Sleep Apnea Mouth Piece: Complete Guide

Key Takeaways
- Do you often wake up feeling tired, even after a full night's sleep? Does your partner complain about your thunderous snoring, sometimes accompanied by gasps or choking sounds? You might be experiencing sleep apnea, a serious condition affecting over 25 million adults in the US. While Continuous
Sleep Apnea Mouth Piece: Complete Guide
Do you often wake up feeling tired, even after a full night's sleep? Does your partner complain about your thunderous snoring, sometimes accompanied by gasps or choking sounds? You might be experiencing sleep apnea, a serious condition affecting over 25 million adults in the US. While Continuous Positive Airway Pressure (CPAP) machines are often the first line of treatment, a sleep apnea mouth piece offers a highly effective and comfortable alternative for many. This comprehensive guide from SmilePedia.net will explore everything you need to know about oral appliances, from how they work to costs, care, and whether they're the right solution for you. We'll delve into the science behind these devices, compare them to other treatments, and provide practical advice to help you achieve restful, restorative sleep.

Key Takeaways:
- Oral Appliances (OAs) are custom-fitted devices worn during sleep to treat mild to moderate obstructive sleep apnea (OSA) and primary snoring.
- They work by repositioning the jaw or tongue to keep the airway open, effectively addressing snoring with mouth closed and open-mouth snoring.
- Types: Mandibular Advancement Devices (MADs) are most common, gently moving the lower jaw forward. Tongue Retaining Devices (TRDs) hold the tongue in place. Custom-fitted devices from a dentist are significantly more effective than over-the-counter options.
- Cost: Custom oral appliances typically range from $1,800 to $3,500 in the US, including consultations, impressions, device fabrication, and adjustments. OTC devices are much cheaper ($50-$200) but generally not recommended for diagnosed OSA.
- Insurance Coverage: Many medical insurance plans, including Medicare, cover custom oral appliances if prescribed for OSA, often treating them as durable medical equipment (DME). Dental insurance typically does not cover OSA treatment.
- Effectiveness: OAs can reduce the Apnea-Hypopnea Index (AHI) by 50% or more in suitable patients, leading to significant improvement in sleep quality and daytime symptoms.
- Timeline: The process from initial consultation to receiving a custom-fitted device usually takes 4-8 weeks, with follow-up adjustments over the next few months to optimize effectiveness and comfort.
What It Is: Understanding the Sleep Apnea Mouth Piece
A sleep apnea mouth piece, also known as an oral appliance (OA) or oral mandibular advancement device (OMAD), is a custom-fitted dental device worn in the mouth during sleep. Its primary purpose is to treat obstructive sleep apnea (OSA) and primary snoring by maintaining an open, unobstructed airway. Unlike CPAP machines, which deliver pressurized air, oral appliances work mechanically to prevent the collapse of soft tissues in the throat that characterize OSA.
These devices are typically small, lightweight, and resemble a sports mouthguard or orthodontic retainer. They are designed to fit precisely over your teeth, similar to how braces work, making them comfortable and easy to wear. For many individuals, particularly those with mild to moderate sleep apnea or those who cannot tolerate CPAP therapy, a sleep apnea mouth piece offers a less intrusive and highly effective treatment option.
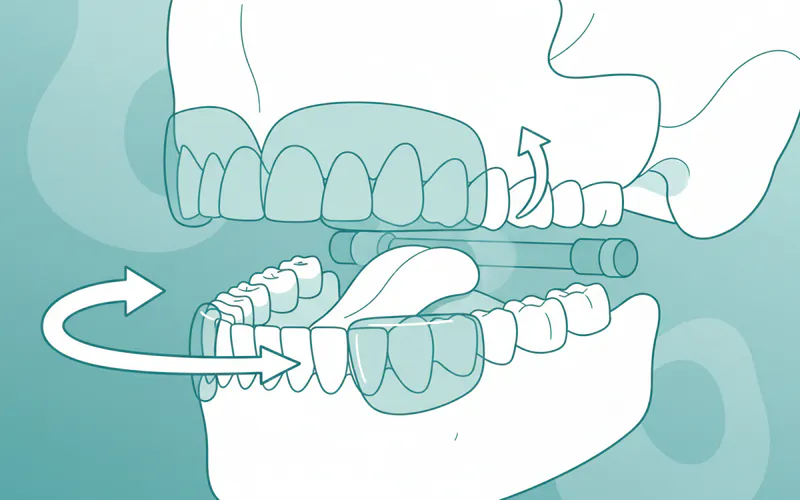
The core mechanism involves either gently advancing the lower jaw (mandible) forward or holding the tongue in a forward position. This action tightens the soft tissues and muscles of the upper airway, preventing them from collapsing backward and blocking the air passage. By keeping the airway open, the device allows for uninterrupted breathing, reducing or eliminating apnea events (pauses in breathing) and hypopneas (shallow breaths), as well as the loud snoring often associated with them.
Types of Sleep Apnea Mouth Pieces and Variations
Not all sleep apnea mouth pieces are created equal. The effectiveness and comfort largely depend on the type, customization, and materials used. The two main categories of oral appliances prescribed for sleep apnea are Mandibular Advancement Devices (MADs) and Tongue Retaining Devices (TRDs).
Mandibular Advancement Devices (MADs)
MADs are the most common type of oral appliance for sleep apnea. They work by holding the lower jaw (mandible) in a slightly forward position, which in turn moves the tongue and soft palate forward. This action prevents the collapse of the soft tissues at the back of the throat and base of the tongue, thereby keeping the airway open.
Key Features of MADs:
- Custom-Fitted: The most effective MADs are custom-made by a qualified dentist specializing in sleep medicine. They involve taking impressions of your teeth to create a precise fit.
- Adjustable: Many custom MADs feature a mechanism (often a screw or strap) that allows for gradual adjustment of the lower jaw's advancement. This titration is crucial for finding the optimal, most comfortable position that effectively treats your apnea.
- Two-Piece Design: Most MADs consist of two separate trays, one for the upper teeth and one for the lower, which are connected by hinges or small rods. This design often allows for some mouth movement, which can be more comfortable for some users.
Tongue Retaining Devices (TRDs)
TRDs are less common than MADs but can be an effective alternative, especially for individuals who cannot tolerate MADs or who have few or no teeth. Instead of moving the jaw, a TRD holds the tongue in a forward position using a suction bulb.
Key Features of TRDs:
- Tongue Stabilization: The device features a small compartment that the tongue fits into, creating suction to keep it from falling back into the airway.
- Jaw-Independent: Since TRDs do not rely on jaw advancement, they can be a good option for people with temporomandibular joint (TMJ) disorders or those who have significant dental issues.
- Customization: While some universal TRDs exist, custom-fitted versions offer better comfort and efficacy.
Custom-Fitted vs. Over-the-Counter (OTC) Devices
This distinction is critical for safety and effectiveness.
Custom-Fitted Oral Appliances
- Prescription Required: These devices are prescribed by a physician (often a sleep physician or pulmonologist) and fitted by a qualified dentist who has expertise in sleep dentistry.
- Precision and Comfort: Made from durable, biocompatible materials based on precise dental impressions, custom devices offer superior fit, comfort, and longevity.
- Adjustability: Custom MADs are often adjustable, allowing the dentist to gradually advance the jaw to the optimal position for treating sleep apnea while minimizing side effects.
- Medical Grade: These are FDA-approved medical devices intended for long-term use in treating a diagnosed medical condition.
- Effectiveness: Clinical studies show custom OAs are highly effective for mild to moderate OSA, reducing AHI significantly.
- Cost: Significantly more expensive than OTC options, ranging from $1,800 to $3,500, but often covered by medical insurance.
Over-the-Counter (OTC) "Boil-and-Bite" Devices
- No Prescription: Available online or in pharmacies, these are typically self-fitted by submerging them in hot water and then biting down to create an impression.
- Limited Customization: While they offer some level of personalization, the fit is rarely as precise or stable as a custom-made device.
- Non-Adjustable (usually): Most OTC devices lack the fine-tuning adjustability crucial for optimizing treatment and comfort.
- Potential Risks: Using an OTC device without a proper diagnosis can mask serious sleep apnea, leading to inadequate treatment and potential health complications. They can also cause dental problems, jaw pain, and gum irritation if not properly fitted or used for prolonged periods.
- Not Recommended for OSA: The American Academy of Sleep Medicine (AASM) and American Dental Association (ADA) strongly recommend against using OTC devices for the treatment of diagnosed obstructive sleep apnea. They might offer some relief for simple snoring, but they are not a substitute for a medical device.
- Cost: Much cheaper, typically ranging from $50 to $200.
Causes of Sleep Apnea and Why a Mouth Piece Helps
Understanding the root causes of obstructive sleep apnea (OSA) helps clarify why a sleep apnea mouth piece is such an effective treatment. OSA occurs when the muscles in your throat relax too much during sleep, causing the soft tissues to collapse and block your airway.
Primary Causes and Contributing Factors:
-
Anatomical Factors:
- Recessed Jaw (Retrognathia): A naturally smaller or set-back lower jaw can predispose individuals to OSA because it reduces the space for the tongue and soft palate.
- Large Tongue (Macroglossia): An unusually large tongue can easily fall back and obstruct the airway.
- Enlarged Tonsils or Adenoids: Especially common in children, these can physically block the airway.
- Obesity: Excess weight, particularly around the neck, can narrow the airway and increase the likelihood of tissue collapse. Fat deposits can thicken the walls of the airway.
- Nasal Obstruction: Chronic nasal congestion, deviated septum, or allergies can force mouth breathing, which can cause the tongue to fall back and narrow the airway. This often leads to snoring with mouth closed as the individual attempts to breathe through their nose but fails, then resorts to mouth breathing.
-
Muscle Tone and Relaxation:
- During deep sleep, throat muscles naturally relax. In individuals with OSA, this relaxation is sufficient to cause the airway to collapse.
- Alcohol and Sedatives: These substances further relax throat muscles, worsening sleep apnea.
- Aging: As we age, muscle tone decreases, making individuals more susceptible to OSA.
-
Other Medical Conditions:
- Hypothyroidism: Can lead to tissue swelling in the neck and tongue.
- Acromegaly: A condition where the body produces too much growth hormone, leading to enlarged soft tissues.
- Allergies/Asthma: Can cause inflammation and swelling in the airway.
How an Oral Appliance Addresses These Causes:
A sleep apnea mouth piece directly counters the anatomical and muscle relaxation factors that lead to airway collapse.
- Mandibular Advancement Devices (MADs): By gently holding the lower jaw forward, MADs create more space in the retrolingual (behind the tongue) and retropalatal (behind the soft palate) regions of the airway. This forward positioning prevents the tongue and soft palate from falling back and blocking airflow. It also tightens the surrounding soft tissues, making them less likely to collapse.
- Tongue Retaining Devices (TRDs): These devices specifically target tongue-based obstructions by holding the tongue in a forward, stabilized position. This is particularly useful for individuals where the tongue is the primary culprit in airway blockage.
By mechanically maintaining an open airway, oral appliances effectively prevent the pauses in breathing and loud snoring that characterize OSA, allowing for continuous, restorative sleep.
Signs and Symptoms of Sleep Apnea
Recognizing the signs and symptoms of sleep apnea is the first step toward diagnosis and treatment. While loud snoring is a hallmark, it's crucial to look beyond that, as many people who snore do not have sleep apnea, and some with sleep apnea may not snore loudly.

Nocturnal Symptoms (During Sleep):
- Loud and Persistent Snoring: Often described as gasping, choking, or snorting sounds, it's frequently reported by a bed partner. This can include snoring with mouth closed, indicating nasal obstruction as a potential contributing factor or an attempt to breathe through the nose.
- Observed Pauses in Breathing: A partner may notice moments where you stop breathing for several seconds, followed by a gasp or choke.
- Gasping or Choking for Air: Waking up suddenly feeling short of breath.
- Restless Sleep: Frequent awakenings, tossing and turning.
- Night Sweats: Excessive sweating during sleep.
- Frequent Nighttime Urination (Nocturia): Sleep apnea can interfere with hormone regulation, leading to increased urine production.
Daytime Symptoms (While Awake):
- Excessive Daytime Sleepiness: Feeling very tired and drowsy throughout the day, despite seemingly adequate sleep. This is often the most impactful symptom.
- Morning Headaches: Waking up with a headache due to poor oxygenation during sleep.
- Irritability and Mood Changes: Sleep deprivation can lead to mood swings, anxiety, and depression.
- Difficulty Concentrating or Memory Problems: Cognitive impairment due to fragmented sleep.
- Decreased Libido: Reduced sex drive.
- Dry Mouth or Sore Throat: Especially upon waking, often due to mouth breathing during sleep.
If you or your partner notice several of these symptoms, it's vital to consult a healthcare professional for an evaluation. Ignoring these signs can lead to serious long-term health complications.
Comprehensive Treatment Options for Sleep Apnea
Treating sleep apnea is crucial for preventing severe health risks. While a sleep apnea mouth piece is a significant option, it's part of a broader spectrum of treatments. Your doctor will recommend the best approach based on your diagnosis, severity of apnea, and personal preferences.
1. Positive Airway Pressure (PAP) Therapy (e.g., CPAP)
- What it is: The most common and highly effective treatment for moderate to severe OSA. A machine delivers a continuous stream of pressurized air through a mask worn over the nose or nose and mouth, keeping the airway open.
- Pros: Highly effective for all severities of OSA; non-invasive; immediate relief of symptoms.
- Cons: Can be noisy; mask discomfort, dryness, or irritation; feeling claustrophobic; portability issues. Compliance is a major challenge for many patients, leading to non-use. Finding the best cpap mask for side sleeper mouth breather can be tricky, as these specific needs require specialized mask designs (e.g., full-face masks or hybrid masks).
- Effectiveness: Gold standard; works for nearly all patients if tolerated.
2. Oral Appliance Therapy (OAT)
- What it is: Custom-fitted sleep apnea mouth pieces (MADs or TRDs) worn during sleep to reposition the jaw or tongue and keep the airway open.
- Pros: Non-invasive; highly portable; much quieter than CPAP; good compliance rates due to comfort and convenience; ideal for mild to moderate OSA or CPAP-intolerant patients. Addresses snoring with mouth closed effectively.
- Cons: Not effective for all types/severities of OSA; potential for temporary jaw discomfort, tooth movement, or excessive salivation; requires regular dental follow-ups.
- Effectiveness: Very effective for mild to moderate OSA; comparable to CPAP for these patients in terms of AHI reduction.
3. Lifestyle Modifications
- What it is: Changes in daily habits and routines to reduce the severity of sleep apnea.
- Pros: No side effects (positive overall health benefits); low to no cost.
- Cons: May not be sufficient as a standalone treatment for moderate to severe OSA; requires significant discipline.
- Examples:
- Weight Loss: Even a 10-15% reduction in body weight can significantly improve OSA symptoms, especially for individuals with obesity.
- Positional Therapy: Avoiding sleeping on your back (supine position) can prevent the tongue and soft palate from falling back. Special pillows or devices can help.
- Avoiding Alcohol and Sedatives: Especially before bedtime, as they relax throat muscles.
- Quitting Smoking: Smoking exacerbates inflammation and fluid retention in the airway.
- Nasal Decongestants/Allergy Treatment: Improving nasal breathing can reduce mouth breathing and related airway collapse.
4. Surgical Interventions
- What it is: Various procedures aimed at increasing the size of the airway or stiffening soft tissues.
- Pros: Can offer a permanent solution for some; may be effective for specific anatomical issues.
- Cons: Invasive; risks associated with surgery (pain, infection, bleeding); not always successful; recovery period.
- Types:
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the back of the throat, including the uvula, soft palate, and tonsils.
- Genioglossus Advancement: Moves a portion of the tongue muscle and its attachment to the lower jaw forward.
- Maxillomandibular Advancement (MMA): A more aggressive surgery that moves both the upper and lower jaws forward, significantly enlarging the airway. Reserved for severe cases.
- Hypoglossal Nerve Stimulation (Inspire Therapy): An implanted device stimulates the hypoglossal nerve, which controls tongue movement, to keep the airway open during sleep.
Comparison of Common Sleep Apnea Treatments
| Feature | CPAP Therapy | Oral Appliance Therapy | Lifestyle Modifications | Surgical Interventions |
|---|---|---|---|---|
| Primary Use | Moderate to Severe OSA | Mild to Moderate OSA; CPAP intolerance | Adjunct to other therapies; mild cases | Severe OSA; specific anatomical issues; CPAP/OA failure |
| Mechanism | Pressurized air keeps airway open | Repositions jaw/tongue | Reduces risk factors; improves overall health | Anatomical modification of airway |
| Effectiveness | High (gold standard) | High for suitable candidates; comparable to CPAP | Variable; rarely curative alone | Variable (depends on surgery type & patient) |
| Invasiveness | Non-invasive | Non-invasive | Non-invasive | Highly invasive |
| Portability | Moderate (machine, mask, tubing) | High (small device) | Excellent (no equipment) | N/A (after recovery) |
| Comfort | Variable (mask fit, pressure issues) | Generally good; some initial discomfort | Excellent | Post-operative pain; long recovery |
| Common Side Effects | Dryness, claustrophobia, skin irritation | Jaw pain, tooth movement, salivation (temporary) | None (positive health benefits) | Pain, infection, bleeding, voice changes, swallowing issues |
| Compliance | Often challenging (due to mask/noise) | Generally high | Requires discipline | N/A (after recovery) |
| Cost (Estimated US) | $800-$3,000 (machine, mask); supplies $100s/yr | $1,800-$3,500 (device + fitting) | Low (diet, exercise); some costs for positional aids | $5,000-$50,000+ (highly variable) |
Pro Tip: For best cpap mask for side sleeper mouth breather, consider full-face masks or hybrid masks that seal around the mouth and nose. Look for lightweight designs with minimal contact points and flexible tubing to accommodate different sleeping positions. Always try on several options under the guidance of a sleep specialist or DME provider.
The Step-by-Step Process for Getting a Sleep Apnea Mouth Piece
Obtaining a custom-fitted sleep apnea mouth piece involves a collaborative effort between your physician and a specially trained dentist. This systematic approach ensures the device is safe, effective, and tailored to your specific needs.
1. Initial Consultation with Your Physician
- Symptoms Review: You'll discuss your symptoms (snoring, daytime fatigue, observed pauses in breathing) with your primary care physician or a sleep specialist.
- Medical History: The doctor will take a comprehensive medical history, including any pre-existing conditions and medications.
- Physical Exam: A physical examination may include assessing your airway, jaw structure, and tonsils.
- Referral for Sleep Study: If sleep apnea is suspected, you'll be referred for a sleep study (polysomnography), either in a sleep lab or with a home sleep apnea test.
2. Sleep Study and Diagnosis
- Polysomnography (PSG): This overnight study records various physiological parameters during sleep (brain waves, oxygen levels, heart rate, breathing effort, leg movements).
- Diagnosis: Based on the results of the sleep study, a sleep physician will diagnose the presence and severity of sleep apnea (mild, moderate, or severe) using the Apnea-Hypopnea Index (AHI). This diagnosis is crucial for insurance coverage and treatment planning.
3. Consultation with a Sleep Dentist
- Referral: If diagnosed with mild to moderate OSA, or if you're intolerant to CPAP, your sleep physician will refer you to a qualified sleep dentist.
- Dental Exam: The dentist will conduct a thorough oral examination, assessing your teeth, gums, jaw joint (TMJ), and overall oral health to ensure you're a suitable candidate for an oral appliance. They'll also check for any conditions that might interfere with the device.
- Discussion of Options: The dentist will explain the types of oral appliances available and recommend the most appropriate one for you.
- Insurance Pre-authorization: The dental office will typically assist with getting pre-authorization from your medical insurance, as oral appliances for OSA are often covered as durable medical equipment (DME).
4. Impressions and Fabrication
- Dental Impressions: If you proceed, the dentist will take precise impressions of your upper and lower teeth. This typically involves using a mold material.
- Bite Registration: They will also take a "bite" registration, which captures the optimal forward position of your lower jaw. This is a critical step for MADs, determining the initial advancement.
- Lab Fabrication: These impressions and bite registrations are sent to a specialized dental laboratory that manufactures the custom oral appliance. This process can take 2-4 weeks.
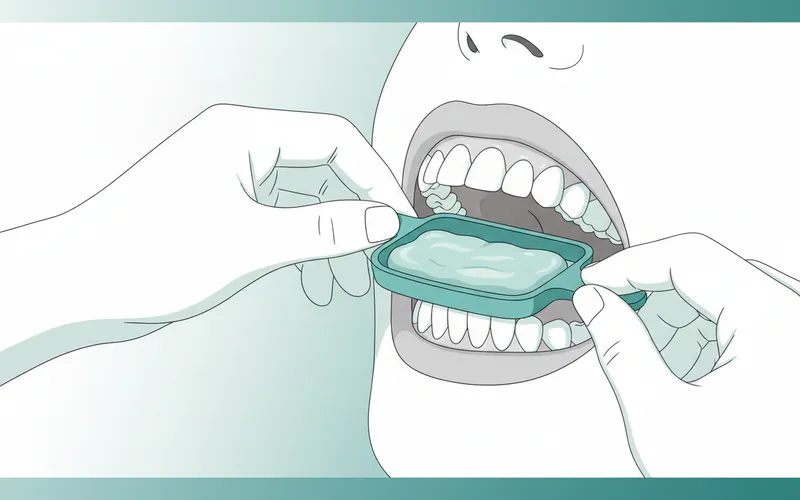
5. Fitting and Initial Adjustment
- Delivery Appointment: Once your custom sleep apnea mouth piece is ready, you'll return to the dentist for the fitting. The dentist will ensure it fits comfortably and securely.
- Initial Adjustment: They will guide you on how to insert and remove the device and provide instructions for care and hygiene. For adjustable MADs, the dentist will set the initial advancement.
- Instructions for Use: You'll be instructed to wear the device every night and to pay attention to your comfort and any changes in symptoms.
6. Follow-Up and Titration
- Initial Follow-Up (2-4 weeks): You'll have follow-up appointments with the dentist to assess comfort, effectiveness, and make any necessary adjustments to the device's advancement. This iterative process, known as titration, is crucial for optimizing treatment. You might be asked to keep a sleep diary.
- Objective Monitoring: After a period of adjustment (typically 3-6 months), your physician may recommend another sleep study with the appliance in place to objectively measure its effectiveness (e.g., AHI reduction).
- Ongoing Monitoring: Regular follow-up appointments with both your sleep physician and sleep dentist (usually annually) are essential to monitor your condition, check the appliance's integrity, and address any potential side effects like tooth movement or jaw discomfort.
This detailed process ensures that your sleep apnea mouth piece is not only effective but also comfortable and tailored to your unique anatomical and physiological needs, providing the best possible outcome for your sleep health.
Cost and Insurance Coverage for Sleep Apnea Mouth Pieces
The financial aspect of a sleep apnea mouth piece is a significant consideration for many patients. Understanding the typical costs and how insurance coverage works in the US is essential.
Average US Costs for Oral Appliances
- Custom-Fitted Oral Appliance: The most effective type, prescribed by a physician and fitted by a sleep dentist, typically ranges from $1,800 to $3,500. This comprehensive fee usually includes:
- Initial dental consultation and examination (sometimes a separate fee of $100-$300).
- Dental impressions and bite registration.
- Fabrication of the custom device by a specialized lab.
- Fitting appointment and initial adjustments.
- Follow-up appointments for titration and monitoring over several months.
- Over-the-Counter (OTC) Boil-and-Bite Devices: These are significantly cheaper, usually ranging from $50 to $200. However, as mentioned, they are not recommended for treating diagnosed sleep apnea due to their limited effectiveness, lack of customization, and potential for adverse effects.
What Influences the Cost?
- Geographic Location: Costs can vary by region (e.g., urban vs. rural, high cost-of-living areas).
- Dentist's Experience and Specialization: Dentists with extensive training and experience in sleep dentistry may charge higher fees.
- Type of Device: While most MADs fall within a similar range, some advanced designs or materials might slightly impact the price.
- Included Services: Always clarify what's included in the total fee (e.g., how many follow-up adjustments are covered).
Insurance Coverage Details
This is where it can get complex, but understanding the key distinctions is vital:
- Medical Insurance (Not Dental Insurance): For a sleep apnea mouth piece prescribed to treat diagnosed obstructive sleep apnea, coverage typically falls under your medical insurance, not your dental insurance. This is because OSA is considered a medical condition, and the oral appliance is classified as Durable Medical Equipment (DME).
- Diagnosis is Key: You MUST have a formal diagnosis of obstructive sleep apnea (mild to moderate, or severe if you are CPAP intolerant) from a sleep study and a physician's prescription for an oral appliance. Without this, medical insurance will deny coverage.
- Deductibles and Co-insurance: Even with medical insurance, you will likely be responsible for your annual deductible and a percentage of the cost (co-insurance) after the deductible is met.
- In-Network vs. Out-of-Network: Check if the sleep dentist is in-network with your medical insurance plan. Out-of-network providers will result in higher out-of-pocket costs.
- Medicare Coverage: Medicare Part B generally covers oral appliances as DME if they are FDA-approved, prescribed by a physician, and provided by a Medicare-enrolled supplier (your sleep dentist's office must be registered as a DME provider).
- Prior Authorization: Many insurance companies require prior authorization before you can receive the device. Your dentist's office usually handles this process, but it can take time (weeks to months).
- Documentation: Ensure all necessary documentation (sleep study results, physician's prescription, letter of medical necessity) is submitted.
Payment Plans and Financing Options
- Dental Office Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay the balance in installments.
- Third-Party Financing: Options like CareCredit or Alphaeon Credit provide low-interest or interest-free financing for healthcare expenses over a set period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts are excellent ways to pay for medical expenses like oral appliances with pre-tax dollars.
Pro Tip: Always call your medical insurance provider directly to confirm your specific benefits for Durable Medical Equipment (DME) related to sleep apnea treatment. Ask about your deductible, co-insurance, and if there are any specific requirements for oral appliances. Get everything in writing if possible.
| Cost Component | Estimated Range (USD) | Insurance Coverage | Notes |
|---|---|---|---|
| Sleep Study (PSG) | $500 - $5,000+ | Medical Insurance | Highly variable by type (home vs. lab) and location; usually covered if medically necessary. |
| Initial Sleep Dentist Consult | $100 - $300 | Medical Insurance | May be covered if coded as a medical visit; check with your provider. |
| Custom Oral Appliance | $1,800 - $3,500 | Medical Insurance | Usually covered as DME with physician's prescription and OSA diagnosis; deductibles/co-insurance apply. |
| Follow-up Adjustments | Included in OA cost | Medical Insurance | Typically included for several months post-fitting; long-term check-ups may be separate charges. |
| OTC Boil-and-Bite Device | $50 - $200 | None | Not recommended for diagnosed OSA; for simple snoring only, without medical oversight. |
Recovery and Aftercare for Your Sleep Apnea Mouth Piece
Getting a sleep apnea mouth piece is just the beginning of your journey to better sleep. Proper recovery, adaptation, and diligent aftercare are essential for long-term success and comfort.

Initial Adjustment Period (First Few Weeks):
- Temporary Discomfort: It's common to experience some initial discomfort, especially in your teeth, gums, and jaw joints (TMJ) during the first few nights or weeks. This is usually mild and resolves as your mouth adapts.
- Jaw Soreness: Your jaw muscles are adjusting to a new position. Gentle jaw exercises (e.g., opening and closing your mouth gently, massaging your jaw) in the morning can help.
- Tooth Sensitivity: Some teeth might feel slightly sore or loose. This typically subsides.
- Excess Salivation or Dry Mouth: Your body's natural response to a foreign object; usually resolves within a few days to weeks.
- Bite Changes: You might notice your bite feels "off" in the morning. This is temporary. After removing the device, your bite should return to normal within 30-60 minutes. Your dentist may provide a "morning repositioner" (a small retainer-like device) to help realign your bite quickly.
- Speech and Swallowing: You might experience slight changes in speech or difficulty swallowing initially. This also improves with practice and adaptation.
Long-Term Aftercare and Maintenance:
- Daily Cleaning:
- Rinse: Immediately after waking, rinse your appliance with cool water.
- Brush: Use a soft-bristle toothbrush and non-abrasive soap (like mild dish soap) or a specialized oral appliance cleaner to gently brush all surfaces. Avoid regular toothpaste, which can be abrasive and damage the material.
- Soak: Periodically (e.g., once a week or as recommended by your dentist), soak the appliance in a dental appliance cleaning solution (e.g., retainer brite, polident for retainers) to remove bacteria and stains.
- Storage: Always store your sleep apnea mouth piece in its protective case when not in use. This prevents damage, loss, and keeps it hygienic. Do not store it in direct sunlight or extreme temperatures.
- Regular Dental Check-ups:
- Sleep Dentist Follow-ups: Continue with your prescribed follow-up appointments with your sleep dentist (typically annually after the initial titration phase). They will check the fit, adjust the device if needed, monitor your oral health, and screen for any potential side effects like tooth movement or TMJ issues.
- General Dental Check-ups: Continue your routine general dental check-ups and cleanings as normal. Inform your general dentist that you are using an oral appliance for sleep apnea.
- Monitoring Symptoms: Continuously monitor your sleep apnea symptoms (snoring, daytime fatigue, choking episodes). If symptoms return or worsen, inform your sleep dentist and physician immediately. The device might need further adjustment, or your condition may have progressed.
- Replacing the Appliance: Oral appliances typically last 3-5 years with proper care, though some may last longer. Over time, materials can wear down or change shape. Your dentist will advise you when replacement is necessary.
Pro Tip: If you experience persistent jaw pain, significant tooth movement, or discomfort that doesn't resolve after the initial adjustment period, contact your sleep dentist. Do not attempt to adjust the device yourself.
Prevention of Sleep Apnea and Snoring
While a sleep apnea mouth piece and other treatments effectively manage existing conditions, certain lifestyle choices and habits can help prevent the onset or worsening of sleep apnea and reduce snoring.
- Maintain a Healthy Weight: Obesity is a significant risk factor for OSA. Losing even a modest amount of weight can significantly reduce throat tissue and improve airway patency. Focus on a balanced diet and regular physical activity.
- Avoid Alcohol and Sedatives Before Bed: These substances relax the muscles in your throat, increasing the likelihood of airway collapse. Avoid them at least 4-6 hours before sleep.
- Quit Smoking: Smoking causes inflammation and fluid retention in the upper airway, narrowing the air passages and contributing to snoring and apnea.
- Sleep on Your Side: Sleeping on your back (supine position) allows gravity to pull the tongue and soft palate backward, obstructing the airway. Side sleeping can significantly reduce snoring and mild apnea events. Positional therapy devices (e.g., special pillows, backpack-like devices that prevent back sleeping) can help.
- Address Nasal Congestion: Chronic nasal congestion from allergies, colds, or anatomical issues (like a deviated septum) can lead to mouth breathing and worsen snoring. Use saline nasal sprays, allergy medications, or consult an ENT for persistent issues. Improving nasal airflow can make a big difference, helping to mitigate snoring with mouth closed if the obstruction is nasal.
- Regular Exercise: Beyond weight management, regular exercise can improve overall muscle tone, including the muscles in your throat, which may help keep the airway open.
- Oral and Maxillofacial Health: Regular dental check-ups can help identify anatomical issues early. In children, early intervention for enlarged tonsils/adenoids or jaw development issues can be preventative.
- Avoid Large Meals Close to Bedtime: Eating heavy meals too close to sleep can contribute to acid reflux, which in turn can exacerbate airway irritation.
Risks and Complications Associated with Oral Appliances
While sleep apnea mouth pieces are generally safe and effective, like any medical device, they come with potential risks and side effects. It's important to be aware of these and discuss any concerns with your sleep dentist.
Common, Mild, and Temporary Side Effects (Often Resolve with Adjustment):
- Jaw Discomfort/Pain (TMJ): The most common side effect, especially in the first few weeks, as your jaw adapts to the new position. This can range from mild soreness to localized pain in the temporomandibular joints.
- Tooth and Gum Sensitivity: Teeth may feel tender or sensitive, and gums might be irritated.
- Excessive Salivation or Dry Mouth: The body's initial reaction to a foreign object in the mouth.
- Temporary Bite Changes: Your bite might feel "off" in the morning, but typically returns to normal within 30-60 minutes after removing the appliance.
- Minor Tooth Movement: While custom devices are designed to minimize this, slight shifts can occur over very long-term use.
Less Common, More Persistent, or Serious Complications:
- Permanent Bite Changes: In rare cases, especially with prolonged use or improper fitting/adjustment, permanent shifts in tooth position or changes to your occlusion (how your upper and lower teeth meet) can occur. This is why regular dental follow-ups are crucial.
- Temporomandibular Joint (TMJ) Dysfunction: While initial jaw discomfort is common, in some individuals, an oral appliance can exacerbate or trigger TMJ disorders, leading to chronic pain, clicking, popping, or difficulty opening/closing the mouth.
- Tooth Sensitivity or Damage: Improperly fitting appliances or excessive force can lead to increased tooth sensitivity, gum recession, or, in very rare instances, damage to dental restorations (crowns, fillings).
- Appliance Breakage or Wear: Oral appliances are made of durable materials, but they can crack, break, or wear down over time, especially if you clench or grind your teeth.
- Ineffectiveness: The appliance may not fully resolve your sleep apnea, or its effectiveness may decrease over time if your condition progresses or the appliance no longer fits properly.
- Difficulty Speaking or Swallowing: While usually temporary, persistent issues can affect quality of life.
Minimizing Risks:
- Custom Fit: Always opt for a custom-fitted device from a qualified sleep dentist. OTC devices carry a higher risk of adverse effects due to poor fit and lack of professional oversight.
- Proper Titration and Follow-up: Regular adjustments by your dentist are vital to find the optimal jaw position that treats your apnea effectively while minimizing discomfort.
- Regular Dental Check-ups: Adhere to your recommended follow-up schedule with your sleep dentist and general dentist to monitor oral health and the appliance's impact.
- Report Symptoms: Immediately report any persistent pain, significant tooth movement, or changes in your bite or TMJ to your dentist.
Children / Pediatric Considerations for Sleep Apnea
Sleep apnea isn't just an adult problem; it affects children too, often with different causes and symptoms. While a sleep apnea mouth piece may be considered in adolescents, the primary treatment for younger children typically differs.
Causes of Pediatric Sleep Apnea:
- Enlarged Tonsils and Adenoids: This is the most common cause of obstructive sleep apnea in children. These lymphatic tissues, located at the back of the throat and nasal cavity, can become overgrown and block the airway during sleep.
- Obesity: Similar to adults, childhood obesity is an increasing risk factor for OSA.
- Craniofacial Abnormalities: Conditions like Down syndrome, Pierre Robin sequence, or certain malocclusions can affect airway anatomy.
- Neuromuscular Disorders: Conditions that affect muscle tone can also contribute.
- Allergies/Chronic Nasal Congestion: Can lead to mouth breathing and airway obstruction.
Signs and Symptoms in Children:
Pediatric symptoms can be subtle and often differ from adults:
- Snoring: Loud, habitual snoring is a major indicator.
- Restless Sleep: Frequent awakenings, unusual sleeping positions (e.g., hyperextending the neck).
- Gasping, Choking, or Pauses in Breathing: Observed by parents.
- Daytime Hyperactivity or ADHD-like Symptoms: Unlike adults, children may become hyperactive or have behavioral issues rather than excessive sleepiness.
- Difficulty Concentrating/Learning Problems: Academic struggles due to fragmented sleep.
- Irritability and Mood Swings.
- Mouth Breathing: Persistent mouth breathing, especially during sleep.
- Bedwetting (Enuresis): May occur due to sleep disruption.
- Slow Growth or Weight Gain (Failure to Thrive): In severe cases.
Treatment Options for Children:
- Adenotonsillectomy: Surgical removal of tonsils and adenoids is often the first-line treatment for pediatric OSA caused by enlarged tissues. It has a high success rate.
- Weight Management: For obese children, weight loss is crucial.
- Allergy Management: Treating allergies can reduce nasal congestion.
- Orthodontic Expansion: For children with narrow dental arches or recessed jaws, orthodontic treatments like rapid palatal expanders (RPEs) can widen the upper jaw and potentially increase airway space.
- CPAP: Used for more severe cases, or when other treatments are ineffective, though compliance can be challenging for children.
- Oral Appliances (Adolescents): A sleep apnea mouth piece (MAD) may be considered for adolescents (typically after permanent teeth have erupted and facial growth is largely complete) with mild to moderate OSA, especially if surgery is not an option or has been unsuccessful. It's less commonly used in very young children due to ongoing growth and development.
Pro Tip: If you suspect your child has sleep apnea, consult your pediatrician. Early diagnosis and treatment are crucial to prevent long-term health, developmental, and behavioral issues.
Frequently Asked Questions
How effective is a sleep apnea mouth piece compared to CPAP?
For individuals with mild to moderate obstructive sleep apnea (OSA), a custom-fitted oral appliance (OA) can be as effective as CPAP therapy in reducing the Apnea-Hypopnea Index (AHI) and improving symptoms like snoring and daytime sleepiness. For severe OSA, CPAP remains the gold standard, but OAs can be a viable alternative for patients who cannot tolerate CPAP.
Does insurance cover the cost of a sleep apnea mouth piece?
Yes, most medical insurance plans in the US, including Medicare, typically cover custom-fitted oral appliances for diagnosed obstructive sleep apnea, treating them as Durable Medical Equipment (DME). However, you'll need a physician's prescription and a formal sleep study diagnosis. Dental insurance usually does not cover sleep apnea treatment. Expect to pay deductibles and co-insurance.
Is wearing a sleep apnea mouth piece painful?
Initially, you may experience some mild discomfort, tenderness in your teeth or jaw, or increased salivation. This is normal as your mouth adjusts and usually subsides within a few days to weeks. If pain persists or is severe, it's crucial to contact your sleep dentist for adjustments.
How long does it take to get used to wearing the device?
Most patients adapt to wearing a sleep apnea mouth piece within a few nights to a couple of weeks. Consistent use every night helps your mouth and jaw get accustomed to the appliance more quickly.
Can a sleep apnea mouth piece cause permanent changes to my teeth or bite?
While temporary changes to your bite are common in the morning, permanent changes to tooth position or occlusion are rare with custom-fitted, properly monitored devices. Regular follow-up appointments with your sleep dentist are crucial to monitor for and prevent such long-term complications. OTC devices carry a higher risk.
How often do I need to replace my oral appliance?
With proper care, a custom-fitted oral appliance typically lasts 3 to 5 years. Your sleep dentist will monitor its condition during your annual check-ups and advise you when replacement is necessary due to wear and tear or changes in your oral anatomy.
Can a sleep apnea mouth piece stop all my snoring, even with my mouth closed?
A custom-fitted oral appliance is highly effective at reducing or eliminating snoring by keeping the airway open. If you experience snoring with mouth closed, it often indicates nasal obstruction. While an oral appliance primarily addresses throat-level obstruction, improving nasal breathing (e.g., with saline rinses or allergy treatment) in conjunction with an OA can provide the most comprehensive relief.
Are there any alternatives to a sleep apnea mouth piece if it doesn't work for me?
Yes, there are several alternatives. These include CPAP therapy (the most common and effective for all severities), lifestyle modifications (weight loss, positional therapy), and various surgical options (e.g., UPPP, genioglossus advancement, hypoglossal nerve stimulation). Your sleep physician and dentist can discuss these options based on your specific condition and preferences.
What makes a custom-fitted device better than an over-the-counter one?
Custom-fitted oral appliances are precisely made from dental impressions, offering superior comfort, fit, and efficacy. They are adjustable, allowing for fine-tuning to optimize treatment and minimize side effects. OTC devices are generic, less effective, can cause dental issues, and should not be used for diagnosed sleep apnea without medical supervision.
Can I use a sleep apnea mouth piece if I have dentures or missing teeth?
It depends. While some oral appliances require a certain number of natural teeth for retention, Tongue Retaining Devices (TRDs) can be an option for individuals with dentures or very few teeth, as they hold the tongue forward independently of the jaw. Your sleep dentist will assess your specific dental situation.
When to See a Dentist or Sleep Specialist
Recognizing when to seek professional help for sleep issues is paramount for your overall health. Don't wait for symptoms to become severe.
See a Dentist or Sleep Specialist if You Experience:
- Loud, Habitual Snoring: Especially if it's disruptive to a bed partner or accompanied by gasping, choking, or pauses in breathing. Even snoring with mouth closed can be a sign of underlying issues.
- Excessive Daytime Sleepiness: Feeling tired, drowsy, or falling asleep unintentionally during the day, even after what you believe was sufficient sleep.
- Morning Headaches or Dry Mouth: Waking up regularly with these symptoms.
- Difficulty Concentrating, Memory Problems, or Irritability: Persistent cognitive or mood changes that impact your daily life.
- Observed Pauses in Breathing During Sleep: If a bed partner notices you stop breathing for periods of time. This is a significant red flag for sleep apnea.
- High Blood Pressure or Other Cardiovascular Issues: Sleep apnea is a major risk factor for these conditions. If you have them, especially if they are difficult to control, your doctor may recommend a sleep evaluation.
- You've been diagnosed with sleep apnea and are struggling with CPAP: If you're CPAP intolerant or non-compliant, a sleep apnea mouth piece may be a suitable alternative.
Emergency vs. Scheduled Appointment Guidance:
- Scheduled Appointment: Most sleep-related issues, including suspected sleep apnea, warrant a scheduled appointment with your primary care physician, who can then refer you to a sleep specialist or sleep dentist. There's usually no immediate emergency unless symptoms are extremely severe.
- Immediate Medical Attention: If you experience severe chest pain, extreme difficulty breathing, or sudden, overwhelming sleepiness that puts you at immediate risk (e.g., while driving), seek emergency medical attention. These could be signs of severe, uncontrolled sleep apnea or other serious health conditions.
Regular check-ups with your dentist are crucial not only for your oral health but also because dentists are often the first healthcare providers to notice signs of sleep-disordered breathing due to their examination of your oral and pharyngeal anatomy. Don't hesitate to discuss any sleep concerns with your dental professional.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
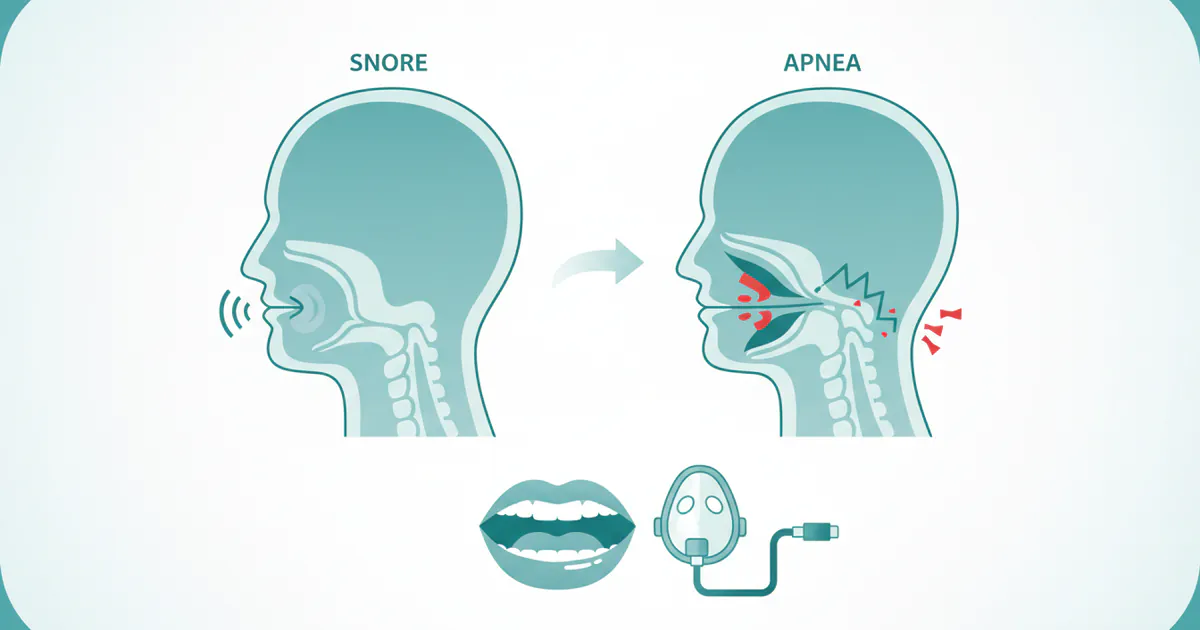
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026