Swelling Under Ear Behind Jaw: Complete Guide
Key Takeaways
- Experiencing swelling under ear behind jaw can be unsettling, often appearing suddenly and causing significant discomfort. While sometimes a minor issue, it can also signal a serious underlying condition requiring immediate medical or dental attention. Did you know that infections originating fr
Experiencing swelling under ear behind jaw can be unsettling, often appearing suddenly and causing significant discomfort. While sometimes a minor issue, it can also signal a serious underlying condition requiring immediate medical or dental attention. Did you know that infections originating from your teeth are a surprisingly common culprit for this type of swelling, potentially leading to complications if left untreated? Ignoring such a symptom can escalate from localized pain to systemic issues, impacting your overall health and well-being.
This comprehensive guide from SmilePedia.net aims to demystify the causes, symptoms, and treatments for swelling under the ear behind the jaw. We'll explore everything from common dental infections and salivary gland issues to swollen lymph nodes, providing you with the knowledge to understand your symptoms and seek appropriate care. You'll learn what to look for, what treatment options are available, typical costs involved, and crucial steps for recovery and prevention. Understanding this complex area is vital for maintaining your oral and general health, empowering you to make informed decisions about your care.
Key Takeaways:
- Swelling under ear behind jaw often indicates an infection (dental, salivary gland, lymph node) or inflammation, and rarely, a benign or malignant growth.
- Immediate dental or medical evaluation is crucial for persistent or worsening swelling, especially if accompanied by fever, difficulty swallowing, or breathing issues.
- Treatment costs can range from $150-$500 for antibiotics and initial consultations to $1,000-$5,000+ for surgical interventions like salivary stone removal or dental extractions, potentially higher for complex cases like tumor removal.
- Recovery timelines vary from a few days with antibiotics to several weeks post-surgery, with proper aftercare being essential for preventing recurrence.
- Dental infections (like abscesses from wisdom teeth) are a common cause and require prompt professional intervention to prevent spread and complications.
- Submandibular gland swelling treatment often involves antibiotics for infection, hydration, massage, and sometimes surgical removal of salivary stones (sialolithiasis).
- Prevention includes rigorous oral hygiene, regular dental check-ups, and staying hydrated to support salivary gland function.
What It Is / Overview
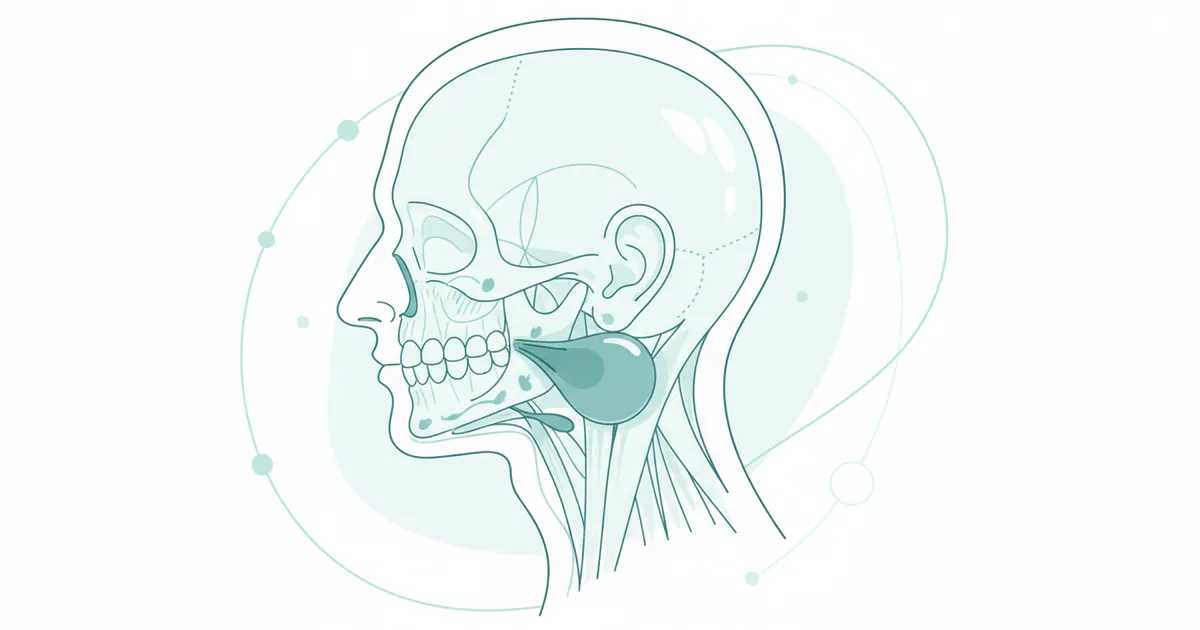
Swelling under the ear behind the jaw refers to an abnormal enlargement or protrusion in the area inferior to the earlobe and posterior to the angle of the mandible (jawbone). This region is anatomically complex, housing major salivary glands (primarily the parotid and submandibular glands), numerous lymph nodes, muscles, nerves, and blood vessels. When swelling occurs here, it indicates an underlying issue affecting one or more of these structures. The swelling can manifest in various ways: it might be soft or firm, painful or painless, localized or diffuse, and can range in size from a small bump to a significant protrusion that visibly alters facial contours. Understanding its characteristics is the first step toward accurate diagnosis and effective treatment.

Types / Variations
The nature of the swelling often depends on the specific structure affected. While the symptom "swelling under ear behind jaw" is singular, the underlying conditions causing it are diverse. Here are the primary types or categories of issues that lead to this symptom:
1. Salivary Gland Swelling (Sialadenitis)
This is a common cause, affecting either the parotid gland (located just in front of and below the ear) or the submandibular gland (located beneath the jawline).
- Parotitis: Inflammation of the parotid gland. Can be viral (e.g., mumps), bacterial, or due to blockages (stones).
- Submandibular Sialadenitis: Inflammation of the submandibular gland. Often caused by stones (sialolithiasis) blocking the duct, leading to bacterial infection.
2. Lymph Node Swelling (Lymphadenitis)
The neck and jaw area are rich in lymph nodes, which are part of the immune system. They can swell in response to infection or inflammation anywhere in the head and neck.
- Infectious Mononucleosis: Viral infection causing widespread lymph node swelling.
- Bacterial Infections: From throat infections (strep throat), ear infections, or dental infections.
- Viral Infections: Common cold, flu, HIV.
3. Dental Infections
Infections originating from teeth can spread to surrounding tissues, causing swelling in the submandibular or parotid regions.
- Dental Abscess: A pocket of pus caused by bacterial infection, often at the root of a tooth.
- Pericoronitis: Inflammation of the gum tissue surrounding a partially erupted wisdom tooth, which can lead to significant swelling in the jaw and neck.
- Cellulitis: A rapidly spreading bacterial infection of the skin and underlying tissues, which can originate from a dental abscess.
4. Cysts and Tumors
Less common but more serious causes include benign or malignant growths.
- Benign Cysts: Such as a branchial cleft cyst (a congenital neck lump) or a sebaceous cyst.
- Benign Tumors: Pleomorphic adenoma (common in salivary glands), lipomas (fatty lumps).
- Malignant Tumors: Salivary gland cancer, lymphoma, squamous cell carcinoma (often associated with head and neck cancer).
5. Other Inflammatory Conditions
- TMJ Disorders: While primarily causing pain, severe temporomandibular joint dysfunction can sometimes present with localized swelling.
- Trauma: Injury to the jaw or neck area can result in immediate swelling due as a response to tissue damage.
Causes / Why It Happens
Understanding the specific causes behind swelling under ear behind jaw is crucial for proper diagnosis. The localized nature of the swelling often points directly to the affected anatomical structure.
1. Infections of the Salivary Glands (Sialadenitis)
Salivary gland infections are a primary reason for this type of swelling.
- Sialolithiasis (Salivary Stones): These calcified deposits can form in the salivary ducts, most commonly in the submandibular gland (Warton's duct) but also in the parotid gland (Stensen's duct). A stone can obstruct the flow of saliva, leading to a backup of saliva, inflammation, and subsequent bacterial infection (acute sialadenitis). The swelling often worsens during or after meals when saliva production increases.
- Bacterial Sialadenitis: Can occur secondary to duct obstruction (stones, strictures), dehydration, poor oral hygiene, or compromised immune systems. Common bacteria include Staphylococcus aureus.
- Viral Sialadenitis (Mumps): The classic example is mumps, a highly contagious viral infection that causes painful swelling of the parotid glands, often on both sides, though it can affect one side initially. Other viruses like influenza, parainfluenza, and Epstein-Barr virus can also cause sialadenitis.
- Autoimmune Conditions: Sjögren's syndrome, for example, can cause chronic inflammation and enlargement of salivary glands.
2. Swollen Lymph Nodes (Lymphadenopathy/Lymphadenitis)
Lymph nodes act as filters for the immune system, trapping bacteria, viruses, and other foreign particles. When an infection or inflammatory process occurs in the head or neck, the regional lymph nodes swell as they work to fight it off.
- Upper Respiratory Infections: Common colds, flu, sinusitis, tonsillitis, pharyngitis, and ear infections are frequent causes of reactive lymphadenopathy in the neck and submandibular regions.
- Dental Infections: An abscessed tooth or severe gum disease can cause the nearby submandibular or cervical lymph nodes to swell as the body fights the bacterial infection.
- Skin Infections: Folliculitis, cellulitis, or other skin lesions on the scalp, face, or neck can trigger regional lymph node swelling.
- Mononucleosis (Mono): Caused by the Epstein-Barr virus, mono is known for causing significant, generalized lymph node swelling, including those behind the jaw.
- Tuberculosis, HIV, Cat Scratch Disease: Less common but important infectious causes.
- Cancer: Lymphoma or metastatic cancer spreading from other areas of the head and neck can cause firm, often painless, persistent lymph node enlargement.
3. Dental Origin
Dental issues are a significant and often overlooked cause of swelling in this area, sometimes requiring urgent attention.
- Periapical Abscess: An infection at the tip of a tooth root, often due to severe tooth decay, trauma, or failed root canal treatment. If the infection spreads from the jawbone into the surrounding soft tissues, it can cause significant facial or submandibular swelling. This is a common cause of swelling under ear behind jaw.
- Pericoronitis: Inflammation and infection of the gum tissue around a partially erupted tooth, most commonly a lower wisdom tooth. Food and bacteria can get trapped under the gum flap, leading to infection that can spread to the jaw, cheek, and neck, causing pain, trismus (difficulty opening mouth), and pronounced swelling.
- Cellulitis (Odontogenic): A rapidly spreading bacterial infection of the skin and subcutaneous tissues originating from an untreated dental abscess. This is a serious condition that can spread to the neck and potentially compromise the airway (Ludwig's Angina).
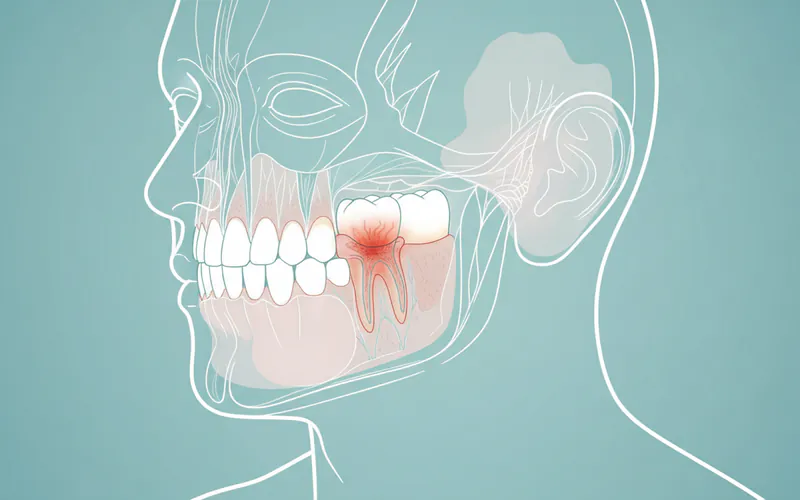
4. Cysts, Tumors, and Other Growths
- Salivary Gland Tumors: Benign tumors like pleomorphic adenomas are common in the parotid gland but can also occur in the submandibular gland. Malignant tumors (e.g., mucoepidermoid carcinoma) are less common but require prompt diagnosis.
- Cysts:
- Branchial Cleft Cysts: Congenital cysts that result from incomplete obliteration of branchial arches during embryonic development, often appearing as a soft, sometimes infected lump in the neck or under the jaw.
- Thyroglossal Duct Cysts: While typically midline, they can sometimes present laterally.
- Dermoid/Epidermoid Cysts: Benign cysts that can occur in various locations.
- Lipomas: Benign fatty tumors that can occur anywhere on the body, including the neck and jaw area.
- Vascular Malformations: Abnormal blood vessel growths.
5. Trauma
- Direct Injury: A blow to the jaw, neck, or ear area can cause localized swelling due to tissue damage and inflammation.
- Fractures: A mandibular fracture, while usually causing more distinct pain and deformity, can also be accompanied by swelling.
6. TMJ Disorders
While not typically causing prominent external swelling, severe temporomandibular joint (TMJ) dysfunction or inflammation (arthrititis) can sometimes lead to mild swelling directly over the joint area, which is just anterior to the ear.
Signs and Symptoms
The accompanying signs and symptoms can provide critical clues about the underlying cause of swelling under ear behind jaw.
- Pain:
- Sharp, throbbing pain: Often indicative of a bacterial infection like a dental abscess or acute sialadenitis.
- Tenderness to touch: Common with lymphadenitis or inflammatory conditions.
- Pain radiating to the ear, head, or neck: Can be associated with dental infections, TMJ issues, or nerve involvement.
- Fever and Chills: Strong indicators of systemic infection (bacterial sialadenitis, severe dental abscess, mumps, severe lymphadenitis).
- Difficulty Swallowing (Dysphagia) or Speaking: Can occur if the swelling is significant and compresses the throat or obstructs movement.
- Difficulty Opening Mouth (Trismus): A hallmark symptom of pericoronitis (wisdom tooth infection), severe dental abscesses, or parotid gland inflammation, as it affects the muscles of mastication.
- Redness and Warmth of the Skin: Localized inflammation and infection will often cause the overlying skin to appear red and feel warm to the touch.
- Pus Drainage: A serious sign of an abscess that has ruptured or is attempting to drain. May be visible in the mouth (from a tooth) or externally.
- Bad Taste in Mouth/Halitosis: Can accompany dental infections or draining abscesses.
- Dry Mouth (Xerostomia): Can be a contributing factor to sialadenitis, or a symptom of autoimmune conditions.
- Fatigue and Malaise: General symptoms of a systemic illness or significant infection.
- Fluctuating Swelling: Swelling that worsens during or after meals is highly suggestive of salivary gland obstruction (sialolithiasis).
- Hard, Fixed Lump: A concern for potential tumor or malignancy, especially if painless and growing steadily.
- Itching: Less common but can be seen with certain skin conditions or allergic reactions.
Pro Tip: Pay close attention to when the swelling started, if it changes with eating, and any other symptoms you're experiencing. This information is vital for your dentist or doctor to make an accurate diagnosis.
Treatment Options
The treatment for swelling under ear behind jaw is entirely dependent on the underlying cause. A thorough diagnostic process is essential before initiating any therapy.
1. For Infections (Bacterial Sialadenitis, Dental Abscess, Bacterial Lymphadenitis)
- Antibiotics: Broad-spectrum antibiotics are typically prescribed to combat bacterial infections. The choice of antibiotic depends on the suspected bacteria and the severity of the infection. Common choices include Amoxicillin, Clindamycin, or Metronidazole.
- Pros: Effectively resolves bacterial infections, often reduces pain and swelling within 24-48 hours.
- Cons: Can have side effects (nausea, diarrhea, allergic reactions), overuse can lead to antibiotic resistance, does not address underlying causes like salivary stones or decayed teeth.
- Pain Management: Over-the-counter pain relievers such as ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are used to manage pain and reduce fever. Prescription pain medication may be needed for severe pain.
- Hydration: Especially important for salivary gland infections. Drinking plenty of water helps stimulate saliva flow and can aid in flushing out bacteria and small stones.
- Warm Compresses: Applying warm, moist compresses to the swollen area can help alleviate pain and encourage drainage, particularly for salivary gland issues and superficial infections.
- Massage: Gently massaging the affected salivary gland can help stimulate saliva flow and potentially dislodge small salivary stones.
- Sialogogues: Sour candies or lemon drops can stimulate saliva flow, which is beneficial for salivary gland issues.
2. For Viral Infections (Mumps, Mononucleosis)
- Supportive Care: Since antibiotics are ineffective against viruses, treatment focuses on managing symptoms. This includes rest, hydration, and pain/fever reducers (acetaminophen, ibuprofen).
- Isolation: To prevent the spread of contagious viral infections like mumps.
3. For Dental Issues (Pericoronitis, Dental Abscess)
- Antibiotics: Often prescribed to control the acute infection.
- Drainage: For a dental abscess, the dentist may drain the pus by incising the swollen gum tissue or through the tooth itself (during a root canal).
- Root Canal Treatment: If the tooth is savable and the infection has reached the pulp.
- Tooth Extraction: For severely decayed, fractured, or problematic teeth (e.g., impacted wisdom teeth causing recurrent pericoronitis), extraction is often the definitive solution.
- Oral Hygiene: Thorough cleaning of the affected area, especially around erupting wisdom teeth, is crucial.
- Pros: Directly addresses the source of infection, prevents recurrence, saves teeth where possible.
- Cons: Can be invasive (extraction, root canal), recovery time, potential for post-operative pain and swelling.
4. For Salivary Stones (Sialolithiasis)
- Conservative Management: Hydration, massage, sialogogues, and warm compresses may help small stones pass on their own.
- Sialendoscopy: A minimally invasive procedure where a tiny endoscope is inserted into the salivary duct to visualize, grasp, and remove stones.
- Pros: Minimally invasive, preserves the gland, faster recovery than open surgery.
- Cons: Not suitable for all stones (e.g., very large or embedded ones), specialized equipment and training required.
- Sialadenectomy (Gland Excision): Surgical removal of the entire affected salivary gland (e.g., submandibular gland excision) for large, recurrent, or deeply embedded stones that cannot be removed by sialendoscopy.
- Pros: Definitive solution, eliminates recurrence from that gland.
- Cons: Invasive surgery, risks include nerve damage (facial nerve for parotid, lingual/hypoglossal for submandibular), scar formation, longer recovery.
5. For Cysts and Tumors
- Biopsy: To determine if the growth is benign or malignant. This can be an incisional biopsy (partially removed) or excisional biopsy (entirely removed).
- Surgical Excision: Most cysts and benign tumors are treated by surgical removal.
- Oncological Treatment: For malignant tumors, treatment may involve surgery (radical excision), radiation therapy, chemotherapy, or a combination of these. This is typically managed by an oncologist in coordination with an oral and maxillofacial surgeon or head and neck surgeon.
6. For Trauma
- Rest and Ice: Initial management for minor trauma.
- Imaging: X-rays or CT scans to rule out fractures.
- Surgical Repair: For severe injuries or fractures.
Comparison of Common Treatments
| Treatment Type | Primary Use Case | Pros | Cons | Typical Duration (Acute Phase) |
|---|---|---|---|---|
| Antibiotics | Bacterial infections (dental, salivary, lymph) | Rapid symptom improvement, non-invasive | Side effects, resistance, doesn't address underlying cause | 7-14 days |
| Tooth Extraction | Severely infected/damaged teeth, pericoronitis | Definitive solution, prevents spread of infection | Invasive, post-op pain/swelling, loss of tooth | 1-2 weeks (healing) |
| Sialendoscopy | Salivary stones (sialolithiasis) | Minimally invasive, gland preservation, fast recovery | Not for all stones, specialized procedure | Days to 1 week |
| Sialadenectomy | Recurrent sialadenitis, large stones, tumors | Definitive for gland issues, tumor removal | Invasive surgery, nerve damage risk, longer recovery | Weeks to months (full recovery) |
| Supportive Care | Viral infections (mumps, mono), minor inflammation | Non-invasive, body heals naturally | Only manages symptoms, requires patience | 1-3 weeks |
| Surgical Excision (Cyst/Tumor) | Cysts, benign/malignant tumors | Definitive removal of growth | Invasive, potential for nerve damage, scarring, complex recovery | Weeks to months |
Step-by-Step Process
The typical process for diagnosing and treating swelling under ear behind jaw involves several stages:
1. Initial Consultation and Examination
- Medical History: Your dentist or doctor will ask about your symptoms (onset, duration, severity, associated symptoms like pain, fever, difficulty eating), past medical conditions, medications, and any recent illnesses or dental work.
- Physical Examination: The clinician will visually inspect the swollen area, palpate (feel) it to assess its size, consistency (soft, firm, fluctuant), tenderness, warmth, and mobility. They will also examine your mouth, throat, and neck for other signs of infection or inflammation. For dental concerns, specific teeth will be examined for decay, cracks, or gum issues.
- Evaluation of Trismus: Assessment of how wide you can open your mouth.
2. Diagnostic Imaging
- Dental X-rays: Periapical, panoramic (Panorex), or bitewing X-rays are crucial for identifying dental infections (abscesses, bone loss) or impacted wisdom teeth.
- Ultrasound: Often the first-line imaging for salivary gland issues, as it can visualize stones, inflammation, and masses, and it's radiation-free.
- CT Scan (Computed Tomography): Provides detailed cross-sectional images of bone and soft tissues, excellent for identifying infections, abscesses, salivary stones, cysts, and tumors, as well as evaluating the extent of infection spread.
- MRI (Magnetic Resonance Imaging): Superior for soft tissue differentiation, particularly useful for characterizing tumors and assessing nerve involvement.
- Sialography: An older technique where contrast dye is injected into the salivary duct to visualize the ductal system for stones or strictures, largely replaced by sialendoscopy and MRI sialography.

3. Laboratory Tests
- Blood Tests: A complete blood count (CBC) can reveal elevated white blood cell counts, indicating infection or inflammation. CRP (C-reactive protein) also indicates inflammation. Specific viral tests may be ordered if mumps or mononucleosis is suspected.
- Cultures: If pus is present, a sample may be sent for bacterial culture to identify the specific pathogen and determine antibiotic sensitivity.
4. Biopsy (If Tumor Suspected)
- Fine Needle Aspiration (FNA) Biopsy: A thin needle is used to extract cells from a suspicious lump for microscopic examination to determine if it's benign or malignant.
5. Treatment Implementation
- Once a diagnosis is made, the appropriate treatment plan is initiated, ranging from antibiotics and supportive care to dental procedures or surgery. This step involves detailed discussions with your healthcare provider about the chosen treatment, its risks, benefits, and expected outcomes.
6. Follow-up Care
- Regular follow-up appointments are crucial to monitor healing, ensure the infection has resolved, or to continue managing chronic conditions. For surgical cases, follow-up ensures proper recovery and addresses any complications.
Cost and Insurance
The cost of treating swelling under ear behind jaw varies widely depending on the underlying cause, the complexity of the treatment, the specialist involved (general dentist, oral surgeon, ENT, infectious disease specialist), and geographic location within the US.
General Cost Ranges (without insurance):
- Initial Consultation & Exam: $75 - $250 (general dentist or primary care physician).
- X-rays (Dental):
- Periapical/Bitewing: $30 - $70 per image
- Panoramic (Panorex): $100 - $200
- Imaging (Medical):
- Ultrasound: $200 - $600
- CT Scan: $500 - $3,000+ (depending on facility and contrast use)
- MRI: $1,000 - $5,000+
- Laboratory Tests (Blood work, cultures): $100 - $500
- Antibiotics: $10 - $100+ (generic vs. brand-name, duration)
- Dental Procedures:
- Dental Abscess Drainage: $150 - $400 (often part of a larger procedure)
- Tooth Extraction (simple): $150 - $450
- Tooth Extraction (surgical, impacted wisdom tooth): $300 - $800 per tooth
- Root Canal Treatment: $800 - $2,000+ (molars typically more expensive)
- Salivary Gland Procedures:
- Sialendoscopy: $1,500 - $5,000+ (can be much higher with facility fees)
- Sialadenectomy (submandibular gland removal): $5,000 - $15,000+ (surgeon's fee + anesthesia + facility fee)
- Biopsy (FNA): $300 - $1,000+ (often includes pathology fees)
- Cyst/Tumor Removal: $2,000 - $20,000+ (highly variable based on size, location, and malignancy)
Insurance Coverage Details:
- Dental Insurance: Typically covers a portion of dental procedures (exams, X-rays, fillings, extractions, root canals). Coverage for major procedures like surgical extractions or root canals can be 50-80% after deductible.
- Medical Insurance: Usually covers consultations with physicians, medical imaging, lab tests, prescriptions, and surgical procedures performed by medical doctors (ENTs, general surgeons, oncologists).
- Co-pays and Deductibles: You will likely be responsible for co-pays for office visits and a deductible before your insurance coverage kicks in for more extensive procedures.
- In-network vs. Out-of-network: Costs will be significantly higher if you go to out-of-network providers.
- Pre-authorization: Many surgical procedures or advanced imaging (CT, MRI) require pre-authorization from your insurance company.
- Overlap: Some procedures, like emergency tooth extractions that lead to cellulitis requiring hospitalization, might involve both dental and medical insurance. Clarify with your providers and insurance company.
Cost-Saving Tips:
- Inquire about Payment Plans: Many dental and medical offices offer installment plans.
- Negotiate Cash Prices: If you are uninsured, ask if there's a discount for paying in cash upfront.
- Community Health Centers: Can offer reduced-cost services for low-income or uninsured individuals.
- Dental Schools: Often provide high-quality care at a lower cost, supervised by experienced faculty.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): Utilize these pre-tax dollars for medical and dental expenses.
- Understand Your Policy: Familiarize yourself with your dental and medical insurance benefits, deductibles, co-pays, and out-of-pocket maximums.
Comparison Table: Treatment Costs (Estimated US without Insurance)
| Treatment Category | Low End (USD) | Mid Range (USD) | High End (USD) | Typical Scenario |
|---|---|---|---|---|
| Initial Visit & Diagnosis | $150 | $400 | $1,000 | Basic exam + dental X-rays; includes lab work or simple ultrasound if needed. |
| Antibiotics Only | $10 | $50 | $100 | Generic prescription for a week-long course. |
| Tooth Extraction (Simple) | $150 | $250 | $450 | Non-surgical removal of an accessible tooth causing infection. |
| Surgical Wisdom Tooth Ext. | $300 | $550 | $800 (per tooth) | Removal of an impacted wisdom tooth. |
| Root Canal Treatment | $800 | $1,200 | $2,000 | Treatment for an infected molar. |
| Sialendoscopy | $1,500 | $3,000 | $5,000 | Minimally invasive stone removal (excluding facility fees for full procedure). |
| Submandibular Gland Excision | $5,000 | $10,000 | $15,000+ | Complex surgical removal, includes surgeon, anesthesia, facility. |
| Cyst/Tumor Biopsy & Removal | $1,000 | $5,000 | $20,000+ | Small, benign cyst removal to complex malignant tumor surgery. |
Note: These are estimates and actual costs may vary based on your location, specific provider, and the complexity of your case.
Recovery and Aftercare
Recovery from swelling under ear behind jaw depends significantly on the cause and the treatment received. Following post-treatment instructions meticulously is crucial for proper healing and preventing complications.
General Aftercare for Infections (Antibiotics, Drainage):
- Complete Antibiotic Course: Always finish the entire course of antibiotics, even if symptoms improve, to prevent recurrence and antibiotic resistance.
- Pain Management: Continue taking prescribed or over-the-counter pain relievers as directed.
- Warm Compresses: Continue applying warm, moist compresses to the affected area to reduce swelling and discomfort.
- Hydration: Drink plenty of fluids, especially if dealing with salivary gland issues.
- Soft Diet: For jaw or mouth discomfort, stick to soft, easy-to-chew foods.
- Good Oral Hygiene: Maintain meticulous oral hygiene, but be gentle around any surgical sites or tender areas.
Specific Aftercare for Dental Procedures (Extraction, Root Canal):
- Extraction Site Care:
- Bite on gauze for 30-60 minutes to stop bleeding.
- Avoid spitting, rinsing vigorously, or using straws for 24-48 hours to prevent dislodging the blood clot (dry socket).
- Eat soft foods, chew on the opposite side.
- Rinse gently with warm salt water after 24 hours.
- Root Canal Care:
- Avoid chewing on the treated tooth until the permanent crown or filling is placed.
- Maintain regular brushing and flossing.
- Report any persistent pain or swelling to your dentist.
Specific Aftercare for Salivary Gland Procedures (Sialendoscopy, Sialadenectomy):
- Sialendoscopy: Minimal downtime. You may experience some swelling or discomfort for a day or two. Continue hydration and possibly gentle massage.
- Sialadenectomy (Gland Removal Surgery):
- Pain and Swelling: Expect pain and significant swelling for several days. Pain medication will be prescribed.
- Incision Care: Keep the surgical incision clean and dry. Follow instructions for dressing changes. Report any signs of infection (increased redness, pus, fever).
- Diet: Soft diet initially, progressing as tolerated.
- Activity Restriction: Avoid strenuous activity, heavy lifting, and bending for 1-2 weeks.
- Nerve Monitoring: Pay attention to any facial weakness or numbness, and report it to your surgeon immediately.
- Follow-up: Crucial for wound check, suture removal, and pathology results.
Recovery Timelines:
- Simple Infections (antibiotic treatment): Symptoms often improve within 2-3 days, full resolution in 1-2 weeks.
- Dental Extraction: Initial healing in 1-2 weeks, full bone healing takes months.
- Sialendoscopy: Recovery typically within a few days.
- Sialadenectomy: Initial recovery (managing pain/swelling) 1-2 weeks, full recovery for strenuous activities can take 4-6 weeks or longer. Nerve recovery can be prolonged.
Pro Tip: If you notice worsening pain, increased swelling, high fever, difficulty breathing, or difficulty swallowing after treatment, seek immediate medical attention. These could be signs of a spreading infection or complication.
Prevention
Preventing swelling under ear behind jaw primarily involves addressing the most common underlying causes.
1. Maintain Excellent Oral Hygiene:
- Brush Twice Daily: Use fluoride toothpaste and brush for at least two minutes, covering all tooth surfaces and the gum line.
- Floss Daily: Remove food particles and plaque from between teeth and under the gum line to prevent gum disease and cavities, which can lead to dental infections.
- Use Mouthwash: An antiseptic mouthwash can help reduce oral bacteria.
- Clean Around Wisdom Teeth: If you have partially erupted wisdom teeth, pay extra attention to keeping the gum flap clean to prevent pericoronitis. Consider early extraction if they are problematic.
2. Regular Dental Check-ups and Cleanings:
- Every 6 Months: Visit your dentist for routine check-ups and professional cleanings. This allows for early detection and treatment of cavities, gum disease, and other dental issues before they become severe and cause infections. The American Dental Association (ADA) strongly recommends these regular visits.
3. Stay Hydrated:
- Drink Plenty of Water: Adequate hydration (aim for 8 glasses of water daily) is essential for healthy salivary gland function. It helps keep saliva flowing, preventing stagnation that can lead to stone formation and infection.
4. Manage Salivary Gland Health:
- Stimulate Saliva Flow: If you are prone to dry mouth or salivary gland issues, use sugar-free gum, lozenges, or sialogogues (sour candies) to encourage saliva production.
- Avoid Dehydrating Agents: Limit caffeine and alcohol, which can contribute to dehydration.
- Quit Smoking: Smoking is a risk factor for various oral and systemic health issues, including potentially impacting salivary gland function.
5. Timely Treatment of Infections:
- Don't Delay Care: Address any signs of infection (sore throat, earache, tooth pain, swollen glands) promptly. Early intervention can prevent infections from spreading and becoming more serious.
6. Vaccinations:
- Mumps Vaccine (MMR): Ensure you and your children are up-to-date on the MMR vaccine to prevent mumps, a common cause of parotid gland swelling.
7. Protect Against Trauma:
- Wear Mouthguards: If participating in contact sports, wear a custom-fitted mouthguard to protect your teeth and jaw from injury.
Risks and Complications
While many causes of swelling under ear behind jaw are treatable, ignoring the symptom or delaying care can lead to significant risks and complications.
1. Spread of Infection:
- Cellulitis/Abscess Progression: A localized infection (dental abscess, sialadenitis) can spread rapidly to surrounding facial and neck tissues, leading to widespread cellulitis.
- Ludwig's Angina: A severe, potentially life-threatening form of cellulitis affecting the floor of the mouth and neck, often originating from dental infections. It can cause airway obstruction due to tongue elevation and significant neck swelling, requiring emergency surgery and intensive care.
- Systemic Sepsis: If the infection enters the bloodstream, it can lead to sepsis, a life-threatening response to infection that can cause organ damage and death.
- Cavernous Sinus Thrombosis: A rare but extremely dangerous complication of facial infections where a blood clot forms in a major vein at the base of the brain, leading to severe headache, vision changes, and neurological deficits.
2. Airway Obstruction:
- Severe swelling in the neck and submandibular region can compress the trachea (windpipe), making it difficult to breathe. This is a medical emergency.

3. Chronic Pain and Discomfort:
- Untreated or recurrent conditions (e.g., chronic sialadenitis, unresolved dental issues) can lead to persistent pain, discomfort, and impaired function (e.g., difficulty chewing, speaking).
4. Facial Nerve Damage:
- Surgical procedures, particularly those involving the parotid gland, carry a risk of temporary or permanent damage to the facial nerve, which controls facial expressions. This can result in facial weakness or paralysis.
- Surgery for submandibular gland issues can risk damage to the lingual nerve (taste, sensation to tongue) or hypoglossal nerve (tongue movement).
5. Salivary Gland Dysfunction:
- Chronic inflammation or repeated infections can permanently damage salivary glands, leading to reduced saliva production (dry mouth) or altered function.
6. Recurrence:
- Salivary stones or infections can recur if the underlying cause (e.g., anatomical predisposition, chronic dehydration) is not addressed or if treatment is incomplete.
7. Scarring and Deformity:
- Surgical interventions, especially for larger cysts or tumors, can result in visible scarring. Extensive infections that lead to tissue destruction can also cause scarring and cosmetic deformities.
8. Malignancy Progression:
- If the swelling is due to a malignant tumor, delayed diagnosis and treatment can allow the cancer to spread, making treatment more difficult and reducing prognosis.
Children / Pediatric Considerations
Swelling under the ear behind the jaw in children can be particularly concerning for parents. While many causes are similar to adults, some are more prevalent or have specific considerations in pediatric populations.
- Mumps: This highly contagious viral infection is a classic cause of parotid gland swelling in unvaccinated children. The widespread use of the MMR vaccine has drastically reduced its incidence, but outbreaks still occur in unvaccinated communities. Symptoms include fever, headache, muscle aches, fatigue, and loss of appetite, followed by painful swelling of the parotid glands, often bilateral.
- Lymphadenitis: Children frequently experience swollen lymph nodes due to common viral upper respiratory infections, strep throat, ear infections, or other childhood illnesses. These are typically tender, mobile, and resolve as the underlying infection clears.
- Dental Infections: While less common in very young children, dental abscesses can occur in primary (baby) teeth due to severe decay or trauma. Erupting permanent molars, including wisdom teeth in adolescents, can also cause localized inflammation and swelling.
- Sialadenitis (Bacterial): Can occur in children, often associated with dehydration or viral infections that predispose to bacterial superinfection.
- Cysts: Congenital cysts like branchial cleft cysts or thyroglossal duct cysts may present as a swelling in the neck or under the jaw in childhood, sometimes becoming infected.
- Kawasaki Disease: A rare inflammatory condition primarily affecting children, which can cause cervical lymph node swelling as one of its diagnostic criteria.
- Diagnosis Challenges: Young children may have difficulty articulating their symptoms, making diagnosis more challenging. Parents should look for behavioral changes, reduced feeding, irritability, and signs of pain.
- Treatment: Antibiotics are prescribed for bacterial infections. For dental issues, treatment might involve fillings, pulpotomies (partial root canal on baby teeth), or extractions. Surgical intervention for salivary stones or cysts is considered when necessary, with careful consideration for the child's growth and development.
- Parental Guidance:
- Monitor Symptoms: Keep a close eye on the swelling for changes in size, pain, redness, or if accompanied by high fever or breathing difficulties.
- Hydration: Ensure children drink plenty of fluids, especially during illness.
- Oral Hygiene: Emphasize good oral hygiene habits from an early age.
- Vaccinations: Ensure your child is up-to-date on all recommended vaccinations, including the MMR.
Cost Breakdown
As detailed in the "Cost and Insurance" section, the financial implications of swelling under ear behind jaw can be substantial, especially without adequate insurance coverage. Here's a summary of the average US costs (low, mid, high) with specific attention to insurance and payment plans.
Average US Costs (Without Insurance)
The range of costs is vast because of the diverse etiologies and treatments involved.
- Conservative Treatment (e.g., antibiotics, pain relievers, minor dental procedure):
- Low: $150 - $300 (initial exam, simple X-ray, generic antibiotic)
- Mid: $300 - $800 (more extensive diagnostics, brand-name antibiotic, simple tooth extraction)
- High: $800 - $2,500 (initial specialist consults, advanced imaging like ultrasound/CT, surgical wisdom tooth extraction)
- Invasive/Surgical Treatment (e.g., sialendoscopy, gland excision, tumor removal):
- Low: $1,500 - $5,000 (less complex sialendoscopy, simple cyst removal)
- Mid: $5,000 - $10,000 (more complex sialendoscopy, submandibular gland excision)
- High: $10,000 - $20,000+ (parotidectomy, complex tumor resection, prolonged hospitalization)
These figures typically include professional fees (dentist, surgeon, radiologist), facility fees (for hospitals or surgical centers), anesthesia fees, and pathology fees for biopsies.
With vs. Without Insurance
- Without Insurance: You are responsible for 100% of the cost. This can quickly become a significant financial burden, especially for emergency care or complex surgeries.
- With Insurance (Dental & Medical):
- Co-pays: Typically $10 - $75 per office visit or specialist visit.
- Deductibles: You must pay a certain amount out-of-pocket (e.g., $500 - $5,000+ annually) before your insurance begins to pay for covered services.
- Coinsurance: After your deductible is met, your insurance will pay a percentage (e.g., 70-90%), and you'll be responsible for the remaining percentage (e.g., 10-30%).
- Out-of-Pocket Maximum: Most policies have an annual limit on how much you'll pay out of pocket, protecting you from catastrophic costs.
- Coverage Limitations: Dental insurance often has annual maximums (e.g., $1,000 - $2,000) which can be quickly exhausted by major procedures like multiple extractions or a root canal. Medical insurance usually has higher maximums but stricter rules for what dental-related issues they cover.
Payment Plans and Financing Options
For those facing high costs, several options can help:
- In-Office Payment Plans: Many dental and medical offices offer interest-free installment plans directly.
- Medical Credit Cards (e.g., CareCredit): These specialized credit cards offer deferred interest plans for healthcare expenses. Ensure you understand the terms to avoid high-interest charges if the balance isn't paid within the promotional period.
- Personal Loans: Banks or credit unions offer personal loans that can cover medical expenses, but they come with interest.
- Hospital Financial Assistance Programs: Many hospitals have programs for uninsured or underinsured patients to reduce costs based on income.
- Negotiation: Especially if paying cash, you can sometimes negotiate a lower price with providers.
Pro Tip: Always get a detailed estimate of costs before any major procedure. Discuss all financial options with your provider's billing department.
Frequently Asked Questions
What does it mean when your lymph nodes swell behind your jaw?
Swollen lymph nodes behind your jaw typically indicate that your body is fighting an infection or inflammation in the head or neck region. This could be due to a common cold, strep throat, an ear infection, a dental abscess, or in some cases, a more serious condition like mononucleosis or, rarely, cancer. They often feel tender and mobile.
Is swelling under the ear behind the jaw always serious?
No, it's not always serious, but it should always be evaluated by a healthcare professional. While minor infections or temporary inflammation can cause it, the swelling can also signal serious issues like a spreading dental abscess (cellulitis), a large salivary stone requiring removal, or even a tumor. Prompt diagnosis is key to appropriate treatment.
How quickly can a swollen gland behind the jaw go down?
The timeline for swelling reduction varies based on the cause. If it's a minor viral infection, swelling might decrease within a few days to a week with rest and supportive care. Bacterial infections treated with antibiotics usually show improvement within 24-48 hours, with full resolution in 7-14 days. If the cause is a salivary stone or dental infection, it might not go down until the obstruction is removed or the infection source is treated.
Can a tooth infection cause swelling behind the ear?
Yes, a severe tooth infection, particularly from a lower molar or wisdom tooth, can definitely cause swelling that extends to the submandibular area and even behind the ear. This happens when the infection spreads from the tooth into the surrounding soft tissues of the jaw and neck, potentially leading to a dental abscess or cellulitis.
What is the typical submandibular gland swelling treatment?
Treatment for submandibular gland swelling usually depends on the cause. If it's an infection (sialadenitis), antibiotics, warm compresses, massage, and increased hydration are common. If a salivary stone (sialolithiasis) is the culprit, conservative measures like increased fluid intake and sialogogues may help small stones pass. Larger or recurrent stones may require minimally invasive sialendoscopy or, in some cases, surgical removal of the gland (sialadenectomy).
When should I be worried about swelling under my jaw?
You should be worried and seek immediate medical attention if the swelling: rapidly worsens, is accompanied by high fever or chills, causes difficulty breathing or swallowing, is extremely painful, is hard and fixed (not movable), or has been present for more than two weeks without improvement. These symptoms can indicate a severe infection or a more serious underlying condition.
Is surgery always required for a swollen gland under the ear?
No, surgery is not always required. Many cases of swollen glands, especially those due to viral infections or minor bacterial infections, resolve with antibiotics and supportive care. Surgery is typically reserved for cases where there's a persistent problem like a large, recurrent salivary stone, a chronic salivary gland infection unresponsive to other treatments, or if a cyst or tumor is identified.
What are the alternatives to antibiotics for this type of swelling?
Alternatives to antibiotics primarily involve supportive care for viral causes (rest, hydration, pain relievers) or direct treatment of the underlying mechanical issue. For salivary stones, alternatives include hydration, massage, sialogogues, or sialendoscopy. For dental issues, root canal therapy or extraction address the source of infection without relying solely on antibiotics, which only treat the acute bacterial spread.
How much does it cost to treat a swollen gland under the ear?
The cost varies dramatically. An initial consultation, some dental X-rays, and antibiotics might be $150-$500. If it requires a surgical procedure like a wisdom tooth extraction, it could be $300-$800 per tooth. More complex procedures like sialendoscopy can range from $1,500-$5,000, and surgical removal of a salivary gland can be $5,000-$15,000+, depending on the facility, surgeon, and anesthesia.
Can TMJ disorder cause swelling under the ear behind the jaw?
While TMJ disorders primarily cause pain and dysfunction in the jaw joint and surrounding muscles, severe inflammation of the joint (arthritis) can sometimes lead to mild, localized swelling directly over the joint area, which is just in front of or below the ear. However, prominent or diffuse swelling further down behind the jaw is less typical for primary TMJ issues and usually points to other causes.
When to See a Dentist
Given the diverse and potentially serious causes of swelling under ear behind jaw, knowing when to seek professional help is paramount.
Immediate Emergency Attention (Call 911 or go to the nearest emergency room):
- Difficulty Breathing: Any shortness of breath, gasping, or noisy breathing.
- Difficulty Swallowing: Severe inability to swallow saliva, food, or liquids.
- Rapidly Spreading Swelling: If the swelling is increasing very quickly, especially if it's extending into your neck or chest.
- High Fever with Chills: Especially if accompanied by severe pain and general malaise.
- Severe Pain that is Unmanageable: Excruciating pain that does not respond to over-the-counter pain medication.
- Any Signs of Facial Weakness or Numbness: These can indicate nerve involvement or a spreading severe infection.
Urgent Dental or Medical Appointment (Within 24-48 hours):
- Persistent Swelling: If the swelling doesn't improve or worsens over 1-2 days.
- Increasing Pain: Pain that is getting worse, even if it's not yet severe.
- Difficulty Opening Your Mouth (Trismus): This is a red flag for spreading dental infections or severe salivary gland inflammation.
- Fluctuating Swelling with Eating: If the swelling appears or worsens during or after meals, suggesting a salivary gland issue.
- Pus Drainage: Any visible pus from the swollen area or in your mouth.
- Swelling with Obvious Dental Pain: If you also have a painful tooth or a noticeable cavity.
Routine Dental or Medical Appointment (If symptoms are mild and non-progressive):
- Mild, Non-Tender Swelling: If the swelling is small, not painful, and you have no other alarming symptoms, you can likely schedule a routine appointment with your dentist or general practitioner.
- Known Viral Illness: If you're recovering from a cold or flu and notice some mild, tender lymph node swelling that is gradually resolving.
In any case of unexplained swelling in this area, it's always best to err on the side of caution and consult with a healthcare professional. Early diagnosis and intervention can prevent minor issues from becoming major health crises.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026