Tmj Face Swelling: Complete Guide
Key Takeaways
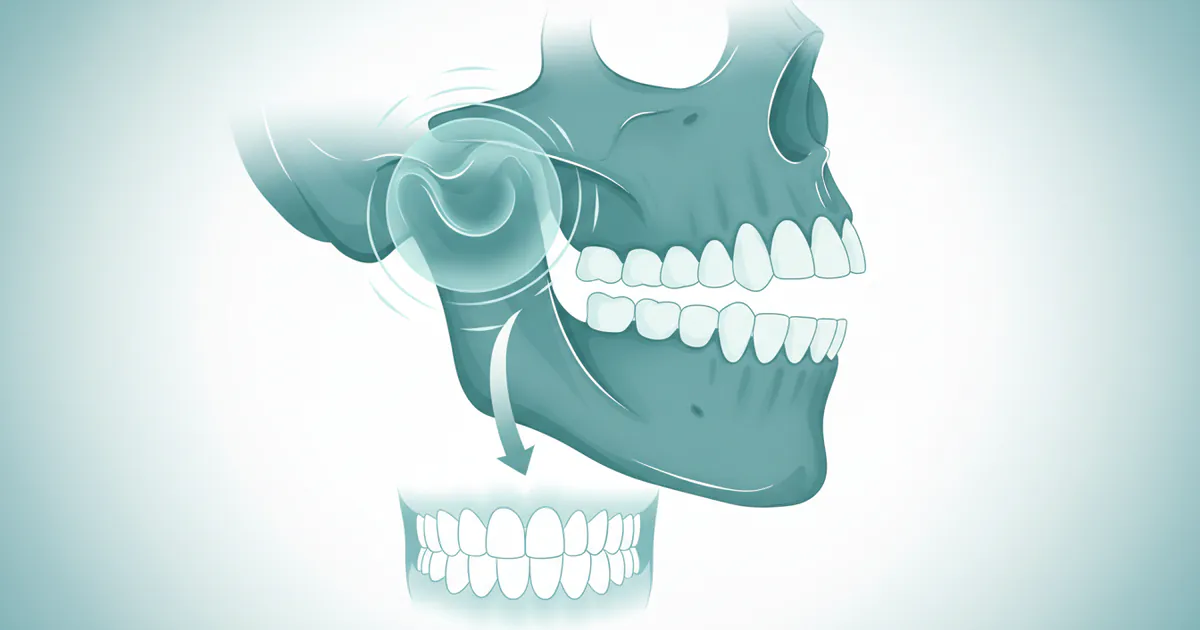
- Have you ever woken up with a swollen face, particularly around your jaw, making it difficult to open your mouth, chew, or even speak comfortably? This disconcerting experience often points to an issue with your temporomandibular joint (TMJ) – the complex hinge connecting your jawbone to your skull.
Tmj Face Swelling: Complete Guide
Have you ever woken up with a swollen face, particularly around your jaw, making it difficult to open your mouth, chew, or even speak comfortably? This disconcerting experience often points to an issue with your temporomandibular joint (TMJ) – the complex hinge connecting your jawbone to your skull. TMJ face swelling is a common and often painful symptom of temporomandibular joint disorders (TMDs), a group of conditions affecting millions of Americans each year. In fact, estimates suggest that over 10 million people in the United States experience TMDs at any given time, with women being disproportionately affected.

While facial swelling near the jaw can be alarming, it's crucial to understand its origins and potential severity. It can range from a minor inflammatory response due to overuse or stress to a sign of more serious underlying conditions, including infections or joint damage. Ignoring such a symptom can lead to chronic pain, permanent joint damage, and significantly diminished quality of life. This comprehensive guide will equip you with the knowledge to understand what causes TMJ face swelling, how to recognize its signs, the various treatment options available, and crucial information on costs, recovery, and prevention. We'll also explore other common causes of facial swelling, such as dry socket molar complications and gums swelling over teeth, to help you differentiate and seek appropriate care when your jaw or face swells.
Key Takeaways:
- TMJ face swelling is a common symptom of temporomandibular joint (TMJ) disorders, often indicating inflammation, muscle strain, or joint dysfunction.
- Early diagnosis and intervention are crucial to prevent chronic pain and long-term joint damage; consult a dentist or oral surgeon if swelling persists.
- Common causes include teeth grinding (bruxism), stress, trauma, arthritis, and dental issues like dry socket or gum infections.
- Treatment options range from conservative self-care (rest, warm/cold packs, soft diet) and medications to oral appliances (splints), physical therapy, and in severe cases, injections or surgery.
- Costs vary widely: self-care is minimal, oral appliances typically range from $300 to $2,500, Botox injections $500 to $1,500 per session, and surgeries can exceed $50,000.
- Many TMJ treatments are covered by medical insurance, though prior authorization and specific codes are often required. Dental insurance may cover some aspects if linked to dental procedures.
- Prevention focuses on stress management, avoiding jaw clenching, maintaining good posture, and regular dental check-ups.
What It Is / Overview
The temporomandibular joints (TMJs) are two of the most complex joints in the body, located on each side of your head, just in front of your ears. These joints, along with several muscles, ligaments, and a small, soft disc, work together to allow you to move your jaw up and down, side to side, and forward and back. This intricate system is essential for speaking, chewing, and swallowing.
TMJ face swelling occurs when there is inflammation, fluid retention, or muscle hypertrophy (enlargement) in the region around these joints. This can be directly within the joint capsule, in the surrounding masticatory muscles (muscles used for chewing), or even in the parotid gland which is located nearby. When the delicate balance of the TMJ system is disrupted, it can lead to a range of symptoms collectively known as temporomandibular joint disorders (TMDs). Swelling is a telltale sign that something is amiss, often indicating an inflammatory response, trauma, or an underlying infection. It can be a localized puffiness or a more diffuse enlargement, sometimes making one side of the face appear noticeably larger than the other.
Types / Variations of TMJ Disorders Leading to Swelling
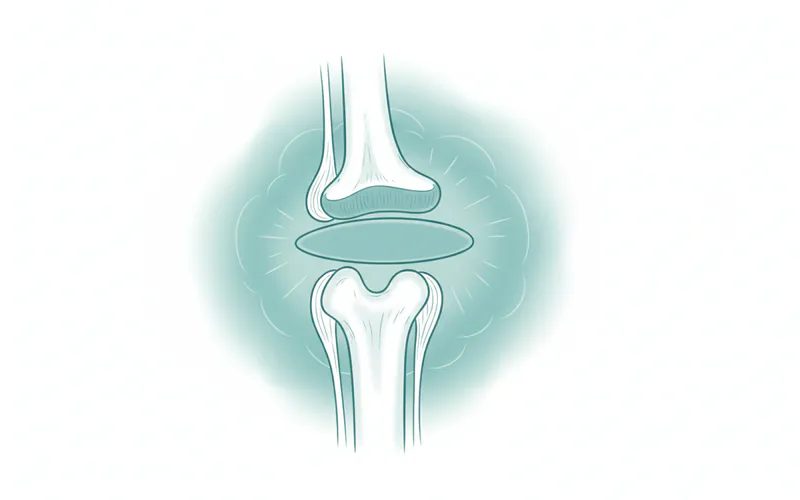
TMJ disorders are broadly classified into three main categories, each with varying presentations that can lead to facial swelling:
- Myofascial Pain: This is the most common type of TMD and involves pain in the muscles that control jaw function, as well as in the muscles of the neck and shoulders. Swelling in these cases is typically due to muscle inflammation, overuse, or spasm. It might present as a generalized puffiness over the cheek or jaw angle, often accompanied by tenderness when touching the affected muscles.
- Internal Derangement of the Joint: This refers to a displaced disc within the joint. Normally, a small, soft disc acts as a cushion between the ball and socket of the TMJ. If this disc slips out of alignment (either partially or completely), it can cause clicking, popping, limited jaw movement, and pain. Persistent displacement or injury to the disc can lead to inflammation within the joint capsule itself, resulting in direct swelling around the joint area, often just in front of the ear.
- Degenerative Joint Disease (Arthritis): Like other joints in the body, the TMJ can be affected by arthritis. This includes osteoarthritis (wear-and-tear arthritis) or inflammatory arthritis (such as rheumatoid arthritis). Degeneration of the joint tissues can lead to chronic inflammation, pain, stiffness, and noticeable swelling around the joint area. This type of swelling is often chronic and may worsen during flare-ups.
In some cases, swelling can be a symptom of a more acute issue, such as a trauma or an infection spreading from adjacent structures.
Causes / Why It Happens
Understanding the root causes of TMJ face swelling is crucial for effective treatment. Multiple factors can contribute to TMDs and the associated swelling:
- Bruxism (Teeth Grinding and Clenching): One of the most common culprits. Chronic clenching or grinding of teeth, especially during sleep (sleep bruxism), puts immense stress on the TMJ and surrounding muscles. This constant strain can lead to muscle fatigue, inflammation, and hypertrophy, causing noticeable swelling. This often manifests as muscle soreness and a tired jaw.
- Stress and Anxiety: Psychological stress often manifests physically. Many people unconsciously clench their jaw or grind their teeth when stressed, directly contributing to muscle tension and inflammation around the TMJ. Stress can also increase overall muscle tension throughout the body, including the jaw, leading to soreness and swelling.
- Trauma to the Jaw, Head, or Neck: A direct blow to the jaw, a whiplash injury, or even a fall that impacts the head can damage the TMJ or its surrounding structures. This can result in acute inflammation, disc displacement, or fracture, all of which can cause immediate and significant swelling. Even seemingly minor injuries can have delayed effects.
- Arthritis: As mentioned, various forms of arthritis can affect the TMJ. Osteoarthritis, resulting from the wear and tear of cartilage, and rheumatoid arthritis, an autoimmune inflammatory disease, can both lead to joint destruction, inflammation, and chronic swelling.
- Malocclusion (Bad Bite): If your teeth don't align properly when you bite down, it can create an imbalance in the forces applied to your TMJs. This uneven stress can lead to muscle strain, joint dysfunction, and chronic inflammation, eventually causing swelling.
- Dental Procedures and Complications: While less common, certain dental procedures or their complications can indirectly contribute to or mimic TMJ-related swelling.
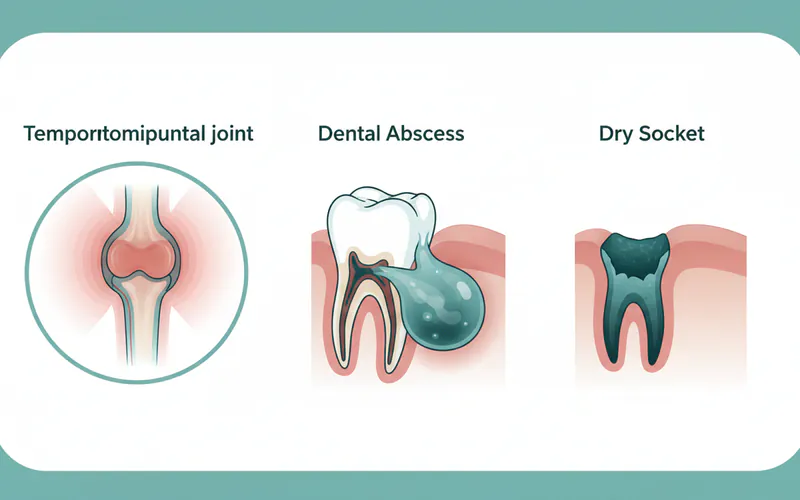
- Dry Socket Molar (Alveolar Osteitis): After a tooth extraction, especially of a molar, the blood clot in the socket can dislodge or dissolve, exposing the bone. This "dry socket" is intensely painful and can lead to localized inflammation. While primarily affecting the extraction site, the severe pain can sometimes radiate, and the adjacent soft tissue can swell, giving the appearance of facial swelling that might be confused with or contribute to TMJ region discomfort. The swelling from a dry socket is usually very localized to the area of the missing tooth, but can sometimes spread.
- Gums Swelling Over Teeth (Pericoronitis or Abscess): An infection of the gums, particularly around partially erupted wisdom teeth (pericoronitis) or a dental abscess (a pocket of pus caused by bacterial infection), can cause significant swelling in the jaw and cheek area. This swelling can often extend up towards the TMJ, creating confusion. A dental abscess often presents with severe pain, sensitivity to hot/cold, and sometimes a fever, distinguishing it from typical TMJ inflammation.
- Connective Tissue Diseases: Conditions like lupus or scleroderma can affect connective tissues throughout the body, including those in the TMJ, leading to inflammation and swelling.
- Infections: Although rare, a bacterial or viral infection directly within the TMJ or in nearby structures (like the parotid gland) can cause acute, painful swelling, often accompanied by fever and malaise.
- Tumors: Extremely rare, but benign or malignant growths in or near the TMJ can cause persistent swelling, pain, and dysfunction. These are typically ruled out with imaging studies.
Signs and Symptoms
Identifying the specific symptoms that accompany TMJ face swelling is key to a correct diagnosis. While swelling itself is noticeable, it's usually part of a broader constellation of symptoms:
- Visible Facial Swelling: Often unilateral (on one side), localized around the jaw joint (just in front of the ear) or extending down the cheek and jawline. It can range from subtle puffiness to a more pronounced enlargement.
- Pain or Tenderness:
- In the jaw joint itself.
- In the chewing muscles (masseter, temporalis).
- Radiating pain to the ear, temple, neck, or shoulders.
- Pain that worsens with jaw movement, chewing, or speaking.
- Limited Jaw Movement: Difficulty opening your mouth fully, making it hard to eat or yawn. The jaw might feel "stiff" or "stuck."
- Locking of the Jaw: The jaw may temporarily lock in an open or closed position, which can be very distressing.
- Clicking, Popping, or Grating Sounds: These sounds occur when you open or close your mouth, indicating a problem with the articular disc within the joint. While not always painful, if accompanied by pain or limited movement, it's a concern.
- Headaches: Often tension-type headaches, located in the temples or behind the eyes, or even migraines.
- Ear-related Symptoms: Earaches, feeling of fullness in the ear, ringing in the ears (tinnitus), or even hearing loss. These are often referred pain from the jaw muscles.
- Changes in Bite: You might feel like your upper and lower teeth don't fit together properly.
- Dizziness or Vertigo: Less common, but some patients report episodes of dizziness.
Distinguishing from other causes of facial swelling: If your swelling is due to a dry socket molar, you'd typically experience:
- Excruciating, throbbing pain days after a tooth extraction.
- A visible empty socket with exposed bone, sometimes with a foul odor.
- Pain radiating to the ear, eye, temple, or neck on the affected side.
- Sometimes a low-grade fever or general malaise. The swelling would be most pronounced directly around the extraction site.
If the issue is gums swelling over teeth (e.g., pericoronitis or a dental abscess), you might see:
- Red, swollen, tender gums, often around a partially erupted wisdom tooth.
- Pus discharge, foul taste in the mouth.
- Severe toothache that worsens with pressure.
- Difficulty swallowing or opening your mouth fully.
- Fever, swollen lymph nodes in the neck. The swelling is typically more localized to the gum/tooth area but can spread significantly.
Treatment Options
Treatment for TMJ face swelling aims to reduce pain, restore normal jaw function, and decrease inflammation. The approach varies greatly depending on the underlying cause and severity, ranging from conservative, non-invasive methods to surgical interventions.
Conservative Treatments (First Line of Defense)
Most TMJ disorders, including those causing swelling, respond well to conservative therapies.
-
Self-Care and Lifestyle Modifications:
- Pros: Inexpensive, non-invasive, empowers the patient.
- Cons: Requires consistency, may not be sufficient for severe cases.
- Description:
- Soft Diet: Avoid hard, chewy, or sticky foods. Cut food into small pieces to minimize jaw strain.
- Warm or Cold Packs: Apply moist heat (warm compress) for 15-20 minutes several times a day to relax tense muscles. Alternatively, use a cold pack to reduce acute inflammation and numb pain.
- Gentle Jaw Exercises: Your dentist or physical therapist may recommend specific stretches to improve jaw mobility and strengthen muscles.
- Stress Management: Techniques like meditation, yoga, deep breathing, and counseling can help reduce jaw clenching and grinding.
- Avoid Excessive Jaw Movements: Limit wide yawns, chewing gum, nail-biting, or resting your chin on your hand.
- Pro Tip: Combine warm compresses with gentle massage on the affected muscles (cheeks, temples) for enhanced relief.
-
Medications:
- Pros: Can provide quick pain relief and reduce inflammation.
- Cons: Potential side effects, temporary relief, doesn't address the root cause.
- Description:
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter options like ibuprofen (Advil, Motrin) or naproxen (Aleve) help reduce pain and inflammation. For more severe cases, prescription-strength NSAIDs may be used.
- Muscle Relaxants: Drugs like cyclobenzaprine (Flexeril) or tizanidine (Zanaflex) can help alleviate muscle spasms and pain, often prescribed for short-term use.
- Corticosteroids: Oral corticosteroids or direct injections into the joint can powerfully reduce inflammation. Used cautiously due to potential side effects.
- Antidepressants: Low doses of tricyclic antidepressants, particularly at bedtime, can help with pain control, muscle relaxation, and improve sleep for chronic TMD sufferers, even without depression.
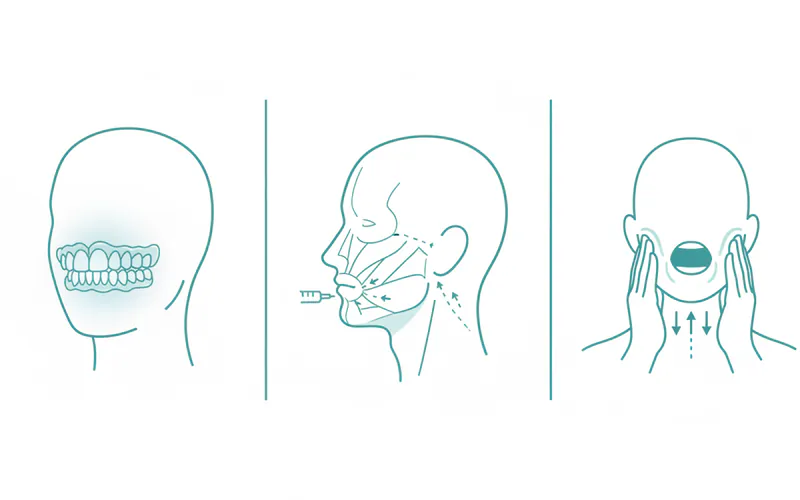
- Botulinum Toxin (Botox) Injections: Injections of Botox into the overactive jaw muscles (masseter, temporalis) can relax them, reducing clenching, grinding, and associated pain and swelling. Effects last typically 3-6 months.
-
Oral Appliances (Occlusal Splints or Nightguards):
- Pros: Protects teeth from grinding, repositions the jaw, reduces muscle activity.
- Cons: Can be expensive, requires custom fitting, compliance is key.
- Description: Custom-made plastic mouthguards that fit over your upper or lower teeth. They come in various types:
- Stabilization Splints: Most common, cover all teeth, help relax jaw muscles and prevent clenching/grinding. Worn primarily at night.
- Repositioning Splints: Less common, designed to temporarily move the jaw into a different position to improve disc alignment. Used for shorter periods and carefully monitored.
- ADA Recommendation: The American Dental Association (ADA) generally supports the use of stabilization splints as a conservative treatment for TMDs.
-
Physical Therapy:
- Pros: Addresses muscle imbalances, improves posture, teaches self-management techniques.
- Cons: Requires multiple sessions, patient commitment.
- Description: A physical therapist experienced in craniomandibular disorders can teach you exercises to stretch and strengthen jaw muscles, improve posture, and reduce tension. Techniques may include massage, ultrasound, trigger point therapy, and transcutaneous electrical nerve stimulation (TENS).
Invasive Treatments (When Conservative Options Fail)
If conservative treatments don't provide sufficient relief after several months, or if there's severe joint damage, more invasive procedures may be considered.
-
Arthrocentesis:
- Pros: Minimally invasive, relatively low risk, can quickly relieve pain and improve jaw mobility.
- Cons: Not effective for all types of TMD, temporary relief for some.
- Description: A procedure performed under local anesthesia where small needles are inserted into the joint. Fluid is flushed through the joint to remove inflammatory byproducts and loosen adhesions, sometimes followed by corticosteroid injection.
-
Arthroscopy:
- Pros: Minimally invasive surgery, allows direct visualization of the joint, faster recovery than open surgery.
- Cons: Requires general anesthesia, still surgical, not suitable for all joint issues.
- Description: A small incision is made, and a tiny camera (arthroscope) is inserted into the joint. The surgeon can then visualize the joint, remove inflamed tissue, wash out the joint, or reposition a displaced disc with tiny instruments.
-
Open-Joint Surgery (Arthroplasty):
- Pros: Can address complex structural problems, potentially providing long-term relief.
- Cons: Highly invasive, longer recovery, higher risks of complications (nerve damage, infection, scarring).
- Description: Reserved for severe cases where other treatments have failed and there is significant joint degeneration, ankylosis (joint fusion), or tumors. It involves a larger incision to directly access and repair or replace joint structures. Options include disc repair, removal of bone spurs, or total joint replacement.
Treatment for Related Causes of Facial Swelling:
- Dry Socket Molar: Treatment focuses on pain management and promoting healing. The dentist will gently clean the socket, remove any debris, and pack it with medicated gauze (often containing eugenol) to soothe the nerve endings. The packing is changed every 24-48 hours until symptoms subside, usually within a week. Pain medication will be prescribed.
- Gums Swelling Over Teeth (Pericoronitis/Abscess):
- Pericoronitis: Initial treatment involves cleaning the area, antibiotics if infection is spreading, and pain relief. Definitive treatment often requires extraction of the affected wisdom tooth or removal of the overlying gum flap (operculum) once the acute infection subsides.
- Dental Abscess: Requires immediate dental intervention to drain the pus and eliminate the source of infection. This may involve root canal therapy, incision and drainage, or tooth extraction, along with antibiotics.
Step-by-Step Process: What to Expect During Treatment
The journey to resolving TMJ face swelling typically follows a structured approach, starting with diagnosis and moving through progressive treatment stages.
-
Initial Consultation and Diagnosis:
- Patient History: Your dentist or oral surgeon will ask about your symptoms, medical history, stress levels, and habits (e.g., teeth grinding).
- Clinical Examination: The dentist will carefully examine your jaw, listen for clicks/pops, feel for tenderness or muscle spasms, and assess your jaw's range of motion. They will also check for signs of gums swelling over teeth or dry socket molar if you've recently had an extraction.
- Imaging: X-rays, CT scans, or MRI scans may be ordered to visualize the joint, disc, and surrounding bone for signs of damage, inflammation, or displacement. An MRI is particularly useful for soft tissue assessment.
-
Developing a Treatment Plan:
- Based on the diagnosis, your healthcare provider will recommend a personalized treatment plan, starting with the least invasive options.
- This plan will outline the specific therapies, expected timeline, and potential costs.
-
Implementing Conservative Treatment (e.g., Oral Appliance Therapy):
- Impression Taking: If an oral appliance (splint/nightguard) is recommended, impressions of your teeth will be taken.
- Appliance Fabrication: A dental lab will custom-make your appliance, usually taking 1-2 weeks.
- Fitting and Adjustments: You'll return for a fitting appointment where the dentist ensures the appliance fits comfortably and makes necessary adjustments to your bite.
- Home Use and Follow-up: You'll be instructed on how to wear and care for your appliance. Regular follow-up appointments (e.g., every 2-4 weeks initially) are crucial for adjustments and monitoring progress.
- Pro Tip: Be diligent in wearing your oral appliance as prescribed, especially during sleep, as this is often when clenching and grinding are most severe.
-
Implementing Other Treatments (e.g., Physical Therapy, Medications, Injections):
- Physical Therapy: You'll have scheduled sessions with a physical therapist, learning exercises and receiving manual therapy. Consistency with home exercises is vital.
- Medications: Prescriptions will be given with instructions on dosage and duration. Report any side effects immediately.
- Botox Injections: These are performed in the clinic, typically taking 15-30 minutes. You may feel mild discomfort, and full effects appear in 1-2 weeks. Repeat injections are usually needed every 3-6 months.
-
Surgical Procedures (if necessary):
- For arthrocentesis or arthroscopy, these are typically outpatient procedures performed under local or general anesthesia. Recovery is usually within a few days to a week.
- Open-joint surgery requires general anesthesia, an overnight hospital stay, and a significantly longer recovery period (weeks to months).
- Post-operative care will involve pain management, dietary restrictions, and specific physical therapy exercises.
-
Ongoing Management and Prevention:
- Once acute symptoms like swelling subside, the focus shifts to long-term management and prevention strategies to avoid recurrence. This may include continued use of oral appliances, stress management, and regular dental check-ups.
Cost and Insurance
The cost of treating TMJ face swelling can vary significantly based on the severity of your condition, the chosen treatment path, your geographic location (urban centers typically have higher costs), and whether you have dental or medical insurance.
Average US Cost Ranges (Without Insurance):
| Treatment Type | Average US Cost Range (Low-Mid-High) | Notes |
|---|---|---|
| Self-Care (Packs, Soft Diet) | $0 - $100 | Minimal, mostly cost of supplies. |
| Over-the-Counter Medications | $10 - $50 | NSAIDs, pain relievers. |
| Prescription Medications | $20 - $200 | Muscle relaxants, stronger NSAIDs, low-dose antidepressants. Varies widely by drug and pharmacy. |
| Custom Oral Appliance (Nightguard) | $300 - $2,500 | Varies by material, complexity, and practitioner. Average is often $600-$1,200. |
| Physical Therapy Session | $50 - $250 per session | Multiple sessions often required (e.g., 6-12 sessions). Total cost can be $300-$3,000+. |
| Botox Injections (Therapeutic) | $500 - $1,500 per session | Price often depends on the number of units required. Needs repeat treatment every 3-6 months. |
| Arthrocentesis | $1,000 - $3,000 per joint | Includes facility fees, anesthesia, and surgeon's fee. |
| TMJ Arthroscopy | $5,000 - $15,000 per joint | More complex, higher facility and anesthesia costs. |
| Open-Joint TMJ Surgery (Arthroplasty) | $15,000 - $50,000+ per joint | Varies greatly based on complexity (e.g., disc repair vs. total joint replacement). Can involve hospital stay. |
| Dry Socket Treatment | $100 - $300 per visit | Follow-up visits for dressing changes. (Initial extraction cost separate). |
| Dental Abscess/Pericoronitis Treatment | $150 - $2,000+ | Depends on severity. May involve antibiotics, incision and drainage, root canal, or extraction. Extraction of wisdom tooth can be $200-$700 for simple, $500-$1,500 for surgical. |
Regional Cost Variations: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles, Boston) compared to rural areas or states with lower costs of living. For instance, a custom nightguard might cost $800 in a rural clinic but $1,500 in a high-end urban practice.
Insurance Coverage Details:
- Medical vs. Dental Insurance: This is a critical distinction for TMJ treatment.
- Medical Insurance: Often covers services deemed medically necessary, such as diagnostics (MRI, CT scans), physical therapy, prescription medications, Botox injections for therapeutic use, and surgical procedures (arthrocentesis, arthroscopy, open-joint surgery). Many plans require a referral from your primary care physician and prior authorization for specialized treatments or surgeries.
- Dental Insurance: Primarily covers dental procedures like cleanings, fillings, crowns, and extractions. It may cover a portion of diagnostic X-rays or a custom nightguard if it's explicitly coded as a dental appliance for bruxism, but often not for direct TMJ disorder treatment. Some dental plans have specific clauses for "medically necessary" oral appliances.
- "Medically Necessary" Definition: Insurance companies typically define what constitutes "medically necessary." They often require documentation of conservative treatment failure before approving more advanced interventions.
- Deductibles and Co-pays: Be prepared for deductibles (the amount you pay before insurance kicks in) and co-pays (a fixed amount you pay for each service) or co-insurance (a percentage of the cost).
- Out-of-Network Costs: If you see providers outside your insurance network, your out-of-pocket costs will be significantly higher.
Payment Plans and Financing Options: Many dental and oral surgery offices offer payment plans directly or through third-party financing companies like CareCredit. These plans allow you to pay for treatment over several months, often with low or no interest for a promotional period. Don't hesitate to discuss financial options with your provider's administrative staff.
Cost-Saving Tips:
- Clarify Coverage Before Treatment: Always contact your insurance provider directly to understand what is covered and what your out-of-pocket expenses will be. Get pre-authorization for significant procedures.
- Seek In-Network Providers: To minimize costs, choose dentists, specialists, and facilities that are in your insurance network.
- Generic Medications: Ask your doctor if generic versions of prescribed medications are available.
- Shop Around (Carefully): For non-emergency treatments like custom nightguards, you might find price variations between dental offices. However, prioritize experience and quality of care over cost alone, especially for complex issues.
- Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs): Use these tax-advantaged accounts to pay for qualified medical and dental expenses.
Recovery and Aftercare
Recovery from TMJ face swelling and its underlying causes is a process that requires patience and adherence to post-treatment guidelines. The duration and specifics of aftercare depend on the type of treatment received.
For Conservative Treatments (Splints, PT, Medications):
- Pain Management: Continue with prescribed or over-the-counter pain relievers as needed. Use warm or cold compresses to soothe discomfort.
- Dietary Modifications: Stick to a soft diet for several weeks, gradually reintroducing firmer foods as tolerated. Avoid biting into hard items (apples, raw carrots) or chewing gum.
- Jaw Exercises: Continue with gentle jaw stretches and exercises as instructed by your physical therapist or dentist to maintain mobility and strength. Consistency is key.
- Oral Appliance Care: Clean your nightguard daily with a soft brush and mild soap or denture cleaner. Store it in a protective case when not in use.
- Follow-up Appointments: Attend all scheduled follow-up visits with your dentist or specialist. These are crucial for monitoring progress, adjusting appliances, and refining your treatment plan.
- Pro Tip: Maintain a stress journal to identify triggers and actively practice relaxation techniques to prevent relapse.
For Invasive Procedures (Arthrocentesis, Arthroscopy, Open Surgery):
- Immediate Post-Op (First Few Days):
- Pain and Swelling: Expect some pain and swelling around the jaw. Your surgeon will prescribe pain medication. Apply ice packs for the first 24-48 hours to reduce swelling.
- Rest: Get plenty of rest. Avoid strenuous activity.
- Soft/Liquid Diet: You will likely be on a liquid or very soft diet initially, progressing slowly.
- Oral Hygiene: Follow specific instructions for keeping the surgical site clean to prevent infection.
- Mid-Term Recovery (Weeks to Months):
- Physical Therapy: This is often a critical component of post-surgical recovery. You'll work with a physical therapist to regain full jaw movement, prevent stiffness, and strengthen muscles.
- Activity Restrictions: Avoid heavy lifting, contact sports, or activities that could impact your jaw.
- Follow-up Appointments: Regular check-ups with your surgeon are essential to monitor healing and assess long-term outcomes.
- Long-Term Management:
- Continue with any prescribed oral appliances or lifestyle modifications.
- Be mindful of jaw habits (clenching, grinding).
- Report any new or returning symptoms to your healthcare provider promptly.
For Dry Socket Molar or Gums Swelling Over Teeth:
- Dry Socket: Continue with medicated dressings as instructed. Avoid smoking, drinking through a straw, or vigorous rinsing, which can dislodge the clot. Pain should gradually subside over 5-7 days.
- Gum Infection/Abscess: Complete your full course of antibiotics, even if symptoms improve. Maintain meticulous oral hygiene. Follow your dentist's instructions regarding any definitive treatment like root canal or extraction.
Prevention
Preventing TMJ face swelling often boils down to managing the underlying causes and protecting your jaw joints.
- Manage Stress: Since stress is a major trigger for jaw clenching and grinding, actively incorporate stress-reduction techniques into your daily routine. This could include meditation, deep breathing exercises, yoga, regular exercise, or professional counseling.
- Avoid Destructive Jaw Habits:
- Stop Clenching/Grinding: If you're aware you clench or grind, consciously try to keep your teeth slightly apart when not eating or speaking. Place your tongue gently on the roof of your mouth behind your upper front teeth.
- Avoid Chewing Gum: Continuous gum chewing puts unnecessary strain on the TMJ.
- Limit Hard/Chewy Foods: Minimize foods that require excessive chewing (e.g., tough meats, raw vegetables, sticky candy).
- Break Other Habits: Don't bite your nails, chew on pens, or hold the phone between your shoulder and ear.
- Maintain Good Posture: Poor posture, especially forward head posture, can strain the neck and jaw muscles, contributing to TMDs. Be mindful of your posture while sitting, standing, and using digital devices.
- Wear an Oral Appliance (if recommended): If you grind or clench your teeth, especially at night, a custom-fitted nightguard can protect your teeth from wear and reduce the stress on your TMJs. Discuss this with your dentist.
- Regular Dental Check-ups: Regular visits allow your dentist to monitor your jaw health, check for signs of bruxism, malocclusion, or early signs of gum disease or other dental infections that could lead to gums swelling over teeth. Addressing these issues proactively can prevent more severe tmj face swelling or other complications.
- Protect Against Trauma: Wear a mouthguard during sports activities that carry a risk of facial injury.
- Address Malocclusion: If you have a misaligned bite, discuss orthodontic treatment options with your dentist or orthodontist.
Risks and Complications
While TMJ disorders are generally not life-threatening, ignoring TMJ face swelling and its underlying causes can lead to a range of complications, some serious.
- Chronic Pain: Untreated TMDs can evolve into persistent, debilitating pain in the jaw, face, head, and neck, significantly impacting quality of life.
- Progressive Joint Damage: Over time, continuous inflammation, disc displacement, and abnormal joint mechanics can lead to irreversible damage to the TMJ, including cartilage erosion and bone changes.
- Permanent Alteration of Bite: Changes in the joint structure can cause your upper and lower teeth to no longer meet correctly, leading to chewing difficulties and further strain.
- Limited Jaw Mobility: The jaw can become increasingly stiff, making it difficult to open or close the mouth, which can affect eating, speaking, and oral hygiene.
- Psychological Impact: Chronic pain and physical limitations can lead to anxiety, depression, sleep disturbances, and a reduced ability to participate in daily activities.
- Surgical Complications (for invasive treatments):
- Infection: As with any surgery.
- Nerve Damage: Damage to facial nerves can cause temporary or permanent numbness, weakness, or paralysis in parts of the face.
- Bleeding: Excessive bleeding during or after surgery.
- Adverse Reaction to Anesthesia:
- Failure of Treatment: The surgery may not fully resolve symptoms, or complications may arise that necessitate further intervention.
- Scarring: Especially with open-joint surgery.
- Complications from Untreated Dental Issues:
- An untreated dry socket molar can lead to delayed healing, chronic pain, and more widespread infection in rare cases.
- Untreated gums swelling over teeth due to infection (like an abscess or severe pericoronitis) can spread to other areas of the face and neck, potentially leading to serious conditions like Ludwig's angina (a severe infection of the floor of the mouth) or sepsis, which are life-threatening medical emergencies.
Comparison Tables
Here are two tables to help compare different aspects of TMJ treatment and differentiate causes of facial swelling.
Table 1: Conservative vs. Invasive TMJ Treatments
| Feature | Conservative Treatments (e.g., Splint, PT, Meds) | Invasive Treatments (e.g., Arthrocentesis, Surgery) |
|---|---|---|
| Approach | Non-surgical, focuses on symptom management and lifestyle changes. | Surgical intervention directly on the joint. |
| Primary Goal | Reduce pain, inflammation, muscle spasms; improve jaw function; prevent damage. | Repair or replace damaged joint structures; remove adhesions; severe pain relief. |
| Effectiveness | Highly effective for most TMD cases (approx. 80-90%). | Reserved for severe, recalcitrant cases; generally effective when conservative fails. |
| Risks | Minimal (e.g., medication side effects, appliance discomfort). | Higher (e.g., infection, nerve damage, anesthesia risks, scarring, failure of treatment). |
| Recovery Time | Days to weeks for initial relief; ongoing management. | Days (arthrocentesis/arthroscopy) to months (open surgery). |
| Cost Range (US) | $10 - $2,500 (depending on combination of treatments). | $1,000 - $50,000+ (depending on procedure and complexity). |
| Insurance Cover. | Often covered by medical insurance for PT, meds; splints may be dental or medical. | Often covered by medical insurance (requires pre-authorization). |
| Pros | Low risk, non-invasive, cost-effective, patient-empowering. | Can resolve structural issues, provides relief when conservative options fail. |
| Cons | Requires patient compliance, may not address severe structural damage. | Higher risk, greater cost, longer recovery, potential for permanent changes. |
Table 2: Common Causes of Facial Swelling Around the Jaw
| Feature | TMJ Inflammation/Disorder (TMD) | Dry Socket Molar | Gums Swelling Over Teeth (Abscess/Pericoronitis) |
|---|---|---|---|
| Location of Swelling | Around the TMJ (in front of ear), jawline, cheek. Often unilateral. | Localized around the extraction site. | Localized on the gums around a specific tooth, can spread to cheek/jaw. |
| Primary Symptoms | Jaw pain, clicking, limited opening, headaches, ear pain. | Severe, throbbing pain days after extraction; foul odor/taste; exposed bone. | Severe toothache, red/swollen gums, pus, fever, bad taste. |
| Onset | Gradual or acute after trauma/stress. | 2-5 days after tooth extraction. | Often acute, can be rapid onset with severe pain. |
| Associated Factors | Bruxism, stress, trauma, arthritis, malocclusion. | Dislodged blood clot after extraction. | Bacterial infection, impacted wisdom tooth, deep cavity. |
| Urgency | Consult dentist if persistent or worsening. | Urgent dental visit needed for pain relief and healing. | Emergency dental visit needed, especially with fever/spreading swelling. |
| Typical Treatment | Conservative (splints, PT, meds) or surgical. | Medicated dressing, cleaning, pain management. | Antibiotics, drainage, root canal, or extraction. |
Children / Pediatric Considerations
While TMJ disorders are often associated with adults, children and adolescents can also experience TMJ face swelling and related symptoms. However, diagnosing and treating TMDs in children requires specific considerations due to their developing facial structures and unique psychological factors.
- Causes in Children:
- Trauma: Falls, sports injuries, or direct blows to the jaw are common causes.
- Bruxism: Many children grind or clench their teeth, especially during sleep. This can be related to stress, allergies, or even malocclusion.
- Orthodontic Treatment: In some cases, extensive orthodontic work or specific types of appliances can influence TMJ function, though this is debated.
- Systemic Conditions: Juvenile idiopathic arthritis or other autoimmune diseases can affect the TMJs in children.
- Habits: Thumb-sucking, nail-biting, or prolonged pacifier use can sometimes contribute to jaw imbalances.
- Symptoms: Children may present with similar symptoms to adults, including jaw pain, headaches, clicking, and difficulty chewing. However, they may struggle to articulate their pain precisely. Parents might notice:
- Difficulty opening mouth fully.
- Changes in eating habits (e.g., favoring soft foods).
- Complaints of earaches or headaches.
- Facial swelling or asymmetry.
- Sounds from the jaw joint during meals.
- Diagnosis: Diagnosis can be challenging as children's symptoms might be attributed to other common childhood ailments. A thorough dental and medical history, physical examination, and sometimes imaging (MRI is preferred over X-rays/CT to avoid radiation) are crucial.
- Treatment: Pediatric TMD treatment is almost always conservative, focusing on gentle, reversible interventions that don't interfere with growth and development.
- Self-care: Soft diet, warm compresses, gentle jaw exercises.
- Behavioral Therapy: Addressing habits like bruxism or stress with relaxation techniques.
- Oral Appliances: Custom-made nightguards can be used, carefully designed to accommodate growth.
- Medications: NSAIDs for pain and inflammation, always under pediatric guidance.
- Physical Therapy: Tailored exercises to improve jaw function.
- Orthodontic Evaluation: If malocclusion is a significant contributing factor, an orthodontist may be consulted, though caution is advised regarding aggressive orthodontic interventions for TMD in children.
- Parental Guidance: Parents play a vital role in observing symptoms, encouraging adherence to treatment plans, and creating a supportive environment. It's crucial for parents to take their child's complaints seriously and seek evaluation from a pediatric dentist or oral surgeon experienced in pediatric TMDs.
Frequently Asked Questions
Q1: Is TMJ swelling dangerous?
A1: While TMJ swelling itself is not usually life-threatening, it indicates an underlying problem that, if left untreated, can lead to chronic pain, progressive joint damage, and significant impact on your quality of life. In rare cases, severe swelling might indicate an infection that needs immediate attention.
Q2: How long does TMJ swelling last?
A2: The duration of TMJ swelling varies. Acute inflammation from overuse or stress might subside within a few days with self-care. Swelling related to chronic conditions like arthritis can be persistent or episodic. With proper treatment, significant improvement is usually seen within a few weeks to months.
Q3: Can TMJ swelling go down on its own?
A3: Minor TMJ swelling related to temporary stress or overuse might decrease with rest, a soft diet, and warm/cold compresses. However, if the swelling is persistent, severe, or accompanied by significant pain or limited jaw movement, it's crucial to see a dentist as it likely won't resolve fully without intervention.
Q4: What helps TMJ swelling?
A4: Initial steps include rest, a soft diet, applying warm or cold compresses, and over-the-counter NSAIDs like ibuprofen. A dentist might recommend a custom oral appliance (nightguard), physical therapy, or prescription muscle relaxants to reduce inflammation and promote healing.
Q5: Is surgery always necessary for TMJ swelling?
A5: No, surgery is considered a last resort for TMJ swelling and related disorders. The vast majority (80-90%) of TMDs respond well to conservative treatments such as oral appliances, physical therapy, medications, and lifestyle modifications. Surgery is typically reserved for severe cases with structural damage that haven't responded to non-invasive approaches.
Q6: Does insurance cover TMJ treatments?
A6: Insurance coverage for TMJ treatments can be complex. Medical insurance often covers diagnostic imaging (MRI), physical therapy, therapeutic Botox injections, and surgical procedures if deemed medically necessary. Dental insurance may cover some aspects like custom nightguards, but it's essential to verify coverage with both your medical and dental insurance providers before starting treatment.
Q7: Can stress cause TMJ swelling?
A7: Yes, stress is a significant contributing factor to TMJ issues, including swelling. Many people unconsciously clench their jaw or grind their teeth (bruxism) when stressed, leading to muscle tension, inflammation, and pain around the TMJ, which can manifest as facial swelling.
Q8: What's the difference between TMJ swelling and a dental abscess?
A8: TMJ swelling is typically centered around the jaw joint (in front of the ear) and may involve jaw pain, clicking, or limited movement. A dental abscess, however, originates from an infected tooth or gum and causes swelling directly around that tooth, often accompanied by severe toothache, pus, sensitivity to hot/cold, and sometimes fever.
Q9: Can a dry socket cause facial swelling similar to TMJ?
A9: A dry socket primarily causes intense pain and localized inflammation at the site of a recent tooth extraction, often with a visible empty socket. While the severe pain can radiate and some surrounding soft tissue swelling may occur, it's typically more localized than diffuse TMJ swelling and is distinctly linked to a recent extraction. It wouldn't present with typical TMJ symptoms like clicking or locking.
Q10: What kind of doctor treats TMJ?
A10: A general dentist is often the first point of contact for TMJ issues. They may refer you to a specialist such as an oral and maxillofacial surgeon, a prosthodontist, an orthodontist, or a pain management specialist, depending on the complexity and cause of your TMJ disorder. Physical therapists and neurologists can also be involved in multidisciplinary care.
When to See a Dentist
Recognizing when to seek professional help for TMJ face swelling is paramount to preventing worsening symptoms and potential complications. While minor, temporary swelling might resolve on its own, certain signs warrant immediate attention.
You should schedule a routine appointment with your dentist if you experience:
- Persistent Facial Swelling: Swelling around your jaw that lasts more than a few days, even if pain is mild.
- Chronic Jaw Pain: Ongoing pain in your jaw, face, ear, or neck, especially if it interferes with daily activities.
- Frequent Jaw Clicking or Popping: While occasional sounds without pain may not be a concern, if they are consistent, painful, or accompanied by limited jaw movement, get it checked.
- Difficulty Chewing or Speaking: Any persistent change in your ability to comfortably open your mouth, chew food, or speak clearly.
- Changes in Your Bite: If you feel your teeth don't fit together as they used to.
You should seek immediate dental or medical attention (Emergency or Urgent Care) if you experience:
- Severe, Rapidly Worsening Swelling: Especially if it spreads quickly to your throat or eye area, or if it makes breathing or swallowing difficult. This could indicate a severe infection.
- Intense, Unbearable Pain: Pain that is not relieved by over-the-counter pain medication and is impacting your ability to function.
- Fever with Swelling: Swelling accompanied by a fever, chills, or general malaise can be a sign of a serious infection (e.g., a dental abscess or spreading infection from a dry socket).
- Inability to Open Your Mouth (Lockjaw): If your jaw locks completely, making it impossible to open or close, this is an urgent situation.
- Swelling Following Recent Dental Surgery: If you develop significant pain, swelling, or a foul odor after a tooth extraction, especially from a dry socket molar, contact your dentist immediately.
- Pus Discharge: Any visible pus draining from the gum line or around a tooth indicates an active infection that requires urgent care.
Don't ignore the warning signs your body sends. Early diagnosis and intervention for TMJ face swelling can make a significant difference in treatment outcomes and your overall oral health and well-being.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
How to Relieve Gum Swelling
When your gums are swollen, it can be an alarming and uncomfortable experience, often signaling an underlying issue that requires attention. Statistics from the Centers for Disease Control and Prevention (CDC) reveal that **nearly half of adults aged 30 or older in the United States have some form o
February 23, 2026
Teeth Swelling: Complete Guide
When you experience teeth swelling, it's more than just a minor discomfort; it's a clear signal from your body that something is amiss within your oral cavity, often indicating an underlying infection or inflammation that requires prompt attention. A recent survey revealed that **over 25% of adu
February 23, 2026
Submandibular Salivary Gland Swelling: Complete Guide
When you notice a peculiar lump or uncomfortable fullness beneath your jaw, it can be an alarming experience. This sensation, often accompanied by pain and difficulty swallowing, could indicate submandibular salivary gland swelling. Affecting an estimated 1 in 10,000 adults annually, conditi
February 23, 2026
What Helps With Gum Swelling
Gum swelling, medically known as gingival swelling or gingivitis, is a common yet often underestimated dental issue affecting millions of Americans. Have you ever woken up with sore, puffy gums that bleed easily when you brush? You're not alone. Research indicates that nearly **half of all a
February 23, 2026