Kidney Disease Bad Breath: Complete Guide
Key Takeaways
- When the delicate balance of your body's internal systems is disrupted, the signs can manifest in surprising ways – sometimes, right under your nose. Did you know that 1 in 7 adults in the US, an estimated 37 million people, may have chronic kidney disease (CKD), and many don't even realize it u
When the delicate balance of your body's internal systems is disrupted, the signs can manifest in surprising ways – sometimes, right under your nose. Did you know that 1 in 7 adults in the US, an estimated 37 million people, may have chronic kidney disease (CKD), and many don't even realize it until it's advanced? One of the lesser-known, yet incredibly impactful, symptoms of compromised kidney function is a distinctive form of bad breath. This isn't your everyday morning breath; kidney disease bad breath can be a persistent, tell-tale sign that your body is struggling to eliminate toxins, and it can significantly impact quality of life and even serve as an early warning.
For those living with kidney issues, or even those at risk, understanding the intricate link between kidney health and oral manifestations, particularly halitosis, is crucial. This comprehensive guide from SmilePedia.net will delve into what causes this specific type of bad breath, what it smells like, and what steps can be taken to manage and mitigate it. We’ll explore the underlying medical conditions, discuss various treatment strategies, provide insights into costs and recovery, and empower you with knowledge to protect both your oral and systemic health. By understanding the connection between your kidneys, your oral microbiome, and bad breath gut health, you can take proactive steps towards a healthier future.
Key Takeaways:
- Uremic Fetor: The characteristic "fishy" or "ammonia-like" odor of bad breath in kidney disease is known as uremic fetor, caused by the buildup of urea and ammonia in the bloodstream.
- Early Warning Sign: Persistent, unusual bad breath can be an early indicator of declining kidney function, warranting immediate medical evaluation.
- Comprehensive Management: Treatment involves managing the underlying kidney disease, meticulous oral hygiene, dietary adjustments, and potentially specific dental interventions.
- Cost of Care: Initial dental consultations for bad breath range from $75-$250. Kidney disease diagnosis and management can be significantly more, with lab tests ($50-$300) and specialist visits ($150-$500).
- Dental Treatments: Solutions like professional cleanings ($80-$200), specialized mouthwashes ($10-$30/month), and saliva substitutes ($15-$40/month) are often recommended.
- Gut Health Connection: An imbalanced gut microbiome can exacerbate bad breath in kidney disease by influencing nitrogenous waste metabolism. Addressing gut health is an emerging area of focus.
- Timelines: Improvement in bad breath typically aligns with successful management of kidney disease and consistent oral hygiene, which can take weeks to months to establish noticeable changes.
What Is Kidney Disease Bad Breath?
Kidney disease bad breath, medically known as uremic fetor, is a distinct and often unpleasant odor emanating from the mouth, particularly characteristic of advanced kidney failure. It’s not simply poor oral hygiene; it’s a systemic symptom reflecting the body's inability to properly filter waste products from the blood. When the kidneys—the body's natural filtration system—fail to function effectively, toxins that would normally be excreted in urine begin to accumulate in the bloodstream and other bodily fluids. This accumulation impacts various systems, including the oral cavity, leading to specific changes in breath.

The odor is frequently described as "fishy," "ammonia-like," or resembling the smell of urine. This distinct scent is primarily due to the breakdown of urea (a waste product of protein metabolism) into ammonia in the saliva. While the exact chemical compounds contributing to the smell are complex, ammonia is a major volatile component. This condition is a significant concern not only for its social implications but also as a potential indicator of severe underlying kidney dysfunction. Understanding uremic fetor is key to recognizing a symptom that extends far beyond typical halitosis, signaling a critical need for medical intervention.
Types of Bad Breath Associated with Kidney Disease
While "uremic fetor" is the primary type of bad breath directly linked to kidney failure, it's important to understand that patients with kidney disease can experience other forms of halitosis, some of which may be exacerbated by their condition:
- Uremic Fetor: As described, this is the classic "ammonia" or "fishy" breath stemming from urea and ammonia buildup. It's most prevalent in end-stage renal disease (ESRD).
- Generalized Halitosis: Patients with kidney disease are often prone to dry mouth (xerostomia) due to medication side effects, reduced fluid intake restrictions, or impaired salivary gland function. Dry mouth reduces saliva's natural cleansing action, allowing oral bacteria to proliferate and produce foul-smelling volatile sulfur compounds (VSCs), leading to general bad breath.
- Infection-Related Halitosis: Kidney disease can weaken the immune system, making individuals more susceptible to oral infections like gum disease (gingivitis, periodontitis), dental abscesses, or oral candidiasis (thrush). These infections produce their own distinct bad odors.
- Metallic Taste (Dysgeusia): While not strictly bad breath, many kidney patients report a persistent metallic or altered taste in their mouth. This taste is also attributed to the accumulation of waste products and can contribute to the overall perception of oral unpleasantness, sometimes accompanying uremic fetor.
It's crucial for dental professionals to differentiate these types of bad breath to ensure appropriate management, whether it's managing the underlying systemic condition or addressing specific oral health issues.
Causes: Why Kidney Disease Leads to Bad Breath
The presence of kidney disease bad breath is a direct consequence of the kidneys' impaired ability to perform their vital filtration role. When kidneys fail, they can no longer effectively remove metabolic waste products from the blood. These toxins then accumulate throughout the body, including the oral cavity. Here’s a detailed look at the root causes and contributing factors:
1. Accumulation of Nitrogenous Waste Products (Uremia)
This is the primary driver of uremic fetor. The kidneys are responsible for filtering waste products like urea, creatinine, and uric acid from the blood. In kidney disease, particularly as it progresses to stages 3-5, these substances build up, a condition known as uremia.
- Urea and Ammonia: Urea is a byproduct of protein metabolism, which the liver converts from ammonia (a highly toxic substance). Healthy kidneys efficiently excrete urea. When kidney function declines, urea levels in the blood (BUN - Blood Urea Nitrogen) rise significantly. Some of this excess urea diffuses into the saliva.
- In the mouth, certain oral bacteria possess an enzyme called urease. This enzyme breaks down the urea in saliva into ammonia. Ammonia has a pungent, acrid smell, similar to urine or certain cleaning products. This conversion is a major contributor to the characteristic "ammonia-like" breath.
- Trimethylamines: Another significant contributor to the "fishy" odor is trimethylamine (TMA). TMA is produced in the gut by certain bacteria as they break down dietary compounds like choline and carnitine. In healthy individuals, TMA is rapidly oxidized in the liver to trimethylamine N-oxide (TMAO) and then excreted by the kidneys. With impaired kidney function, TMA and TMAO accumulate, leading to their excretion via breath and sweat, giving a distinctive fishy smell.
2. Xerostomia (Dry Mouth)
Dry mouth, or xerostomia, is a common complaint among individuals with kidney disease, and it plays a significant role in exacerbating bad breath.
- Reduced Saliva Production: This can be due to several factors:
- Medications: Many medications prescribed for kidney disease (e.g., diuretics, blood pressure medications) have xerostomia as a common side effect.
- Fluid Restrictions: Patients with advanced kidney disease are often advised to restrict fluid intake to manage edema and blood pressure, which can reduce salivary flow.
- Damage to Salivary Glands: Long-term uremia can directly affect the function of salivary glands, impairing their ability to produce adequate saliva.
- Impact of Dry Mouth: Saliva is crucial for oral health. It naturally cleanses the mouth, neutralizes acids, and washes away food particles and bacteria. When saliva flow is reduced, food debris and dead cells accumulate, leading to increased bacterial growth. These bacteria produce volatile sulfur compounds (VSCs) like hydrogen sulfide and methyl mercaptan, which are highly odorous and contribute to general halitosis.
3. Oral Microbiome Dysbiosis
The balance of bacteria in the mouth, known as the oral microbiome, can be significantly altered in kidney disease.
- Shift in Bacterial Populations: The altered oral environment (changes in pH, reduced saliva, presence of urea) can favor the growth of specific types of bacteria. For example, an increase in urease-producing bacteria (which convert urea to ammonia) is common.
- Gut Microbiome and Oral-Systemic Link: The bad breath gut health connection is particularly relevant here. The gut microbiome plays a critical role in metabolizing various compounds, including nitrogenous waste products. In kidney disease, there's often a significant dysbiosis (imbalance) in the gut microbiome. This altered gut flora can produce more uremic toxins, which then enter the bloodstream and contribute to the overall uremic load, ultimately impacting breath. Research suggests a bidirectional relationship where changes in the oral microbiome can also influence the gut microbiome.
4. Poor Oral Hygiene and Associated Conditions
While not a direct cause of uremic fetor, poor oral hygiene can significantly worsen existing bad breath in kidney patients.
- Increased Risk of Oral Infections: Patients with kidney disease are more susceptible to:
- Periodontal Disease: Chronic inflammation of the gums, often leading to deep pockets where bacteria thrive and produce VSCs.
- Dental Caries (Cavities): Reduced saliva and changes in diet can increase cavity risk.
- Oral Candidiasis (Thrush): A fungal infection common in immunocompromised individuals.
- Inflammation and Systemic Impact: Oral infections like periodontitis create an inflammatory burden that can further strain the immune system and potentially worsen systemic conditions, including kidney disease itself. The bacteria and their byproducts contribute directly to foul breath.
5. Dietary Factors
Dietary restrictions and preferences in kidney disease can also play a role.
- Protein Intake: While protein intake is often managed in kidney disease, dietary protein is the source of urea. High protein intake without adequate kidney function will lead to more urea production.
- Specific Foods: Certain foods can temporarily worsen breath, though this is secondary to the metabolic issues.
Signs and Symptoms
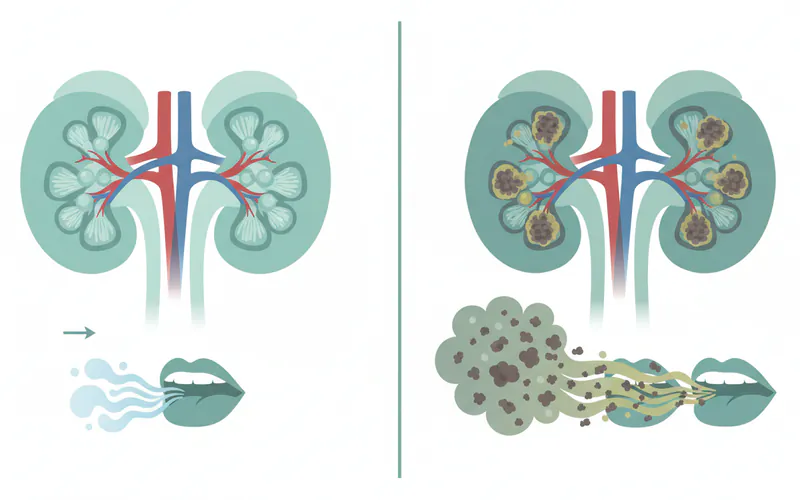
Recognizing the signs and symptoms associated with kidney disease bad breath is crucial for early detection and intervention. While bad breath itself is a symptom, it's often accompanied by other oral and systemic manifestations of kidney dysfunction.
Oral Signs and Symptoms:
- Uremic Fetor (Ammonia/Fishy Breath): This is the most distinctive oral symptom. The breath smells like ammonia, urine, or stale fish. It's usually constant and not resolved by typical oral hygiene practices.
- Metallic Taste (Dysgeusia): A persistent, unpleasant metallic, sour, or ammonia-like taste in the mouth is very common. This often precedes or accompanies the bad breath.
- Xerostomia (Dry Mouth): As discussed, significantly reduced saliva flow leading to a constantly dry, sticky feeling in the mouth. This can make speaking, chewing, and swallowing difficult.
- Stomatitis: Inflammation of the mucous membranes of the mouth, which can manifest as redness, soreness, and ulcerations. Uremic stomatitis, though rare in its severe form, can be very painful.
- Oral Lesions and Ulcers: Patients with kidney disease may develop ulcers on the oral mucosa, tongue, or lips. These can be painful and contribute to discomfort.
- Petechiae or Ecchymoses: Small red or purple spots (petechiae) or larger bruises (ecchymoses) in the mouth may indicate bleeding tendencies due to platelet dysfunction often seen in advanced kidney disease.
- Increased Plaque and Tartar Buildup: Reduced salivary flow and altered oral chemistry can accelerate plaque accumulation, increasing the risk of cavities and gum disease.
- Gum Bleeding and Inflammation: Gingivitis and periodontitis are common, leading to red, swollen, and bleeding gums. This contributes to general bad breath and can worsen systemic inflammation.
- Pallor of Oral Mucosa: The lining of the mouth may appear pale due to anemia, which is a common complication of kidney disease.
- Enamel Abnormalities: In children with kidney disease, dental enamel development can be affected, leading to hypoplasia (thin or pitted enamel) and increased cavity risk.
Systemic Signs and Symptoms of Kidney Disease:
It's important to remember that kidney disease bad breath is a symptom of a larger systemic issue. Other signs of declining kidney function include:
- Fatigue and Weakness: Due to anemia and toxin buildup.
- Swelling (Edema): In the legs, ankles, feet, or face, caused by fluid retention.
- Changes in Urination: Frequent urination (especially at night), foamy urine, or reduced urine output.
- Muscle Cramps or Weakness: Due to electrolyte imbalances.
- Nausea and Vomiting: Caused by toxin buildup.
- Loss of Appetite: Often accompanying nausea and metallic taste.
- Skin Itching or Dryness: Due to mineral and bone disorder and toxin accumulation.
- Difficulty Concentrating or Mental Fog: Known as "uremic encephalopathy."
- High Blood Pressure: Kidneys play a crucial role in regulating blood pressure.
If you or someone you know exhibits a combination of these symptoms, especially persistent, unusual bad breath, it is imperative to seek prompt medical attention.
Treatment Options for Kidney Disease Bad Breath
Effectively treating kidney disease bad breath requires a dual approach: managing the underlying kidney disease and implementing targeted oral health strategies. Since the bad breath is a symptom of systemic dysfunction, merely addressing the oral symptoms without treating the kidney disease will offer only temporary relief.
1. Medical Management of Kidney Disease (Primary Treatment)
The most effective way to eliminate uremic fetor is to improve kidney function or manage the accumulation of waste products.
- Dialysis: For patients with end-stage renal disease (ESRD), dialysis (hemodialysis or peritoneal dialysis) is the cornerstone treatment. Dialysis artificially filters the blood, removing urea, creatinine, and other toxins that cause bad breath.
- Pros: Directly removes waste products, significantly improving uremic fetor and overall health. Life-sustaining for ESRD patients.
- Cons: Time-consuming (hemodialysis typically 3 times a week for several hours), can have side effects (fatigue, hypotension), requires significant lifestyle adjustments.
- Kidney Transplant: A successful kidney transplant can completely restore kidney function, eliminating uremic fetor and many other symptoms of kidney disease.
- Pros: Offers the best long-term outcome, restores natural kidney function, significantly improves quality of life.
- Cons: Major surgery with significant risks, lifelong immunosuppressant medication, limited availability of donor organs, potential for rejection.
- Dietary Modifications: Working with a registered dietitian specializing in kidney disease is crucial.
- Protein Management: Moderate protein intake, often with a focus on high-quality proteins, can reduce urea production without causing malnutrition.
- Fluid and Electrolyte Management: Carefully managing fluid intake and electrolytes (potassium, sodium, phosphorus) is vital to reduce the overall burden on the kidneys.
- Pros: Can slow disease progression, reduce toxin buildup, improve overall well-being.
- Cons: Requires strict adherence, can be challenging to maintain.
- Medication Management: Addressing underlying conditions like high blood pressure, diabetes, and managing anemia can slow kidney disease progression. Medications to reduce phosphorus levels (phosphate binders) can also reduce the overall toxin burden.
2. Targeted Oral Health Interventions (Supportive Treatment)
While kidney disease management is primary, specific oral care strategies are essential to mitigate bad breath and maintain oral health.
- Meticulous Oral Hygiene:
- Brushing: Brush teeth at least twice daily with a soft-bristled brush and fluoride toothpaste. Consider an electric toothbrush for enhanced plaque removal.
- Flossing: Floss daily to remove interdental plaque and food particles.
- Tongue Cleaning: Crucial for removing bacteria, dead cells, and volatile compounds that accumulate on the tongue surface. Use a tongue scraper or the back of your toothbrush.
- Pros: Directly reduces bacterial load, improves general halitosis, and enhances overall oral hygiene.
- Cons: Requires consistent effort; may be difficult for patients with severe dry mouth or oral lesions.
- Antimicrobial Mouthrinses:
- Chlorhexidine Gluconate (CHX): Prescription-strength antiseptic rinse. Effective against a broad spectrum of oral bacteria. Used cautiously and usually short-term due to potential for staining and altered taste.
- Alcohol-Free Mouthwashes: Over-the-counter options containing cetylpyridinium chloride (CPC) or zinc can help neutralize odors and reduce bacteria. Always choose alcohol-free options to avoid exacerbating dry mouth.
- Pros: Reduces oral bacteria, freshens breath.
- Cons: CHX can cause staining and taste alteration; some OTC rinses may contain irritants.
- Saliva Substitutes and Stimulants for Dry Mouth (Xerostomia):
- Artificial Saliva Products: Gels, sprays, and rinses designed to mimic natural saliva. Brands like Biotene, XyliMelts, or Oasis can provide relief.
- Saliva Stimulants (Prescription): Medications like pilocarpine or cevimeline can increase saliva production in some patients, though they may have systemic side effects.
- Pros: Alleviates discomfort from dry mouth, helps with lubrication, and improves natural cleansing.
- Cons: Temporary relief, requires frequent application; prescription stimulants have side effects.
- Regular Dental Check-ups and Professional Cleanings:
- Frequency: Patients with kidney disease may require more frequent dental visits (e.g., every 3-4 months instead of 6) to monitor oral health, manage plaque/tartar, and address any infections promptly.
- Periodontal Treatment: Management of gum disease, from scaling and root planing to more advanced therapies, is critical.
- Pros: Prevents progression of oral diseases, identifies issues early, helps maintain optimal oral hygiene.
- Cons: Can be an added financial and time burden; requires coordination with medical team.
- Addressing Oral Infections: Prompt treatment of any dental caries, abscesses, or oral candidiasis is essential.
- Pros: Eliminates sources of foul odor and reduces oral pain and systemic inflammatory load.
- Cons: Requires specific dental procedures (fillings, extractions, antifungal medications).
Pro Tip: Always inform your dentist about your kidney disease diagnosis, current medications, and dialysis schedule. This allows them to coordinate care with your nephrologist and adjust dental treatments as needed, especially regarding medications (e.g., antibiotics, pain relievers) and potential bleeding risks.
Comparison of Oral Hygiene Strategies for Kidney Disease Bad Breath
| Strategy | Description | Pros | Cons | Estimated Monthly Cost (US) |
|---|---|---|---|---|
| Meticulous Home Care | Brushing (2x/day), flossing (1x/day), tongue scraping (1x/day) | Foundation of oral health, cost-effective, empowers patient. | Requires consistent effort and correct technique. | $10-$30 (toothpaste, brush) |
| Antimicrobial Mouthrinses | Alcohol-free rinses with CPC, zinc, or prescription CHX (short-term) | Reduces oral bacteria, neutralizes odors. | CHX can stain teeth/alter taste; some OTC rinses may irritate. | $10-$30 (OTC), $20-$40 (CHX) |
| Saliva Substitutes | Gels, sprays, lozenges (e.g., Biotene, XyliMelts) for dry mouth relief. | Alleviates dry mouth discomfort, aids natural cleansing. | Temporary relief, requires frequent reapplication. | $15-$40 |
| Professional Cleanings | Scaling, root planing, oral health education by dentist/hygienist (often every 3-4 months). | Removes stubborn plaque/tartar, treats gum disease, monitors oral health. | Can be costly without insurance, requires regular appointments. | $0-$200 (co-pay/out-of-pocket) |
Step-by-Step Process: Managing Kidney Disease Bad Breath
Managing kidney disease bad breath involves a coordinated effort between you, your nephrologist (kidney specialist), and your dentist. Here’s a typical step-by-step process you can expect:
Step 1: Initial Recognition and Medical Consultation
- Recognize the Signs: You might first notice a persistent, unusual odor in your breath (ammonia-like, metallic, fishy) that doesn't go away with brushing. You might also experience dry mouth or a metallic taste.
- Consult Your Physician/Nephrologist: If you suspect kidney issues, or if you already have a diagnosis, inform your medical doctor immediately about your breath changes. They will conduct tests to assess your kidney function, such as:
- Blood tests: Creatinine, BUN (Blood Urea Nitrogen), Glomerular Filtration Rate (GFR).
- Urine tests: Urinalysis, albumin-to-creatinine ratio.
- Imaging: Ultrasound of kidneys.
- Diagnosis and Staging: Based on test results, your doctor will diagnose kidney disease and determine its stage (Stages 1-5). The severity of bad breath often correlates with the stage of kidney failure.
Step 2: Referral to a Dental Professional
- Referral: Your nephrologist may refer you to a dentist or oral medicine specialist experienced in managing patients with systemic conditions. If not, proactively schedule an appointment with your dentist and inform their office about your kidney disease.
- Comprehensive Dental Examination: Your dentist will perform a thorough examination, including:
- Assessment of your breath odor.
- Evaluation for dry mouth.
- Check for gum disease (gingivitis, periodontitis).
- Screening for cavities, oral infections (like candidiasis), or lesions.
- Review of your medical history and medications.
Step 3: Coordinated Treatment Planning
- Medical Treatment Plan: Your nephrologist will initiate or adjust your kidney disease management, which may include:
- Medications to control blood pressure or diabetes.
- Dietary counseling (e.g., protein restriction, fluid management).
- Preparation for or initiation of dialysis if necessary.
- Evaluation for kidney transplant.
- Dental Treatment Plan: Your dentist, in consultation with your nephrologist, will develop an oral care plan. This might involve:
- Professional Cleaning: Thorough scaling and root planing to remove plaque and tartar and manage gum disease.
- Oral Hygiene Instruction: Detailed guidance on brushing, flossing, and especially tongue scraping techniques.
- Prescription/Recommendation for Oral Products: Specific mouthwashes (e.g., chlorhexidine for short-term use, alcohol-free rinses), saliva substitutes, or fluoride applications.
- Treatment of Oral Infections: Fillings for cavities, antibiotics for infections, antifungal medication for thrush.
- Addressing Dry Mouth: Recommendations for over-the-counter products or, rarely, prescription saliva stimulants.
Step 4: Ongoing Management and Monitoring
- Adherence to Medical Treatment: This is paramount. Consistent dialysis, medication adherence, and dietary compliance are critical for reducing the systemic toxins that cause bad breath.
- Consistent Oral Care: Diligently follow your personalized oral hygiene routine at home.
- Regular Dental Visits: Continue with scheduled dental check-ups, often more frequent than for the general population (e.g., every 3-4 months), to monitor oral health and adjust strategies as needed.
- Monitor for Improvement: As kidney function improves (via dialysis or transplant) and oral care is optimized, you should notice a reduction in the intensity of bad breath and other oral symptoms.
- Communication: Maintain open communication with both your nephrologist and dentist, reporting any changes in your breath, oral comfort, or overall health.
Cost and Insurance
Understanding the costs associated with managing kidney disease bad breath involves considering both the underlying medical treatment for kidney disease and specific dental interventions. Prices vary significantly based on geographic location, insurance coverage, and the specific providers involved.
Medical Costs for Kidney Disease Management:
The primary cost driver will be the treatment of the kidney disease itself, which can be substantial.
- Initial Diagnosis:
- Physician Visit: $150 - $500 (specialist visit, without insurance)
- Blood Tests (Creatinine, BUN, GFR, Electrolytes): $50 - $300
- Urinalysis: $20 - $100
- Kidney Ultrasound: $200 - $800
- Ongoing Management (without insurance, per visit/month):
- Nephrologist Visits: $150 - $450 per visit (typically every 3-6 months)
- Prescription Medications: Highly variable, from $20 - $500+ per month, depending on drug type and brand/generic status.
- Dialysis (for ESRD):
- Hemodialysis: Can cost $50,000 - $100,000+ per year. Each session can range from $500 - $1,500.
- Peritoneal Dialysis: May be slightly less, but still in the tens of thousands annually.
- Kidney Transplant:
- Surgery: Can exceed $200,000 - $400,000 for the procedure alone.
- Lifelong Immunosuppressants: $10,000 - $25,000+ per year.
Dental Costs for Bad Breath Management:
These costs are more manageable but can add up, especially with more frequent visits.
- Initial Dental Consultation/Exam: $75 - $250
- Routine Professional Cleaning (Prophylaxis): $80 - $200 (often required every 3-4 months for kidney patients)
- Scaling and Root Planing (for Periodontal Disease): $200 - $500 per quadrant (may be needed if gum disease is present)
- Tongue Scrapers: $5 - $15
- Specialized Toothpaste/Mouthwashes: $10 - $30 per month (e.g., alcohol-free, fluoride-rich)
- Saliva Substitutes (Gels, Sprays): $15 - $40 per month
- Treatment of Oral Infections (e.g., Fillings, Antifungals): Varies widely; fillings $100 - $350 per tooth, antifungals $20 - $100.
Insurance Coverage:
- Medical Insurance:
- Medicare/Medicaid: For individuals with ESRD, Medicare usually covers a significant portion of dialysis, transplant, and associated medical costs. Medicaid also provides coverage for eligible low-income individuals.
- Private Insurance: Most private health insurance plans cover kidney disease diagnosis and treatment, but patients will be responsible for deductibles, co-pays, and co-insurance. The specific coverage for nephrologist visits, lab tests, dialysis, and medications depends on the plan.
- Out-of-Pocket Maxima: Be aware of your plan's annual out-of-pocket maximum, which limits how much you'll pay in a given year.
- Dental Insurance:
- Basic Coverage: Most dental insurance plans cover preventive care (exams, cleanings) at a high percentage (80-100%).
- Major Procedures: Fillings, scaling and root planing, and other restorative work are typically covered at a lower percentage (50-80%), often after a deductible is met.
- Limits: Many plans have annual maximums (e.g., $1,000 - $2,000) that can quickly be met if extensive treatment is needed.
- Saliva Substitutes: These are often considered over-the-counter and usually not covered by dental insurance.
Payment Plans and Financing Options:
- Dental Office Payment Plans: Many dental offices offer in-house payment plans for larger treatments, allowing you to pay in installments.
- Medical Payment Plans: Hospitals and clinics often have financial assistance programs or payment plans for patients with significant medical bills.
- CareCredit/Other Medical Credit Cards: These specialized credit cards offer deferred interest or low-interest financing for healthcare expenses.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): If you have these, you can use pre-tax dollars to cover eligible medical and dental expenses.
Pro Tip: Discuss all treatment costs and insurance coverage details with your medical and dental providers' billing departments before commencing treatment. They can help you understand your estimated out-of-pocket expenses and explore available financial options.
Recovery and Aftercare
Recovery and aftercare for kidney disease bad breath are intrinsically linked to the successful management of the underlying kidney condition. While eliminating the core cause takes precedence, meticulous oral aftercare is essential for sustained improvement in breath and overall oral health.
1. Recovery from Kidney Disease Treatment:
- Post-Dialysis: After each dialysis session, patients often experience temporary fatigue, but the removal of toxins generally leads to an overall feeling of improved well-being. The intensity of uremic fetor should significantly decrease within hours to a day post-dialysis. Consistency with dialysis schedule is key.
- Post-Kidney Transplant: Recovery from a kidney transplant is a major process, typically involving several days to weeks in the hospital and months of careful monitoring. As the new kidney starts functioning, blood urea and creatinine levels normalize. This normalization directly leads to the resolution of uremic fetor and metallic taste, often within days to weeks of a successful transplant. Lifelong immunosuppression and adherence to medication are critical to prevent rejection and maintain the health of the transplanted kidney.
2. Ongoing Oral Aftercare and Maintenance:
Even with successful kidney disease management, continuous attention to oral hygiene is vital due to the inherent susceptibility of kidney patients to oral issues.
- Daily Oral Hygiene Routine:
- Brushing: Continue to brush thoroughly twice a day for at least two minutes with a soft-bristled toothbrush and fluoride toothpaste. Consider a power toothbrush for enhanced plaque removal.
- Flossing: Floss daily to remove interdental plaque and food debris.
- Tongue Cleaning: This remains critical. Gently scrape your tongue from back to front daily using a tongue scraper to remove bacterial buildup and reduce odor-producing compounds.
- Managing Dry Mouth (Xerostomia):
- Regular Hydration: Sip water frequently (within fluid restrictions advised by your doctor).
- Saliva Substitutes: Use over-the-counter gels, sprays, or lozenges as needed to keep your mouth moist.
- Xylitol Products: Chew xylitol gum or suck on xylitol candies (sugar-free) to stimulate saliva flow, but ensure they fit into your dietary restrictions.
- Avoid Irritants: Steer clear of alcohol-based mouthwashes, tobacco, and excessive caffeine, which can exacerbate dry mouth.
- Dietary Awareness:
- Kidney-Friendly Diet: Adhere strictly to the dietary recommendations from your nephrologist and dietitian. This helps control the buildup of toxins that contribute to bad breath.
- Limit Odor-Producing Foods: While less impactful than systemic issues, temporarily limiting foods with strong odors (e.g., garlic, onions) can help if you're sensitive.
- Regular Dental Check-ups:
- Increased Frequency: Kidney patients often benefit from more frequent dental check-ups and professional cleanings, typically every 3-4 months, instead of the standard six. This allows your dental team to closely monitor your oral health, manage plaque/tartar, and detect any issues early.
- Communication: Continue to inform your dental team about your kidney health status and any changes in your medications.
- Monitoring for Oral Complications: Be vigilant for any signs of new oral issues, such as:
- Persistent dry mouth
- Sores or ulcers
- Bleeding gums
- Unusual tastes or odors returning
- Pain or sensitivity in teeth or gums
- Report these to your dental professional promptly.
The goal of aftercare is not just to eliminate bad breath, but to maintain optimal oral health, which, in turn, supports your overall systemic health and quality of life while managing kidney disease.
Prevention of Kidney Disease Bad Breath
Preventing kidney disease bad breath primarily involves preventing or effectively managing kidney disease itself. Early intervention and proactive health measures are key.
1. Prevent or Manage Kidney Disease:
- Control Underlying Conditions: The leading causes of kidney disease are diabetes and high blood pressure.
- Diabetes Management: Maintain strict control over blood sugar levels through diet, exercise, and medication as prescribed. Regular A1C monitoring is essential.
- Blood Pressure Control: Keep blood pressure within healthy targets (e.g., generally below 120/80 mmHg) through lifestyle changes, diet (low sodium), and appropriate medications.
- Healthy Lifestyle:
- Balanced Diet: Consume a diet rich in fruits, vegetables, and whole grains. Limit processed foods, excessive sodium, and unhealthy fats.
- Regular Exercise: Aim for at least 150 minutes of moderate-intensity exercise per week.
- Maintain Healthy Weight: Obesity increases the risk of both diabetes and high blood pressure, thereby increasing kidney disease risk.
- Avoid Smoking: Smoking damages blood vessels throughout the body, including the kidneys, and exacerbates high blood pressure.
- Moderate Alcohol Intake: Excessive alcohol can harm the kidneys.
- Avoid Nephrotoxic Drugs: Be cautious with medications that can harm the kidneys, especially non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen, particularly if used long-term or in high doses, especially if you have existing kidney concerns. Always consult your doctor before taking new medications.
- Regular Medical Check-ups: Especially if you have risk factors (diabetes, high blood pressure, family history), regular blood and urine tests can detect early signs of kidney damage before symptoms appear.
2. Promote Excellent Oral Hygiene (Even Before Symptoms):
- Consistent Daily Routine: Implement a rigorous daily oral hygiene routine: brush twice daily with fluoride toothpaste, floss daily, and use a tongue scraper. This reduces the overall bacterial load in the mouth, preventing general halitosis and reducing the substrate (food debris, dead cells) for urea-to-ammonia conversion.
- Hydration: Maintain good hydration to promote healthy salivary flow, which naturally cleanses the mouth.
- Regular Dental Visits: Schedule routine dental check-ups and professional cleanings every six months (or more frequently if recommended). This allows dentists to identify and treat gum disease, cavities, and other oral infections early, preventing them from exacerbating any systemic issues.
- Address Dry Mouth: If you experience dry mouth due to medications or other factors, use saliva substitutes or stimulants as needed.

By focusing on kidney health and maintaining optimal oral hygiene, individuals can significantly reduce their risk of developing kidney disease bad breath.
Risks and Complications
The risks and complications associated with kidney disease bad breath primarily stem from the underlying kidney disease itself, but the oral manifestations can also have their own set of challenges. Ignoring persistent bad breath linked to kidney disease can lead to several adverse outcomes.
1. Complications Related to Untreated Kidney Disease:
If the bad breath is a symptom of undiagnosed or poorly managed kidney disease, the risks are severe:
- Progression to End-Stage Renal Disease (ESRD): Without proper medical intervention, kidney disease will continue to worsen, eventually leading to ESRD, requiring dialysis or a kidney transplant for survival.
- Cardiovascular Disease: Kidney disease significantly increases the risk of heart disease, heart attack, and stroke.
- Anemia: Kidneys produce erythropoietin, a hormone that stimulates red blood cell production. Kidney failure leads to anemia, causing fatigue and weakness.
- Bone Disease: Imbalances in calcium, phosphorus, and vitamin D metabolism can lead to weakened bones and increased fracture risk.
- Nerve Damage (Neuropathy): Toxin buildup can damage nerves, leading to numbness, tingling, or pain, often in the extremities.
- Fluid Overload: Leading to swelling (edema), high blood pressure, and potentially fluid in the lungs (pulmonary edema), which can be life-threatening.
- Electrolyte Imbalances: High potassium or phosphorus levels can be dangerous, affecting heart rhythm and muscle function.
- Weakened Immune System: Increased susceptibility to infections.
2. Oral Complications:
While not as immediately life-threatening as systemic complications, neglecting oral health in the context of kidney disease carries its own risks:
- Severe Oral Infections:
- Advanced Periodontal Disease: Uncontrolled gum disease can lead to tooth loss and chronic pain. The inflammation from gum disease can also contribute to systemic inflammation, potentially worsening kidney function or cardiovascular health.
- Dental Abscesses: Untreated cavities can progress to severe infections, causing pain, swelling, and potentially spreading infection to other parts of the body.
- Oral Candidiasis: Chronic dry mouth and a compromised immune system increase the risk of fungal infections (thrush), which can be painful and make eating difficult.
- Nutritional Deficiencies: Painful oral lesions, severe dry mouth, and an altered sense of taste (metallic taste) can make eating difficult and unpleasant, leading to reduced food intake and malnutrition, further complicating kidney disease management.
- Poor Quality of Life: Persistent bad breath and unpleasant taste can severely impact an individual's self-esteem, social interactions, and mental well-being, leading to social isolation and depression.
- Exacerbation of Systemic Inflammation: Oral infections release inflammatory mediators into the bloodstream. In a patient already battling systemic inflammation due to kidney disease, this can exacerbate the overall inflammatory burden and potentially worsen their medical condition.
- Medication Interactions: If dental infections require antibiotics, these must be carefully chosen and dosed by a dentist in consultation with a nephrologist, due to potential interactions or altered metabolism in kidney patients.
It's clear that kidney disease bad breath is more than just an inconvenience; it's a critical symptom that demands attention. Early detection and comprehensive management of both the kidney disease and oral health issues are vital to prevent these severe risks and complications.
Children / Pediatric Considerations
Kidney disease can affect children, sometimes even from birth (congenital kidney disease) or developing later in childhood. When it does, kidney disease bad breath can also manifest in pediatric patients, presenting unique challenges for diagnosis and management.
- Similar Causes: The underlying mechanisms for bad breath in children with kidney disease are similar to adults: accumulation of urea and ammonia (uremic fetor), dry mouth, and altered oral microbiome.
- Difficulty in Diagnosis: Young children may not be able to articulate symptoms like "metallic taste" or "dry mouth." Parents might notice a persistent, unusual odor from their child's breath, especially if it's not typical morning breath or food-related. This can be one of the earliest signs prompting a medical investigation.
- Developmental Impact: Chronic kidney disease in children can affect overall growth and development. This includes dental development, potentially leading to:
- Enamel Hypoplasia: Defects in enamel formation, resulting in thinner, pitted, or discolored enamel. This makes teeth more susceptible to cavities.
- Delayed Tooth Eruption: Teeth may emerge later than expected.
- Increased Caries Risk: A combination of enamel defects, dry mouth, altered saliva, and sometimes sugar-containing medications can significantly increase the risk of dental cavities.
- Oral Lesions: Children with kidney disease can also develop oral ulcers or inflammation, making eating and speaking uncomfortable.
- Treatment Considerations:
- Pediatric Nephrologist: Management of kidney disease in children requires a specialized pediatric nephrologist.
- Pediatric Dentist: A pediatric dentist with experience in treating medically complex patients is crucial. They can tailor oral hygiene instructions, recommend fluoride treatments, and manage any developmental or carious lesions.
- Medication Adjustments: Dosing of medications (including antibiotics for dental infections) must be carefully adjusted for a child's weight and kidney function.
- Anxiety and Cooperation: Dental visits can be more challenging for children, especially those with chronic illnesses. A gentle approach, clear explanations, and possibly sedation options may be necessary.
- Parental Role: Parents play a critical role in observing their child's breath, taste, and oral comfort, implementing daily oral hygiene, and ensuring adherence to medical and dental appointments. Early recognition of an unusual breath odor should prompt a discussion with the child's pediatrician or nephrologist.
Pro Tip for Parents: If your child has kidney disease, ensure they have regular dental check-ups starting from the eruption of their first tooth. Discuss fluoride varnish applications and dietary guidance with their pediatric dentist to protect their vulnerable teeth.
Frequently Asked Questions
What does kidney disease bad breath smell like specifically?
Kidney disease bad breath, known as uremic fetor, often has a distinctive ammonia-like, urine-like, or "fishy" odor. This is due to the buildup of urea and ammonia in the bloodstream and saliva, which are not properly filtered by failing kidneys. It's often persistent and not easily masked by typical oral hygiene.
Can bad breath be the only symptom of kidney disease?
While bad breath can be one of the earliest noticeable symptoms, it is rarely the only symptom of kidney disease, especially as the condition progresses. It often co-occurs with other signs like fatigue, swelling, changes in urination, metallic taste, or dry mouth. However, a persistent, unexplained ammonia-like breath should always prompt a medical evaluation for kidney function.
How quickly does bad breath improve after starting dialysis?
For most patients, the characteristic uremic fetor significantly improves within a few hours to a day after a dialysis session. As dialysis effectively removes accumulated toxins like urea and ammonia from the blood, their concentration in saliva decreases, leading to fresher breath. Consistent adherence to the dialysis schedule is key for sustained improvement.
Is the metallic taste always present with kidney disease bad breath?
Many individuals with kidney disease report a metallic or altered taste (dysgeusia), which often accompanies uremic fetor. This taste is also attributed to the buildup of waste products. While common, not everyone experiences it, and its intensity can vary among patients.
Are there any specific foods to avoid if I have kidney disease and bad breath?
While directly impacting bad breath, adhering to a kidney-friendly diet recommended by your nephrologist and dietitian is crucial. This typically involves managing protein intake to reduce urea production. Beyond that, avoiding strong-smelling foods like excessive garlic, onions, or certain spices might help reduce general halitosis, but it won't address the underlying uremic fetor.
Can over-the-counter mouthwashes help with kidney disease bad breath?
Over-the-counter mouthwashes, especially alcohol-free antimicrobial rinses containing ingredients like cetylpyridinium chloride (CPC) or zinc, can help reduce the general bacterial load in the mouth and mask some odors. However, they will not eliminate the uremic fetor, which originates from systemic toxins. For true improvement, the underlying kidney disease must be managed. Always choose alcohol-free options to avoid drying out the mouth further.
What is the connection between bad breath and gut health in kidney disease?
The connection is significant. In kidney disease, an imbalanced gut microbiome (dysbiosis) can lead to an increased production of uremic toxins, such as trimethylamines (which contribute to the "fishy" odor) and indoxyl sulfate, by specific gut bacteria. These toxins then enter the bloodstream and contribute to the overall uremic load, impacting breath. Research is ongoing into how modulating the gut microbiome might benefit kidney patients and their associated bad breath.
How often should someone with kidney disease see a dentist?
Individuals with kidney disease often benefit from more frequent dental check-ups and professional cleanings, typically every 3-4 months, compared to the standard six months. This allows for closer monitoring of oral health, aggressive management of plaque and tartar, and early detection and treatment of oral infections exacerbated by their condition.
Is kidney disease bad breath painful?
The bad breath itself is not painful, but the associated oral conditions often are. Dry mouth can lead to discomfort, burning sensations, and difficulty eating. Oral lesions, ulcers, or severe gum disease (periodontitis) commonly seen in kidney patients can cause significant pain, tenderness, and difficulty with chewing and speaking.
What role does dry mouth play in kidney disease bad breath?
Dry mouth (xerostomia) is a very common symptom in kidney disease, often due to medications or fluid restrictions. Reduced saliva means less natural cleansing of the mouth. This allows food particles and bacteria to accumulate, producing volatile sulfur compounds (VSCs) that contribute to general bad breath and can exacerbate the underlying uremic fetor. Managing dry mouth is therefore an important part of a comprehensive treatment plan.
When to See a Dentist
While your nephrologist will manage your kidney disease, your dentist plays a crucial role in managing the oral manifestations, including kidney disease bad breath. Knowing when to seek dental attention is vital.
Immediate Attention (Red Flags):
- Sudden onset of severe, persistent bad breath with an ammonia or fishy odor: Especially if you don't have a known kidney disease diagnosis, this warrants an immediate call to your physician or nephrologist, followed by a dental consultation.
- New or worsening oral pain, swelling, or bleeding: This could indicate a severe infection (like an abscess) or advanced gum disease, which needs urgent dental care, particularly if you have a compromised immune system due to kidney disease.
- Difficulty eating or swallowing due to oral sores, ulcers, or dry mouth: This can lead to nutritional deficiencies and significant discomfort, requiring prompt dental and potentially medical intervention.
- Signs of oral candidiasis (thrush), such as white, cottage-cheese-like patches in the mouth: This fungal infection requires specific antifungal treatment from your dentist or doctor.
Routine Care and Scheduled Appointments:
- If you have a known kidney disease diagnosis and persistent bad breath: Schedule a dental check-up promptly. Your dentist can help manage oral hygiene, address dry mouth, and treat any contributing oral conditions.
- Regular dental check-ups: Even if your bad breath is controlled, aim for more frequent dental visits (e.g., every 3-4 months) as recommended by your dental team and in consultation with your nephrologist.
- Before starting dialysis or undergoing a kidney transplant: A comprehensive dental evaluation is often recommended to clear any potential sources of infection that could complicate these medical procedures.
- Anytime you notice changes in your oral health: This includes persistent dry mouth, changes in taste, gum sensitivity, or new spots/lesions in your mouth.
Always inform your dental office about your complete medical history, especially your kidney disease diagnosis and current medications, before any appointments. This allows your dental team to provide the safest and most effective care tailored to your specific health needs.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026