain in end-stage disease.
- Cons: Major surgery, very high cost, long recovery, potential for long-term complications, revision surgeries may be needed.
Step-by-Step Process: What to Expect During Treatment
Navigating TMJ treatment can feel overwhelming, but understanding the typical process can help ease concerns.
1. Initial Consultation and Diagnosis
- Patient History: The specialist will ask detailed questions about your symptoms, medical history (including any medications like bisphosphonates due to the risk of osteonecrosis of the jaw), dental history, and lifestyle.
- Physical Examination: This involves palpating your jaw muscles, listening for sounds (clicks, pops, crepitus) during jaw movement, checking your range of motion, and assessing your bite.
- Imaging:
- X-rays: Panoramic X-rays show the overall jaw structure.
- CT Scans: Provide detailed images of the bone structure of the joint, useful for identifying degenerative changes or fractures.
- MRI Scans: The gold standard for visualizing the soft tissues, especially the articular disc, and can detect inflammation or displacement. An MRI is crucial for evaluating disc position and soft tissue integrity.
2. Treatment Planning
Based on the diagnosis, your specialist will develop a personalized treatment plan, starting with the least invasive options. This may involve referrals to other specialists (e.g., physical therapist, pain management).
3. Implementation of Conservative Therapies
- Oral Appliance (Splint): If prescribed, impressions of your teeth will be taken to fabricate a custom guard. You'll receive instructions on wear and care, and follow-up appointments for adjustments.
- Physical Therapy: You'll attend sessions with a physical therapist who will guide you through exercises and manual therapies.
- Medication: Your specialist will prescribe appropriate medications and monitor their effectiveness and any side effects.
4. Monitoring and Adjustment
Regular follow-up appointments are essential to assess your progress. Your specialist will make adjustments to your treatment plan as needed, based on symptom improvement or persistence.
5. Progression to Advanced Treatments (If Necessary)
If conservative methods don't provide sufficient relief after a reasonable period (typically 3-6 months), your specialist may discuss minimally invasive procedures (like arthrocentesis or Botox injections) or, as a last resort, surgical options. Each step will involve detailed discussions about risks, benefits, and expected outcomes.
Cost and Insurance: US Price Ranges and Coverage
The cost of TMJ treatment in the US can vary significantly based on the severity of the condition, the type of treatment, the specialist's fees, geographical location, and insurance coverage.
Average US Cost Ranges (Without Insurance):
| Treatment Type | Average Cost Range (USD) | Notes |
|---|---|---|
| Initial Consultation | $150 - $400 | Includes examination and diagnosis. May be covered by medical insurance if the dentist is in-network. |
| Diagnostic Imaging | ||
| - X-rays | $50 - $200 | Panoramic. |
| - CT Scan | $300 - $800 | |
| - MRI Scan | $800 - $3,000+ | Often the most expensive diagnostic tool, but crucial for soft tissue evaluation. Cost varies by facility and whether contrast is used. |
| Oral Appliances | $300 - $1,500 | Custom-made splints or nightguards. Cheaper OTC guards are available but rarely provide adequate long-term solution. |
| Physical Therapy | $75 - $250 per session | Often requires multiple sessions (e.g., 6-12 sessions). A full course could be $450 - $3,000+. |
| Medications | $20 - $200 per month | Depends on the specific drug (NSAIDs, muscle relaxants, antidepressants). |
| Botox Injections | $500 - $1,500 per session | For jaw muscles. Effects last 3-6 months, so multiple sessions per year are often needed. |
| Arthrocentesis | $1,500 - $3,000+ per joint | May vary based on anesthesia type and facility fees. |
| TMJ Arthroscopy | $5,000 - $15,000+ | Depends on the complexity of the procedure and facility. |
| Open-Joint Surgery | $15,000 - $30,000+ | Significant cost due to surgeon's fees, anesthesia, hospital/facility charges. |
| Total Joint Replacement | $30,000 - $50,000+ | Can be significantly higher in complex cases or if custom prosthetics are required. Excludes potential physical therapy and recovery costs. Often considered a life-altering investment. |
Insurance Coverage Details:
This is one of the most confusing aspects of TMD treatment.
- Medical vs. Dental Insurance: Many TMD treatments are considered medical issues rather than purely dental. This is a critical distinction. Medical insurance is more likely to cover diagnosis, physical therapy, medications, injections, and surgical procedures. Dental insurance typically covers things like tooth extractions, fillings, and basic oral care.
- Coding: Ensure your provider uses the correct medical codes (ICD-10 for diagnosis, CPT for procedures) when submitting claims. Mis-coding can lead to denied claims.
- Pre-authorization: Many medical insurance plans require pre-authorization for advanced diagnostic tests (MRI) and surgical procedures. Your specialist's office should assist with this.
- HMOs vs. PPOs: HMO plans may require referrals from your primary care physician to see a specialist, while PPOs offer more flexibility.
- Exclusions: Some insurance policies specifically exclude TMD treatments, or limit coverage for certain appliances or procedures. Always contact your insurance provider directly to understand your specific benefits, deductibles, co-pays, and out-of-pocket maximums for TMD-related care.
- Medicare/Medicaid: Coverage for TMD under Medicare and Medicaid varies. Generally, medically necessary surgical procedures and some diagnostic tests may be covered, but conservative treatments like oral appliances or physical therapy might have limited coverage.
Pro Tip: When evaluating a TMJ specialist near you, ask their office about their billing practices and if they have staff dedicated to navigating insurance claims for TMD.
Recovery and Aftercare: Post-Treatment Guidance
Recovery varies greatly depending on the treatment.
For Conservative Treatments (Splints, PT, Medications):
- Consistency is Key: Wear your oral appliance as directed. Diligently perform prescribed exercises.
- Diet: Continue a soft diet if recommended, especially during flare-ups.
- Pain Management: Use OTC pain relievers or prescribed medications as needed.
- Follow-up: Attend all follow-up appointments for adjustments to appliances or assessment of progress.
For Minimally Invasive Procedures (Arthrocentesis, Injections):
- Immediate Care: You might experience some swelling or soreness at the injection site. Apply ice packs as advised.
- Activity Restriction: Your specialist might recommend avoiding strenuous jaw movements for a few days.
- Rehabilitation: Often followed by a short course of physical therapy to regain full range of motion.
For Surgical Procedures (Arthroscopy, Open-Joint, Replacement):
- Hospital Stay: Varies from outpatient (arthroscopy) to several days (total joint replacement).
- Pain Management: Stronger pain medications will be prescribed.
- Diet: Liquid or soft diet for several weeks to months, progressing slowly back to normal foods.
- Physical Therapy: Crucial for regaining jaw mobility and strength. This is often the longest phase of recovery, potentially lasting several months to a year for complex surgeries.
- Swelling/Bruising: Expect swelling and bruising, especially with open surgery, which will subside over weeks.
- Follow-up: Frequent post-operative appointments to monitor healing and progress.
- Activity Restrictions: Avoid strenuous activity and contact sports for an extended period.
General Aftercare:
- Avoid Clenching/Grinding: Continue stress management techniques and consistent use of nightguards if bruxism is a factor.
- Posture Awareness: Maintain good posture to support overall musculoskeletal health.
- Regular Dental Check-ups: Ensure your general dentist monitors your bite and oral health.
Prevention: How to Avert TMJ Issues
While not all TMDs are preventable (e.g., those due to severe trauma or autoimmune diseases), many cases can be mitigated or prevented by adopting certain habits:
- Manage Stress: Practice stress-reduction techniques like meditation, deep breathing, yoga, or counseling to minimize jaw clenching and grinding.
- Avoid Excessive Jaw Movements: Limit wide yawning, excessive gum chewing, nail biting, and holding a phone between your ear and shoulder.
- Maintain Good Posture: Be mindful of your head, neck, and shoulder alignment, especially when working at a computer or looking at mobile devices. Poor posture can strain jaw muscles.
- Dental Care: Regular dental check-ups can identify early signs of bruxism or bite problems. Your dentist can recommend a nightguard if you grind or clench your teeth.
- Ergonomics: Ensure your workspace is ergonomically sound to prevent neck and shoulder strain that can refer to the jaw.
- Balanced Diet: A diet rich in anti-inflammatory foods may support overall joint health.
- Address Sleep Issues: If you have sleep apnea, treating it can sometimes reduce bruxism and related TMJ strain.
Risks and Complications: What Can Go Wrong
While most TMJ treatments are safe and effective, like any medical intervention, there are potential risks and complications:
From Untreated or Chronic TMD:
- Chronic Pain: Persistent, debilitating pain in the jaw, head, and neck.
- Permanent Jaw Locking: Inability to open or close the mouth due to disc displacement without reduction.
- Joint Degeneration: Progressive wear and tear of the joint, leading to osteoarthritis.
- Malnutrition: Difficulty eating a varied diet due to pain or limited jaw opening.
- Psychological Impact: Depression, anxiety, and reduced quality of life due to chronic pain.
From Treatments:
- Oral Appliances: Initial discomfort, speech difficulties, potential for minor tooth movement if not properly adjusted.
- Injections (Corticosteroid/Botox): Temporary pain or bruising at the injection site, infection (rare), temporary facial weakness or asymmetry (Botox), allergic reaction.
- Arthrocentesis: Swelling, bruising, infection (rare), temporary numbness from local anesthetic, damage to adjacent structures (very rare).
- Surgery (Arthroscopy, Open-Joint, Replacement):
- Infection: A risk with any surgery.
- Nerve Damage: Potential for temporary or permanent damage to facial nerves, leading to numbness, weakness, or paralysis.
- Bleeding/Hematoma: Accumulation of blood under the skin.
- Scarring: More pronounced with open-joint surgery.
- Ankylosis: Fusion of the joint, severely limiting movement (rare).
- Hearing Changes: Temporary or permanent, due to proximity to the ear.
- Failure of Treatment: Symptoms may persist or recur, requiring further intervention.
- Hardware Complications (Joint Replacement): Fracture, loosening, or infection of prosthetic components, requiring revision surgery.
Osteonecrosis of the Jaw (ONJ) as a Distinct Risk:
As discussed under "Causes," while not a direct complication of TMJ surgery itself (unless surgery occurs in an already compromised bony area), it is critical for patients to understand that certain medications, particularly bisphosphonates, can lead to ONJ. If you are on these medications and require any oral surgery (including potentially extensive TMJ surgery or even routine dental extractions), your TMJ specialist and oral surgeon must be fully aware. They will coordinate with your prescribing physician to assess the risk and manage your care appropriately, as ONJ requires very specific and careful management to prevent progression. For patients with ONJ, TMJ-like symptoms might arise from the bone death itself or accompanying infection, and treatment would focus on the ONJ rather than typical TMD protocols.
Comparison Table: Types of TMJ Specialists
Finding the right "TMJ specialist near me" can be confusing as various dental and medical professionals may treat TMDs. Here's a comparison:
| Specialist Type | Primary Focus for TMD | Common Treatments Provided | Key Differentiator |
|---|---|---|---|
| Oral & Maxillofacial Surgeon | Surgical intervention for complex TMD, trauma, or joint pathology. | Arthroscopy, open-joint surgery, total joint replacement, biopsies. | Highly trained in surgical management of the jaw and facial structures. Best for structural issues requiring surgery. |
| Prosthodontist | Restoring oral function through prosthetic devices and bite correction. | Occlusal splints, full mouth reconstruction, orthodontic coordination. | Expertise in bite relationships, prosthetics, and non-surgical management of TMD related to occlusion. |
| Orthodontist | Correcting malocclusion and jaw alignment. | Braces, aligners, sometimes used in conjunction with splints. | Focuses on teeth and jaw alignment. May treat TMD related to bite, but less on pain management directly. Not all orthodontists specialize in TMD. |
| Pain Management Specialist | Managing chronic pain conditions, often in a multidisciplinary team. | Injections (steroids, Botox), nerve blocks, medication management. | Specialized in pain pathways and pharmacological/interventional pain relief. Often works with TMJ patients for symptom management. |
| Physical Therapist | Rehabilitating musculoskeletal function and reducing muscle pain. | Jaw exercises, manual therapy, posture correction, modalities (ultrasound). | Non-invasive approach focusing on muscle function, mobility, and posture. Crucial for recovery and long-term management. |
| General Dentist | Initial diagnosis, conservative management, referrals. | Basic oral appliance (nightguard), simple pain management, referrals. | Often the first point of contact. Can manage mild cases but typically refers complex TMD to specialists. |
| Neurologist | Diagnosing and treating neurological conditions impacting facial pain. | Medication for neuropathic pain, Botox for chronic migraines. | May be consulted if TMD symptoms overlap with neuropathic pain conditions (e.g., trigeminal neuralgia) or severe headaches not resolved by other means. |
| Rheumatologist | Diagnosing and treating autoimmune or inflammatory joint diseases. | Medication for systemic inflammatory conditions (e.g., rheumatoid arthritis). | Consulted if an autoimmune condition (like rheumatoid arthritis) is suspected to be causing or contributing to the TMJ inflammation and degeneration. |
Children / Pediatric Considerations
TMJ disorders are less common in children but can occur. Pediatric TMD symptoms might be subtle or manifest differently than in adults.

Common Signs in Children:
- Clicking or Popping: Parents might notice sounds during chewing or yawning.
- Limited Opening: Difficulty opening the mouth wide, sometimes impacting eating.
- Headaches: Often misdiagnosed as tension headaches without considering jaw involvement.
- Facial Pain: General discomfort around the jaw or ears.
- Behavioral Changes: Irritability or changes in eating habits due to discomfort.
Causes in Children:
- Trauma: Falls, sports injuries, or dental procedures.
- Bruxism: Teeth grinding, especially at night, which is common in children but can become problematic if persistent and painful.
- Orthodontic Issues: Severe malocclusion, though rarely the sole cause.
- Juvenile Idiopathic Arthritis: An autoimmune condition that can affect the TMJ in children.
Treatment for Children:
- Conservative First: Similar to adults, treatment starts with conservative approaches.
- Soft Diet: Temporary dietary modifications.
- Physical Therapy: Gentle exercises and stretches.
- Oral Appliances: Custom nightguards to protect teeth from bruxism and help position the jaw. These must be frequently adjusted as the child grows.
- Stress Management: Helping children manage stress can reduce clenching.
- Close Monitoring: Specialists carefully monitor growth and development to ensure any intervention doesn't negatively impact jaw growth. Surgery is extremely rare and only considered in severe cases after all other options have been exhausted.
Parents concerned about their child's jaw health should consult a pediatric dentist or a TMJ specialist who has experience treating younger patients.
Cost Breakdown: Navigating TMJ Treatment Expenses
Understanding the potential costs is essential for planning your TMJ treatment. Here’s a more granular look:
| Service/Treatment | Low Range (USD) | Mid Range (USD) | High Range (USD) | Notes |
|---|---|---|---|---|
| Initial Exam & Diagnosis | $150 | $250 | $400 | Excludes advanced imaging. |
| X-rays (Panoramic) | $50 | $100 | $200 | Usually covered by dental insurance. |
| MRI of TMJ | $800 | $1,500 | $3,000 | Can vary significantly by location (urban vs. rural) and facility type. Often covered by medical insurance if deemed medically necessary. |
| Custom Oral Splint/Nightguard | $300 | $750 | $1,500 | Laboratory fees and specialist's expertise play a role. OTC options are cheaper but not recommended for clinical TMD. |
| Physical Therapy (per session) | $75 | $120 | $250 | Many require 6-12 sessions. Total cost can be $450 - $3,000+. Medical insurance often covers a portion. |
| Botox Injections (per session) | $500 | $1,000 | $1,500 | Cost depends on units used and provider's fee. Effects last 3-6 months. |
| Arthrocentesis (per joint) | $1,500 | $2,500 | $3,000+ | Includes facility fees, anesthesia. Often covered by medical insurance. |
| TMJ Arthroscopy | $5,000 | $10,000 | $15,000+ | Surgeon's fee, anesthesia, operating room costs. |
| Open-Joint Surgery | $15,000 | $22,000 | $30,000+ | More complex, higher hospital and anesthesia costs. |
| Total Joint Replacement | $30,000 | $40,000 | $50,000+ | Includes the cost of the prosthetic joint, extensive surgery, and post-operative care. Often covered by medical insurance for severe cases. |
With vs. Without Insurance:
- Without Insurance: You are responsible for the full cost. Negotiate cash payment discounts with providers.
- With Insurance (Medical):
- Deductible: The amount you must pay out-of-pocket before your insurance starts to cover costs.
- Co-pay: A fixed amount you pay for each visit or service after your deductible is met.
- Co-insurance: A percentage of the cost you pay for services after your deductible is met (e.g., insurance pays 80%, you pay 20%).
- Out-of-Pocket Maximum: The most you will pay for covered services in a plan year. Once reached, insurance typically covers 100% of remaining costs.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many specialists offer interest-free payment plans for a portion of the cost.
- Medical Credit Cards: Companies like CareCredit offer special financing options for healthcare expenses, often with interest-free periods if paid in full within a certain timeframe.
- Personal Loans: Banks or credit unions offer personal loans, but these come with interest rates.
Cost-Saving Tips:
- Verify Insurance Coverage: Call your medical insurance provider directly and ask specific questions about TMD coverage, CPT codes, and pre-authorization requirements.
- Get Multiple Opinions: For complex or expensive treatments, getting a second opinion can confirm the diagnosis and treatment plan.
- Negotiate Cash Prices: If uninsured, ask for a discount for paying in cash or upfront.
- University Dental Schools: These often offer high-quality care at a reduced cost, as procedures are performed by students under expert supervision.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): Use pre-tax dollars for qualified medical expenses, including TMJ treatment.
Frequently Asked Questions
What kind of doctor is a TMJ specialist?
A TMJ specialist isn't a single type of doctor but rather a dental or medical professional with advanced training and experience in diagnosing and treating temporomandibular disorders. This can include oral and maxillofacial surgeons, prosthodontists, orthodontists with a TMD focus, or pain management specialists. Your general dentist can often make an initial assessment and refer you to the most appropriate specialist based on your symptoms.
How long does it take to treat TMJ?
The duration of TMJ treatment varies greatly depending on the severity of the disorder and the type of treatment. Conservative therapies like splint use or physical therapy might show improvement within weeks to a few months. More complex issues requiring injections or surgery will involve longer recovery periods, potentially spanning several months to a year, including post-operative physical rehabilitation.
Is TMJ curable or just manageable?
For many people, TMJ disorders are manageable, with symptoms significantly improving or resolving with conservative treatments. For some, especially those with severe structural damage, the condition might require ongoing management rather than a complete "cure." The goal is always to achieve long-term pain relief and restore optimal jaw function, often through a combination of therapies.
What are the most effective home remedies for TMJ pain?
Effective home remedies include applying moist heat or cold packs to the jaw, eating soft foods, avoiding extreme jaw movements (like wide yawning or gum chewing), performing gentle jaw stretches recommended by a professional, and practicing stress-reduction techniques to minimize clenching. OTC pain relievers like ibuprofen can also help manage acute pain and inflammation.
Is TMJ pain a sign of something more serious?
While most TMJ pain is not life-threatening, persistent or severe jaw pain, especially if accompanied by swelling, numbness, or difficulty opening your mouth, warrants professional evaluation. It's crucial to rule out other conditions, such as infections, nerve issues (like trigeminal neuralgia), or in rare cases, even osteonecrosis of the jaw, which require distinct medical attention.
How much does an MRI for TMJ cost with insurance?
With medical insurance, the cost of an MRI for TMJ can range from a few hundred dollars to over $1,000, depending on your deductible, co-insurance, and the specific facility. You'll typically pay your deductible first, then a co-insurance percentage. It's vital to get pre-authorization from your insurance company to ensure coverage and avoid unexpected out-of-pocket expenses.
Can TMJ cause ear pain and ringing?
Yes, TMJ disorders are a common cause of ear-related symptoms, including earaches (otalgia), ringing in the ears (tinnitus), a feeling of fullness in the ear, and even dizziness or vertigo. This is because the TMJ is located very close to the ear canal, and the nerves and muscles involved in jaw function also influence the ear region, leading to referred pain and dysfunction.
What is the role of physical therapy in TMJ treatment?
Physical therapy plays a crucial role in managing TMJ disorders by improving jaw mobility, reducing muscle tension, strengthening supporting muscles, and correcting posture. A physical therapist will use techniques like manual therapy, therapeutic exercises, and modalities (e.g., ultrasound) to alleviate pain and restore normal function, often in conjunction with other treatments.
Can orthodontics fix TMJ?
Orthodontics can help resolve TMJ symptoms in some cases, particularly when a significant malocclusion (bad bite) is a contributing factor to jaw strain. However, orthodontics alone is not a universal cure for all TMJ disorders. It's often used as part of a broader treatment plan and should be pursued under the guidance of a TMJ-focused orthodontist or in consultation with an oral surgeon.
What foods should I avoid with TMJ?
To reduce strain on your jaw, it's advisable to avoid hard, chewy, or crunchy foods like tough meats, crusty bread, nuts, hard candies, and sticky foods like caramel. Also, avoid chewing gum. Opt for softer foods such as soups, mashed potatoes, yogurt, smoothies, cooked vegetables, and tender meats cut into small pieces.
When to See a Dentist
It's important to know when your jaw pain or discomfort warrants a visit to a professional.
Clear Warning Signs for a Scheduled Appointment:
- Persistent Jaw Pain: If your jaw pain, tenderness, or aching around the ear or face lasts for more than a few days and doesn't improve with simple home care.
- Chronic Headaches/Earaches: If you experience frequent headaches or ear pain that isn't explained by other conditions and might be linked to jaw function.
- Clicking, Popping, or Grating Sounds with Pain: While occasional clicking without pain might be benign, if these sounds are accompanied by pain or discomfort, it's a sign to seek evaluation.
- Difficulty Chewing or Swallowing: If eating has become consistently uncomfortable or painful.
- Limited Jaw Movement: If you find it hard to open your mouth wide, or your jaw feels stiff in the morning.
- Changes in Your Bite: If you notice a sudden shift in how your teeth fit together.
Red Flags for More Immediate Attention (Consider an Urgent Appointment):
- Jaw Locking: If your jaw locks in an open or closed position, making it impossible to move your mouth. This can be a sign of disc displacement without reduction.
- Severe, Acute Pain: If you experience sudden, excruciating jaw pain that incapacitates you.
- Swelling and Fever: If jaw pain is accompanied by significant facial swelling, redness, and fever, it could indicate an infection or a more serious inflammatory process.
- Numbness or Tingling: If you experience unexplained numbness, tingling, or weakness in your jaw or face, which could suggest nerve involvement or other underlying issues.
- Exposed Bone in the Jaw: Particularly if you have a history of bisphosphonate use or radiation therapy, the presence of exposed bone or non-healing ulcers in the jaw area could indicate osteonecrosis of the jaw (ONJ) and requires urgent evaluation.
Don't wait for your symptoms to become debilitating. Early diagnosis and intervention by a qualified professional can significantly improve outcomes and prevent the progression of TMJ disorders. If you're searching for a tmj specialist near me, SmilePedia.net encourages you to take that step towards better jaw health and overall well-being.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026