Sleep Apnea Mouth Guard vs Cpap: Complete Comparison Guide
Key Takeaways
- Almost 30 million adults in the United States suffer from sleep apnea, a serious condition that goes far beyond just loud snoring. If left untreated, this disruptive sleep disorder can lead to a cascade of severe health issues, including heart disease, stroke, high blood pressure, diabetes, and
Almost 30 million adults in the United States suffer from sleep apnea, a serious condition that goes far beyond just loud snoring. If left untreated, this disruptive sleep disorder can lead to a cascade of severe health issues, including heart disease, stroke, high blood pressure, diabetes, and debilitating daytime fatigue. When faced with a sleep apnea diagnosis, many patients find themselves weighing their options, often deciding between the two most common and effective treatments: a sleep apnea mouth guard vs CPAP. This complete comparison guide from SmilePedia.net aims to provide you with an in-depth understanding of both continuous positive airway pressure (CPAP) therapy and oral appliance therapy (OAT), equipping you with the knowledge to make an informed decision for your health and well-being. We’ll delve into how each treatment works, their respective benefits and drawbacks, costs, and what you can expect from the treatment process, helping you find the path to restful, life-saving sleep.
Key Takeaways:
- CPAP is the gold standard for moderate to severe sleep apnea, offering highly effective airway support through pressurized air.
- Oral appliances (mouth guards) are a preferred alternative for mild to moderate sleep apnea or for patients intolerant to CPAP, working by repositioning the jaw.
- Cost varies significantly: A CPAP setup can range from $800-$3,000 (machine, mask, accessories), with ongoing supply costs of $300-$500 annually. Custom oral appliances typically cost $1,800-$3,500 (dental consultation, impressions, fitting, follow-ups), with minimal ongoing costs.
- Insurance coverage is common for both, but deductibles and co-pays apply. Always verify with your specific plan.
- Compliance is key: While CPAP is highly effective, adherence rates can be challenging for some. Oral appliances generally boast higher compliance due to comfort and portability.
- Consult a sleep specialist: A comprehensive sleep study is essential for diagnosis, and a sleep physician will recommend the most appropriate therapy. Dental professionals specializing in sleep dentistry create custom oral appliances.
- Trial periods are common: Many providers offer trials for CPAP masks or oral appliances to ensure patient comfort and effectiveness before final commitment.
Understanding Sleep Apnea: More Than Just Snoring
Sleep apnea is a chronic medical condition characterized by repeated pauses in breathing or shallow breaths during sleep. These interruptions can last from a few seconds to several minutes and may occur 5 to 30 times or more per hour. When breathing pauses, your brain briefly wakes you up to restart breathing, often without you even realizing it. This constant disruption prevents you from achieving deep, restorative sleep, leading to a host of health problems.
What is Sleep Apnea?
There are three main types of sleep apnea:
- Obstructive Sleep Apnea (OSA): This is the most common type, accounting for about 85-90% of cases. OSA occurs when the muscles in the back of your throat relax too much, causing the soft tissue to collapse and block the airway, despite efforts to breathe.
- Central Sleep Apnea (CSA): Less common, CSA happens when your brain fails to send the proper signals to the muscles that control breathing, leading to a temporary cessation of breathing effort.
- Mixed Sleep Apnea: A combination of both OSA and CSA.
For the purpose of this article, we will primarily focus on Obstructive Sleep Apnea, as it is the type most commonly treated with both CPAP and oral appliances.
Causes and Risk Factors
While anyone can develop sleep apnea, certain factors increase your risk:
- Obesity: Excess weight, particularly around the neck, can narrow the airway. This is the single strongest risk factor.
- Neck Circumference: A thick neck may indicate a narrower airway.
- Anatomical Features: A narrow throat, enlarged tonsils or adenoids, a deviated septum, or a small lower jaw with an overbite can predispose individuals.
- Age: The risk increases with age, though it can affect people of all ages.
- Gender: Men are two to three times more likely to have sleep apnea than women, although the risk increases for women after menopause.
- Family History: If family members have sleep apnea, you may be at higher risk.
- Alcohol and Sedatives: These substances relax the throat muscles, worsening apnea.
- Smoking: Smokers are three times more likely to have OSA, as smoking can increase inflammation and fluid retention in the upper airway.
- Nasal Congestion: Chronic nasal congestion, from allergies or anatomical issues, can make breathing difficult during sleep.
Signs and Symptoms
Recognizing the signs of sleep apnea is the first step toward diagnosis and treatment. Common symptoms include:
- Loud, chronic snoring: Often punctuated by pauses in breathing.
- Gasping or choking during sleep: Reported by a bed partner.
- Excessive daytime sleepiness (hypersomnia): Feeling tired even after a full night's sleep.
- Morning headaches.
- Difficulty concentrating or memory problems.
- Irritability or mood changes.
- Dry mouth or sore throat upon waking.
- Frequent nighttime urination (nocturia).
- High blood pressure (hypertension).
The Serious Health Risks of Untreated Sleep Apnea
Untreated sleep apnea is far more than an inconvenience; it's a significant threat to your long-term health. The repeated drops in blood oxygen levels and fragmented sleep can lead to:
- Cardiovascular Problems: Increased risk of high blood pressure, heart attack, stroke, irregular heartbeats (arrhythmias), and heart failure.
- Type 2 Diabetes: Sleep apnea can impair the body's use of insulin.
- Metabolic Syndrome: A cluster of conditions including high blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels, which increase the risk of heart disease, stroke, and diabetes.
- Fatigue-Related Accidents: Increased risk of drowsy driving accidents and workplace errors.
- Complications with Medications and Surgery: Patients with sleep apnea are at higher risk of complications from general anesthesia and certain medications.
CPAP Therapy: The Gold Standard for Sleep Apnea Treatment
Continuous Positive Airway Pressure (CPAP) therapy is widely recognized as the most effective and often the first-line treatment for moderate to severe Obstructive Sleep Apnea. It works by providing a continuous stream of pressurized air through a mask, keeping the airway open during sleep.
What is CPAP?
A CPAP machine consists of a small bedside unit that generates air pressure, a hose that connects the machine to a mask, and the mask itself, which is worn over the nose, mouth, or both. The constant stream of air acts as a "pneumatic splint," preventing the collapse of the soft tissues in the throat that characterize OSA.
Types of CPAP Devices
While "CPAP" is a general term, there are variations:
- Standard CPAP: Delivers a constant, single pressure throughout the night.
- APAP (Automatic Positive Airway Pressure): Automatically adjusts the air pressure throughout the night based on your breathing patterns, providing just enough pressure to keep the airway open. This can be more comfortable for some.
- BiPAP (Bilevel Positive Airway Pressure) / VPAP: Delivers two distinct pressures – a higher pressure during inhalation and a lower pressure during exhalation. Often prescribed for individuals who can't tolerate CPAP, or those with central sleep apnea or other respiratory conditions.
Understanding CPAP Masks
Choosing the right mask is crucial for comfort and compliance. CPAP masks come in various styles:
- Nasal Pillows: Small cushions that fit directly into the nostrils. They are lightweight and offer a clear field of vision, ideal for claustrophobic individuals or those who wear glasses.
- Nasal Masks: Cover the entire nose. They create a seal around the nose and are a good option for people who breathe primarily through their nose but need more coverage than nasal pillows provide.
- Full-Face Masks: Cover both the nose and mouth. These are particularly beneficial for CPAP masks for mouth breathers, individuals with chronic nasal congestion, or those who consistently open their mouth during sleep. While larger, modern designs are often lightweight and designed for comfort.
The CPAP Treatment Process
- Diagnosis: Begins with a visit to a sleep specialist or primary care doctor, followed by a sleep study (polysomnography) performed overnight in a lab or at home. The study measures various physiological parameters to diagnose sleep apnea and determine its severity (measured by AHI - Apnea-Hypopnea Index).
- Prescription: If sleep apnea is diagnosed, a sleep physician will prescribe CPAP therapy, specifying the pressure settings.
- Titration Study (if applicable): Sometimes, a second sleep study is done to determine the optimal pressure setting for your CPAP machine.
- Machine Setup and Mask Fitting: You'll work with a CPAP provider to select the most comfortable and effective mask. They will demonstrate how to use and clean the equipment.
- Acclimation and Follow-up: It can take time to adjust to CPAP therapy. Regular follow-ups with your physician are essential to monitor progress and address any issues. Modern CPAP machines often have data tracking capabilities that your doctor can review remotely.
Pros and Cons of CPAP
Pros:
- Highly Effective: Considered the gold standard, it effectively eliminates apneas and hypopneas for most users.
- Reduces Health Risks: Significantly lowers the risk of cardiovascular disease, stroke, and other sleep apnea-related complications.
- Immediate Symptom Relief: Many users experience improved sleep quality and reduced daytime fatigue quickly.
- Non-Invasive (relatively): No surgery or medications involved.
Cons:
- Compliance Issues: Some find the mask uncomfortable, noisy, or claustrophobic, leading to inconsistent use.
- Side Effects: Dry mouth/nose, skin irritation from the mask, nasal congestion, mask leaks, and aerophagia (swallowing air). Humidifiers can help with dryness.
- Portability: Can be cumbersome for travel, though travel-sized machines exist.
- Noise: While modern machines are quiet, some people are sensitive to the low hum.
- Maintenance: Requires regular cleaning and replacement of supplies (masks, filters, tubing).
Cost and Insurance for CPAP
The cost of CPAP therapy in the US can vary significantly based on the machine type, mask, and whether you purchase or rent.
- CPAP Machine: A basic standard CPAP machine can range from $250-$800. Auto-CPAP (APAP) and BiPAP machines are generally more expensive, $800-$2,500+.
- CPAP Mask: Masks range from $80-$250, depending on the type and brand.
- Accessories & Supplies: Humidifiers (often integrated), tubing, filters, headgear, and cleaning supplies can add $100-$300 initially and require ongoing replacement.
- Ongoing Costs: Masks should be replaced every 3-6 months, cushions monthly, filters every 2-4 weeks, and tubing every 6-12 months. This amounts to roughly $300-$500 annually for supplies.
Insurance Coverage: Most health insurance plans, including Medicare and Medicaid, cover CPAP therapy if medically necessary. However, they typically require a formal diagnosis via a sleep study and a physician's prescription.
- Deductibles and Co-pays: You will likely be responsible for meeting your deductible and paying co-pays.
- Rental Programs: Many insurance companies initially cover CPAP as a rental for 3-13 months before you own it, to ensure compliance. If you stop using it, they may stop coverage.
- Out-of-pocket: Without insurance, you could easily spend $800-$3,000 or more upfront, plus ongoing supply costs.
CPAP Aftercare and Maintenance
Proper cleaning and maintenance are vital for effective and hygienic CPAP therapy.
- Daily Cleaning: Wash your mask cushion and humidifying chamber with mild soap and water daily.
- Weekly Cleaning: Wash the mask frame, headgear, and tubing weekly.
- Filter Replacement: Replace disposable filters every 2-4 weeks. Non-disposable filters should be cleaned monthly.
- Component Replacement: Replace masks and headgear every 3-6 months, and tubing every 6-12 months.
- Regular Check-ups: Continue follow-up appointments with your sleep physician to review data, adjust settings, and address any issues.
Oral Appliance Therapy: The Sleep Apnea Mouth Guard
For many individuals with mild to moderate obstructive sleep apnea, or for those who cannot tolerate CPAP, a sleep apnea mouth guard (also known as an oral appliance) offers an effective, discreet, and portable treatment option. These custom-fitted devices are worn in the mouth during sleep, similar to a sports mouthguard or orthodontic retainer.
What is an Oral Appliance?
An oral appliance for sleep apnea is a custom-made dental device designed to keep the airway open by repositioning the jaw, tongue, or both. It works by preventing the soft tissues in the throat from collapsing and obstructing breathing. Oral appliance therapy (OAT) is recognized by the American Academy of Sleep Medicine (AASM) as a first-line treatment for mild to moderate OSA and a viable alternative for patients with severe OSA who are unable to use CPAP.
Types of Sleep Apnea Mouth Guards
There are two primary types of custom oral appliances:
- Mandibular Advancement Devices (MADs): These are the most common type. MADs work by gently pushing the lower jaw (mandible) forward and down. This slight forward movement pulls the base of the tongue and other soft tissues away from the back of the throat, opening the airway. Most MADs are adjustable, allowing a sleep dentist to fine-tune the degree of jaw advancement for optimal effectiveness and comfort.
- Tongue Retaining Devices (TRDs): TRDs work by holding the tongue in a forward position using a suction bulb. This prevents the tongue from falling back into the throat and blocking the airway. TRDs are often recommended for patients who cannot tolerate a MAD due to specific dental issues or TMJ problems.
Pro Tip: Avoid over-the-counter (OTC) boil-and-bite mouthguards marketed for snoring. While some may offer temporary relief for simple snoring, they are not medically approved or fitted for sleep apnea. They can be ineffective, uncomfortable, and potentially cause jaw problems or tooth misalignment if used long-term without professional supervision. A custom-made device from a qualified sleep dentist is crucial for safety and efficacy.
The Oral Appliance Treatment Process
- Diagnosis: Similar to CPAP, the process begins with a formal diagnosis of sleep apnea via a sleep study.
- Dental Consultation: If OAT is deemed appropriate, you will be referred to a dentist specializing in sleep medicine. They will conduct a thorough oral examination, including assessing your jaw, teeth, and airway, and taking X-rays or 3D scans.
- Impressions and Fabrication: The dentist will take impressions or digital scans of your teeth and mouth. These are sent to a dental lab to custom-fabricate your appliance. This ensures a precise, comfortable fit.
- Fitting and Adjustment: Once the appliance is ready (typically 2-4 weeks), you will return for a fitting. The dentist will ensure it fits properly and comfortably. For MADs, initial adjustments may be made to advance the jaw slightly.
- Titration and Follow-up: You'll wear the appliance at home, and the dentist will gradually adjust the jaw advancement over several weeks or months, based on your comfort and symptom improvement. A follow-up sleep study or home sleep test may be recommended to confirm the appliance's effectiveness. Regular follow-up appointments are critical to monitor progress and address any dental changes.
Pros and Cons of Sleep Apnea Mouth Guards
Pros:
- Comfortable and Less Invasive: Generally well-tolerated, discreet, and easy to wear.
- Portable: Small, lightweight, and ideal for travel.
- Quiet: No machinery noise.
- High Compliance: Patients often find it easier to use consistently than CPAP.
- Effective for Snoring: A mouth piece to stop snoring is a common and effective benefit even for non-apneic snoring.
- No Electricity Needed: Can be used anywhere.
Cons:
- Less Effective for Severe OSA: While some severe cases can benefit, OAT is generally not as effective as CPAP for very high AHI scores.
- Potential Side Effects: Jaw soreness (TMJ issues), tooth movement, changes in bite, increased salivation or dry mouth, and gum irritation. These are usually mild and manageable, often resolving with continued use or adjustments.
- Not a Cure: Like CPAP, it manages symptoms but doesn't cure the underlying condition.
- Requires Regular Dental Visits: Ongoing follow-ups with a sleep dentist are necessary to monitor the fit and ensure dental health.
- Maintenance: Requires daily cleaning and careful handling.
Cost and Insurance for Oral Appliances
The cost of a custom sleep apnea mouth guard (oral appliance) is an investment in your health, reflecting the specialized dental expertise and custom fabrication.
- Initial Consultation & Exam: $150-$400, may include X-rays and imaging.
- Custom Oral Appliance: $1,800-$3,500. This fee typically includes impressions, the device fabrication, multiple fitting appointments, and initial adjustment visits. Prices can vary geographically and by the complexity of the device.
- Follow-up Adjustments: May be included in the initial cost for a certain period, or charged separately at $50-$150 per visit.
- Replacement: Appliances typically last 3-5 years, requiring replacement due to wear and tear or changes in your oral anatomy.
Insurance Coverage: Many medical insurance plans now cover oral appliance therapy for OSA if it's medically prescribed and fabricated by a qualified dentist.
- Medical Insurance, Not Dental: Crucially, OAT is typically covered under your medical insurance benefits, not your dental insurance. This is because it treats a medical condition.
- Prior Authorization: Your insurance company will likely require prior authorization, a sleep study diagnosis, and a physician's prescription.
- Deductibles and Co-insurance: You'll be responsible for your deductible and co-insurance percentages, which could range from 20-50% of the total cost.
- Medicare: Medicare Part B may cover oral appliances under specific conditions if prescribed by a physician and provided by an approved supplier.
Mouth Guard Aftercare and Maintenance
Caring for your oral appliance ensures its longevity and effectiveness.
- Daily Cleaning: Clean your appliance daily with a soft toothbrush and non-abrasive soap or denture cleaner. Rinse thoroughly.
- Storage: Store it in its protective case when not in use to prevent damage and keep it clean.
- Avoid Heat: Never expose the appliance to hot water, direct sunlight, or extreme heat, as this can warp the plastic.
- Regular Dental Check-ups: Continue seeing your sleep dentist and general dentist regularly (typically every 6 months for general dental health, and annually for the sleep appliance) to monitor fit, efficacy, and check for any dental or jaw changes. The ADA recommends regular dental visits for OAT patients.
Sleep Apnea Mouth Guard vs CPAP: A Head-to-Head Comparison
Choosing between a sleep apnea mouth guard and CPAP can be a complex decision, often influenced by the severity of your sleep apnea, personal preferences, lifestyle, and tolerance for each device. Here's a detailed comparison to help clarify the differences.
Efficacy and Severity
- CPAP: Unquestionably the most effective treatment, especially for moderate to severe OSA. It can virtually eliminate apneas and hypopneas, significantly reducing AHI scores. Its consistent, customizable air pressure ensures a consistently open airway.
- Oral Appliance: Highly effective for mild to moderate OSA. Studies show it can reduce AHI by 50% or more and often normalize breathing for these patients. For severe OSA, it's considered a second-line option for those who cannot tolerate or fail CPAP. Its effectiveness can vary more between individuals.
Comfort and Portability
- CPAP: Comfort is highly individual and depends heavily on mask fit. Some find the mask, tubing, and air pressure intrusive or claustrophobic. Portability is a drawback for many; while travel CPAP machines exist, the equipment is still bulkier than an oral appliance and requires an electrical outlet.
- Oral Appliance: Generally considered more comfortable and less intrusive, as it's small, worn inside the mouth, and silent. It's highly portable, fitting into a small case, making it ideal for travel and camping.
Compliance Rates
- CPAP: While highly effective, average compliance rates (using it for at least 4 hours per night, 70% of nights) hover around 50-70%. Challenges include mask discomfort, skin irritation, air pressure intolerance, and claustrophobia.
- Oral Appliance: Often boasts higher compliance rates, frequently above 70%, primarily due to its comfort, ease of use, and portability. Patients tend to be more willing to use a small, quiet device every night.
Side Effects and Risks
- CPAP: Common side effects include dry mouth/nose (can be mitigated with humidifiers), mask leaks, skin irritation, and nasal congestion. Rarely, aerophagia (swallowing air) can cause bloating. Risks are generally low and mostly related to discomfort or non-compliance.
- Oral Appliance: Potential side effects include jaw soreness, temporomandibular joint (TMJ) discomfort, tooth movement, changes in bite alignment, and increased salivation or dry mouth. These are usually manageable with adjustments by the sleep dentist. Long-term use requires ongoing monitoring for permanent bite changes.
Cost Comparison (Initial vs. Ongoing)
Table 1: CPAP vs. Oral Appliance Therapy Comparison
| Feature | CPAP Therapy (Continuous Positive Airway Pressure) | Oral Appliance Therapy (OAT) / Sleep Apnea Mouth Guard |
|---|---|---|
| Primary Mechanism | Delivers pressurized air to keep airway open | Repositions jaw/tongue to open airway |
| Target Severity | Moderate to severe OSA; also for mild if other treatments fail | Mild to moderate OSA; severe OSA (if CPAP intolerant) |
| Effectiveness | Gold standard, very high efficacy (can normalize AHI for most) | High efficacy for mild/moderate; variable for severe |
| Comfort | Highly individual, potential for mask discomfort, noise, claustrophobia | Generally high, discreet, silent |
| Portability | Moderate (requires power, travel machines exist) | Excellent (small, no power needed) |
| Compliance Rates | 50-70% (can be challenging for some) | Often >70% (due to comfort and ease of use) |
| Common Side Effects | Dry mouth/nose, mask leaks, skin irritation, nasal congestion | Jaw soreness, tooth movement, bite changes, salivation |
| Professional | Sleep Physician (diagnosis, prescription, monitoring); Durable Medical Equipment (DME) Provider | Sleep Dentist (fitting, adjustments, follow-up); Sleep Physician (diagnosis) |
| Maintenance | Daily cleaning, frequent replacement of masks, filters, tubing | Daily cleaning, annual dental check-ups for appliance integrity |
Table 2: Estimated Costs: CPAP vs. Oral Appliance (US)
| Cost Component | CPAP Therapy (Typical Range) | Oral Appliance Therapy (Typical Range) |
|---|---|---|
| Sleep Study (Diagnostic) | $300-$5,000 (Home Sleep Test: $300-$600; In-lab PSG: $1,000-$5,000) | $300-$5,000 (Same as CPAP, required for diagnosis) |
| Initial Device | $250-$2,500+ (Machine only, APAP/BiPAP higher) | $1,800-$3,500 (Custom fabrication, fitting, initial adjustments) |
| Masks/Accessories (Initial) | $80-$250 (First mask) | N/A (included in device cost) |
| Ongoing Supplies (Annual) | $300-$500 (Masks, cushions, filters, tubing replacements) | $50-$150 (Annual check-up/adjustment, occasional cleaning supplies) |
| Professional Visits | Follow-ups with Sleep Physician (variable co-pays) | Follow-ups with Sleep Dentist (variable co-pays for adjustments/monitoring) |
| Total Initial Outlay (approx.) | $800-$3,000 (without insurance) | $2,100-$3,900 (without insurance, including initial exam) |
| Typical Lifespan | Machine: 3-5 years; Masks: 3-6 months | Appliance: 3-5 years |

Beyond CPAP and Oral Appliances: Other Treatment Considerations
While CPAP and oral appliances are the most common treatments, other options exist, either as standalone therapies or in conjunction with primary treatments.
Lifestyle Modifications
Often the first recommendation, lifestyle changes can significantly improve or even resolve mild sleep apnea:
- Weight Loss: Even a modest weight reduction can decrease the severity of OSA.
- Avoid Alcohol and Sedatives: Especially before bed, as they relax throat muscles.
- Change Sleep Position: Sleeping on your side instead of your back can prevent the tongue and soft palate from falling back and blocking the airway. Positional therapy devices can help.
- Quit Smoking: Smoking contributes to inflammation and fluid retention in the airway.
- Treat Nasal Congestion: Address allergies or anatomical issues that cause chronic stuffiness.
Surgical Options
Surgical interventions are generally considered when other treatments have failed or are not tolerated, and they address specific anatomical obstructions. They are more invasive and carry higher risks.
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the back of the throat, including the uvula, tonsils, and part of the soft palate. Effectiveness varies.
- Genioglossus Advancement: Tightens the tendon that connects the tongue to the lower jaw, preventing the tongue from falling back.
- Maxillomandibular Advancement (MMA): A more aggressive surgery that moves both the upper and lower jaws forward, significantly enlarging the airway. Highly effective but involves extensive recovery.
- Inspire Upper Airway Stimulation: An implanted device that monitors breathing and delivers mild stimulation to the hypoglossal nerve, moving the tongue forward during sleep. Approved for moderate to severe OSA in patients who can't use CPAP.
- Tonsillectomy and Adenoidectomy: Often curative for children with OSA caused by enlarged tonsils/adenoids, and sometimes helpful for adults.
Preventing Sleep Apnea: Proactive Steps for Better Sleep
While not always entirely preventable, especially if genetic or anatomical factors are involved, certain proactive steps can reduce your risk of developing sleep apnea or lessen its severity.
Healthy Lifestyle Choices
- Maintain a Healthy Weight: This is the most significant preventable risk factor. A balanced diet and regular exercise can make a substantial difference.
- Limit Alcohol and Sedatives: Especially in the hours leading up to bedtime.
- Quit Smoking: Eliminates a major irritant and inflammatory factor in the airway.
- Establish a Regular Sleep Schedule: Consistent sleep patterns promote better overall sleep health.
- Avoid Sleeping on Your Back: Train yourself to sleep on your side using pillows or positional devices.
Addressing Underlying Health Conditions
- Manage Allergies and Nasal Congestion: Treat chronic stuffiness that can force mouth breathing and exacerbate apnea.
- Control Blood Pressure and Diabetes: These conditions are often linked to sleep apnea and managing them can improve overall health and potentially sleep apnea severity.
Risks and Complications of Sleep Apnea Treatments
While both CPAP and oral appliance therapy are generally safe and effective, it's important to be aware of potential side effects and complications.
CPAP-Related Complications
- Mask Leaks: The most common problem, reducing effectiveness and causing noise. Can be addressed by trying different masks or adjusting fit.
- Skin Irritation/Pressure Sores: From tight mask straps or improper fit.
- Dry Mouth/Nose and Nasal Congestion: The continuous airflow can dry out airways. Humidifiers and heated tubing are often used to combat this.
- Aerophagia (Swallowing Air): Can lead to bloating, gas, and stomach discomfort. Adjusting pressure or trying APAP/BiPAP can help.
- Claustrophobia: Some individuals struggle with the feeling of wearing a mask. Nasal pillow masks or desensitization techniques can be helpful.
Oral Appliance-Related Complications
- Jaw Discomfort (TMJ issues): Especially in the initial weeks. Most resolve as the jaw adapts; persistent pain requires adjustment by the sleep dentist.
- Tooth Movement: Over long periods, the constant pressure can cause minor shifts in tooth position or bite changes. Regular dental check-ups are crucial to monitor this.
- Increased Salivation or Dry Mouth: Some people experience one or the other, often temporary.
- Gum or Tooth Sensitivity: Can occur initially but usually subsides.
- Difficulty Speaking or Swallowing: While wearing the device, which is usually only during sleep, so not a major concern.
Children / Pediatric Considerations
Sleep apnea isn't just an adult problem; it affects children too, with an estimated 1-4% of children having OSA. Pediatric sleep apnea can have serious consequences on a child's development, behavior, and academic performance.
- Signs in Children: May differ from adults. Look for loud snoring, gasping, pauses in breathing, restless sleep, mouth breathing, bedwetting, morning headaches, difficulty waking up, hyperactivity, difficulty concentrating, and poor school performance.
- Causes in Children: Enlarged tonsils and adenoids are the most common cause. Obesity is also a growing factor. Other causes include cranioiofacial abnormalities (e.g., small jaw, cleft palate) or neuromuscular disorders.
- Diagnosis: Requires a thorough evaluation by a pediatric sleep specialist and typically an overnight sleep study.
- Treatment Options for Children:
- Tonsillectomy and Adenoidectomy: Often the first-line and curative treatment for children with enlarged tonsils/adenoids.
- Orthodontic Expansion: For children with narrow palates, orthodontists can expand the upper jaw, which can widen the airway.
- CPAP: Used for children who do not respond to surgery, those with severe OSA, or those with underlying medical conditions. Pediatric-sized masks and lower pressure settings are used.
- Oral Appliances: Custom-made oral appliances may be an option for older children or adolescents, especially when anatomical factors other than tonsils/adenoids are at play, or when CPAP isn't tolerated. These are carefully designed to accommodate growth and development.
- Lifestyle Modifications: Weight management and addressing allergies are also important.
Parents who suspect their child may have sleep apnea should consult their pediatrician who can refer them to a pediatric sleep specialist. Early diagnosis and treatment are crucial to prevent long-term health and developmental issues.
Cost Breakdown: Financial Aspects of Sleep Apnea Treatment
Understanding the financial implications of sleep apnea treatment is a key part of the decision-making process. As detailed in the comparison tables, costs vary, but here's a consolidated view.
Average US Costs (Low, Mid, High)
- Diagnostic Sleep Study:
- Home Sleep Test: $300-$600 (lower cost, often first step)
- In-lab Polysomnography: $1,000-$5,000 (more comprehensive, but expensive)
- CPAP Therapy (Initial Setup):
- Low (Basic CPAP, standard mask): $500-$1,000
- Mid (APAP, quality mask): $1,000-$1,800
- High (BiPAP, premium mask, humidifier): $1,800-$3,000+
- Oral Appliance Therapy (Custom):
- Typical Range: $1,800-$3,500 (includes consultation, impressions, device, fitting, and initial adjustments)
With vs. Without Insurance
- With Insurance: Most medical insurance plans (including Medicare and Medicaid) cover sleep apnea diagnosis and treatment as medically necessary.
- You will be responsible for your deductible (which could be several hundred to several thousand dollars annually), co-insurance (a percentage of the cost after deductible, typically 10-50%), and co-pays for office visits.
- For example, if your deductible is $1,000 and your oral appliance costs $2,500, you'd pay the first $1,000, then perhaps 20% of the remaining $1,500 ($300), for a total out-of-pocket of $1,300.
- Without Insurance: You will pay the full cash price. Many clinics and DME providers offer discounts for self-pay patients. Budget for the higher end of the ranges mentioned above.
Payment Plans and Financing Options
Many dental and sleep clinics, as well as Durable Medical Equipment (DME) providers, understand the financial burden and offer solutions:
- In-house Payment Plans: Some providers allow you to pay in installments over several months.
- Third-Party Financing: Options like CareCredit, LendingClub, or similar medical credit cards offer low or no-interest financing for qualified individuals over a set period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts can be used to pay for sleep apnea diagnosis and treatment expenses.
Cost-Saving Tips
- Verify Insurance Coverage: Always call your medical insurance provider before starting treatment to understand your benefits, deductibles, co-pays, and whether prior authorization is needed. Confirm if they cover both CPAP and oral appliances, and under what conditions.
- Shop Around: For CPAP equipment and supplies, prices can vary between DME providers and online retailers.
- Ask About Self-Pay Discounts: If uninsured or with a high deductible, ask providers for cash-pay discounts.
- Consider Renting First: Some CPAP providers offer rental programs, which can be less expensive upfront, especially if you're unsure about long-term compliance.
- Buy Generic Supplies: For CPAP, generic masks, filters, and tubing can sometimes be less expensive than brand-name versions.
- Maximize FSA/HSA: Plan your contributions to these accounts to cover anticipated medical expenses.
Frequently Asked Questions
Is a sleep apnea mouth guard as effective as CPAP?
A custom sleep apnea mouth guard (oral appliance) is highly effective for mild to moderate obstructive sleep apnea, often normalizing breathing. For severe OSA, CPAP remains the gold standard. While a mouth guard may not be as effective as CPAP for every case, it's a strong alternative for many, especially those who struggle with CPAP use, and often achieves similar positive health outcomes for appropriate candidates.
Can a mouthguard really stop snoring?
Yes, a custom-fitted oral appliance designed to advance the lower jaw or hold the tongue forward can be very effective at stopping or significantly reducing snoring. Snoring often occurs when soft tissues vibrate in a partially obstructed airway; by opening the airway, a mouth guard prevents these vibrations. Even for individuals without sleep apnea, a custom mouth piece to stop snoring can provide substantial relief.
How long does it take to get used to a sleep apnea mouth guard?
Most patients adjust to wearing a sleep apnea mouth guard within a few days to a few weeks. Initial side effects like jaw soreness, increased salivation, or tooth sensitivity typically subside as your mouth and jaw adapt. Your sleep dentist will provide guidance and make adjustments to ensure comfort and effectiveness.
What are the main reasons people choose a mouth guard over CPAP?
People often choose a sleep apnea mouth guard due to its portability, comfort, silence, and discreet nature. It's an excellent option for travelers, those with claustrophobia, individuals sensitive to air pressure, or those who find CPAP masks and tubing cumbersome. It generally has higher long-term compliance rates compared to CPAP.
Is a CPAP mask comfortable for mouth breathers?
Yes, there are specific CPAP masks for mouth breathers designed to provide comfort and effectiveness. Full-face masks cover both the nose and mouth, ensuring that air pressure is delivered even if you breathe through your mouth. Some nasal masks can be used with a chin strap to keep the mouth closed, but full-face masks are generally the most reliable solution for consistent mouth breathing.
Will insurance cover a sleep apnea mouth guard?
Many medical insurance plans, including Medicare, do cover custom-made oral appliances for obstructive sleep apnea if it's prescribed by a physician and fabricated by a qualified dentist. It's crucial to confirm coverage with your specific insurance provider, as prior authorization and a sleep study diagnosis are usually required. Remember, it's typically covered under medical, not dental, benefits.
Can I try a mouth guard before committing to CPAP?
Yes, for mild to moderate obstructive sleep apnea, many sleep physicians will offer oral appliance therapy as an initial treatment option. It's a common pathway for patients who prefer a less invasive solution or those for whom CPAP is not suitable. A sleep study is always necessary for diagnosis regardless of the chosen treatment path.
What happens if I stop using my sleep apnea treatment?
Stopping treatment, whether CPAP or an oral appliance, means your sleep apnea symptoms and associated health risks will likely return. This includes snoring, daytime fatigue, and increased risk of serious conditions like heart disease, stroke, and diabetes. Consistent adherence to your prescribed therapy is vital for managing the condition and protecting your health.
How often do I need to replace my CPAP machine and mask?
CPAP machines are typically replaced every 3-5 years, depending on insurance coverage and usage. Masks, headgear, and cushions need more frequent replacement: mask cushions usually monthly, entire masks and headgear every 3-6 months, and tubing every 6-12 months. Filters are replaced every 2-4 weeks or monthly.
Are there any permanent solutions for sleep apnea?
While lifestyle changes can sometimes resolve mild sleep apnea, especially weight loss, and tonsillectomy/adenoidectomy can cure many children, most adult sleep apnea treatments manage the condition rather than cure it permanently. Surgical options exist for adults but are not always 100% effective or without risk, and are typically reserved for specific anatomical issues or when other treatments fail.
When to See a Dentist or Sleep Specialist
Recognizing when to seek professional help is paramount for managing sleep apnea and protecting your health.
You should see a dentist specializing in sleep medicine if:
- You've been diagnosed with mild to moderate obstructive sleep apnea and are seeking an alternative to CPAP.
- You've tried CPAP but can't tolerate it due to discomfort, claustrophobia, or other side effects.
- You experience chronic snoring, even if you don't have a formal sleep apnea diagnosis, and are looking for a mouth piece to stop snoring.
- You have an existing oral appliance and notice it's no longer comfortable, effective, or shows signs of wear and tear.
- You experience new jaw pain, tooth sensitivity, or bite changes after starting oral appliance therapy.
You should see a sleep specialist (sleep physician) if:
- You or your bed partner suspect you have sleep apnea (e.g., loud snoring, gasping, daytime fatigue). This is the first and most crucial step for diagnosis.
- You have been diagnosed with moderate to severe obstructive sleep apnea and require a CPAP prescription or advice on management.
- You've been using CPAP or an oral appliance, but your symptoms haven't improved, or you're experiencing new problems with your treatment.
- You have other health conditions (high blood pressure, diabetes, heart disease) that are exacerbated by poor sleep or could be linked to undiagnosed sleep apnea.
- Your child exhibits signs of sleep apnea, such as loud snoring, restless sleep, or behavioral issues.
Don't ignore the signs of sleep apnea. Early diagnosis and appropriate treatment, whether it's a sleep apnea mouth guard, CPAP, or a combination of therapies, can dramatically improve your quality of life and safeguard your long-term health. Consult with a qualified healthcare professional on SmilePedia.net to determine the best path for you.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
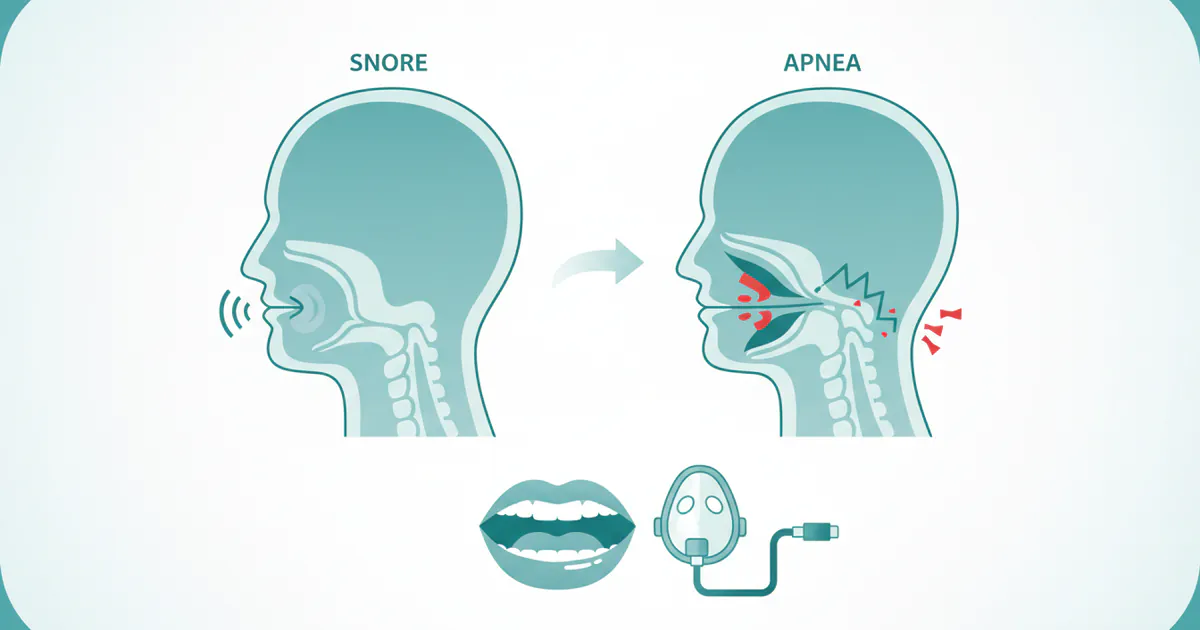
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026