Mouth Taping Sleep Apnea: Complete Guide

Key Takeaways
- Do you often wake up with a dry mouth, sore throat, or feeling as if you haven't slept at all, despite spending hours in bed? You're not alone. Millions of Americans suffer from sleep-disordered breathing, with Obstructive Sleep Apnea (OSA) affecting an estimated 22 million adults in the U.S., m
Mouth Taping Sleep Apnea: Complete Guide
Do you often wake up with a dry mouth, sore throat, or feeling as if you haven't slept at all, despite spending hours in bed? You're not alone. Millions of Americans suffer from sleep-disordered breathing, with Obstructive Sleep Apnea (OSA) affecting an estimated 22 million adults in the U.S., many of whom remain undiagnosed. While the traditional image of sleep apnea might involve loud snoring and CPAP machines, an increasing number of individuals are exploring various methods to improve their sleep and breathing, including the increasingly popular, yet controversial, practice of mouth taping sleep apnea. But is mouth taping a safe and effective solution for sleep apnea, or a risky trend? This comprehensive guide from SmilePedia.net delves deep into the topic, exploring what mouth taping entails, its purported benefits, significant risks, and medically recognized treatments for sleep apnea, such as using a CPAP mouth guard or other mouth appliance for sleep apnea. We'll help you understand the science, the concerns, and the best path forward for achieving truly restorative sleep.
Key Takeaways:
- Mouth Taping is NOT a medically recognized treatment for Obstructive Sleep Apnea (OSA). Its efficacy for OSA is unproven, and it can be dangerous.
- Primary Purpose: Mouth taping is typically used by individuals seeking to promote nasal breathing during sleep, often for habitual mouth breathing or snoring, not for diagnosed sleep apnea.
- Significant Risks: Taping can worsen sleep apnea, lead to breathing difficulties, panic, skin irritation, and is contraindicated for conditions like nasal obstruction, severe asthma, or uncontrolled sleep apnea.
- Effective Sleep Apnea Treatments: Medically proven options include Continuous Positive Airway Pressure (CPAP), Oral Appliance Therapy (OAT) (e.g., a custom mouth appliance for sleep apnea or CPAP mouth guard), lifestyle modifications, and surgery.
- Cost of Oral Appliances: Custom oral appliances typically range from $1,800 to $4,500 in the U.S., often covered by medical insurance if prescribed by a dentist and physician.
- Diagnosis is Crucial: If you suspect sleep apnea, a definitive diagnosis through a sleep study (polysomnography), costing $500-$5,000 without insurance, is essential before considering any intervention.
- Always Consult a Professional: Never attempt to self-treat sleep apnea with mouth taping. Consult your dentist and physician for proper diagnosis and a safe, effective treatment plan.
What It Is: Understanding Mouth Taping and Sleep Apnea
To understand the discussion around mouth taping sleep apnea, it's crucial to first define both components clearly.
What is Mouth Taping?
Mouth taping involves applying a small piece of specially designed, hypoallergenic tape over your lips before sleeping. The intent is to keep your mouth closed, thereby forcing you to breathe exclusively through your nose throughout the night. Proponents of mouth taping claim it can lead to a host of benefits, including reduced snoring, improved sleep quality, better oral hygiene (by preventing dry mouth), and potentially even better facial development in children. The underlying premise is that nasal breathing is the optimal and natural way to breathe, offering numerous physiological advantages over mouth breathing.
What is Sleep Apnea?
Sleep apnea is a serious sleep disorder characterized by repeated interruptions in breathing during sleep. These pauses, called apneas, can last from a few seconds to more than a minute and can occur hundreds of times per night. When breathing stops, the brain briefly rouses the person from sleep to restart breathing, often accompanied by a gasp or snort. While the individual may not remember these awakenings, they fragment sleep, preventing deep, restorative sleep.
The most common form is Obstructive Sleep Apnea (OSA), which occurs when the muscles in the back of your throat relax too much, causing the soft tissue to collapse and block the airway. Less common forms include Central Sleep Apnea (CSA), where the brain fails to send proper signals to the muscles that control breathing, and Complex Sleep Apnea, a combination of both.
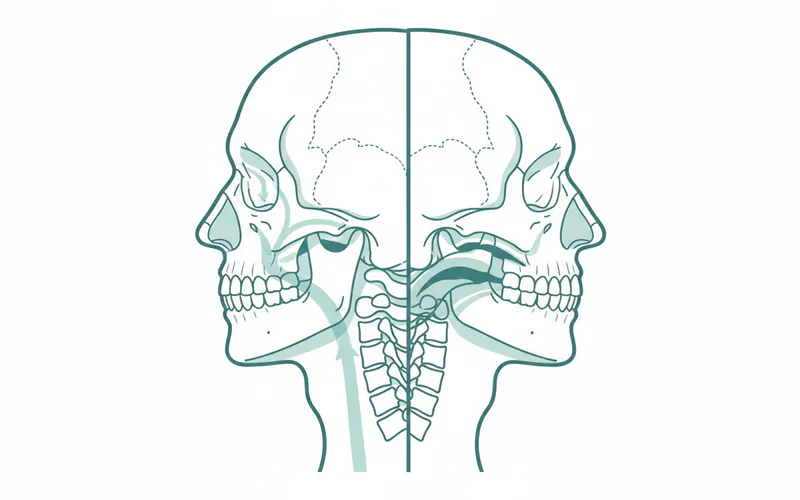
Why Mouth Taping for Sleep Apnea is a Risky Misconception
The growing interest in mouth taping sleep apnea stems from a common, but often misguided, belief that promoting nasal breathing alone can resolve the underlying mechanisms of sleep apnea. While nasal breathing is indeed superior, mouth taping does not address the root cause of OSA, which is a physical obstruction or collapse of the airway. In fact, for someone with undiagnosed or poorly managed sleep apnea, mouth taping can be counterproductive and even dangerous.
The Problem with Mouth Breathing
Chronic mouth breathing, especially during sleep, is a common issue with several negative health consequences, including:
- Dry Mouth: Leads to increased risk of cavities, gum disease, and bad breath.
- Snoring: Often exacerbates or causes snoring.
- Poor Sleep Quality: Less efficient oxygen intake.
- Facial Development Issues (in children): Can contribute to malocclusion, narrow dental arches, and other orthodontic problems.
- Exacerbation of Asthma and Allergies: Nasal breathing filters and warms air, which mouth breathing bypasses.
It is this link between mouth breathing and poor health outcomes that drives the interest in solutions like mouth taping. However, simply forcing the mouth closed does not resolve the structural issues that lead to OSA.
Types / Variations of Mouth Taping
While the core concept is simple, there are some variations in how people approach mouth taping:
- Standard Vertical Strip: A single, small strip of tape placed vertically over the center of the lips, allowing the corners of the mouth to remain untaped for slight airflow if necessary. This is often recommended for beginners.
- Horizontal Strip: A wider strip of tape applied horizontally across the entire width of the lips. This method offers more complete mouth closure but might feel more restrictive.
- "X" Shape: Two strips of tape creating an "X" over the lips.
- Porous/Hypoallergenic Tapes: Specific brands market "mouth tape" made from medical-grade, breathable, hypoallergenic materials designed for sensitive skin. These are preferred over regular household tapes.
- DIY Methods: Some people use common medical tapes like micropore tape. However, using non-specific tapes can lead to skin irritation, allergic reactions, or even difficulty removing.
Pro Tip: If considering mouth taping for general mouth breathing (and NOT sleep apnea), always opt for specialized, medical-grade mouth tape designed for this purpose. Never use duct tape, masking tape, or other non-skin-safe adhesives.
Causes / Why Sleep Apnea Happens
Understanding the causes of sleep apnea is crucial to appreciating why mouth taping is not an effective treatment.
Root Causes of Obstructive Sleep Apnea (OSA)
OSA primarily results from anatomical and physiological factors that lead to airway collapse during sleep:
- Relaxation of Throat Muscles: During sleep, muscles in the soft palate, tongue, and throat naturally relax. In individuals with OSA, this relaxation is sufficient to cause the airway to narrow or completely close.
- Excess Weight/Obesity: Extra fat deposits around the upper airway can narrow the breathing passage, making it more prone to collapse. This is a major risk factor, with studies showing a strong correlation.
- Neck Circumference: A thick neck may indicate narrower airways.
- Enlarged Tonsils or Adenoids: Especially common in children, these can physically obstruct the airway.
- Craniofacial Structure: Certain anatomical features, such as a recessed chin, narrow jaw, large tongue, or a deviation in the nasal septum, can predispose individuals to OSA.
- Alcohol and Sedatives: These substances relax throat muscles, increasing the risk of airway collapse.
- Smoking: Smokers are three times more likely to have OSA, possibly due to inflammation and fluid retention in the upper airway.
- Nasal Congestion: Chronic nasal obstruction (allergies, deviated septum) can make it difficult to breathe through the nose, leading to mouth breathing and potentially worsening OSA symptoms.
- Genetics: OSA often runs in families, suggesting a genetic predisposition.
How Mouth Breathing Relates (and doesn't) to OSA
While mouth breathing can be a symptom or a contributing factor to some issues, it is rarely the sole cause of OSA. Often, mouth breathing occurs because the nasal airway is already obstructed (e.g., allergies, deviated septum) or because the oral airway is used as a compensatory mechanism when the pharyngeal airway collapses during sleep. Forcing the mouth shut with tape without addressing the underlying nasal obstruction or pharyngeal collapse simply shifts the problem, potentially creating a complete airway blockage.
Signs and Symptoms of Sleep Apnea and Mouth Breathing
Recognizing the signs is the first step towards proper diagnosis and treatment.
Common Signs and Symptoms of Obstructive Sleep Apnea
Many symptoms occur during sleep and are often reported by a bed partner:
- Loud and Frequent Snoring: Often punctuated by silences, followed by gasps or choking sounds.
- Observed Pauses in Breathing: A bed partner might notice periods when you stop breathing.
- Daytime Sleepiness/Fatigue: Despite sleeping for seemingly enough hours, you feel excessively tired during the day.
- Morning Headaches: Due to decreased oxygen and increased carbon dioxide levels overnight.
- Dry Mouth or Sore Throat Upon Waking: Often a sign of mouth breathing during sleep.
- Irritability or Mood Changes: Resulting from chronic sleep deprivation.
- Difficulty Concentrating/Memory Problems.
- High Blood Pressure (Hypertension): OSA is a significant risk factor for cardiovascular disease.
Signs of Chronic Mouth Breathing
These can occur with or without sleep apnea:
- Chapped Lips.
- Bad Breath (Halitosis).
- Red, Swollen Gums (Gingivitis).
- Crowded Teeth or Malocclusion (especially in children, due to altered facial development).
- Frequent Ear Infections (in children).
- Allergies or Persistent Nasal Congestion.
If you or a loved one experiences any combination of these symptoms, especially loud snoring and daytime fatigue, it's critical to seek professional medical evaluation.
Treatment Options for Sleep Apnea (and the Role of Mouth Taping)
This section outlines medically recognized treatments for sleep apnea, distinguishing them clearly from mouth taping.
Medically Recognized Treatments for Obstructive Sleep Apnea
The primary goal of sleep apnea treatment is to keep the airway open during sleep.
-
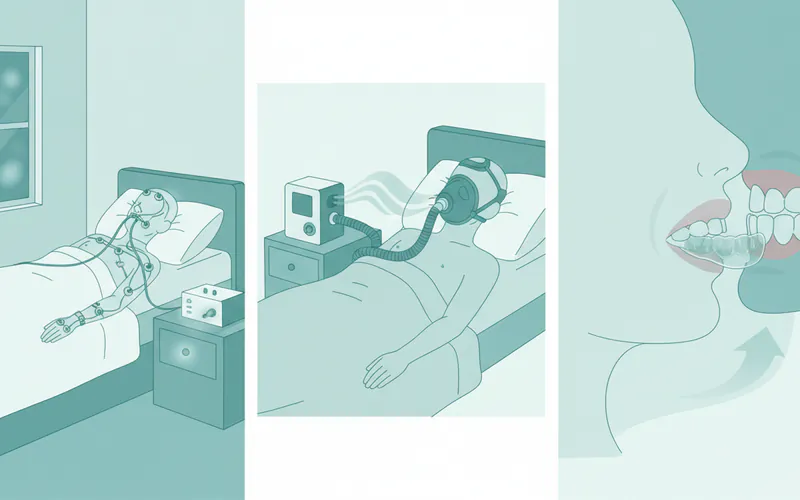
Continuous Positive Airway Pressure (CPAP):
- Description: The gold standard treatment. A machine delivers a continuous stream of air through a mask worn over the nose or nose and mouth, creating enough pressure to keep the airway open.
- Pros: Highly effective, quickly reduces symptoms and health risks.
- Cons: Can be cumbersome, uncomfortable for some (mask fit, noise, dry air), requires consistent use.
- Cost: CPAP machines range from $500 to $3,000, with masks and supplies costing $100-$500 annually. Often covered by medical insurance.
-
Oral Appliance Therapy (OAT):
- Description: A custom-fitted mouth appliance for sleep apnea, often resembling a sports mouthguard, is worn during sleep. These devices work by either repositioning the lower jaw and tongue forward (Mandibular Advancement Devices - MADs) or holding the tongue in place (Tongue Retaining Devices - TRDs), thereby keeping the airway open. These are sometimes referred to colloquially as a CPAP mouth guard, though they are distinct from CPAP and function differently.
- Pros: Non-invasive, more comfortable and portable than CPAP for many, highly effective for mild to moderate OSA.
- Cons: Not suitable for severe OSA, may cause jaw discomfort, tooth movement, or excessive salivation initially. Requires careful monitoring by a dentist specializing in sleep medicine.
- Cost: Custom oral appliances typically range from $1,800 to $4,500 in the U.S., including fitting and follow-up adjustments. Often covered by medical insurance.
-
Lifestyle Changes:
- Description: For mild OSA or as an adjunct to other therapies.
- Pros: No cost, improves overall health.
- Cons: May not be sufficient for moderate to severe OSA.
- Examples: Weight loss, avoiding alcohol and sedatives before bed, quitting smoking, sleeping on your side (positional therapy), treating nasal congestion.
-
Surgery:
- Description: Various surgical procedures can enlarge the airway, such as uvulopalatopharyngoplasty (UPPP), genial advancement, or jaw repositioning (maxillomandibular advancement).
- Pros: Can offer a permanent solution for some.
- Cons: Invasive, recovery time, not always successful, potential complications.
- Cost: Highly variable, ranging from $5,000 to $50,000+, depending on the procedure.
-
Emerging Therapies:
- Hypoglossal Nerve Stimulation: An implanted device stimulates the nerve that controls tongue movement, keeping the airway open.
- Expiratory Positive Airway Pressure (EPAP) Devices: Small, disposable devices placed at the nostrils to create back pressure during exhalation.
The Role of Mouth Taping for Sleep Apnea: CAUTION ADVISED
Let's be clear: Mouth taping is NOT a medically endorsed or proven treatment for Obstructive Sleep Apnea.
- No Scientific Evidence: There is currently no robust scientific evidence or clinical trials supporting the use of mouth taping as a safe or effective treatment for diagnosed sleep apnea. The American Dental Association (ADA) and American Academy of Sleep Medicine (AASM) do not recommend it for OSA.
- Potential Dangers: Forcing a person with OSA to breathe exclusively through their nose when their primary airway obstruction is further down the throat can be extremely dangerous. It can worsen apneas, lead to severe oxygen desaturation, and increase the risk of serious cardiovascular events.
- Misdirection: Focusing on mouth taping for sleep apnea can delay proper diagnosis and treatment with proven therapies, allowing the condition to worsen and increase health risks.
- Limited Application: At best, mouth taping might be considered by individuals with habitual mouth breathing or simple snoring (not related to OSA) and only after consultation with a doctor or dentist to rule out underlying conditions and nasal obstructions. Even then, its benefits are largely anecdotal.
Pro Tip: If you have been diagnosed with sleep apnea, or suspect you might have it, do NOT attempt to use mouth taping as a treatment. Consult with a sleep physician or a dentist specializing in sleep medicine.
Step-by-Step Process for Diagnosing and Treating Sleep Apnea
Understanding the journey from suspicion to effective treatment is vital.
1. Initial Consultation with Your Doctor/Dentist
- Symptoms Discussion: Discuss your symptoms (snoring, daytime fatigue, dry mouth, etc.) with your primary care physician or your dentist. Your dentist may be the first to notice signs like a highly vaulted palate, tongue indentations, or signs of bruxism (teeth grinding) often associated with OSA.
- Physical Examination: Examination of your mouth, throat, and neck.
- Risk Assessment: Your doctor will assess risk factors like weight, neck circumference, and family history.
2. Sleep Study (Polysomnography)
- Purpose: The definitive diagnostic tool for sleep apnea. It monitors various physiological parameters during sleep.
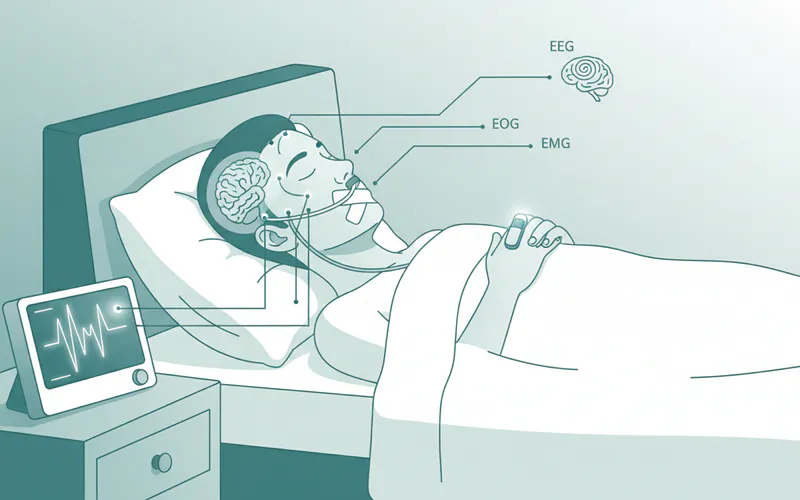
- Process:
- In-Lab Sleep Study: You'll spend a night at a sleep center. Technicians will attach sensors to your head, face, chest, and limbs to monitor: brain waves (EEG), eye movements (EOG), muscle activity (EMG), heart rate (ECG), breathing effort, airflow, blood oxygen levels (oximetry), and snoring.
- Home Sleep Apnea Test (HSAT): A portable device that you use at home. It's less comprehensive than an in-lab study but can accurately diagnose moderate to severe OSA. HSATs typically measure airflow, breathing effort, heart rate, and blood oxygen levels.
- Cost: In-lab studies range from $1,500 to $5,000+ without insurance. Home tests are generally $500 to $1,500. Most medical insurance plans cover sleep studies when medically indicated.
- Timeline: Scheduling can take weeks, results usually within 1-2 weeks after the study.
3. Diagnosis and Treatment Plan Development
- Results Interpretation: A sleep physician interprets the sleep study results, determining the presence and severity of sleep apnea (mild, moderate, or severe) based on the Apnea-Hypopnea Index (AHI).
- Personalized Plan: Based on the diagnosis, medical history, and patient preferences, the physician will recommend the most appropriate treatment, which may include CPAP, OAT, lifestyle changes, or other interventions.
4. Implementation of Treatment
- CPAP: If prescribed, you'll work with a durable medical equipment (DME) provider to select and fit a CPAP machine and mask. Initial titration studies may be needed to find the optimal pressure.
- Oral Appliance Therapy (OAT): If recommended, your general dentist or an oral sleep appliance dentist will take impressions of your teeth and jaw to fabricate a custom mouth appliance for sleep apnea. Multiple appointments are typically needed for fitting and adjustments to ensure comfort and effectiveness.
5. Follow-up and Monitoring
- Regular Check-ups: Regular follow-up with your sleep physician and dentist (for OAT users) is crucial to monitor treatment effectiveness, address any issues, and ensure long-term compliance.
- Treatment Adjustments: CPAP pressure, oral appliance settings, or other aspects of the treatment plan may need adjustments over time.
Cost and Insurance for Sleep Apnea Treatment
Understanding the financial aspect is a key concern for many patients.
Average US Price Ranges (Without Insurance)
| Treatment/Service | Low End (USD) | High End (USD) | Notes |
|---|---|---|---|
| Initial Doctor's Visit | $100 | $300 | Varies by provider and region. |
| In-Lab Sleep Study (Polysomnography) | $1,500 | $5,000+ | Can vary widely by facility, location, and comprehensiveness. |
| Home Sleep Apnea Test (HSAT) | $500 | $1,500 | More affordable, but may not be suitable for all cases. |
| CPAP Machine | $500 | $3,000 | Basic models vs. advanced models with humidifiers, data tracking. |
| CPAP Mask & Supplies (Annual) | $100 | $500 | Masks need periodic replacement (every 3-6 months). |
| Custom Oral Appliance (OAT) | $1,800 | $4,500 | Includes initial consultation, impressions, fitting, adjustments. |
| Sleep Apnea Surgery | $5,000 | $50,000+ | Highly variable depending on the specific procedure. |
| Mouth Tape (Monthly) | $10 | $30 | For specialized, medical-grade tape. (Not a medical treatment!) |
Insurance Coverage Details
- Medical Insurance: Most medical insurance plans (including Medicare and many private plans) do cover the diagnosis and treatment of sleep apnea when it is deemed medically necessary. This typically includes:
- Consultations with a sleep physician.
- Sleep studies (both in-lab and home tests).
- CPAP machines and supplies (often considered Durable Medical Equipment, DME).
- Custom oral appliances (OAT) when prescribed by a physician and fabricated by a qualified dentist.
- Dental Insurance: While oral appliances are fabricated by dentists, they are generally covered under medical insurance as a treatment for a medical condition (sleep apnea), not dental insurance. Some dental plans may offer limited coverage for oral appliances, but medical insurance is the primary payer.
- Pre-authorization: It's common for insurance companies to require pre-authorization for sleep studies, CPAP machines, and oral appliances. Always check with your insurance provider before undergoing tests or starting treatment to understand your specific coverage, deductibles, co-pays, and out-of-pocket maximums.
Payment Plans and Financing Options
For costs not covered by insurance:
- Dental/Medical Offices: Many dental and medical practices offer in-house payment plans or work with third-party financing companies (e.g., CareCredit) that provide low-interest or interest-free payment options.
- Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs): These tax-advantaged accounts can be used to pay for qualified medical expenses, including sleep apnea diagnosis and treatment.
Recovery and Aftercare for Sleep Apnea Treatment
Effective sleep apnea treatment often requires ongoing commitment and care.
For CPAP Users:
- Adaptation Period: It can take several weeks to get used to wearing the mask and sleeping with the machine. Patience is key.
- Mask Fit and Comfort: Work with your DME provider to find the most comfortable and effective mask. Poor fit can lead to leaks, skin irritation, or discomfort.
- Cleaning and Maintenance: Regularly clean your mask, tubing, and humidifier water chamber to prevent bacterial growth and maintain hygiene. Replace supplies (mask cushions, filters) as recommended.
- Troubleshooting: Address issues like dry mouth, nasal congestion, or machine noise with your sleep physician.
For Oral Appliance Therapy (OAT) Users:
- Initial Adjustments: It's normal to experience some jaw soreness, tooth tenderness, or increased salivation when first using a mouth appliance for sleep apnea. These usually subside within a few days to weeks.
- Regular Dental Check-ups: Your dentist will need to monitor the fit and effectiveness of your appliance, making adjustments as needed. This often involves follow-up appointments every 3-6 months initially, then annually.
- Oral Hygiene: Clean your appliance daily according to your dentist's instructions to prevent bacterial buildup.
- Jaw Exercises: Your dentist may recommend daily jaw exercises to prevent any permanent changes to your bite.
- Long-term Monitoring: Even with OAT, some individuals may still require periodic sleep studies to ensure the treatment remains effective over time.
For Lifestyle Changes:
- Consistent Effort: Maintaining a healthy weight, avoiding sedatives, and consistent side sleeping requires ongoing discipline.
- Nasal Health: If nasal congestion is a factor, regular use of nasal sprays, antihistamines, or addressing a deviated septum can improve nasal breathing and the efficacy of other treatments.
Prevention of Sleep Apnea and Chronic Mouth Breathing
While not all cases of sleep apnea are preventable, there are steps you can take to reduce your risk and prevent chronic mouth breathing.
Preventing Sleep Apnea:
- Maintain a Healthy Weight: Losing even a small amount of weight can significantly reduce the severity of OSA.
- Avoid Alcohol and Sedatives: Especially in the hours leading up to bedtime, as they relax throat muscles.
- Quit Smoking: Smoking increases inflammation and fluid retention in the airway.
- Sleep on Your Side: Sleeping on your back can exacerbate airway collapse.
- Address Nasal Congestion: Treat allergies, deviated septums, or chronic sinusitis to ensure clear nasal passages.
- Manage Underlying Medical Conditions: Control conditions like hypothyroidism or acid reflux, which can contribute to OSA.
Preventing Chronic Mouth Breathing (especially in children):
- Early Intervention: For children, early diagnosis and treatment of conditions like enlarged tonsils/adenoids or nasal allergies are crucial.
- Orthodontic Consultation: A pediatric dentist or orthodontist can assess craniofacial development and identify issues that may predispose a child to mouth breathing or sleep-disordered breathing. Early orthodontic intervention (e.g., palate expanders) can help create adequate space for the tongue and improve nasal breathing.
- Myofunctional Therapy: This involves exercises to strengthen oral and facial muscles and promote proper tongue posture and nasal breathing habits.
- Allergy Management: Control environmental allergies that lead to chronic nasal congestion.
Risks and Complications: Mouth Taping vs. Untreated Sleep Apnea
It's vital to differentiate the risks of an unproven home remedy from the severe complications of an untreated medical condition.
Risks and Complications of Mouth Taping (Especially for Sleep Apnea)
- Worsening Sleep Apnea: The most significant risk. Taping your mouth shut can completely obstruct your airway if you have underlying OSA, leading to dangerously low oxygen levels (hypoxemia), increased strain on the heart, and potentially severe cardiovascular events like heart attack or stroke.
- Breathing Difficulties and Panic: Waking up unable to breathe through your nose can induce extreme panic and anxiety.
- Skin Irritation: Adhesives can cause rashes, allergic reactions, or even skin tearing upon removal.
- Obstructed Nasal Breathing: If you have undiagnosed nasal congestion, allergies, or a deviated septum, mouth taping can completely block your breathing, making it impossible to get enough air.
- Delayed Diagnosis and Treatment: Relying on mouth taping can delay or prevent you from seeking proper medical diagnosis and treatment for sleep apnea, allowing the condition to progress and cause long-term health damage.
- Aspiration Risk: In rare cases, if you need to vomit during sleep, having your mouth taped shut could lead to aspiration of stomach contents into the lungs.
Contraindications for Mouth Taping (even for general mouth breathing):
- Diagnosed or suspected sleep apnea
- Nasal obstruction (deviated septum, severe allergies, chronic congestion)
- Asthma, chronic bronchitis, or other respiratory conditions
- Panic disorder or claustrophobia
- Loose teeth or gum disease
- Oral sores or injuries
- Anyone with conditions that might lead to nausea or vomiting during sleep
Risks and Complications of Untreated Obstructive Sleep Apnea
Untreated OSA is far more than just loud snoring; it's a serious medical condition with severe long-term health consequences:
- Cardiovascular Problems: High blood pressure (hypertension), heart attack, stroke, irregular heartbeats (arrhythmias), and heart failure.
- Diabetes: OSA increases insulin resistance, raising the risk of developing type 2 diabetes.
- Weight Gain: Sleep deprivation alters hormones that regulate appetite, leading to increased cravings for high-calorie foods.
- Accidents: Severe daytime sleepiness drastically increases the risk of drowsy driving accidents and workplace errors.
- Mood Disorders: Increased risk of depression and anxiety.
- Concentration and Memory Issues: Chronic sleep deprivation impairs cognitive function.
- Complications with Medications and Surgery: Untreated OSA can lead to complications with general anesthesia and certain medications.
Comparison Table: Mouth Taping vs. Medically Proven Treatments for Sleep Apnea
| Feature | Mouth Taping (for OSA) | Oral Appliance Therapy (OAT) | CPAP (Continuous Positive Airway Pressure) |
|---|---|---|---|
| Medical Efficacy | No proven efficacy for OSA. Anecdotal for mouth breathing. | Proven efficacy for mild to moderate OSA. | Gold standard, proven efficacy for all severities of OSA. |
| Mechanism | Forces nasal breathing, does not address airway collapse. | Repositions jaw/tongue to open airway. | Delivers pressurized air to keep airway open. |
| Risks | High risk (worsens OSA, panic, suffocation). | Minor side effects (jaw soreness, tooth movement, salivation). | Minor side effects (mask discomfort, dry mouth, skin irritation). |
| Cost | Low ($10-$30/month) | Moderate ($1,800-$4,500 one-time) | High ($500-$3,000 machine; $100-$500/year supplies) |
| Insurance Cov. | None | Often covered by medical insurance (with prescription). | Often covered by medical insurance (with prescription). |
| Comfort/Portability | High (if tolerated for mouth breathing) | High (custom fit, portable) | Moderate (can be bulky, noise, mask issues) |
| Professional Oversight | None (self-applied) | Required (Dentist specializing in sleep medicine, Sleep Physician) | Required (Sleep Physician, DME provider) |
| Best For | Not recommended for OSA. Only for habitual mouth breathing (with medical clearance). | Mild to moderate OSA, CPAP intolerant. | All severities of OSA. |
Children / Pediatric Considerations
Sleep apnea and mouth breathing in children are serious concerns that can have profound impacts on their development and health.

Mouth Breathing in Children
Chronic mouth breathing in children, often due to enlarged tonsils and adenoids, allergies, or a narrow upper jaw, can lead to:
- Abnormal Facial Development: Can result in a long, narrow face, recessed chin, gummy smile, and a higher arched palate (often associated with crossbites or other orthodontic issues). This is sometimes referred to as "adenoid facies."
- Dental Problems: Increased risk of cavities (due to dry mouth), gingivitis, and malocclusion (misaligned teeth).
- Poor Sleep Quality: Leads to daytime fatigue, irritability, and difficulty concentrating in school.
- Speech Issues: Can affect speech articulation.
- Behavioral Problems: Often misdiagnosed as ADHD due to hyperactivity and inattention stemming from chronic sleep deprivation.
Pediatric Sleep Apnea
Pediatric OSA affects 1-5% of children and is most commonly caused by enlarged tonsils and adenoids. Unlike adults who often present with daytime sleepiness, children with OSA may exhibit:
- Hyperactivity or Aggression.
- Difficulty in School.
- Growth Problems.
- Bedwetting.
- Frequent Night Awakenings.
- Heavy Snoring (though not all children who snore have OSA).
Guidance for Parents:
- Observe Your Child: Pay attention to snoring, gasping, pauses in breathing, or chronic mouth breathing during sleep. Also note daytime symptoms like hyperactivity, fatigue, or academic struggles.
- Consult a Pediatrician and/or Pediatric Dentist: If you have concerns, seek professional evaluation. A pediatrician can check for enlarged tonsils/adenoids or allergies. A pediatric dentist can assess craniofacial development and oral habits.
- Sleep Study: If OSA is suspected, a pediatric sleep study may be recommended.
- Treatment Options: For children, treatment often involves tonsillectomy and adenoidectomy (T&A) if enlarged tonsils/adenoids are the cause. Orthodontic interventions, such as palate expanders, can also be used to widen the dental arch and improve nasal breathing space. In some cases, CPAP may be necessary.
- Mouth Taping in Children: Absolutely NOT recommended for children. The risks of airway obstruction and psychological distress are even higher in children, and there is zero scientific basis for its use in pediatric sleep apnea.
Cost Breakdown for Sleep Apnea Diagnosis & Treatment (Summary)
To consolidate information, here's a general summary of costs. Remember, these are average ranges and can vary by region, provider, and specific patient needs.
| Item/Service | Average Low (USD) | Average Mid (USD) | Average High (USD) | With Insurance (Est. Out-of-Pocket) | Without Insurance (Est. Total) |
|---|---|---|---|---|---|
| Initial Doctor's Consultation | $100 | $200 | $300 | $0 - $100 | $100 - $300 |
| Home Sleep Apnea Test (HSAT) | $500 | $800 | $1,500 | $100 - $500 | $500 - $1,500 |
| In-Lab Sleep Study (Polysomnography) | $1,500 | $3,000 | $5,000+ | $300 - $1,500 | $1,500 - $5,000+ |
| CPAP Machine (incl. basic mask) | $500 | $1,500 | $3,000 | $200 - $1,000 | $500 - $3,000 |
| Annual CPAP Supplies (masks, filters) | $100 | $300 | $500 | $50 - $200 | $100 - $500 |
| Custom Oral Appliance (OAT) | $1,800 | $3,000 | $4,500 | $500 - $2,000 | $1,800 - $4,500 |
| Sleep Apnea Surgery (e.g., UPPP) | $5,000 | $15,000 | $50,000+ | $1,000 - $10,000+ | $5,000 - $50,000+ |
Cost-Saving Tips:
- Verify Insurance Coverage: Always contact your medical insurance provider before any tests or treatments to confirm what is covered, understand your deductible, co-pays, and out-of-pocket maximums.
- Ask for Itemized Bills: Review all charges carefully.
- Generic CPAP Masks/Supplies: Some CPAP components may have more affordable generic options.
- Consider Home Sleep Tests: If appropriate for your situation, an HSAT is significantly cheaper than an in-lab study.
- Payment Plans: Inquire about financing options or payment plans offered by dental or medical offices.
Frequently Asked Questions
Is mouth taping a safe and effective treatment for sleep apnea?
No, mouth taping is not a medically recognized or proven treatment for sleep apnea. Its efficacy is unproven, and it carries significant risks, including worsening airway obstruction and causing dangerously low oxygen levels, especially for individuals with diagnosed or undiagnosed sleep apnea.
What is the difference between mouth taping and a CPAP mouth guard or oral appliance?
Mouth taping attempts to force nasal breathing by physically closing the mouth and has no scientific backing for sleep apnea. A CPAP mouth guard is a colloquial term often used for a custom-fitted oral appliance for sleep apnea (like a Mandibular Advancement Device). These appliances are medically prescribed, custom-fabricated by a dentist, and work by repositioning the jaw or tongue to keep the airway open. They are a proven treatment for mild to moderate OSA.
How much does a mouth appliance for sleep apnea typically cost?
A custom-fitted oral appliance for sleep apnea in the U.S. generally ranges from $1,800 to $4,500. This cost usually includes the initial consultation, impressions, fabrication of the appliance, and multiple adjustment appointments with the dentist. Most medical insurance plans cover oral appliances when prescribed by a sleep physician and fabricated by a qualified dentist.
Does insurance cover oral appliance therapy for sleep apnea?
Yes, most medical insurance plans (not dental insurance) cover oral appliance therapy (OAT) for sleep apnea when it is deemed medically necessary and prescribed by a sleep physician. However, coverage details, deductibles, and co-pays can vary significantly, so it's essential to verify with your specific insurance provider.
How painful is wearing a mouth appliance for sleep apnea?
While there might be an initial adjustment period, most patients find oral appliances comfortable to wear. Some common initial side effects include mild jaw soreness, tooth tenderness, or increased salivation, which typically subside within a few days to weeks. Your dentist will make precise adjustments to ensure optimal comfort and effectiveness.
Can mouth taping help with snoring if I don't have sleep apnea?
For individuals with simple snoring caused by habitual mouth breathing and no underlying sleep apnea, mouth taping might anecdotally reduce snoring by promoting nasal breathing. However, it's crucial to first be evaluated by a medical professional to rule out sleep apnea or any nasal obstructions, as self-treating snoring without proper diagnosis can be risky.
Are there any alternatives to CPAP for sleep apnea?
Yes, absolutely. For mild to moderate sleep apnea, oral appliance therapy (OAT) using a custom mouth appliance for sleep apnea is a highly effective alternative. Other options include lifestyle modifications (weight loss, positional therapy), surgical interventions, and newer therapies like hypoglossal nerve stimulation, depending on the individual's specific condition and severity.
How long does it take to get used to a sleep apnea treatment like CPAP or an oral appliance?
The adaptation period varies for each individual. For CPAP, it can take several weeks to a few months to become fully comfortable with the mask and airflow. For an oral appliance, initial minor discomfort typically resolves within a few days to weeks as your mouth and jaw adjust to the device. Consistency and patience are key for both.
What are the dangers of leaving sleep apnea untreated?
Untreated sleep apnea carries severe health risks, including a significantly increased risk of high blood pressure, heart attack, stroke, irregular heartbeats, type 2 diabetes, and depression. It also causes chronic daytime fatigue, which can impair cognitive function and increase the risk of accidents.
Should I try mouth taping before seeing a doctor for suspected sleep apnea?
Absolutely not. If you suspect you have sleep apnea, it is imperative to seek a professional medical diagnosis from a sleep physician. Attempting to self-treat with mouth taping can mask symptoms, delay proper diagnosis, and potentially lead to dangerous complications due to airway obstruction.
When to See a Dentist
Given the nuanced relationship between mouth breathing, snoring, and sleep apnea, knowing when to consult a dental professional is crucial.
Red Flags that Warrant Immediate Dental/Medical Attention:
- Loud, chronic snoring accompanied by gasps, choking, or observed pauses in breathing during sleep.
- Severe daytime sleepiness or fatigue, despite adequate hours of sleep.
- Frequent morning headaches.
- Sudden onset of persistent dry mouth or sore throat upon waking.
- Any difficulty breathing during sleep, especially if you have tried mouth taping and experienced increased discomfort or panic.
- For children: Chronic mouth breathing, loud snoring, restless sleep, behavioral issues (hyperactivity, inattention), or slow growth.
These symptoms could indicate moderate to severe sleep apnea or another serious underlying issue that requires prompt medical evaluation.
When to Schedule a Routine Dental Appointment (and discuss concerns):
- You have chronic bad breath, even with good oral hygiene, and you suspect mouth breathing.
- You frequently wake up with a very dry mouth or chapped lips.
- Your dentist notices signs of bruxism (teeth grinding) or wear patterns on your teeth, which can be associated with sleep-disordered breathing.
- You are concerned about your child's facial development or oral habits like chronic mouth breathing.
- You are a light snorer but do not experience daytime fatigue, and you want to explore non-invasive options to reduce snoring (after sleep apnea has been ruled out by a physician).
Your dentist can be an invaluable partner in identifying potential signs of sleep apnea and guiding you toward appropriate diagnostic and treatment pathways. Many dentists specialize in dental sleep medicine and can fabricate custom oral appliances if prescribed by a sleep physician. Do not delay in seeking professional advice if you have any concerns about your sleep or breathing. Your health, and the quality of your sleep, depend on it.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
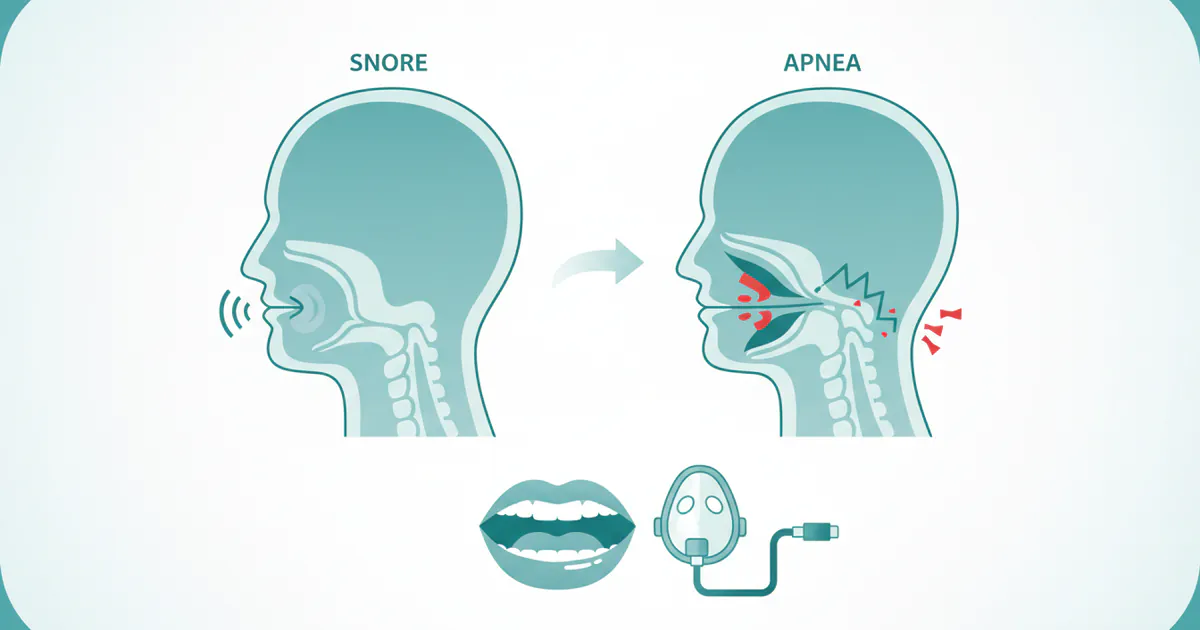
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026