Root Canal Treatment Side Effects: Complete Guide
Key Takeaways
- Few dental procedures evoke as much apprehension as the root canal. For many, the very mention of "root canal" conjures images of intense pain and discomfort. However, modern dentistry has transformed this vital procedure into a highly effective and often pain-free way to save a damaged tooth. While
Root Canal Treatment Side Effects: Complete Guide
Few dental procedures evoke as much apprehension as the root canal. For many, the very mention of "root canal" conjures images of intense pain and discomfort. However, modern dentistry has transformed this vital procedure into a highly effective and often pain-free way to save a damaged tooth. While the fear of pain during the procedure is largely outdated, it's natural to wonder about potential root canal treatment side effects and what to expect during and after the process. Understanding these potential outcomes, both common and rare, is crucial for anyone considering or undergoing this restorative treatment.
This comprehensive guide from SmilePedia.net aims to demystify root canal treatment, shedding light on why it's performed, what the process entails, and critically, the full spectrum of potential side effects. We'll delve into everything from the mild, temporary discomfort you might experience to rarer complications, offering clear, medically accurate information to help you feel informed and prepared. By the end, you'll have a complete picture, empowering you to make the best decisions for your oral health.
Key Takeaways:
- Root canal treatment is a highly successful procedure (over 95% success rate) designed to save a natural tooth from extraction.
- Post-treatment discomfort is common but usually mild, manageable with over-the-counter pain relievers, and resolves within a few days.
- Serious root canal treatment side effects like persistent infection or nerve damage are rare but require immediate dental attention.
- The average cost for a root canal in the US ranges from $700 to $2,000 for front teeth and $1,000 to $2,500 for molars, often covered partially by dental insurance.
- Recovery typically involves 1-3 days of mild soreness, with full recovery taking up to a week.
- Maintaining good oral hygiene and regular dental check-ups are key to preventing the need for future root canal treatments.
- Modern root canal procedures are performed under local anesthesia, making them no more painful than a standard filling.
What Is a Root Canal Procedure: Overview
A root canal is an endodontic procedure designed to treat infection or inflammation in the dental pulp, the soft tissue inside your tooth. The pulp contains nerves, blood vessels, and connective tissue, extending from the crown of your tooth down to the root tips. When this pulp becomes infected or irreversibly damaged, it can cause significant pain and, if left untreated, lead to a severe abscess, bone loss, and eventually tooth loss.
The core objective of a root canal procedure is to remove the infected or inflamed pulp, thoroughly clean and disinfect the inside of the tooth, and then fill and seal the space. This process eliminates the infection and prevents its spread, while preserving the natural tooth structure. Preserving your natural tooth is always the preferred option over extraction, as it maintains your bite, prevents adjacent teeth from shifting, and avoids the need for more complex and costly restorative options like dental implants or bridges.
![Cross-section diagram of a tooth showing infected pulp, with arrows indicating the steps of a root canal: access, cleaning, shaping, filling(/restorative-dentistry/5-tooth-bridge-complete-guide), and crown placement.]
Types and Variations of Root Canal Treatment
While the fundamental principles remain the same, there are a few variations of root canal treatment depending on the tooth's condition and location.
Standard Root Canal Treatment (RCT)
This is the most common type, performed on a tooth with infected or damaged pulp. It involves accessing the pulp chamber, cleaning out the canals, shaping them, and then filling them with a biocompatible material (gutta-percha) before sealing the tooth. A dental crown is almost always placed afterward to protect the weakened tooth.
Endodontic Retreatment
Sometimes, a tooth that has already undergone a root canal can become re-infected or fail to heal properly. This can happen years after the initial procedure if new decay develops, a crown becomes loose, or if the original treatment missed a canal or didn't adequately seal the tooth. During retreatment, the previous filling material is removed, the canals are re-cleaned, re-shaped, and re-filled. This process is often more complex than the initial root canal.
Apicoectomy (Root-End Resection)
If an infection persists or redevelops at the very tip of the tooth's root after a standard root canal, an apicoectomy may be recommended. This surgical procedure involves making an incision in the gum tissue to expose the bone and the infected root tip. The very end of the root tip is then removed along with any surrounding infected tissue. A small filling is placed to seal the end of the root canal. This is typically performed by an endodontist, a dental specialist in root canal treatment.
Pulpotomy and Pulpectomy (Pediatric Considerations)
For children, especially in primary (baby) teeth, variations like pulpotomy and pulpectomy are common. These procedures aim to save the baby tooth until it's naturally ready to fall out, preserving space for permanent teeth. (More details in the Pediatric Considerations section).
Causes: Why a Root Canal Might Be Needed
A root canal becomes necessary when the dental pulp, the living tissue inside your tooth, becomes infected or irreversibly inflamed. Several factors can lead to this condition:
- Deep Dental Decay: This is the most common cause. When a cavity is left untreated, bacteria erode the enamel and dentin, eventually reaching the pulp chamber. Once bacteria enter the pulp, they cause inflammation (pulpitis) and infection.
- Trauma to the Tooth: A severe blow or injury to a tooth can damage the pulp, even if there's no visible crack or chip. The trauma can disrupt the blood supply to the pulp, causing it to die and become infected over time.
- Cracked or Chipped Tooth: Cracks or chips that extend into the pulp can create an entry point for bacteria, leading to infection. Even seemingly minor cracks can propagate under chewing pressure.
- Repeated Dental Procedures: Multiple fillings or extensive dental work on the same tooth can sometimes irritate the pulp, leading to inflammation that may eventually become irreversible.
- Large Fillings: Over time, large fillings can sometimes fail, allowing bacteria to seep underneath and infect the pulp.
- Periodontal Disease: In advanced cases, severe gum disease can expose the root tips and allow bacteria to enter the pulp from the outside, though this is less common.
Signs and Symptoms Indicating a Need for a Root Canal
Recognizing the signs and symptoms of pulp infection is crucial for seeking timely treatment and preventing further complications. The symptoms can vary in intensity and may include:
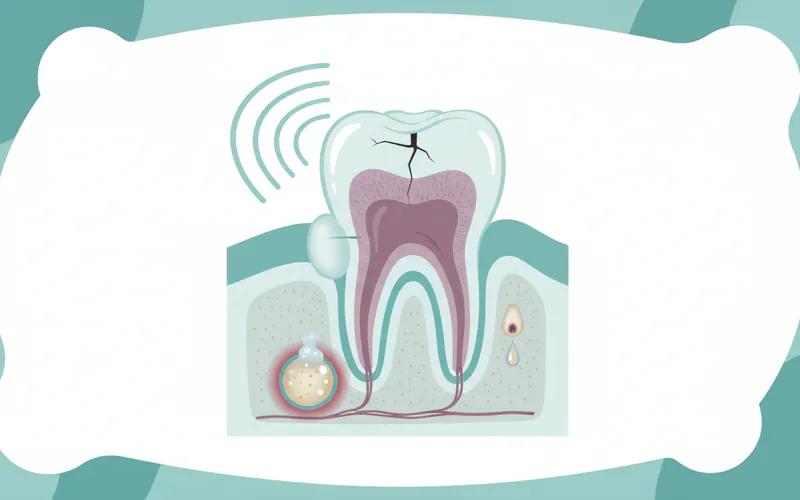
- Persistent Pain: This is the most common symptom. The pain can range from mild to severe and may be constant or intermittent. It might worsen when chewing or applying pressure to the tooth.
- Sensitivity to Hot and Cold: Lingering sensitivity to hot or cold temperatures, even after the stimulus is removed, is a strong indicator of pulp damage. If the sensitivity persists for more than a few seconds, it often means the pulp is irreversibly inflamed.
- Swelling and Tenderness in the Gums: The area around the affected tooth may become swollen, tender, or inflamed due to infection spreading from the pulp.
- Pimple-like Bump on the Gums (Fistula): An abscess can form at the root tip, leading to a small bump or "pimple" on the gums. This is a sign of pus draining from the infection.
- Darkening or Discoloration of the Tooth: A tooth may become darker or grayish if the pulp has died, as the internal tissues break down.
- Pain When Chewing or Touching the Tooth: The infection can cause inflammation of the ligaments surrounding the tooth, making it painful to bite down or even touch.
- Loose Tooth: In advanced stages of infection, the tooth may become slightly loose due to bone loss around the root.
It's important to note that sometimes, a tooth requiring a root canal may show no symptoms at all, or only very mild ones. This is why regular dental check-ups are vital, as your dentist can identify issues with X-rays before they become symptomatic.
Treatment Options: Root Canal vs. Extraction
When faced with a severely infected or damaged tooth, the primary treatment options are a root canal or tooth extraction.
Root Canal Treatment (RCT)
Pros:
- Preserves Natural Tooth: The biggest advantage is saving your own tooth, maintaining your natural bite and smile.
- Prevents Shifting of Adjacent Teeth: An extracted tooth can lead to adjacent teeth drifting out of alignment, causing bite problems and potential TMD issues.
- Avoids More Complex Procedures: Eliminates the need for a dental implant or bridge, which are typically more invasive and costly.
- High Success Rate: Modern root canals have a success rate exceeding 95% when performed correctly.
Cons:
- Cost: Can be more expensive than a simple extraction, especially with the added cost of a dental crown.
- Time: Requires at least one, often two or more, dental appointments.
- Potential for Complications: Though rare, complications can occur (discussed in the "Risks and Complications" section).
- Requires Crown: Almost always necessitates a dental crown afterward, which adds to the cost and treatment time.
Tooth Extraction
Pros:
- Immediate Pain Relief: Removes the source of infection and pain relatively quickly.
- Lower Initial Cost: A simple extraction is generally less expensive than a root canal.
Cons:
- Loss of Natural Tooth: Requires replacement to maintain oral health and aesthetics.
- Bone Loss: The jawbone supporting the missing tooth will begin to resorb (shrink) over time.
- Shifting Teeth: Adjacent teeth can drift into the gap, causing bite issues and affecting chewing efficiency.
- Need for Replacement: Requires a dental implant, bridge, or partial denture to fill the gap, incurring additional costs and procedures. These replacement options can be significantly more expensive and invasive than a root canal.
Comparison Table: Root Canal vs. Extraction
| Feature | Root Canal Treatment | Tooth Extraction |
|---|---|---|
| Primary Goal | Save the natural tooth | Remove the infected/damaged tooth |
| Cost (Initial) | Moderate to high (incl. crown) | Low to moderate (simple extraction) |
| Cost (Total) | Often lower than extraction + replacement | Higher if replaced with implant/bridge |
| Procedure Time | 1-2 appointments, 60-90 min each | 1 appointment, 30-60 min |
| Recovery | Mild soreness 1-3 days, full recovery ~1 week | Mild soreness 1-5 days, longer if surgical |
| Preserves Tooth? | Yes | No |
| Bone Loss? | No | Yes, over time in the extraction site |
| Impact on Bite? | Maintains natural bite | Can alter bite if not replaced |
| Aesthetics | Maintains natural smile (with crown) | Gap in smile (unless replaced) |
| Long-term | Tooth can last a lifetime with proper care | Requires costly and invasive replacement |
Step-by-Step Process: What to Expect During Treatment
Understanding the root canal procedure can significantly alleviate anxiety. Here's a typical step-by-step breakdown:
-
Diagnosis and Anesthesia:
- Your dentist or endodontist will thoroughly examine your tooth, take X-rays, and conduct diagnostic tests to confirm the need for a root canal.
- Local anesthesia is administered to numb the affected tooth and surrounding gum tissue. This ensures you feel no pain during the procedure.
- Pro Tip: If you have dental anxiety, discuss sedation options (e.g., nitrous oxide, oral conscious sedation) with your dentist beforehand.
-
Isolation of the Tooth:
- A small sheet of rubber, called a dental dam, is placed around the tooth. This isolates the tooth, keeping it dry and clean from saliva and preventing bacteria from entering during the procedure. It also protects you from swallowing any debris.
-
Access Opening:
- A small opening is created in the crown of the tooth, usually on the chewing surface of molars or the back surface of front teeth, to gain access to the pulp chamber and root canals.
-
Pulp Removal and Cleaning:
- Tiny dental instruments, called files, are used to remove the infected or inflamed pulp tissue from the pulp chamber and root canals.
- The canals are then meticulously cleaned and shaped to prepare them for filling. The endodontist also uses antibacterial solutions (like sodium hypochlorite) to disinfect the canals, washing away bacteria and debris. This is a critical step to prevent future infection.
-
Filling the Canals (Obturation):
- Once the canals are thoroughly cleaned and shaped, they are filled with a biocompatible, rubber-like material called gutta-percha. This material is inserted along with an adhesive sealer to completely fill and seal the canals, preventing re-entry of bacteria.
-
Temporary Filling/Restoration:
- After the canals are sealed, the access opening in the tooth's crown is sealed with a temporary filling.
- In some cases, if there's extensive infection, the dentist might place a temporary filling and schedule a second appointment to ensure the infection has cleared before placing a permanent filling and crown.
-
Placement of Permanent Restoration (Dental Crown):
- After a few days or weeks, typically once the tooth has settled, a permanent restoration is placed. This is almost always a dental crown. A crown covers the entire biting surface of the tooth, providing strength and protection to the treated tooth, which can become brittle after a root canal.
- Your dentist will prepare the tooth, take impressions, and fit a custom-made crown.
- Pro Tip: Do not delay the placement of your permanent crown. A temporary filling is not strong enough to withstand chewing forces long-term, and delaying the crown significantly increases the risk of tooth fracture or re-infection.
Cost and Insurance: US Price Ranges
The cost of a root canal in the United States can vary significantly based on several factors, including the type of tooth, the complexity of the case, the dentist's or endodontist's fees, and geographic location.
Average US Costs (Without Insurance):
- Front Tooth (Incisors/Canines): Generally the least expensive due to having 1-2 canals. Average cost ranges from $700 to $1,500.
- Premolar (Bicuspid): Typically has 1-2 canals. Average cost ranges from $800 to $1,800.
- Molar: The most expensive due to having 3-4 or more canals and being more difficult to access. Average cost ranges from $1,000 to $2,500.
- Endodontic Retreatment: Can be 10-25% more expensive than an initial root canal due to the added complexity of removing previous filling material.
- Apicoectomy: A surgical procedure, often ranging from $900 to $2,000.
Note: These prices do not include the cost of the dental crown, which is essential after a root canal and can add an additional $800 to $2,500 per tooth, depending on the material and lab fees.
Cost with Insurance Coverage:
Most dental insurance plans provide some coverage for root canal treatment, as it is considered a major restorative procedure.
- Typical Coverage: Insurance often covers 50% to 80% of the root canal procedure after your deductible is met.
- Deductibles: You will typically need to pay an annual deductible (e.g., $50-$100) before your insurance starts covering costs.
- Annual Maximums: Most plans have an annual maximum benefit (e.g., $1,000-$2,000). If your root canal and crown exceed this, you'll pay the difference.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) for major procedures like root canals.
Pro Tip: Always contact your dental insurance provider directly or have your dental office submit a pre-treatment estimate ("pre-auth") to understand your specific coverage, out-of-pocket costs, and any limitations before proceeding with treatment.
Cost Comparison Table: Root Canal Procedure (US Averages)
| Tooth Type | General Dentist (Range) | Endodontist (Range) | With Insurance (50% Coverage Example) |
|---|---|---|---|
| Front Tooth | $700 - $1,200 | $900 - $1,500 | $350 - $750 |
| Premolar | $800 - $1,500 | $1,000 - $1,800 | $400 - $900 |
| Molar | $1,000 - $2,000 | $1,200 - $2,500 | $500 - $1,250 |
| Dental Crown | $800 - $2,500 (additional cost) | $800 - $2,500 (additional cost) | $400 - $1,250 |
| Total (Molar + Crown) | $1,800 - $4,500 (approx.) | $2,000 - $5,000 (approx.) | $900 - $2,500 (approx.) |
Note: These are average ranges. Actual costs may vary.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer flexible payment plans, allowing you to pay for treatment in installments.
- Dental Credit Cards: Options like CareCredit offer special financing for healthcare expenses, often with interest-free periods if paid in full within a certain timeframe.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer, you can use these tax-advantaged accounts to pay for dental treatment.
Recovery and Aftercare
Proper aftercare is crucial for a smooth recovery and the long-term success of your root canal treatment.
Immediate Post-Procedure:
- Numbness: The local anesthetic will wear off in a few hours. Avoid chewing on the treated side until the numbness completely subsides to prevent accidental biting of your tongue, cheek, or lip.
- Mild Discomfort: It's common to experience mild to moderate soreness, sensitivity, or tenderness in the treated tooth and surrounding gum tissue for a few days. This is often due to inflammation from the cleaning process.
- Pain Management:
- Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage discomfort.
- Your dentist may prescribe stronger pain medication if necessary, though this is less common.
- Apply a cold compress to the outside of your cheek if you experience swelling, for 15-20 minutes at a time.
Dietary Guidelines:
- Soft Foods: Stick to soft foods for the first few days. Examples include yogurt, soup, mashed potatoes, scrambled eggs, and smoothies.
- Avoid Chewing on the Treated Tooth: Especially if you only have a temporary filling, avoid chewing hard, sticky, or crunchy foods on the treated side until your permanent crown is placed. This prevents damage to the temporary filling or fracture of the tooth.
Oral Hygiene:
- Continue Brushing and Flossing: Maintain your regular oral hygiene routine, brushing and flossing gently around the treated tooth.
- Rinsing: Rinsing with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) several times a day can help reduce inflammation and keep the area clean.
Follow-Up Appointments:
- Permanent Restoration: Your most important follow-up is to get your permanent dental crown placed. Do not skip or delay this appointment.
- Regular Check-ups: Continue with your routine dental check-ups every six months. Your dentist will monitor the treated tooth with X-rays to ensure complete healing.
Pro Tip: If you experience severe pain that doesn't subside with medication, significant swelling that worsens, or an allergic reaction, contact your dentist or endodontist immediately.
Prevention: How to Avoid Needing a Root Canal
The best treatment for a root canal is preventing the need for one altogether. Here's how you can reduce your risk:
- Practice Excellent Oral Hygiene:
- Brush your teeth at least twice a day with fluoride toothpaste for two minutes each time.
- Floss daily to remove plaque and food particles from between teeth and under the gumline.
- Use an antimicrobial mouthwash to further reduce bacteria.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every six months for professional cleanings and examinations. Early detection of cavities or cracks can prevent them from reaching the pulp.
- Limit Sugary and Acidic Foods/Drinks:
- Reduce your consumption of sugary snacks, sodas, and acidic beverages, which contribute to tooth decay.
- Wear a Mouthguard:
- If you play contact sports, wear a custom-fitted mouthguard to protect your teeth from trauma that could lead to pulp damage.
- If you grind or clench your teeth (bruxism), wear a nightguard to prevent tooth wear and cracks.
- Prompt Treatment of Dental Issues:
- Don't ignore tooth sensitivity or minor pain. Address cavities or chips promptly before they worsen and involve the pulp.
Risks and Complications: Root Canal Treatment Side Effects
While root canal treatment has a very high success rate, like any medical procedure, it carries potential risks and complications. Understanding these root canal treatment side effects can help you be prepared and know when to seek further professional advice.
Common, Mild Side Effects (Usually Temporary):
- Post-Treatment Pain and Sensitivity:
- Description: This is the most common side effect. After the anesthesia wears off, you may experience mild to moderate pain, aching, or tenderness in the treated tooth and surrounding gums. The tooth might also be sensitive to pressure or biting.
- Cause: This pain is primarily due to inflammation in the tissues surrounding the tooth root as they heal from the cleaning and shaping process. It's not usually a sign of ongoing infection.
- Management: Typically managed effectively with over-the-counter pain relievers (ibuprofen, acetaminophen). It usually subsides within a few days to a week.
- Swelling:
- Description: Minor swelling of the gums or cheek near the treated tooth can occur.
- Cause: Inflammatory response to the procedure.
- Management: Cold compresses can help reduce swelling. It generally resolves within 1-3 days.
- Jaw Soreness:
- Description: Your jaw may feel sore or stiff from keeping your mouth open for an extended period during the procedure.
- Management: Jaw exercises, warm compresses, and over-the-counter pain relievers can alleviate discomfort.
Uncommon, More Serious Complications (Requires Further Intervention):
- Persistent Infection or Re-infection:
- Description: Despite meticulous cleaning, bacteria can sometimes remain or re-enter the tooth, leading to persistent symptoms or a new infection. This is the most common reason for root canal failure.
- Causes:
- Missed Canals: Some teeth, especially molars, have complex root canal anatomy with extra canals that might be very narrow or difficult to locate and clean, leading to residual infection.
- Incomplete Cleaning: If all bacteria or infected tissue aren't removed, the infection can linger.
- New Decay/Restoration Failure: If the final crown or filling leaks or new decay forms, bacteria can re-enter the tooth.
- Root Fracture: An undetected crack in the root can allow bacteria to seep in, leading to re-infection.
- Signs: Lingering pain, swelling, sensitivity to hot/cold, or the development of a "pimple" on the gum.
- Management: Often requires endodontic retreatment or an apicoectomy. In severe cases, extraction might be necessary.
- Root Fracture:
- Description: A treated tooth can become brittle over time and is more susceptible to fracture, especially if a permanent crown is delayed or not placed. Fractures can be vertical (extending down the root) or horizontal.
- Causes: Weakened tooth structure, chewing on hard foods, trauma, or insufficient support from the final restoration.
- Signs: Pain when biting, sensitivity to cold, or a "cracked tooth syndrome" sensation.
- Management: Depending on the severity and location of the fracture, treatment options range from bonding to extraction. Vertical root fractures often lead to extraction.
- Discoloration of the Treated Tooth:
- Description: The treated tooth may appear darker or grayish over time.
- Causes: This can occur due to residual blood products within the dentin tubules or the filling material itself.
- Management: Internal tooth bleaching (walking bleach technique) or placing a porcelain veneer or crown can restore the tooth's natural appearance.
- Allergic Reaction:
- Description: Though rare, some individuals may have an allergic reaction to materials used during the procedure, such as latex in the dental dam, antibiotics, or the gutta-percha filling material.
- Signs: Rash, itching, swelling, or difficulty breathing.
- Management: Immediate medical attention is required.
- Nerve Damage:
- Description: Extremely rare, but possible during lower molar root canals due to the proximity of the inferior alveolar nerve (which provides sensation to the lower lip and chin) or the lingual nerve (which provides sensation to the tongue). Damage can result in numbness, tingling, or altered sensation.
- Cause: Direct trauma from instruments or chemical irritation.
- Management: Often temporary and resolves over weeks or months. In some cases, it can be permanent.
- Perforation of the Root or Pulp Chamber:
- Description: During the cleaning and shaping process, a dental instrument can accidentally create a small hole (perforation) in the side of the tooth root or pulp chamber.
- Causes: Complex root anatomy, calcified canals, or operator error.
- Management: Small perforations can often be sealed with a biocompatible material (like MTA). Larger perforations can compromise the tooth's long-term prognosis and may lead to extraction.
- Instrument Separation:
- Description: A small dental file can sometimes break off inside the root canal.
- Causes: Complex canal anatomy, overuse of instruments, or operator error.
- Management: Often, the separated fragment can be retrieved or bypassed. If it cannot be removed, and the canal is well-cleaned beyond the fragment, the tooth may still heal successfully. If the fragment blocks access to an infected area, an apicoectomy or retreatment may be necessary.
- Overfill or Underfill of Root Canals:
- Description: The gutta-percha filling material might extend slightly beyond the root tip (overfill) or not completely fill the canal (underfill).
- Cause: Difficulty in accurately determining root canal length.
- Management: Small overfills are often asymptomatic and don't require intervention. Significant underfills can leave space for bacteria to thrive, potentially requiring retreatment.
Pro Tip: Choosing an experienced endodontist for complex cases, especially molars or retreatments, can significantly reduce the risk of these more serious complications. Endodontists have specialized training, equipment (like operating microscopes), and expertise in managing challenging root canal anatomies.
Children / Pediatric Considerations
Root canal treatment is not just for adults. Children can also require similar procedures to save infected primary (baby) teeth. The goal in pediatric endodontics is to preserve the primary tooth until it naturally exfoliates, maintaining space for the permanent tooth and ensuring proper chewing and speech development.
Pulpotomy ("Baby Root Canal"):
- Description: This procedure involves removing only the infected part of the pulp tissue located in the crown of the tooth, leaving the healthy pulp in the root canals intact.
- When It's Used: Typically performed when decay has reached the pulp but the infection is limited to the coronal (crown) portion of the pulp and has not spread into the root canals.
- Process: The infected pulp is removed, and a medicated material is placed over the remaining healthy pulp to promote healing and protect it. The tooth is then sealed and usually covered with a stainless steel crown.
Pulpectomy:
- Description: A more extensive procedure similar to a full root canal in adults, where all of the pulp tissue (both in the crown and the root canals) is removed.
- When It's Used: When the infection has spread throughout the entire pulp chamber and into the root canals of a primary tooth.
- Process: The infected pulp is removed, the canals are cleaned and disinfected, and then filled with a resorbable material (unlike permanent gutta-percha used in adult teeth) that will naturally dissolve as the permanent tooth erupts. The tooth is then sealed and often restored with a stainless steel crown.
Importance of Saving Primary Teeth:
- Space Maintenance: Baby teeth act as natural space holders for permanent teeth. Premature loss of a primary tooth can lead to adjacent teeth shifting, causing crowding or misalignment issues for the erupting permanent tooth.
- Chewing and Speech: Primary teeth are essential for proper chewing, nutrition, and the development of clear speech.
- Self-Esteem: A healthy smile contributes to a child's confidence.
Pro Tip for Parents: If your child complains of persistent toothache, sensitivity, or you notice swelling or a "pimple" on their gums, seek dental care immediately. Early intervention can prevent minor issues from escalating into complex infections.
Frequently Asked Questions
Q1: Do root canals hurt?
A: Modern root canal procedures are performed under local anesthesia, meaning you should not feel any pain during the treatment itself. The dentist will ensure the area is completely numb before beginning. Any discomfort you might feel is typically pressure or vibrations, not sharp pain. The reputation for pain often stems from older techniques or the severe pain experienced before treatment due to the infection.
Q2: How long does a root canal procedure take?
A: A standard root canal procedure usually takes between 60 to 90 minutes for a single appointment. However, more complex cases, especially on molars with multiple canals or re-treatments, may require longer appointments or two separate visits to ensure thorough cleaning and disinfection.
Q3: How long does recovery from a root canal take?
A: Most patients experience mild soreness or tenderness for 1 to 3 days after the procedure, which can be managed with over-the-counter pain relievers. Full recovery, where the tooth feels completely normal, typically takes about a week. It's crucial to avoid chewing on the treated tooth until your permanent crown is placed to prevent complications.
Q4: How long do root canals last?
A: With proper care and a timely placed permanent crown, a root canal-treated tooth can last a lifetime. Its longevity is comparable to other natural teeth. Regular oral hygiene, routine dental check-ups, and addressing any new decay promptly are essential for its long-term success.
Q5: What are the alternatives to a root canal?
A: The primary alternative to a root canal is tooth extraction. If the tooth is extracted, the missing tooth will need to be replaced with either a dental implant, a fixed bridge, or a removable partial denture to prevent issues like bone loss, shifting teeth, and bite problems. Each alternative has its own costs, benefits, and drawbacks.
Q6: Is it better to get a root canal or pull the tooth?
A: In most cases, it is highly recommended to save your natural tooth with a root canal. Preserving your natural tooth maintains your bite, prevents adjacent teeth from shifting, and avoids the need for more complex and often more expensive replacement options like dental implants or bridges. Extraction should generally be considered a last resort when a root canal is not viable.
Q7: Can a root canal get re-infected?
A: Yes, it is possible for a root canal-treated tooth to become re-infected or to fail to heal properly. This can occur years after the initial treatment due to new decay, a compromised crown or filling, a missed canal during the original procedure, or a root fracture. In such cases, endodontic retreatment or an apicoectomy may be necessary.
Q8: What kind of dentist performs root canals?
A: Both general dentists and endodontists perform root canal treatments. Endodontists are dental specialists who have completed an additional 2-3 years of advanced training specifically focused on the dental pulp and conditions related to it. For complex cases, re-treatments, or teeth with unusual anatomy, consulting an endodontist is often recommended as they have specialized equipment and expertise.
Q9: Will my tooth look different after a root canal?
A: A treated tooth might sometimes darken slightly over time due to internal staining. However, this is largely addressed by placing a dental crown, which covers the entire tooth and restores its natural appearance. For front teeth, internal bleaching can also be an option to lighten the tooth's color before placing a restoration.
Q10: When can I eat normally after a root canal?
A: You should avoid chewing on the treated tooth until the numbness from the anesthetic wears off completely. After that, stick to soft foods for the first few days to a week. Once your permanent dental crown is placed (typically a week or two after the root canal), you can generally resume eating normally. However, it's always wise to avoid excessively hard or sticky foods on any crowned tooth to prevent damage.
When to See a Dentist
While root canal treatment is highly effective, it's essential to be vigilant for signs that require immediate dental attention, both before and after the procedure.
Red Flags Requiring Immediate Attention (Emergency Care):
- Severe, Unrelenting Pain: If you experience intense, throbbing pain that doesn't subside with over-the-counter pain medication, whether before or after a root canal, it could indicate a severe infection or a complication.
- Significant Swelling: Swelling of the gums, jaw, or face, especially if it's rapidly worsening or accompanied by difficulty breathing or swallowing, is a sign of a serious spreading infection (abscess) and requires emergency care.
- Fever: A fever combined with tooth pain or swelling suggests a systemic infection.
- Pus Drainage: If you notice pus draining from the affected tooth or a "pimple" on your gums, this indicates an active infection.
- Trauma to a Tooth: If you experience a blow to a tooth that causes it to become loose, cracked, or severely painful, seek immediate dental evaluation.
Routine Care and Post-Procedure Guidance:
- Lingering Sensitivity or Pain (beyond a few days): While mild discomfort is normal for a few days post-root canal, persistent or worsening pain, or sensitivity to hot/cold, indicates a potential issue requiring follow-up with your dentist or endodontist.
- Loss of Temporary Filling/Crown: If your temporary filling falls out or your temporary crown becomes dislodged, contact your dentist right away to get it replaced. This protects the treated tooth from bacteria and prevents fracture.
- Discoloration of the Tooth: If your tooth begins to darken significantly after treatment, discuss options for cosmetic improvement with your dentist.
- Routine Check-ups: Regular dental check-ups and cleanings (every six months) are crucial for monitoring the health of your root canal-treated tooth and your overall oral health.
Don't hesitate to contact your dental professional if you have any concerns about your oral health, especially regarding a treated tooth. Early detection and intervention are key to preventing minor issues from escalating into major problems.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Stop Throbbing Pain After Root Canal
Undergoing a root canal procedure is often a necessary step to save a tooth severely damaged by decay or infection, preventing further complications and excruciating pain. While the procedure itself is performed under local anesthesia to ensure comfort, it's common for patients to experience some le
February 22, 2026
Root Canal After Care: Complete Guide
A root canal procedure can be a tooth-saving treatment, offering relief from pain and preventing further infection. However, the success and longevity of this crucial dental intervention heavily rely on diligent root canal after care. Neglecting post-treatment instructions can lead to complicati
February 22, 2026

Can You Drive After a Root Canal
Undergoing a root canal procedure can understandably bring up a host of questions and concerns, from understanding the process itself to managing recovery. One of the most common and practical inquiries people have is: can you drive after a root canal? The answer isn't always a simple yes or no,
February 22, 2026
Is a Root Canal Painful
When facing the prospect of a root canal, one of the most common and immediate questions that comes to mind is: is a root canal painful? It's a valid concern, stemming from outdated perceptions and anecdotal stories. However, modern root canal therapy is a highly effective and generally comforta
February 22, 2026