Mild Bruxism Teeth: Complete Guide
Key Takeaways
- Do you ever wake up with a dull headache, a sore jaw, or find yourself clenching your teeth during the day without realizing it? You're not alone. An estimated 10-15% of adults and up to 30% of children experience bruxism, a condition characterized by grinding, clenching, or gnashing of teeth. W
Mild Bruxism Teeth: Complete Guide
Do you ever wake up with a dull headache, a sore jaw, or find yourself clenching your teeth during the day without realizing it? You're not alone. An estimated 10-15% of adults and up to 30% of children experience bruxism, a condition characterized by grinding, clenching, or gnashing of teeth. While severe bruxism can lead to significant dental damage, many people experience mild bruxism teeth, a less aggressive form that often goes unnoticed until subtle symptoms accumulate. Understanding mild bruxism is crucial because, left unaddressed, it can progress, leading to more serious health issues like TMJ disorders, cracked teeth, and chronic pain. This comprehensive guide will equip you with everything you need to know about mild bruxism, from its causes and symptoms to effective treatment strategies and preventive measures, ensuring your dental health and overall well-being.

Key Takeaways:
- What is Mild Bruxism? It's involuntary clenching or grinding of teeth that doesn't yet cause significant dental damage or severe symptoms, but can lead to subtle issues like jaw stiffness, headaches, and minor tooth sensitivity.
- Common Causes: Stress, anxiety, certain medications, sleep disorders (like mild sleep apnea), and even malocclusion (misaligned bite) are frequent contributors.
- Primary Symptoms: Watch for morning headaches, unexplained tooth sensitivity, slight jaw fatigue, minor tooth wear, or subtle indentations on the tongue or cheek lining.
- Treatment Options: Lifestyle modifications (stress reduction), over-the-counter or custom-fit mouthguards (ranging from $25-$50 for OTC to $300-$800+ for custom), biofeedback, and behavioral therapies are highly effective for managing mild bruxism.
- Cost & Insurance: Basic OTC nightguards are inexpensive, while custom dental appliances can range from $300 to $800 in the US, potentially covered partially by dental insurance, especially if medically necessary for sleep bruxism.
- Prevention: Stress management, regular dental check-ups, avoiding stimulants before bed, and practicing jaw relaxation techniques are key to preventing mild bruxism from worsening.
- When to See a Dentist: If you suspect mild bruxism, notice persistent jaw pain, increasing tooth sensitivity, or your symptoms interfere with daily life, schedule an appointment promptly to prevent progression to severe damage.
What It Is: An Overview of Mild Bruxism
Bruxism, derived from the Greek word "brychein" meaning "to gnash the teeth," is a parafunctional oral habit, meaning it involves the oral system in ways other than its primary functions like eating and speaking. While often associated with aggressive grinding, bruxism exists on a spectrum of severity. Mild bruxism teeth refers to the early, less intense, and often intermittent form of this condition.
Unlike severe bruxism, which can cause obvious tooth wear, fractures, and intense jaw pain, mild bruxism might manifest as subtle discomfort or barely perceptible dental changes. It's often characterized by unconscious clenching or gentle grinding that doesn't immediately alarm the individual or their dentist. However, "mild" doesn't mean "harmless." Even low-grade, consistent pressure on your teeth can accumulate over time, leading to cumulative strain on your dental structures and temporomandibular joints (TMJ), which connect your jaw to your skull.
Differentiating Mild from Severe Bruxism
The key distinction lies in the frequency, intensity, and resulting damage.
-
Mild Bruxism:
- Frequency: Intermittent, occasional, or less prolonged episodes.
- Intensity: Less forceful clenching or grinding.
- Symptoms: Subtle, such as morning jaw stiffness, slight tooth sensitivity, occasional headaches, minor tooth wear that might not be visible without close dental inspection.
- Dental Damage: Minimal, often superficial wear facets (polished spots on tooth surfaces) or slight enamel erosion.
- Impact on Life: Usually doesn't significantly interfere with daily activities, but can be a source of mild chronic discomfort.
-
Severe Bruxism:
- Frequency: Frequent, prolonged, or nightly episodes.
- Intensity: Very forceful clenching or grinding.
- Symptoms: Intense chronic jaw pain, frequent headaches, migraines, facial muscle soreness, audible grinding sounds (often reported by partners), significant tooth sensitivity.
- Dental Damage: Pronounced tooth wear, flattened biting surfaces, chipped or fractured teeth, receding gums, loose teeth, damage to existing dental work (crowns, fillings), and significant TMJ dysfunction.
- Impact on Life: Can severely impair eating, speaking, sleep, and overall quality of life.
The challenge with mild bruxism is its insidious nature. Because the symptoms are often vague and can be attributed to other causes (like stress or a poor night's sleep), it can be overlooked. Early identification and intervention are crucial to prevent its progression to a more damaging, severe form.
Types of Bruxism: Awake vs. Sleep
Bruxism generally falls into two main categories, irrespective of its severity:
Awake Bruxism (Diurnal Bruxism)
Awake bruxism refers to clenching or grinding that occurs while you are awake. This type of bruxism is often unconscious but can also be semi-conscious, where you realize you're doing it but struggle to stop.
- Characteristics: Typically involves clenching rather than grinding. People might press their teeth together forcefully in response to stress, concentration, or even during routine tasks like driving or working on a computer.
- Triggers: High-stress situations, anxiety, anger, intense focus, or even certain medications (e.g., antidepressants like SSRIs).
- Symptoms: Often manifests as jaw tension, headaches (especially tension headaches), and occasional tooth sensitivity during the day. Since it's often clenching, the tell-tale grinding sound may not be present, making diagnosis harder.
- Management for Mild Awake Bruxism: Primarily behavioral. Awareness, stress reduction techniques, biofeedback, and consciously training yourself to relax your jaw muscles are key.
Sleep Bruxism (Nocturnal Bruxism)
Sleep bruxism occurs during sleep and is classified as a sleep-related movement disorder. It's often entirely unconscious, making it harder to detect without external cues.
- Characteristics: Can involve both clenching and grinding, sometimes quite forcefully. It typically happens during the lighter stages of sleep or during sleep arousal.
- Triggers: While stress and anxiety play a role, sleep bruxism is often associated with sleep disorders like sleep apnea, snoring, and gastroesophageal reflux disease (GERD). Certain medications and recreational drugs can also contribute.
- Symptoms: Often results in morning headaches, sore jaw muscles upon waking, tooth sensitivity that is worse in the mornings, and sometimes indentations on the side of the tongue or inside of the cheek where the teeth have pressed. A sleeping partner might report hearing grinding sounds.
- Management for Mild Sleep Bruxism: Primarily involves dental appliances (nightguards/mouthguards) to protect the teeth, along with addressing underlying sleep disorders or stress.
It's important to note that an individual can experience both awake and sleep bruxism. For mild bruxism teeth, distinguishing between the two types helps in tailoring the most effective treatment strategy, especially concerning how to stop teeth clenching during the day or protecting teeth grinding molars at night.
Causes: Why Mild Bruxism Happens
The precise cause of bruxism is complex and often multifactorial, meaning several factors can contribute simultaneously. For mild bruxism, these factors might be present in a less intense or consistent manner than in severe cases.
1. Stress and Anxiety
This is perhaps the most widely recognized and significant contributor to both awake and sleep bruxism. Psychological stress, emotional tension, frustration, and anxiety can all trigger jaw clenching and teeth grinding. The jaw muscles unconsciously tense up as a physical manifestation of emotional strain. Even mild, chronic stress can lead to mild bruxism teeth.
2. Malocclusion and Dental Factors
While less definitively proven than stress, some dental professionals believe that misaligned teeth (malocclusion), missing teeth, or poorly fitted dental restorations (like crowns or fillings) can contribute. If your teeth don't fit together properly, your jaw might unconsciously seek a more comfortable position, leading to grinding or clenching. This is particularly relevant for teeth grinding molars, as they bear the brunt of the bite force.
3. Sleep Disorders
Sleep bruxism is closely linked with other sleep-related breathing disorders, most notably sleep apnea. When breathing is momentarily interrupted during sleep, the body's natural response can include clenching or grinding as an effort to open the airway. Even mild, undiagnosed sleep-disordered breathing can trigger mild bruxism. Snoring is also often associated.
4. Medications and Lifestyle Factors
- Medications: Certain medications, especially selective serotonin reuptake inhibitors (SSRIs) used for depression and anxiety, can have bruxism as a side effect. Other drugs like amphetamines (e.g., Adderall) and ecstasy are also known culprits.
- Stimulants: Excessive consumption of caffeine, alcohol, and nicotine (smoking) can disrupt sleep patterns and increase muscle tension, potentially exacerbating or triggering bruxism.
- Recreational Drugs: Substance abuse, particularly stimulants, can significantly contribute to bruxism.
5. Other Potential Factors
- Personality Type: Individuals with aggressive, competitive, or hyperactive personality types may be more prone to bruxism.
- Genetics: There may be a genetic predisposition, as bruxism sometimes runs in families.
- Neurological Conditions: Though rare, certain neurological conditions like Parkinson's disease can be associated with bruxism.
For individuals experiencing mild bruxism, understanding these potential causes is the first step toward effective management. Identifying and addressing the root cause, whether it's daily stress or a mild sleep disturbance, is crucial for long-term relief and prevention.
Signs and Symptoms: What to Look For
Detecting mild bruxism can be tricky because its symptoms are often subtle and can easily be mistaken for other issues. However, being vigilant about these indicators can help you catch the condition early before it progresses.
1. Morning Headaches and Facial Pain
- Description: You might wake up with a dull, persistent headache, especially in the temples or forehead. This is often a tension headache caused by strained jaw muscles overnight. Mild facial pain or tenderness, particularly around the jaw joints and cheeks, is also common.
- Why it's mild: Unlike severe bruxism where headaches can be debilitating migraines, mild bruxism typically causes less intense, more localized morning discomfort.
2. Jaw Stiffness or Fatigue
- Description: Your jaw might feel stiff, tired, or achy, especially in the morning. You might notice a slight clicking or popping sound when you open or close your mouth, or mild difficulty opening your mouth wide.
- Why it's mild: The stiffness is usually temporary and resolves within a few hours. In severe cases, jaw locking or chronic pain is common.
3. Increased Tooth Sensitivity
- Description: You may experience mild sensitivity to hot, cold, or sweet foods and drinks. This happens as the grinding or clenching wears down the protective enamel, exposing the underlying dentin.
- Why it's mild: The sensitivity is often intermittent or mild, affecting specific
teeth grinding molarsor a few teeth, rather than widespread, excruciating pain typical of severe bruxism.
4. Minor Tooth Wear
- Description: A dentist might notice subtle signs of wear on the chewing surfaces of your teeth, particularly on your
teeth grinding molars. These might appear as small, polished, flat spots called "wear facets," or slight chipping at the edges of teeth. - Why it's mild: The wear is superficial and doesn't yet compromise the tooth's structure significantly. Severe bruxism leads to deeply flattened teeth, fractures, and exposed dentin.
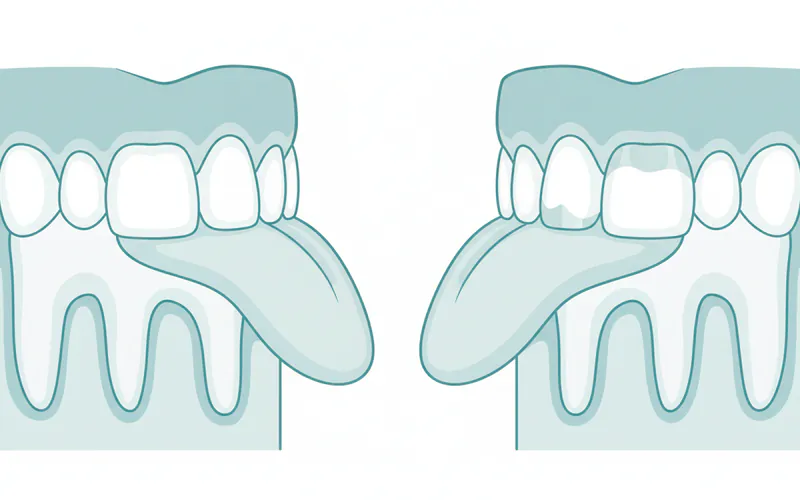
5. Indentations on Tongue or Inner Cheek
- Description: You might notice subtle scalloped edges or indentations along the sides of your tongue (crenated tongue) or white lines (linea alba) on the inside of your cheeks. These are caused by the pressure of the teeth pressing against the soft tissues.
- Why it's mild: These indentations are usually faint and not painful, unlike the more pronounced and sometimes ulcerated soft tissue damage seen in severe cases.
6. Unexplained Toothaches
- Description: You might experience dull, persistent toothaches that don't seem to be related to cavities or other obvious dental issues.
- Why it's mild: The pain is usually manageable and not sharp or throbbing like that of an abscess.
Pro Tip: Keep a symptom journal for a week or two. Note down when you experience jaw pain, headaches, or tooth sensitivity, and if there are any associated triggers like stress or a restless night's sleep. This detailed information will be invaluable for your dentist during diagnosis.
Treatment Options for Mild Bruxism Teeth
Fortunately, mild bruxism is highly treatable, often with conservative, non-invasive methods. The goal is to alleviate symptoms, protect teeth from further damage, and address the underlying causes.
1. Oral Appliances (Mouthguards/Nightguards)
This is the most common and effective treatment for both awake and sleep bruxism, particularly for protecting teeth grinding molars.
-
Custom-Made Nightguards:
- Description: Fabricated by your dentist after taking impressions of your teeth. Made from durable acrylic, these fit precisely over your upper or lower teeth. They act as a protective barrier, preventing direct contact between your teeth and distributing clenching forces evenly.
- Pros: Superior fit, comfort, and durability. Highly effective at preventing tooth wear and reducing jaw strain. Can last for several years.
- Cons: Higher initial cost. Requires a dental visit.
- Cost: $300 - $800+ in the US, depending on materials, complexity, and regional dental fees. Some dental insurance plans may cover a portion.
-
Over-the-Counter (OTC) Mouthguards:
- Description: Available at pharmacies. "Boil-and-bite" guards are molded to your teeth at home. Softer, generic guards are also available.
- Pros: Inexpensive, readily available, provides immediate, temporary relief and protection.
- Cons: Less durable, poorer fit (can be bulky or uncomfortable), may not stay in place well, can potentially shift your bite if used long-term or improperly, and may not be suitable for significant bruxism.
- Cost: $25 - $50.
Pro Tip: If you opt for an OTC guard as a temporary measure, ensure it fits snugly and doesn't interfere with your breathing. Always discuss its suitability with your dentist.
2. Stress Management Techniques
Since stress and anxiety are major contributors, addressing them is paramount for how to stop teeth clenching.
- Mindfulness & Meditation: Practices that focus on present moment awareness can reduce overall stress levels.
- Yoga & Deep Breathing Exercises: Promote relaxation and can reduce muscle tension throughout the body, including the jaw.
- Cognitive Behavioral Therapy (CBT): A type of therapy that helps identify and change negative thought patterns and behaviors contributing to stress.
- Exercise: Regular physical activity is an excellent stress reliever.
- Adequate Sleep: Prioritizing 7-9 hours of quality sleep can significantly reduce stress and improve muscle recovery.
3. Biofeedback
- Description: This technique uses electronic devices to monitor physiological responses (like muscle tension) and provide real-time feedback. For bruxism, a device might alert you when you start clenching, helping you consciously relax your jaw.
- Pros: Teaches self-awareness and self-regulation. Non-invasive.
- Cons: Can be expensive, requires specialized equipment and training, effectiveness varies.
4. Behavioral Therapies and Jaw Relaxation Techniques
- Awareness Training: Consciously monitoring your jaw position throughout the day. The "lips together, teeth apart" mantra helps maintain a relaxed jaw.
- Jaw Exercises: Gentle stretches and massages can relieve tension in the jaw muscles. Your dentist or a physical therapist can demonstrate specific exercises.
- Avoid Stimulants: Reducing caffeine, alcohol, and nicotine intake, especially before bed, can help relax jaw muscles and improve sleep quality.
5. Dental Corrections
In some cases, if malocclusion is identified as a significant contributing factor, minor dental adjustments might be recommended.
- Occlusal Adjustments (Enameloplasty): Reshaping the biting surfaces of a few teeth to improve the bite relationship.
- Orthodontics: In rare cases of severe misalignment, braces or clear aligners might be considered, though this is less common for mild bruxism unless other orthodontic needs exist.
6. Medications (Less Common for Mild Bruxism)
- Muscle Relaxants: Prescribed for short-term use to alleviate acute jaw pain and muscle spasms, but not a long-term solution.
- Botulinum Toxin (Botox): Injections into the jaw muscles (masseters) can temporarily paralyze them, reducing clenching intensity. While effective, it's typically reserved for severe, persistent bruxism when other treatments have failed, due to its cost and invasive nature. It's rarely recommended for mild cases.
Comparison Table: Mouthguard Options for Bruxism
| Feature | Custom-Fitted Nightguard (Dentist) | Over-the-Counter Nightguard (Boil-and-Bite) |
|---|---|---|
| Fit & Comfort | Excellent; molded precisely to your teeth for optimal comfort. | Variable; can be bulky, uncomfortable, or ill-fitting. |
| Material | Durable acrylic (hard or soft-hard laminate) for longevity. | Softer plastic or rubber; less durable. |
| Protection | Superior protection against tooth wear and even force distribution. | Basic protection; may not cover all teeth grinding molars effectively. |
| Durability | 2-5+ years with proper care. | 3-6 months, often less. |
| Cost (US) | $300 - $800+ (varies by region/materials). | $25 - $50. |
| Insurance | Often partially covered by dental insurance for sleep bruxism. | Rarely covered by insurance. |
| Dental Oversight | Required; ensures proper fit and addresses bite issues. | No professional oversight; self-fitted. |
| Effectiveness | Highly effective for reducing symptoms and preventing damage. | Limited; suitable for temporary or very mild symptoms. |
Step-by-Step Process: What to Expect During Treatment
If you suspect you have mild bruxism, seeking professional dental advice is the first and most crucial step. Here’s a typical journey through diagnosis and treatment:

Step 1: Initial Dental Consultation and Diagnosis
- Your Role: Schedule an appointment with your dentist. Be prepared to discuss your symptoms (headaches, jaw pain, sensitivity), when they occur (morning, daytime), potential stressors, and any observations from family members (e.g., grinding sounds).
- Dentist's Role:
- Clinical Examination: Your dentist will visually inspect your teeth for signs of wear, chips, or fractures, particularly on
teeth grinding molars. They will examine your jaw muscles for tenderness, swelling, or hypertrophy (enlargement). Your bite will also be assessed. - Palpation: They will gently feel your jaw joints and muscles to check for pain or tenderness.
- Discussion: They'll ask about your medical history, sleep habits, stress levels, and medications.
- Diagnosis: Based on the examination and your reported symptoms, your dentist will diagnose mild bruxism. They may also suggest screening for related issues like sleep apnea if indicated.
- Clinical Examination: Your dentist will visually inspect your teeth for signs of wear, chips, or fractures, particularly on
Step 2: Treatment Planning and Discussion
- Dentist's Role: Your dentist will present a range of treatment options tailored to your specific case of mild bruxism, explaining the pros and cons of each. For mild cases, this typically involves oral appliances, behavioral strategies, and stress management.
- Your Role: Actively participate in the discussion. Ask questions about costs, expected outcomes, and the commitment required for each option. This is where you'll decide on the best course of action, often starting with the least invasive.
Step 3: Appliance Fabrication (If Chosen)
- If choosing a custom nightguard:
- Impressions: The dental team will take impressions (molds) of your upper and/or lower teeth. Some modern practices use digital scans instead of physical molds.
- Bite Registration: They will record how your upper and lower jaws come together to ensure the nightguard fits your natural bite.
- Lab Fabrication: The impressions/scans are sent to a dental lab where your custom nightguard is fabricated, a process that usually takes 1-2 weeks.
Step 4: Appliance Fitting and Adjustments
- Dentist's Role: Once your custom nightguard is ready, you'll return for a fitting appointment. The dentist will ensure it fits comfortably and securely, without impinging on your gums or interfering with your bite. They will make any necessary adjustments on the spot.
- Your Role: Provide honest feedback about the fit and feel. You'll receive instructions on
how to stop teeth clenching(e.g., with awareness), how to insert and remove the guard, and how to clean and care for it.
Step 5: Implementing Behavioral and Lifestyle Changes
- Your Role: This is an ongoing process.
- Stress Management: Integrate techniques like meditation, yoga, or professional counseling into your routine.
- Awareness: Practice conscious jaw relaxation throughout the day ("lips together, teeth apart").
- Dietary Changes: Reduce caffeine, alcohol, and nicotine.
- Sleep Hygiene: Establish a consistent sleep schedule and create a relaxing bedtime routine.
- Dentist's Role: Offer resources or referrals to specialists (e.g., therapists, sleep specialists) if needed.
Step 6: Follow-up and Monitoring
- Dentist's Role: Schedule follow-up appointments (typically a few weeks after starting treatment) to check on your progress, evaluate the nightguard's effectiveness, and assess any changes in your symptoms or dental health.
- Your Role: Report any improvements or lingering issues. Your dentist will continue to monitor your teeth for wear and your jaw for any signs of worsening bruxism. Nightguards typically need replacement every 2-5 years.
This structured approach ensures that your mild bruxism is effectively managed and that you receive ongoing care to prevent its progression.
Cost and Insurance: Understanding the Financial Aspect
The cost of treating mild bruxism varies significantly based on the chosen treatment method and your geographic location within the US.
Average US Costs for Common Treatments:
| Treatment Type | Average US Cost Range (Without Insurance) | Notes |
|---|---|---|
| Over-the-Counter Nightguard | $25 - $50 | Readily available, temporary solution. |
| Custom-Fitted Nightguard | $300 - $800+ | Most common and effective dental appliance. Prices vary by material and region. |
| Occlusal Adjustment (Minor) | $50 - $200 per tooth | Minor reshaping of a few teeth to correct bite issues. |
| Biofeedback Therapy | $75 - $200 per session | Often requires multiple sessions; may or may not be covered by medical insurance. |
| Cognitive Behavioral Therapy (CBT) | $100 - $250 per session | Varies widely by therapist, region, and whether individual/group sessions. |
| Botox Injections (for Bruxism) | $500 - $1,500+ per session | Typically for severe bruxism; requires repeat injections every 3-6 months. |
| Initial Dental Exam | $50 - $150 | Often covered by dental insurance. |
Costs are estimates and can vary. It's always best to get a detailed quote from your dental provider.
Insurance Coverage Details:
Navigating insurance for bruxism treatment can be complex, as coverage depends on whether your plan classifies bruxism as a dental or medical issue, and the specific codes used by your dentist.
-
Dental Insurance:
- Custom Nightguards: Many dental insurance plans offer partial coverage for custom nightguards, especially if they are deemed medically necessary for sleep bruxism. You might find coverage ranging from 50% to 80% after meeting your deductible. The procedure code D9940 (occlusal guard) is typically used.
- Dental Exams & X-rays: Routine diagnostic services that lead to a bruxism diagnosis are almost always covered at a high percentage (80-100%).
- Occlusal Adjustments: Minor adjustments might be covered, but extensive bite correction (orthodontics) is usually considered cosmetic unless it's for severe functional impairment.
- What's NOT Covered: Over-the-counter nightguards are generally not covered.
-
Medical Insurance:
- Oral Appliances for Sleep Apnea: If your bruxism is linked to sleep apnea, and a custom oral appliance is prescribed to manage sleep apnea, it might be covered by your medical insurance as a Durable Medical Equipment (DME) item. This is more common for severe cases but worth exploring for mild symptoms potentially linked to sleep-disordered breathing.
- CBT/Biofeedback: Therapy sessions with licensed professionals (psychologists, physical therapists) might be covered under your medical plan's mental health or rehabilitation benefits.
- Botox Injections: If deemed medically necessary for severe chronic bruxism or TMJ disorders, some medical plans might offer limited coverage, but it's rare for mild bruxism.
Pro Tip: Always call your insurance provider directly before starting treatment. Ask about coverage for specific procedure codes (e.g., D9940 for nightguards), your deductible, co-insurance, and annual maximums. Get pre-authorization if possible.
Recovery and Aftercare: Sustaining Relief
Managing mild bruxism is often an ongoing process that requires consistent effort. Recovery isn't about a single cure, but about sustained relief and preventing progression.
1. Consistent Use of Oral Appliances
- Nightguards: If you're using a custom nightguard, wear it every night as instructed by your dentist, even if your symptoms improve. Consistency is key to protecting your teeth and maintaining jaw relaxation.
- Cleaning: Clean your nightguard daily with a toothbrush and mild soap or a non-abrasive denture cleaner. Rinse thoroughly. Store it in its protective case when not in use to prevent bacterial growth and damage.
- Inspection: Periodically check your nightguard for signs of wear and tear, cracks, or damage. A worn nightguard needs to be replaced to ensure continued protection.
2. Adherence to Stress Management
- Daily Practice: Integrate stress-reducing activities (meditation, deep breathing, yoga, exercise) into your daily routine. Don't wait for stress to build up; proactive management is more effective.
- Identify Triggers: Become aware of situations or emotions that trigger your clenching or grinding. Once identified, you can develop coping strategies.
3. Continual Awareness and Behavioral Modification
- Jaw Relaxation: Make "lips together, teeth apart" your mantra. Periodically check in with your jaw throughout the day to ensure it's relaxed.
- Avoid Habits: Be mindful of habits like chewing gum excessively, biting nails, or clenching your jaw when concentrating, as these can exacerbate bruxism.
4. Regular Dental Check-ups
- Monitoring: Continue with your regular dental check-ups (typically every 6 months). Your dentist will monitor your teeth for any new signs of wear, assess your jaw joints, and check the fit and condition of your nightguard.
- Adjustments: Your bite can change over time, requiring minor adjustments to your nightguard or even to your natural teeth (occlusal adjustment) to maintain optimal function and comfort.
5. Healthy Lifestyle Choices
- Balanced Diet: Support overall health, including oral health.
- Limit Stimulants: Reduce consumption of caffeine, alcohol, and nicotine, especially in the hours leading up to bedtime.
- Adequate Sleep: Prioritize quality sleep to help your body and jaw muscles fully recover and relax.
By consistently adhering to these aftercare practices, you can effectively manage mild bruxism, prevent it from worsening, and protect your dental health for years to come.
Prevention: Stopping Bruxism Before It Starts or Worsens
While you might not be able to eliminate all potential causes of bruxism, there are several proactive steps you can take to prevent its onset or stop mild bruxism from progressing to a more severe form. This is especially important for how to stop teeth clenching and reduce teeth grinding molars.
1. Stress Reduction Techniques
- Practice Relaxation: Incorporate daily relaxation techniques such as meditation, deep breathing exercises, progressive muscle relaxation, or mindfulness. Even 10-15 minutes a day can make a significant difference.
- Manage Workload: Learn to delegate, set boundaries, and avoid overcommitting.
- Seek Support: If stress or anxiety feels overwhelming, consider talking to a therapist or counselor.
2. Improve Sleep Hygiene
- Consistent Schedule: Go to bed and wake up at the same time each day, even on weekends.
- Create a Routine: Develop a relaxing bedtime routine, such as a warm bath, reading a book, or listening to calming music.
- Optimize Sleep Environment: Ensure your bedroom is dark, quiet, and cool.
- Avoid Stimulants Before Bed: Limit caffeine, alcohol, and nicotine for several hours before sleep.
- Screen Time: Reduce exposure to screens (phones, tablets, computers, TV) at least an hour before bedtime, as blue light can disrupt melatonin production.
3. Develop Jaw Awareness
- Conscious Relaxation: Throughout the day, periodically check your jaw position. Your teeth should not be touching when your jaw is at rest. The correct resting position is "lips together, teeth apart."
- "N" Sound Test: Gently make an "N" sound; the position your tongue takes against the roof of your mouth is its natural resting position, which should leave your teeth slightly separated.
- Post-it Note Reminders: Place sticky notes on your computer, dashboard, or other frequently seen places to remind you to relax your jaw.
4. Avoid Hard, Chewy, or Crunchy Foods
- Reduce Strain: Temporarily avoiding extremely hard candies, ice chewing, tough meats, or excessive gum chewing can give your jaw muscles a break and reduce strain.
5. Address Underlying Health Issues
- Sleep Apnea Screening: If you snore loudly, experience daytime fatigue, or have observed breathing pauses during sleep, talk to your doctor about screening for sleep apnea. Treating sleep apnea can significantly reduce sleep bruxism.
- Medication Review: If you start a new medication and notice bruxism symptoms, discuss it with your prescribing doctor. They may be able to adjust the dosage or suggest an alternative.
6. Regular Dental Check-ups
- Early Detection: Regular visits allow your dentist to spot early signs of wear on your
teeth grinding molarsor other symptoms before they become severe. Early detection leads to easier and more effective intervention.
Risks and Complications: What Can Go Wrong
While mild bruxism might seem benign, ignoring it can lead to a cascade of more serious dental and health problems over time. The "mild" can easily become "severe."
1. Progression to Severe Bruxism
The most significant risk is that mild bruxism will worsen in frequency and intensity. What starts as occasional clenching can evolve into nightly, forceful grinding, leading to rapid and extensive damage.
2. Significant Tooth Damage
- Tooth Wear: Chronic grinding wears down the enamel, leading to flattened, shortened teeth. This exposes the softer dentin underneath, which wears even faster.
- Fractures and Chips: The immense pressure can cause teeth to chip, crack, or even fracture, potentially leading to nerve damage and requiring complex procedures like root canals, crowns, or even extractions. This is particularly concerning for
teeth grinding molarsthat experience the highest bite forces. - Loose Teeth: Persistent clenching and grinding can weaken the bone and ligaments supporting the teeth, causing them to become loose.
- Damage to Restorations: Fillings, crowns, bridges, and veneers can be damaged, cracked, or dislodged by bruxism, requiring costly replacements.
3. Temporomandibular Joint (TMJ) Disorders
The TMJ is a complex joint, and chronic strain from bruxism can lead to:
- Pain and Tenderness: In and around the jaw joint, ears, face, and neck.
- Clicking or Popping: Sounds when moving the jaw.
- Limited Jaw Movement: Difficulty opening or closing the mouth completely, or a jaw that gets "stuck" or "locked."
- Headaches and Migraines: Chronic tension in the jaw muscles can trigger severe headaches and migraines, extending beyond typical morning tension.
4. Gum Recession and Bone Loss
The forces of bruxism can contribute to gum recession and potentially exacerbate periodontal disease (gum disease) by weakening the supporting structures around the teeth.

5. Sleep Disturbances for Partners
While primarily affecting the individual, loud teeth grinding molars can significantly disturb a sleeping partner, leading to relationship strain and sleep deprivation for both individuals.
6. Impact on Quality of Life
Chronic pain from bruxism (headaches, jaw pain), difficulty eating, or concerns about dental damage can significantly reduce a person's quality of life, leading to irritability, fatigue, and difficulty concentrating.
By understanding these potential risks, individuals with mild bruxism are empowered to take proactive steps towards prevention and early intervention, protecting both their oral health and overall well-being.
Children / Pediatric Considerations
Bruxism is surprisingly common in children, affecting an estimated 15-30% of those under the age of 11. While it's often a temporary and benign condition in kids, parents should be aware of the signs and when to seek dental advice.
Why Children Grind Their Teeth
- Developing Jaw and Teeth: Children's jaws and teeth are constantly changing. They may grind as their baby teeth come in, as they lose baby teeth, or as their permanent teeth erupt. This is often a way for them to explore their bite.
- Stress and Anxiety: Just like adults, children can experience stress from school, family changes, new environments, or even excitement.
- Allergies and Ear Infections: Nasal congestion from allergies or ear infections can cause children to unconsciously clench or move their jaw in an attempt to clear their airways or alleviate discomfort.
- Sleep Disorders: Snoring or mild sleep apnea can also trigger sleep bruxism in children.
- Malocclusion: Sometimes, a slight misalignment of baby teeth can contribute.
Signs and Symptoms in Children
- Audible Grinding: Parents often notice grinding sounds at night.
- Morning Headaches or Facial Pain: Though less common in young children, older children might report these.
- Tooth Sensitivity: Complaining of pain when eating hot or cold foods.
- Wear on Baby Teeth: Your child's dentist might observe flattened baby teeth.
- Jaw Soreness: Child complains of a sore jaw.
When to Be Concerned and See a Pediatric Dentist
Most cases of childhood bruxism resolve on their own by the time permanent teeth fully erupt. However, consult a pediatric dentist if:
- Your child complains of persistent jaw pain or headaches.
- There's significant or rapid wear on their teeth.
- They experience noticeable tooth sensitivity.
- The grinding sounds are very loud or frequent, disrupting their sleep or yours.
- You notice swelling around their jaw.
Treatment for Pediatric Bruxism
- Observation: For most mild cases, the primary "treatment" is simply observation.
- Stress Management: Help children manage stress through open communication, consistent routines, and relaxing bedtime activities.
- Nightguards: Custom-fitted nightguards are typically not recommended for very young children as their mouths are constantly changing. They might be considered for older children or teenagers with severe symptoms or significant tooth wear, but often as a temporary measure.
- Addressing Underlying Issues: Treating allergies, ear infections, or sleep apnea can help.
Pro Tip for Parents: Focus on creating a calm and positive bedtime routine. If you're concerned, don't hesitate to mention it to your pediatric dentist at your child's next check-up. They can monitor your child's dental development and offer tailored advice.
Cost Breakdown: A Detailed Look at Expenses
Understanding the potential financial commitment for bruxism treatment is crucial for planning. While a nightguard is the most common intervention for mild bruxism teeth and teeth grinding molars, other costs can arise.
Average US Costs (Low, Mid, High Estimates):
| Service/Item | Low Estimate (US$) | Mid Estimate (US$) | High Estimate (US$) | Details |
|---|---|---|---|---|
| Initial Dental Exam & X-rays | $50 | $150 | $250 | This is the starting point for diagnosis. Often covered by dental insurance. |
| Over-the-Counter Nightguard | $25 | $35 | $50 | DIY, temporary. |
| Custom Hard Acrylic Nightguard | $300 | $550 | $800 | Durable, precise fit, often covers full arch. Material and lab fees vary. |
| Custom Soft/Dual Laminate Nightguard | $250 | $450 | $700 | Softer inner layer for comfort, harder outer layer for durability. |
| Occlusal Adjustment (minor) | $50 | $100 | $200 | Per tooth, for minor bite correction. |
| Biofeedback Session | $75 | $120 | $200 | Per session; several sessions typically required. |
| CBT/Therapy Session | $100 | $175 | $250 | Per session; can be ongoing. Medical insurance may apply. |
| Full Mouth Series X-rays | $75 | $150 | $250 | May be needed for detailed assessment of tooth wear and bone structure. |
| Follow-up Appointments | $0 | $50 | $100 | May be included in initial cost or charged separately, depending on the clinic. |
With vs. Without Insurance:
- Without Insurance (Out-of-Pocket): You will be responsible for 100% of all costs. A custom nightguard would typically fall in the $300-$800+ range. Other services like exams and X-rays would add to this.
- With Dental Insurance:
- Deductible: You'll likely need to pay an annual deductible (e.g., $50-$150) before your insurance starts covering costs.
- Co-insurance: After your deductible, insurance might cover 50-80% of the cost for a custom nightguard (code D9940). This means your out-of-pocket for a $500 nightguard could be $100-$250 if your plan covers 60-80%.
- Annual Maximums: Most dental plans have annual maximums (e.g., $1,000-$2,000). If you have other dental work, you might hit this limit.
- Waiting Periods: Some plans have waiting periods for major services, which might include nightguards.
- Medical Insurance: For treatments like CBT or if an oral appliance is prescribed for sleep apnea, your medical insurance might cover a portion under mental health or DME benefits. This often comes with its own deductible and co-pays.
Payment Plans and Financing Options:
Many dental practices understand the financial burden and offer solutions:
- In-house Payment Plans: Some offices allow you to pay in installments over several months, often without interest.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare credit cards or loans that can cover dental expenses. These often offer interest-free periods if paid off within a certain timeframe.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these pre-tax dollars to pay for bruxism treatments, including nightguards, exams, and therapy sessions.
Cost-Saving Tips:
- Shop Around: Get quotes from a few different dentists. Prices can vary.
- Utilize Insurance: Understand your benefits thoroughly and get pre-authorization for costly treatments.
- Dental Schools: Dental schools often offer services at reduced rates, as they are training future dentists.
- Preventative Care: Regular cleanings and check-ups can catch bruxism early, preventing more costly treatments down the line.
- Address Root Causes: Investing in stress management or sleep apnea treatment can ultimately save you money on dental repairs caused by uncontrolled bruxism.
Frequently Asked Questions
What does mild bruxism feel like?
Mild bruxism often feels like a subtle, persistent tension in your jaw muscles, especially upon waking. You might notice slight headaches around your temples, a dull toothache on your molars, or a general feeling of fatigue in your jaw. It typically doesn't involve intense pain or significant interference with daily activities, but rather a low-level chronic discomfort.
Can mild bruxism go away on its own?
Sometimes, mild bruxism, especially in children or if triggered by a temporary stressor, can resolve on its own once the underlying cause is removed. However, in adults, if the contributing factors like stress or certain habits persist, it's more likely to continue or even worsen without intervention. It's always best to address it to prevent long-term damage.
How do I stop teeth clenching during the day?
Stopping daytime clenching primarily involves awareness and behavioral techniques. Consciously monitor your jaw position, aiming for "lips together, teeth apart" at rest. Set visual or auditory reminders, practice jaw relaxation exercises, and use stress management techniques throughout the day to reduce overall muscle tension.
Can stress alone cause mild bruxism?
Yes, stress is a major contributing factor to bruxism, both awake and sleep-related. Emotional tension, anxiety, and daily stressors can lead to involuntary muscle contraction, including the powerful jaw muscles, resulting in clenching or grinding, even at a mild level. Managing stress is often a key component of treatment.
Is a nightguard always necessary for mild bruxism?
Not always, but it's a highly recommended and effective first line of defense, especially for sleep bruxism affecting teeth grinding molars. For very mild cases, initial interventions might focus solely on stress management and behavioral changes. However, a nightguard provides crucial physical protection for your teeth and jaw joints, preventing wear and allowing muscles to relax.
How long does it take for bruxism treatment to work?
You might notice an improvement in symptoms like morning headaches and jaw soreness within a few days to a couple of weeks of consistently using a nightguard. Behavioral and stress management techniques require ongoing practice, with noticeable improvements often appearing over several weeks or months as new habits form.
What's the average cost of a custom nightguard in the US?
A custom-fitted nightguard from a dentist in the US typically ranges from $300 to $800 or more, depending on the materials used (hard acrylic is more durable and costly), the complexity of your bite, and regional dental fees. Dental insurance often covers a portion of this cost.
Can mild bruxism lead to TMJ problems?
Yes, absolutely. Even mild, chronic clenching and grinding place undue stress on the temporomandibular joints (TMJs) and the surrounding muscles. Over time, this constant strain can contribute to the development or exacerbation of TMJ disorders (TMDs), leading to symptoms like jaw pain, clicking, popping, and limited jaw movement.
Are there natural remedies for mild bruxism?
Natural remedies primarily focus on stress reduction and muscle relaxation. These include herbal teas (chamomile, valerian root), essential oil diffusers (lavender), warm compresses on the jaw, gentle jaw massages, yoga, meditation, and ensuring adequate sleep. While they can help manage symptoms, they don't replace professional dental evaluation or appliances for tooth protection.
Can lifestyle changes prevent mild bruxism from worsening?
Yes, significant lifestyle changes can play a crucial role in preventing mild bruxism from progressing. Reducing caffeine and alcohol intake, quitting smoking, adopting stress-reducing practices, improving sleep hygiene, and maintaining awareness of jaw clenching habits are all effective strategies to mitigate the triggers and severity of bruxism.
When to See a Dentist
Recognizing when your mild symptoms warrant a professional dental visit is critical for preventing more severe complications. Don't wait until the damage is extensive.
Red Flags That Need Immediate Attention:
- Sudden, Sharp, or Intense Jaw Pain: Especially if it restricts your ability to open or close your mouth fully.
- Jaw Locking or Clicking with Pain: If your jaw gets stuck or makes loud, painful noises when you move it.
- Severe Tooth Sensitivity: Pain that is constant, throbbing, or unbearable, which might indicate nerve involvement or a cracked tooth.
- Dental Fractures: Any visible crack, chip, or breakage in your teeth, especially if it causes pain.
- Difficulty Eating: If chewing becomes consistently painful or difficult.
- Audible Grinding: If a sleeping partner reports loud, frequent grinding sounds, indicating a higher intensity of sleep bruxism.
When to Schedule a Routine Appointment:
- Persistent Mild Symptoms: If you consistently experience morning headaches, jaw stiffness, or mild tooth sensitivity for more than a few weeks.
- Suspected Clenching/Grinding: If you or a family member suspects you are clenching or grinding, even if symptoms are subtle.
- Changes in Your Bite: If you notice your teeth don't fit together as they used to.
- Indented Tongue or Cheek Marks: These are clear signs of pressure, even if not painful.
- Concerns About Tooth Wear: If you notice any flattening or wearing down of your teeth, particularly your
teeth grinding molars. - New or Increased Stress: If you're going through a period of increased stress or anxiety and want to proactively prevent bruxism from developing or worsening.
Remember, early detection and intervention are key to managing mild bruxism effectively and protecting your long-term oral health. Your dentist can accurately diagnose the condition, rule out other potential issues, and recommend the most appropriate course of action tailored to your specific needs.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

What Causes Teeth Grinding in Sleep
More than one in ten adults—and even more children—clench or grind their teeth during sleep, a condition known medically as sleep bruxism. For many, it's an unconscious habit that goes unnoticed until significant damage or discomfort arises. Waking up with a dull, constant headache, jaw pain, or
February 23, 2026
How to Not Grind Teeth at Night
More than one in ten adults and a significant percentage of children experience teeth grinding, medically known as bruxism, a condition that often goes unnoticed, especially when it occurs during sleep. If you've woken up with a sore jaw, a dull headache, or noticed your teeth becoming unusually
February 23, 2026

What Is Jaw Clenching
Do you often wake up with a dull headache, a sore jaw, or unexplained tooth sensitivity? You're not alone. Approximately 1 in 10 adults and up to 3 in 10 children experience some form of bruxism, a condition characterized by grinding, gnashing, or clenching your teeth. At the heart of this wides
February 23, 2026
Severe Bruxism Molars: Complete Guide
When the quiet of the night is shattered by a grinding, grating sound, or when you wake up with an aching jaw and teeth that feel oddly sensitive, it’s often a sign of bruxism. But what happens when this condition intensifies, leading to significant damage, especially to your back teeth? This is the
February 23, 2026