Botox for Jaw Clenching: Complete Guide
Key Takeaways
- Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. An estimated one in three adults experiences bruxism, the medical term for teeth grinding or jaw clenching, with a significant percentage doing so unconsciously during sleep. While some mig
Botox for Jaw Clenching: Complete Guide
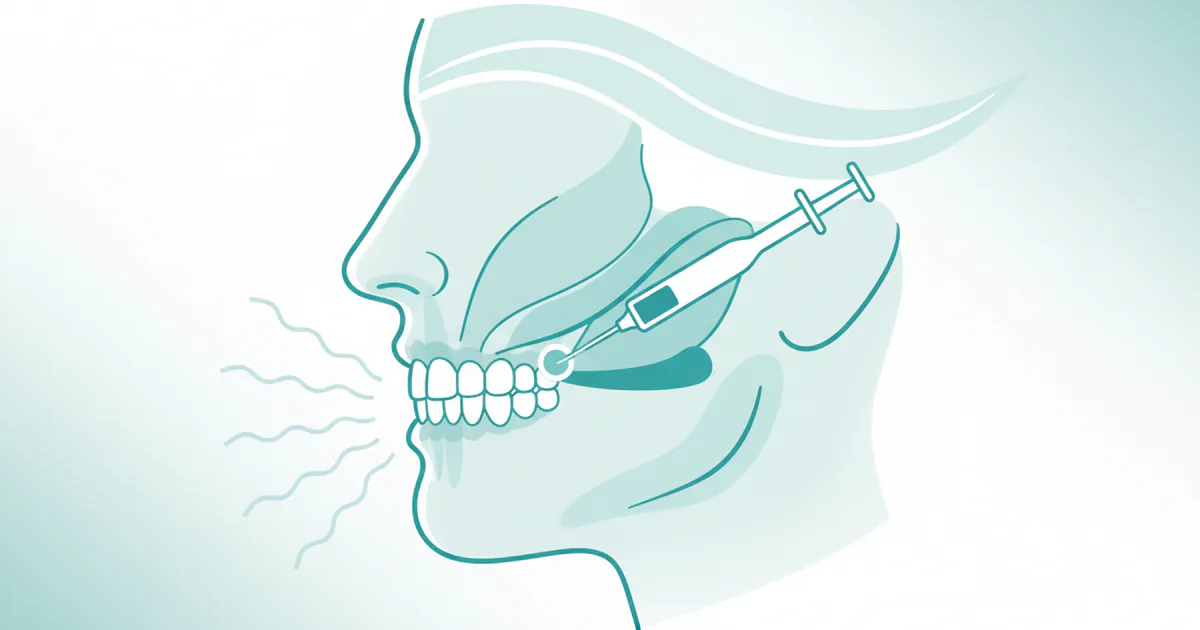
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. An estimated one in three adults experiences bruxism, the medical term for teeth grinding or jaw clenching, with a significant percentage doing so unconsciously during sleep. While some might dismiss it as a minor annoyance, chronic jaw clenching can lead to severe dental damage, persistent pain, and significantly impact your quality of life. For many grappling with this persistent condition, traditional treatments offer some relief, but a more targeted solution has emerged: Botox for jaw clenching. This comprehensive guide will delve into everything you need to know about using Botox to alleviate jaw pain and protect your teeth, exploring its efficacy, safety, cost, and what to expect throughout the process. We'll also cover the broader landscape of bruxism, from its causes and symptoms to other treatment options, ensuring you have the complete picture to make an informed decision about your dental health.
Key Takeaways:
- Botox for jaw clenching targets and relaxes the powerful masseter muscles, reducing involuntary clenching and grinding.
- Treatment typically involves 20-50 units of Botox per side, administered in a quick, in-office procedure lasting about 10-20 minutes.
- Results usually become noticeable within 3-7 days and reach full effect in 1-2 weeks, lasting an average of 3-6 months.
- The average cost for Botox jaw treatment in the US ranges from $500 to $1,500 per session, depending on location, provider, and units needed. Most dental insurance plans do not cover cosmetic Botox but may offer partial coverage for medically necessary treatments if specific criteria are met.
- Potential side effects are generally mild and temporary, including temporary muscle weakness, bruising, or a slight change in smile. Serious complications are rare with an experienced provider.
- Botox is a complementary treatment, often used in conjunction with other therapies like nightguards, stress management, and lifestyle changes, for optimal, long-term relief from bruxism symptoms.
- For children, "teeth grinding in sleep kids" is common and usually resolves naturally; Botox is not a recommended treatment for pediatric bruxism.
What It Is: Understanding Bruxism and Botox's Role
Bruxism is a condition characterized by grinding, gnashing, or clenching your teeth. It can occur while you're awake (awake bruxism) or, more commonly, during sleep (sleep bruxism). While occasional teeth grinding may not cause harm, when it occurs regularly, it can lead to a host of problems, including worn-down teeth, damaged dental restorations, jaw pain, headaches, and even temporomandibular joint (TMJ) disorders.
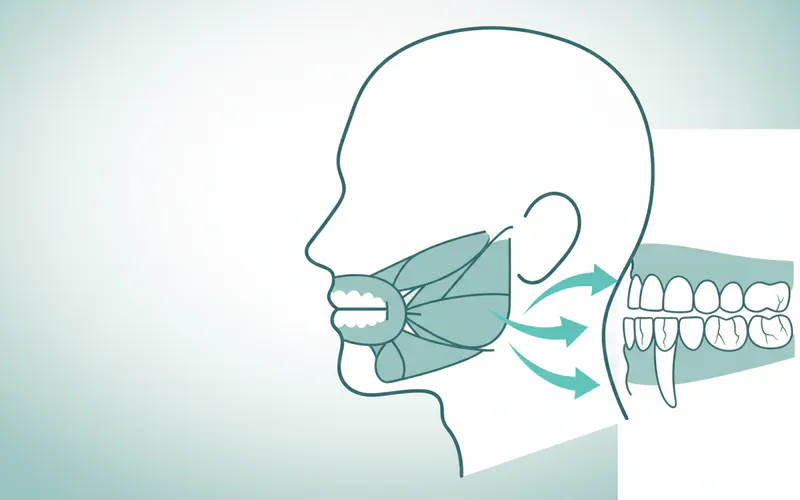
The primary muscles responsible for jaw clenching are the masseter muscles, located on the sides of your face, connecting your cheekbone to your lower jaw. When these muscles are overused or hyperactive due to bruxism, they can become enlarged, tense, and painful. This constant strain is what leads to the characteristic symptoms of jaw clenching and grinding.
Botulinum Toxin Type A, commonly known by brand names like Botox®, Dysport®, Xeomin®, and Jeuveau®, is a neurotoxin that temporarily paralyzes or weakens muscle activity. While widely recognized for its cosmetic applications in reducing wrinkles, its therapeutic use in dentistry and medicine has expanded significantly. When injected into the masseter muscles, Botox works by blocking nerve signals that tell the muscles to contract. This controlled weakening of the muscle reduces the intensity and frequency of involuntary clenching and grinding, thereby relieving symptoms and protecting teeth from further damage. It doesn't permanently paralyze the muscles but rather relaxes them enough to lessen the force of clenching without affecting essential functions like speaking or chewing.
Types of Bruxism and Why It Happens
Understanding the different manifestations and underlying causes of bruxism is crucial for effective management.
Types of Bruxism
- Awake Bruxism: This occurs when you unconsciously clench your jaw or grind your teeth while awake. It's often a response to stress, anxiety, concentration, or even during activities like heavy lifting. People with awake bruxism may not even realize they are doing it until symptoms like jaw pain or headaches develop.
- Sleep Bruxism: This is the more common and often more damaging form, occurring unconsciously during sleep. Because you're unaware of it, it can be harder to control and often leads to more significant dental wear and pain. Many people discover they have sleep bruxism because a partner hears them grinding their teeth at night or their dentist notices the tell-tale signs of tooth wear during a routine check-up. This is often referred to as "teeth grinding in sleep kids" when it affects children.
Causes and Contributing Factors
Bruxism is a complex condition with various potential causes and contributing factors. It's often multifactorial, meaning several elements might be at play:
- Stress and Anxiety: This is arguably the most common culprit. High levels of psychological stress, anxiety, anger, or tension can lead to jaw clenching, both consciously and unconsciously.
- Sleep Disorders: Conditions like sleep apnea, snoring, and other sleep-disordered breathing can disrupt sleep patterns and are strongly linked to sleep bruxism. The body may clench the jaw in an effort to open the airway.
- Misaligned Teeth (Malocclusion): An improper bite or crooked teeth can sometimes contribute to bruxism, as the jaw muscles work harder to find a comfortable resting position.
- Certain Medications: Some antidepressants (especially SSRIs) and antipsychotics can have bruxism as a side effect.
- Lifestyle Factors:
- Caffeine and Alcohol: Excessive consumption of caffeine (coffee, energy drinks) and alcohol can exacerbate bruxism.
- Smoking: Nicotine is a stimulant and can contribute to muscle hyperactivity.
- Recreational Drugs: Amphetamines and ecstasy are known to cause severe bruxism.
- Neurological Conditions: Rare cases of bruxism can be associated with conditions like Parkinson's disease, Huntington's disease, or other neurological disorders.
- Genetic Factors: There's some evidence to suggest a genetic predisposition to sleep bruxism.
- Age: While bruxism can affect anyone, it's particularly common in young children and tends to decrease with age.
Signs and Symptoms: What to Look For
Recognizing the early signs of teeth grinding and jaw clenching is critical for timely intervention and preventing more severe problems. Many individuals don't realize they have bruxism until their dentist points out the physical evidence or they start experiencing noticeable symptoms.
Look out for these common indicators:
- Tooth Sensitivity or Pain: Unexplained sensitivity to hot, cold, or pressure, often generalized across multiple teeth. The constant force of grinding wears down enamel, exposing the sensitive dentin underneath.
- Worn-Down, Chipped, or Fractured Teeth: Flattened chewing surfaces, small chips, or even cracks in teeth are classic signs of bruxism. Fillings and crowns can also be damaged or dislodged.
- Loose Teeth: Persistent grinding can put excessive stress on the periodontal ligaments that hold teeth in place, potentially leading to tooth mobility.
- Sore Jaw Muscles or Pain: Aching or tightness in the jaw, especially upon waking. This pain can radiate to the ears or neck.
- Facial Pain: Generalized pain across the face, particularly around the temples and cheeks.
- Headaches: Frequent tension-type headaches, often starting in the temples and radiating across the forehead, are a common symptom. These are often worse in the morning.
- Earaches: While not a true ear infection, jaw clenching can cause referred pain that feels like an earache due to the proximity of the jaw joint to the ear canal.
- Jaw Locking or Limited Opening: Difficulty opening your mouth fully, or a sensation that your jaw is "locking" or getting stuck.
- Clicking, Popping, or Grating Sounds in the Jaw Joint: These sounds, medically known as crepitus or clicking, can indicate issues with the temporomandibular joint (TMJ) due to strain.
- Indentations on the Tongue or Inner Cheeks: The constant pressure from clenching can cause the tongue to develop scalloped edges or leave imprints on the inside of your cheeks.
- Sleep Disruption: While you may not be aware of your own grinding, a sleep partner might hear you. Sleep bruxism can also lead to fragmented sleep, leaving you feeling unrested even after a full night.
Pro Tip: If you notice any of these signs, especially if they are persistent, schedule an appointment with your dentist. They can properly diagnose bruxism and recommend the most appropriate course of action.
Treatment Options for Bruxism and Jaw Clenching
While our focus is on Botox for jaw clenching, it's important to understand the full spectrum of available treatments. Botox is often most effective when integrated into a broader management strategy.
1. Oral Appliances (Nightguards or Splints)
- What it is: Custom-made acrylic mouthguards worn over the teeth, primarily at night, to create a physical barrier between the upper and lower teeth.
- Pros: Protects teeth from wear and fracture, can reduce jaw muscle activity by providing a more stable bite, non-invasive, widely recommended by the ADA.
- Cons: Can be uncomfortable for some, requires consistent wear, doesn't stop the clenching itself, can be costly for custom versions (over-the-counter options are less effective and potentially harmful).
- Cost: $300-$800 for a custom-fitted guard from a dentist; $20-$100 for boil-and-bite options.
2. Lifestyle Modifications & Stress Management
- What it is: Techniques to reduce stress and promote relaxation, which are major triggers for bruxism.
- Pros: Addresses root causes, no side effects, improves overall well-being, cost-effective.
- Cons: Requires discipline and consistent effort, results may not be immediate.
- Examples: Meditation, yoga, deep breathing exercises, regular exercise, therapy/counseling, limiting caffeine and alcohol intake, establishing a relaxing bedtime routine.
3. Behavioral Therapies
- What it is: Techniques aimed at retraining jaw muscles and increasing awareness.
- Pros: Can be effective for awake bruxism, empowers patients with self-management tools.
- Cons: Less effective for sleep bruxism, requires active participation.
- Examples: Biofeedback, habit awareness training (e.g., placing the tongue between teeth to prevent clenching).
4. Physical Therapy
- What it is: Exercises and manual therapy to release tension in jaw muscles and improve jaw mobility.
- Pros: Reduces muscle soreness and stiffness, improves range of motion.
- Cons: Requires consistency, may need multiple sessions.
5. Medications
- What it is: Rarely used, usually for short-term relief or in severe cases.
- Pros: Can provide temporary relief from pain and muscle spasm.
- Cons: Potential for side effects, often not a long-term solution.
- Examples: Muscle relaxants (e.g., cyclobenzaprine) for short-term use, anti-inflammatory drugs (NSAIDs) for pain, sometimes low-dose tricyclic antidepressants.
6. Orthodontic Treatment
- What it is: If a significant malocclusion (bad bite) is identified as a primary contributor, orthodontic treatment (braces, aligners) may be considered.
- Pros: Addresses underlying structural issues, can provide long-term correction.
- Cons: Expensive, time-consuming, not always directly related to bruxism, and usually only considered after other options fail.
7. Botox Injections (Therapeutic Botulinum Toxin)
- What it is: The primary focus of this article, involving injections into the masseter muscles to reduce muscle activity.
- Pros: Directly targets the overactive muscles, significantly reduces clenching force, alleviates pain and headaches, protects teeth, can slim a wide jawline.
- Cons: Temporary effect (3-6 months), requires repeat treatments, cost is out-of-pocket for most, potential mild side effects.
Step-by-Step Process: What to Expect During Botox Treatment
If you decide that Botox for jaw clenching is the right path for you, here’s a typical overview of the treatment process:
1. Initial Consultation and Assessment
- Purpose: Your first visit involves a thorough discussion with a qualified healthcare provider (dentist specializing in TMJ/oral facial pain, oral surgeon, or cosmetic dermatologist). They will evaluate your symptoms, medical history, current medications, and perform a physical examination of your jaw muscles.
- Discussion Points: You’ll discuss your goals for treatment, potential risks, expected outcomes, and alternative therapies. The provider will assess the size and strength of your masseter muscles to determine the appropriate dosage of Botox.
- Preparation: You may be advised to avoid blood-thinning medications (like aspirin, ibuprofen, certain supplements) for a week prior to treatment to minimize bruising, if medically cleared by your physician.
2. Treatment Planning
- Dosage: Based on the assessment, the provider will decide the number of units of Botox needed. For therapeutic jaw clenching, this typically ranges from 20 to 50 units per side, with more severe cases requiring higher doses.
- Injection Sites: The specific injection points within the masseter muscles will be marked.
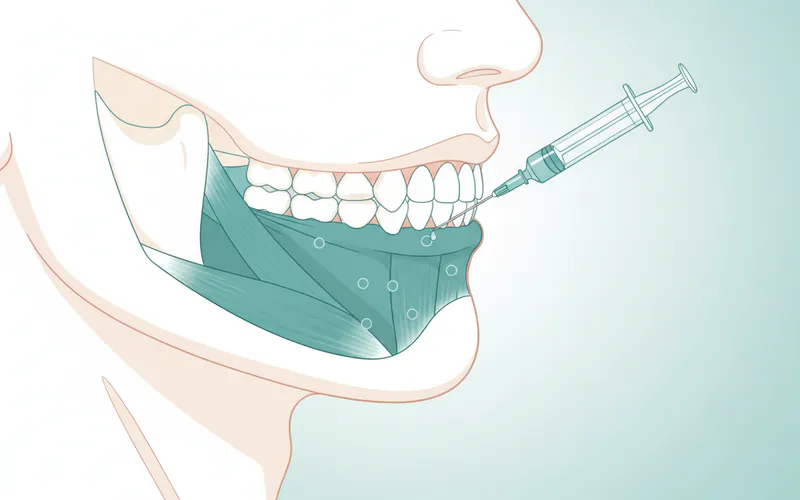
3. The Injection Procedure
- Preparation: The skin around the injection sites will be cleaned with an antiseptic wipe. A topical numbing cream may be applied, though many patients find the injections tolerable without it.
- Injection: Using a very fine needle, the Botox is injected directly into the designated masseter muscle points on each side of the face. The injections are quick, usually lasting only a few seconds each. You might feel a slight pinch or pressure.
- Duration: The entire injection process typically takes only 10 to 20 minutes.
- Post-Injection: The provider may apply gentle pressure to the injection sites to minimize bruising.
4. Immediate Aftercare
- Activity: You can generally resume most normal activities immediately.
- Instructions: You’ll be advised to avoid rubbing or massaging the treated area for at least 24 hours to prevent the Botox from spreading to unintended muscles. Also, avoid strenuous exercise, lying down flat, or wearing tight-fitting hats for a few hours.
Cost and Insurance: Understanding the Financial Aspect
The cost of Botox for jaw clenching can be a significant factor in your decision. It's important to understand the various elements that contribute to the overall price and what to expect regarding insurance coverage in the US market.
Average US Price Ranges
The cost of Botox for therapeutic jaw clenching typically ranges from $500 to $1,500 per session. This wide range is influenced by several factors:
- Location: Prices can vary significantly by geographic region. Major metropolitan areas (e.g., New York, Los Angeles) often have higher costs than rural or less populated areas.
- Provider Expertise: Highly experienced practitioners, specialists (like oral surgeons, TMJ dentists, or neurologists), or those in high-end clinics may charge more per unit or per session.
- Number of Units Needed: The primary driver of cost is the amount of Botox (measured in units) required. A typical therapeutic dose for bruxism can range from 20-50 units per masseter muscle, sometimes more for very strong muscles. If a provider charges $10-$20 per unit, then 40 units per side (80 units total) would cost $800-$1,600.
- Consultation Fees: Some clinics may charge a separate consultation fee, which might or might not be applied towards the treatment cost.
- Follow-up Appointments: Some providers include a follow-up visit in the initial cost, while others may charge for it separately.
Example Cost Breakdown by Units (Illustrative)
| Units of Botox (Total) | Average Low Cost (US) | Average Mid Cost (US) | Average High Cost (US) |
|---|---|---|---|
| 40 (20 per side) | $400 | $600 | $800 |
| 60 (30 per side) | $600 | $900 | $1,200 |
| 80 (40 per side) | $800 | $1,200 | $1,600 |
| 100 (50 per side) | $1,000 | $1,500 | $2,000 |
| Note: Prices are estimates and can vary widely. Always get a personalized quote. |
Insurance Coverage Details
- Cosmetic vs. Therapeutic: Most dental and medical insurance plans do not cover Botox injections for purely cosmetic purposes (e.g., wrinkle reduction).
- Medical Necessity: However, if Botox is deemed medically necessary to treat a condition like chronic bruxism, TMJ disorder, or myofascial pain that has not responded to other conventional treatments, some insurance plans may offer partial coverage.
- Criteria for Coverage:
- Diagnosis: A clear diagnosis of bruxism or TMJ disorder from a qualified medical professional.
- Failed Conservative Treatments: Documentation that other less invasive treatments (e.g., nightguards, physical therapy, medications) have been tried and failed to provide adequate relief.
- Prior Authorization: Your provider will likely need to submit a detailed request for prior authorization to your insurance company, outlining the medical necessity and expected benefits.
- Specific Plan Details: Coverage depends entirely on your specific insurance policy. Plans can vary greatly in what they cover for "therapeutic Botox."
- Out-of-Pocket Expenses: Even with partial coverage, you will likely still be responsible for deductibles, co-pays, and co-insurance. Many patients find that therapeutic Botox remains an out-of-pocket expense.
Payment Plans and Financing Options
Since insurance coverage is often limited, many providers offer:
- Payment Plans: In-house payment plans, allowing you to pay for treatment in installments.
- Third-Party Financing: Options like CareCredit, which offer special financing for healthcare expenses, often with interest-free periods if paid in full within a certain timeframe.
Pro Tip: Always clarify the total cost with your provider upfront, including all units, follow-up fees, and potential insurance billing procedures. Get a written estimate before proceeding.
Recovery and Aftercare
The recovery period after Botox injections for jaw clenching is generally quick and straightforward, with minimal downtime.
Immediate Post-Treatment (First 24-48 Hours)
- Activity: You can typically resume most daily activities immediately after your appointment.
- Avoid Rubbing/Massaging: It's crucial to avoid rubbing, massaging, or applying excessive pressure to the treated area for at least 24 hours. This prevents the Botox from migrating to unintended muscles, which could lead to unwanted side effects.
- Avoid Strenuous Exercise: Refrain from heavy exercise, hot baths, saunas, or anything that significantly increases blood flow to the face for 24-48 hours.
- Avoid Lying Flat: Try to avoid lying down for 4-6 hours post-injection.
- Mild Side Effects: You might experience mild redness, swelling, or pinpoint bruising at the injection sites. These are usually temporary and resolve within a few hours to a few days. Applying a cold compress gently can help reduce swelling and bruising.
Short-Term (First 1-2 Weeks)
- Onset of Effects: You will typically start to notice the effects of Botox within 3-7 days, with the full therapeutic effect becoming apparent around 1-2 weeks. During this time, you should feel a gradual reduction in jaw clenching intensity and associated pain.
- Chewing: While your jaw muscles will be weaker, you should still be able to chew normally. Your body will adjust, and other muscles will compensate for the reduced masseter strength.
- Jawline Slimming: If one of your goals was also a slimmer jawline (due to masseter hypertrophy from chronic clenching), you'll start to see this aesthetic change emerge over several weeks as the muscle gradually atrophies from disuse.
Long-Term (Beyond 2 Weeks)
- Duration of Effect: The therapeutic effects of Botox for jaw clenching typically last for 3 to 6 months. The duration can vary between individuals and with subsequent treatments. Over time, many patients find that the effects last longer, and they may require fewer units per session as the masseter muscles diminish in size and strength.
- Repeat Treatments: To maintain the benefits, repeat injections are necessary. Your provider will recommend a schedule based on your individual response and symptom recurrence.
- Complementary Therapies: Continue with any other recommended treatments, such as wearing a nightguard, stress management techniques, or physical therapy, as these can enhance and prolong the benefits of Botox.
Prevention: Strategies to Mitigate Jaw Clenching
While Botox offers excellent relief for existing jaw clenching, preventing the issue or reducing its severity can significantly improve your long-term oral health and comfort.
- Stress Management: Since stress and anxiety are primary triggers for bruxism, effective stress reduction is paramount.
- Mindfulness & Meditation: Regular practice can help calm the nervous system.
- Yoga & Deep Breathing: Promotes relaxation and reduces overall tension.
- Exercise: Physical activity is a natural stress reliever.
- Therapy: Cognitive-Behavioral Therapy (CBT) can help manage anxiety and stress.
- Identify and Avoid Triggers:
- Caffeine and Alcohol: Reduce or eliminate consumption, especially in the evenings, as they are stimulants that can worsen bruxism.
- Nicotine: Smoking and other nicotine products can stimulate muscle activity.
- Recreational Drugs: Avoid substances known to induce bruxism.
- Establish a Relaxing Bedtime Routine:
- Wind-Down Activities: Read a book, listen to calming music, take a warm bath before bed.
- Avoid Screens: Limit screen time (phones, tablets, computers) for at least an hour before sleep.
- Comfortable Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Jaw and Facial Exercises: Gently stretching and relaxing jaw muscles can reduce tension. Your dentist or a physical therapist can recommend specific exercises.
- Maintain Good Oral Posture:
- Awareness: During the day, try to be mindful of your jaw position. Keep your teeth slightly apart, with your tongue resting on the roof of your mouth.
- "Lips Together, Teeth Apart": This simple mantra can help you maintain proper resting jaw posture.
- Regular Dental Check-ups: Your dentist can monitor for early signs of teeth grinding and suggest interventions before significant damage occurs. They can also ensure your bite is stable.
- Address Sleep Disorders: If you suspect a sleep disorder like sleep apnea, consult a doctor. Treating the underlying sleep issue can often reduce or eliminate sleep bruxism.
Risks and Complications
While Botox injections for jaw clenching are generally considered safe when performed by a qualified and experienced practitioner, it's essential to be aware of potential risks and complications.
Common, Mild, and Temporary Side Effects
These usually resolve within a few days to a week:
- Pain, Bruising, or Swelling at Injection Site: This is the most common side effect and can be minimized with proper aftercare.
- Headache: A mild headache can occur shortly after treatment but typically subsides quickly.
- Temporary Muscle Weakness: You might feel a slight weakness in your jaw muscles, especially when chewing hard or tough foods. This is usually mild and temporary as the muscles adapt.
- Asymmetry: Very occasionally, one side might respond slightly differently, leading to temporary facial asymmetry. This is often correctable with a touch-up.
- "Botox Smile": In rare cases, if the Botox spreads to nearby muscles that control smiling, it can temporarily affect your smile, making it look asymmetrical or strained. This is usually temporary and resolves as the Botox wears off.
- Dry Mouth: Some individuals report temporary dry mouth.
Less Common but Potentially More Significant Complications
These are rare, especially with an experienced injector:
- Difficulty Chewing: If too much Botox is injected or if it spreads, it can lead to more pronounced difficulty chewing, though this is typically temporary.
- Dysphagia (Difficulty Swallowing): Extremely rare, but possible if the Botox affects muscles involved in swallowing.
- Allergic Reaction: While rare, some individuals can have an allergic reaction to Botox, which can range from hives and itching to more severe symptoms like swelling of the face, lips, or tongue, and difficulty breathing.
- Infection: As with any injection, there's a small risk of infection at the injection site, though this is minimized by proper sterile technique.
- Spread to Other Muscles: If the Botox diffuses beyond the targeted masseter muscles, it can affect adjacent muscles, leading to unintended muscle weakness or facial drooping. This risk is very low with precise injection techniques.
Pro Tip: Always choose a board-certified and experienced healthcare provider (dentist, oral surgeon, dermatologist, or plastic surgeon) who is knowledgeable in facial anatomy and has specific experience with therapeutic Botox injections for bruxism. Discuss all your medical conditions and medications with your provider before treatment.
Children / Pediatric Considerations
Bruxism, particularly "teeth grinding in sleep kids," is a very common phenomenon in children. While it can be alarming for parents to hear, it's important to understand that pediatric bruxism is often a temporary and benign condition that differs significantly from adult bruxism.
Prevalence and Causes in Children
- High Incidence: Up to 3 out of 10 children grind or clench their teeth, with the peak incidence typically between ages 3 and 12.
- Common During Sleep: Most children grind their teeth during sleep, often during periods of stress, growth, or when erupting new teeth.
- Developmental Factors: Teething pain, misaligned primary (baby) teeth, or changes in bite as permanent teeth emerge can be triggers.
- Stress and Anxiety: Similar to adults, stress from school, new siblings, or even exciting events can manifest as bruxism.
- Medical Conditions: Less commonly, it can be associated with allergies, sleep apnea, or certain medications.
Signs and Symptoms in Children
- Audible Grinding: The most obvious sign is hearing your child grind their teeth at night.
- Jaw Pain or Soreness: Children might complain of a sore jaw or face, especially in the morning.
- Headaches: Unexplained headaches, often reported upon waking.
- Tooth Sensitivity: Though less common in children, they might complain about sensitive teeth.
- Worn or Chipped Teeth: Your pediatric dentist is often the first to notice flattened tooth surfaces or minor chips during a routine exam.
Treatment and Management for Children
- Observation is Key: For most children, bruxism resolves on its own without intervention as they grow and their dental structure matures. Many outgrow it by adolescence.
- Addressing Stress: If stress or anxiety is suspected, focus on relaxation techniques, a consistent bedtime routine, and open communication with your child.
- Dental Appliances (Rare): Custom nightguards are rarely recommended for young children, as their jaws are still growing and teeth are changing. They might be considered in severe cases of significant tooth wear, but only after careful consideration by a pediatric dentist.
- No Botox for Children: It is crucial to emphasize that Botox injections are NOT a recommended or appropriate treatment for pediatric bruxism. The safety and efficacy of Botox in children for this indication have not been established, and their developing facial structures and muscles warrant a conservative approach.
- When to See a Dentist: If your child's bruxism is causing persistent pain, significant tooth wear, or is accompanied by other concerning symptoms (like difficulty sleeping or breathing), consult a pediatric dentist. They can monitor the situation, rule out underlying issues, and provide guidance specific to your child's development.
Frequently Asked Questions
Q1: How long does Botox for jaw clenching last?
A: The effects of Botox for jaw clenching typically last between 3 to 6 months. Individual results can vary based on factors like metabolism, muscle strength, and the number of units injected. Many patients find that with consistent treatments, the effects may last longer over time as the masseter muscles gradually atrophy.
Q2: Is Botox for jaw clenching painful?
A: Most patients describe the injections as a mild, brief pinch or sting. A very fine needle is used, and the procedure is quick. Many providers offer a topical numbing cream prior to injection to minimize discomfort, making the experience generally well-tolerated.
Q3: How quickly will I see results from Botox for jaw clenching?
A: You can typically expect to feel the initial effects, such as reduced clenching intensity, within 3 to 7 days after the injections. The full therapeutic benefits, including significant pain relief and potential jawline slimming, usually become apparent within 1 to 2 weeks.
Q4: Will Botox affect my ability to chew or speak?
A: No, when performed correctly by an experienced professional, Botox for jaw clenching should not impair your ability to chew, speak, or make normal facial expressions. The goal is to weaken the masseter muscles just enough to reduce involuntary clenching, not to paralyze them entirely. You might feel a slight, temporary weakness when chewing very hard foods initially.
Q5: Can I get Botox for jaw clenching if I'm pregnant or breastfeeding?
A: No, Botox is generally contraindicated during pregnancy and breastfeeding. There isn't enough research on the safety of Botox for pregnant or lactating individuals, so it's best to avoid it during these periods to ensure the safety of both mother and child.
Q6: Are there any alternatives to Botox for jaw clenching?
A: Yes, several alternatives exist, often used in conjunction with or prior to Botox. These include custom nightguards (occlusal splints) to protect teeth, stress management techniques, physical therapy, behavioral therapy, and, in some cases, muscle relaxants or other medications.
Q7: Does dental insurance cover Botox for jaw clenching?
A: Most dental and medical insurance plans do not cover Botox for cosmetic purposes. However, if Botox is deemed medically necessary to treat severe chronic bruxism or TMJ disorder that has not responded to other conservative treatments, some insurance plans may offer partial coverage. Prior authorization and detailed documentation of medical necessity are usually required. It's crucial to check with your specific insurance provider.
Q8: Can Botox injections help with TMJ pain?
A: Yes, Botox can be an effective treatment for temporomandibular joint (TMJ) disorders, particularly those associated with muscle hyperactivity, jaw clenching, and grinding. By relaxing the overactive masseter and sometimes temporalis muscles, it can significantly reduce pain, headaches, and tension related to TMJ.
Q9: Will Botox change my facial appearance?
A: While the primary goal is therapeutic, a common side effect (often desired) of masseter Botox is a subtle slimming of the jawline. Over time, as the masseter muscles weaken and slightly shrink due to reduced activity (muscle atrophy), the lower face can appear more V-shaped. This is generally considered a cosmetic benefit.
Q10: How many units of Botox are typically needed for jaw clenching?
A: The typical dosage for therapeutic jaw clenching ranges from 20 to 50 units per side, for a total of 40 to 100 units. The exact amount depends on the individual's muscle strength, the severity of their bruxism, and the provider's assessment.
When to See a Dentist
Recognizing when to seek professional dental or medical attention for jaw clenching is crucial for preventing long-term damage and managing pain effectively.
Schedule a Routine Appointment If You Notice:
- Persistent Jaw Soreness or Fatigue: If you frequently wake up with a tired or aching jaw.
- Dull Headaches: Particularly those that occur in the temples or forehead upon waking.
- Increased Tooth Sensitivity: Especially if it's generalized and not linked to a specific tooth issue like a cavity.
- Early Signs of Teeth Grinding: Your partner mentions hearing you grind your teeth at night, or you notice minor chips or wear facets on your teeth during your daily routine.
- Indentations on Your Tongue or Cheeks: Scalloped edges on your tongue or white lines on your inner cheeks (linea alba) can indicate clenching or grinding.
- Difficulty or Discomfort While Chewing: If it feels harder to chew certain foods, or your jaw tires easily.
Seek Prompt Dental Attention (Within a Few Days) If You Experience:
- Significant Tooth Damage: Chipped, fractured, or loose teeth that appear to be worsening rapidly.
- Severe Jaw Pain: Pain that is debilitating, interferes with eating, or doesn't respond to over-the-counter pain relievers.
- Limited Jaw Movement: Inability to open your mouth fully, or your jaw feels "stuck" or locks frequently.
- Loud Clicking or Popping in the Jaw Joint: Especially if accompanied by pain or difficulty moving your jaw.
- Pain Radiating to Your Ears, Neck, or Shoulders: This can indicate a more advanced TMJ issue or muscle spasm.
Emergency Dental Visit (Immediate Attention) Is Needed For:
- Acute Jaw Dislocation: If your jaw is visibly out of alignment or you cannot close your mouth.
- Excruciating Pain: Unbearable pain in your jaw or face that comes on suddenly and severely.
- Facial Swelling with Fever: This could indicate an infection that requires immediate medical intervention.
Remember, early diagnosis and intervention are key to managing bruxism and preventing its more damaging consequences. Your dental professional can offer tailored advice, diagnose the extent of the problem, and recommend the most appropriate treatment plan for your specific needs, potentially including Botox for jaw clenching as a targeted solution.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026