Dry Mouth at Night: Complete Guide

Key Takeaways
- Waking up with a parched mouth, a sticky tongue, or a persistent thirst can be more than just an annoyance; it's a common symptom of a condition known medically as xerostomia, or dry mouth at night. For an estimated 10-30% of adults in the United States, this nightly discomfort is a reality,
Dry Mouth at Night: Complete Guide
Waking up with a parched mouth, a sticky tongue, or a persistent thirst can be more than just an annoyance; it's a common symptom of a condition known medically as xerostomia, or dry mouth at night. For an estimated 10-30% of adults in the United States, this nightly discomfort is a reality, impacting sleep quality, oral health, and overall well-being. Far from being a mere inconvenience, chronic dry mouth, especially while you sleep, can signal underlying health issues and significantly increase your risk for serious dental problems like cavities and gum disease.

Understanding what causes dry mouth and how to effectively manage it is crucial for maintaining optimal oral health and ensuring restful sleep. This comprehensive guide from SmilePedia.net will delve deep into the nuances of nocturnal dry mouth, exploring its common causes, identifiable symptoms, a wide range of treatment options, preventative measures, and critical insights into when to seek professional dental or medical advice. We aim to equip you with the knowledge to identify, address, and overcome the challenges of dry mouth at night, helping you reclaim comfortable nights and healthier mornings.
Key Takeaways:
- Prevalence: Dry mouth affects 10-30% of adults, with symptoms often worse at night.
- Primary Cause: Medications are the leading cause, accounting for roughly 70% of chronic dry mouth cases. Over 500 prescription and OTC drugs can reduce saliva flow.
- Serious Consequences: Untreated chronic dry mouth increases the risk of tooth decay by up to 3 times, gum disease, oral infections (like thrush), and difficulty eating/speaking.
- Initial Steps: Start with lifestyle modifications (hydration, humidifiers) and over-the-counter saliva substitutes (gels, sprays). These can cost $5-$25 per product monthly.
- Professional Intervention: If lifestyle changes and OTC remedies are insufficient, consult a dentist. Diagnosis may involve salivary flow tests (sialometry) at $50-$200.
- Prescription Options: For severe cases, prescription medications like pilocarpine or cevimeline can stimulate saliva production, costing $30-$150 per month (often covered by insurance).
- Long-term Management: Regular dental check-ups (every 3-6 months), prescription fluoride products, and ongoing hydration are essential for managing chronic dry mouth.
What Dry Mouth at Night Is: An Overview
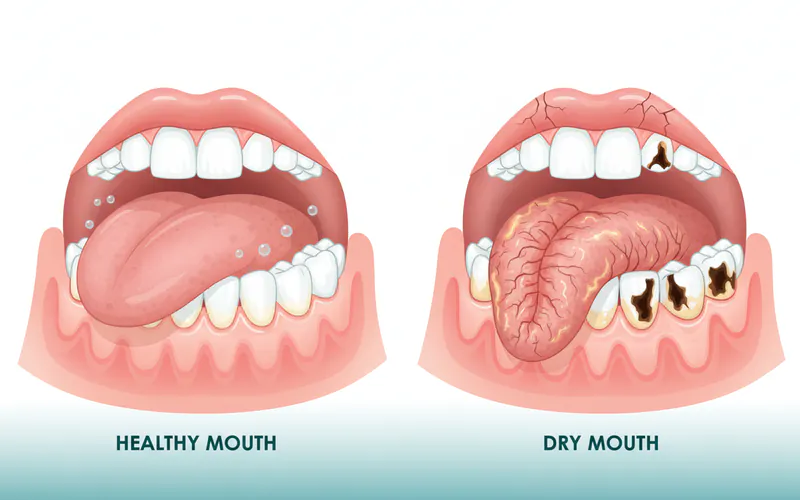
Dry mouth at night, clinically known as nocturnal xerostomia, is the subjective sensation of having an insufficient amount of saliva in your mouth during sleep. Saliva plays a vital role in maintaining oral health: it moistens food, aids in chewing and swallowing, begins the digestion process, neutralizes acids produced by bacteria, washes away food particles, and contains minerals and enzymes that protect tooth enamel and fight infections. When saliva flow is reduced or absent, especially for extended periods during the night, these protective functions diminish significantly.
Unlike temporary thirst, chronic dry mouth indicates a persistent problem with salivary gland function. While experiencing occasional dryness is normal, especially after strenuous exercise or insufficient fluid intake, persistent dry mouth at night can be a sign of an underlying health issue or a side effect of medication. It's often more pronounced at night because salivary glands naturally produce less saliva during sleep, and factors like mouth breathing can exacerbate the problem. This combination creates an environment ripe for discomfort and potential oral health complications.
The Role of Saliva
To fully grasp the impact of dry mouth, it's essential to understand the multifaceted roles of saliva:
- Lubrication: Saliva lubricates the mouth and throat, making it easier to speak, chew, and swallow.
- Protection: It helps protect teeth against decay by neutralizing acids and washing away food debris. It also contains antimicrobial agents that combat bacteria, viruses, and fungi.
- Digestion: Enzymes in saliva (like amylase) begin the breakdown of starches and fats, aiding in digestion.
- Taste: Saliva dissolves food chemicals, allowing taste buds to perceive flavors.
- Remineralization: Saliva is rich in calcium and phosphate, which help remineralize tooth enamel and repair early decay.
When saliva production falters, particularly overnight when the mouth is typically at its driest, all these crucial functions are compromised, leading to a cascade of oral and systemic health issues.
Causes of Dry Mouth at Night: Why It Happens
Understanding what causes dry mouth is the first step toward effective management. The causes are diverse, ranging from common lifestyle habits to serious medical conditions and medication side effects. Often, it's a combination of factors that contribute to the severity of dry mouth at night.
1. Medications (Most Common Cause)
Over 500 prescription and over-the-counter (OTC) medications list dry mouth as a potential side effect. This makes medication the single most common cause of chronic xerostomia. The effect can be dose-dependent, meaning higher doses may lead to more severe dryness.
- Antihistamines: Used for allergies and colds (e.g., diphenhydramine, loratadine).
- Decongestants: (e.g., pseudoephedrine, phenylephrine).
- Antidepressants and Anxiolytics: Many types, including tricyclic antidepressants (e.g., amitriptyline) and SSRIs (e.g., fluoxetine).
- Antihypertensives (Blood Pressure Medications): Especially diuretics (e.g., hydrochlorothiazide) and beta-blockers.
- Pain Medications: Opioids and certain non-steroidal anti-inflammatory drugs (NSAIDs).
- Muscle Relaxants: (e.g., cyclobenzaprine).
- Antiparkinsonian Drugs: Used to treat Parkinson's disease.
- Chemotherapy Drugs: Often cause severe dry mouth.
- Anticholinergics: Used for conditions like overactive bladder or IBS.
2. Medical Conditions
Several systemic diseases can directly or indirectly affect salivary gland function:
- Sjögren's Syndrome: An autoimmune disease where the immune system attacks moisture-producing glands, including salivary glands. This is a significant cause of chronic dry mouth and dry eyes.
- Diabetes: Poorly controlled blood sugar can lead to dehydration and nerve damage affecting salivary glands.
- Sleep Apnea: Obstructive Sleep Apnea (OSA) often involves mouth breathing or using CPAP machines, which can dry out the mouth and throat.
- Nerve Damage: Injury or surgery to the head and neck area can damage nerves responsible for salivary gland stimulation.
- Autoimmune Diseases: Beyond Sjögren's, conditions like rheumatoid arthritis, lupus, and scleroderma can also impact salivary glands.
- HIV/AIDS: Can directly affect salivary glands or be a side effect of medications.
- Alzheimer's and Parkinson's Disease: These neurological conditions can lead to reduced saliva production or difficulty in managing saliva.
- Stroke: Can result in nerve damage affecting salivary gland function.
- Thyroid Disorders: Hypothyroidism can sometimes contribute to dry mouth.
- Anxiety and Depression: The conditions themselves and their treatments can cause dry mouth.
3. Lifestyle Factors
Your daily habits can significantly influence saliva production:
- Dehydration: Insufficient fluid intake is a direct cause of reduced saliva.
- Mouth Breathing: Especially common during sleep, mouth breathing causes rapid evaporation of saliva. This is a major contributor to dry mouth at night. Causes include nasal congestion, deviated septum, enlarged tonsils/adenoids, or simply habit.
- Smoking and Tobacco Use: Tobacco products, in any form, severely reduce saliva flow and irritate oral tissues.
- Alcohol Consumption: Alcohol is a diuretic and can lead to dehydration, exacerbating dry mouth.
- Caffeine: High intake of caffeinated beverages (coffee, tea, sodas) can also have a diuretic effect.
- Diet: A diet high in salty, dry, or spicy foods can worsen dry mouth symptoms.
- Stress and Anxiety: Can trigger a "fight or flight" response, reducing saliva production.
4. Cancer Treatments
- Radiation Therapy: Head and neck radiation therapy can cause severe and often permanent damage to salivary glands, leading to chronic dry mouth. The severity depends on the dose and area treated.
- Chemotherapy: Certain chemotherapy drugs can temporarily reduce saliva flow.
5. Age-Related Changes
While aging itself doesn't directly cause dry mouth, older adults are more prone to factors that do, such as:
- Taking multiple medications (polypharmacy).
- Having more systemic health conditions.
- Changes in body hydration status.
Signs and Symptoms of Dry Mouth at Night
The symptoms of dry mouth extend far beyond simply feeling thirsty. They can significantly impact your oral health, comfort, and quality of life. Recognizing these signs, especially when they occur or worsen during the night, is key to seeking timely treatment.
Common signs and symptoms of dry mouth at night include:
- Waking up with a dry or sticky feeling in your mouth: This is the most common and direct indicator.
- Frequent thirst, especially at night: You might find yourself reaching for water multiple times during the night or immediately upon waking.
- Difficulty speaking, chewing, or swallowing: Lack of lubrication makes these basic functions challenging. Food may feel dry and hard to move around your mouth.
- Sore throat or hoarseness: The lack of saliva can irritate the throat, leading to a persistent sore throat or a change in voice.
- Cracked lips and corners of the mouth (cheilosis): Dryness can cause the delicate skin around the mouth to crack and become painful.
- Bad breath (halitosis): Saliva helps wash away odor-causing bacteria. Without enough saliva, bacteria can proliferate, leading to persistent bad breath.
- Changes in taste (dysgeusia): Food may taste bland, metallic, or simply different.
- Tongue changes: The tongue may appear dry, red, raw, or grooved. It might stick to the roof of your mouth.
- Increased tooth decay (cavities): Saliva neutralizes acids and washes away food particles. Reduced saliva means less protection, making teeth much more vulnerable to decay, particularly at the gumline.
- Gum inflammation and disease (gingivitis/periodontitis): Without saliva's protective properties, gums are more susceptible to bacterial infections.
- Oral infections: An increase in fungal infections like oral thrush (candidiasis) is common due to the lack of antimicrobial properties of saliva.
- Problems with dentures: Dentures may slip, cause sores, or become uncomfortable to wear due due to lack of lubrication and suction.
- Burning or tingling sensation in the mouth: This is a condition known as burning mouth syndrome, sometimes associated with dry mouth.
If you experience several of these symptoms consistently, particularly if they interfere with your sleep or daily activities, it's crucial to consult a dentist or physician.
Treatment Options for Dry Mouth at Night
Effectively managing dry mouth at night often requires a multi-faceted approach, targeting both symptom relief and, where possible, the underlying cause. Treatment options range from simple lifestyle adjustments to prescription medications.
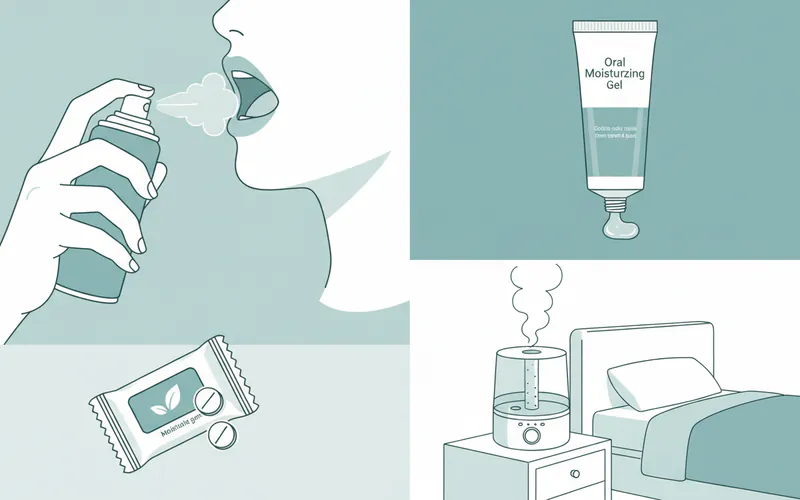
1. Lifestyle Modifications and Home Remedies
These are often the first line of defense and can significantly alleviate mild to moderate symptoms.
- Hydration: Sip water frequently throughout the day and keep a glass of water by your bedside.
- Pros: Natural, inexpensive, no side effects.
- Cons: Not always sufficient for severe cases; frequent trips to the bathroom at night can disrupt sleep.
- Humidifier: Using a cool-mist humidifier in your bedroom at night can add moisture to the air and help reduce oral dryness.
- Pros: Simple, effective for mouth breathers.
- Cons: Requires regular cleaning to prevent mold growth; may not fully address severe internal causes.
- Avoid Irritants:
- Caffeine & Alcohol: Limit or avoid, especially before bed, as they can be dehydrating.
- Tobacco: Quitting smoking or using smokeless tobacco is paramount. Tobacco significantly reduces saliva flow.
- Salty, Spicy, Dry Foods: These can further irritate a dry mouth.
- Sugary/Acidic Foods & Drinks: Avoid these to reduce the risk of accelerated tooth decay, as saliva isn't there to neutralize them.
- Breathe Through Your Nose: If mouth breathing is an issue, address underlying causes like nasal congestion.
- Pro Tip: Try nasal strips or a saline nasal spray before bed to improve nasal airflow. Consider consulting an ENT for persistent nasal obstruction.
- Chew Sugar-Free Gum or Suck on Sugar-Free Candies: These stimulate saliva production through mechanical action. Look for products containing Xylitol, which also helps prevent cavities.
- Pros: Readily available, provides immediate relief.
- Cons: Can sometimes lead to digestive upset (xylitol); temporary effect.
- Oral Hygiene: Maintain meticulous oral hygiene with fluoride toothpaste. Regular brushing and flossing are even more critical when saliva protection is reduced.
2. Over-the-Counter (OTC) Products
Many products are designed to mimic saliva or moisturize the oral cavity.
- Saliva Substitutes: Sprays, gels, rinses, or lozenges that contain ingredients like carboxymethylcellulose or hydroxyethylcellulose to coat oral tissues and provide moisture.
- Pros: Provide immediate, temporary relief; non-pharmacological.
- Cons: Frequent reapplication needed, especially at night; can feel thick or unnatural to some.
- Cost: $5 - $25 per product for a month's supply.
- Oral Moisturizers: Gels or rinses specifically formulated to adhere to oral tissues and provide lasting moisture. Some contain xylitol.
- Pros: Longer-lasting relief than sprays; can be applied before bed.
- Cons: May still require reapplication; can be expensive.
- Cost: $10 - $30 per product monthly.
- Fluoride Products: High-fluoride toothpastes, mouthwashes, or gels are crucial to prevent rampant decay associated with dry mouth.
- Pros: Essential for preventing cavities, which are a major complication.
- Cons: Prescription strength fluoride products require a dentist's recommendation.
- Cost: OTC fluoride toothpaste is standard; prescription fluoride can be $10-$20 for a tube.
3. Prescription Medications
When OTC remedies and lifestyle changes aren't enough, dentists or physicians may prescribe medications to stimulate saliva production. These are known as sialagogues.
- Pilocarpine (Salagen®): A cholinergic agonist that stimulates salivary glands.
- Pros: Can significantly increase natural saliva production for many patients.
- Cons: Requires consistent dosing; potential side effects include sweating, nausea, dizziness, increased urination. Not suitable for everyone (e.g., certain heart conditions, asthma).
- Cost: $30 - $100 per month, depending on dosage and generic vs. brand.
- Cevimeline (Evoxac®): Another cholinergic agonist, similar to pilocarpine, often prescribed for Sjögren's Syndrome.
- Pros: Similar efficacy to pilocarpine; some patients tolerate it better.
- Cons: Similar side effects (sweating, nausea, vision changes); also requires consistent dosing.
- Cost: $50 - $150 per month, depending on dosage and generic vs. brand.
4. Addressing Underlying Causes
Treating the root cause is often the most effective long-term solution.
- Medication Review: Discuss your medications with your doctor or dentist. They may be able to adjust dosages or switch to alternative drugs with fewer dry mouth side effects. Never stop taking prescribed medication without consulting your doctor.
- Sleep Apnea Treatment: If sleep apnea is contributing to mouth breathing and dry mouth, CPAP therapy or oral appliances can help. Addressing the sleep apnea itself improves overall health.
- Management of Systemic Diseases: Properly managing conditions like diabetes or autoimmune diseases (e.g., Sjögren's) can alleviate dry mouth symptoms.
- Referral to Specialists: For complex cases, referral to an oral medicine specialist, ENT, or rheumatologist may be necessary.
Step-by-Step Process: Managing Dry Mouth at Night
Effectively diagnosing and treating dry mouth at night involves a systematic approach, typically starting with your primary care physician or dentist.

Step 1: Initial Consultation and Diagnosis
- Dental/Medical History: Your dentist or doctor will ask about your symptoms, duration, severity, and any aggravating/alleviating factors. They will review your complete medical history, including all current medications (prescription, OTC, supplements), medical conditions, and lifestyle habits (smoking, alcohol, diet).
- Oral Examination: The dentist will carefully examine your mouth for signs of dryness (e.g., sticky tissues, lack of saliva pooling, red or fissured tongue, increased decay, gum inflammation, oral thrush).
- Salivary Flow Test (Sialometry): This test measures the rate of saliva production. You might be asked to spit into a cup over a certain period, or a device might be used to collect saliva. Both unstimulated and stimulated (e.g., chewing on paraffin wax) flow rates can be measured.
- Cost: Typically $50 - $200, often covered by dental insurance if medically necessary.
- Diagnostic Tests (if needed):
- Blood Tests: To check for underlying conditions like Sjögren's syndrome (autoantibodies), diabetes (blood glucose), or thyroid issues.
- Imaging: Rarely, advanced imaging (e.g., sialography, MRI) of salivary glands might be used to check for blockages or structural problems.
- Referrals: If an underlying systemic cause is suspected, you may be referred to an internist, rheumatologist, or endocrinologist. If sleep apnea is a concern, a sleep specialist may be recommended.
Step 2: Developing a Treatment Plan
Based on the diagnosis, your dental professional will develop a personalized treatment plan:
- Identify and Address Underlying Causes:
- Medication Adjustment: Discuss with your prescribing physician whether medication changes (dose, alternative drug) are possible.
- Medical Condition Management: Work with your doctor to manage conditions like diabetes or Sjögren's syndrome.
- Sleep Apnea Intervention: If diagnosed, follow recommendations for CPAP, oral appliances, or surgery.
- Symptom Relief and Oral Protection:
- Recommendation of OTC Products: Your dentist will recommend specific brands of saliva substitutes (gels, sprays, rinses) or oral moisturizers and provide guidance on their use. They might suggest products with xylitol.
- Prescription for Sialagogues: If OTC options are insufficient, prescription medications like pilocarpine or cevimeline may be considered, particularly for severe cases or conditions like Sjögren's.
- Prescription Fluoride: High-concentration fluoride toothpaste or gels will likely be prescribed to prevent rampant decay.
- Oral Hygiene Instruction: Detailed guidance on brushing, flossing, and potentially using interdental brushes, emphasizing consistency.
- Dietary Counseling: Advice on avoiding sugary, acidic, sticky, and overly dry foods.
Step 3: Implementation and Follow-up
- Consistent Application: Follow the recommended schedule for applying OTC products or taking prescription medications. Consistency is key for managing dry mouth at night.
- Lifestyle Changes: Implement recommended hydration strategies, humidifier use, and tobacco/alcohol cessation.
- Regular Dental Check-ups: Due to the increased risk of decay and gum disease, more frequent dental visits (e.g., every 3-6 months instead of 6-12 months) are often recommended. These appointments will include professional cleanings and fluoride applications.
- Monitor Symptoms: Keep track of how your symptoms respond to treatment. Report any improvements or worsening of dry mouth to your dentist or doctor.
- Adjustments: Your treatment plan may need adjustments over time based on your response and any changes in your health status or medications.
This systematic approach ensures that both the symptoms and the underlying causes of dry mouth at night are addressed comprehensively, leading to better oral health and improved quality of life.
Cost and Insurance for Dry Mouth Treatment
The cost of managing dry mouth at night can vary widely depending on the underlying cause, the severity of symptoms, and the chosen treatment options. Understanding these costs and potential insurance coverage is important for patients in the US.
Average US Price Ranges for Dry Mouth Treatments
| Treatment/Service | Average Cost Range (Without Insurance) | Insurance Coverage | Notes |
|---|---|---|---|
| Initial Dental Exam & Consultation | $50 - $150 | Usually covered | Basic examination to identify symptoms and potential causes. |
| Salivary Flow Test (Sialometry) | $50 - $200 | Often covered | Diagnostic test to measure saliva production. Coverage depends on medical necessity. |
| OTC Saliva Substitutes/Gels/Sprays | $5 - $25 per product (monthly) | Rarely covered | Non-prescription items like Biotene®, XyliMelts®. Ongoing cost. |
| OTC Xylitol Gum/Mints | $5 - $15 per pack | No coverage | Aides in saliva stimulation, cavity prevention. |
| Cool-Mist Humidifier | $30 - $100 | No coverage | One-time purchase, can help with nocturnal dry mouth from mouth breathing. |
| Prescription Fluoride Toothpaste/Gel | $10 - $30 per tube | Often covered | High-strength fluoride (e.g., Prevident®) to prevent rampant decay. Typically lasts 1-3 months. |
| Pilocarpine (Generic) | $30 - $100 per month | Often covered | Prescription medication to stimulate saliva. Cost varies by dose, pharmacy, and generic availability. |
| Cevimeline (Generic) | $50 - $150 per month | Often covered | Prescription medication, often for Sjögren's-related dry mouth. Cost varies. |
| Treating Related Complications: | |||
| * Dental Fillings | $100 - $400 per filling | Often 50-80% covered | Dry mouth significantly increases cavity risk. Costs depend on material and size. |
| * Gum Disease Treatment | $200 - $1,500+ | Often 50-80% covered | Deep cleaning (scaling and root planing) can be expensive, and advanced gum disease may require surgical intervention. |
| * Oral Thrush Treatment | $20 - $50 (antifungal medication) | Often covered | Prescription antifungal medication (e.g., Nystatin) to treat yeast infections common with dry mouth. |
| Sleep Apnea Diagnosis (Sleep Study) | $500 - $3,000+ | Often covered | If sleep apnea is suspected as a cause. In-lab studies are more expensive than home sleep tests. Medical insurance typically covers this. |
| CPAP Machine (for Sleep Apnea) | $500 - $2,500 | Often 80-100% covered | One-time purchase for treating sleep apnea; medical insurance usually covers a significant portion after deductible. Accessories like humidifiers and masks have ongoing costs. |
| Oral Appliance (for Sleep Apnea) | $1,800 - $3,500 | Often 80-100% covered | Custom-fitted appliance by a dentist, covered by medical insurance for OSA treatment. |
Insurance Coverage Details
- Dental Insurance:
- Typically covers preventive care (exams, cleanings, fluoride treatments) at a high percentage (80-100%). Given the increased risk of decay, more frequent cleanings might be covered, but check your plan's limits.
- Covers restorative procedures like fillings at 50-80%, after a deductible.
- Diagnostic tests like salivary flow tests may be covered if deemed medically necessary by your dentist.
- Most dental plans do not cover prescription medications, which fall under medical insurance.
- Medical Insurance:
- Often covers prescription medications like pilocarpine or cevimeline, especially for conditions like Sjögren's Syndrome, though deductibles and co-pays will apply.
- Covers diagnostic tests (blood work, specialist referrals) related to underlying medical conditions causing dry mouth.
- Plays a crucial role if dry mouth is linked to conditions like sleep apnea (covering sleep studies, CPAP machines, or oral appliances).
Cost-Saving Tips
- Generic Medications: Always ask your doctor if a generic version of a prescribed medication is available. Generics are significantly cheaper.
- Manufacturer Coupons/Patient Assistance Programs: For brand-name prescription drugs, check the manufacturer's website for coupons or patient assistance programs.
- Shop Around: Prices for OTC products and even some dental procedures can vary between pharmacies and dental offices.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): Use pre-tax dollars from an HSA or FSA to pay for qualified medical and dental expenses, including OTC dry mouth products and deductibles.
- Payment Plans: Many dental offices offer in-house payment plans for more expensive treatments like fillings or gum disease therapy.
- Community Health Clinics/Dental Schools: These often provide services at a reduced cost.
- Preventive Care: Adhering to strict oral hygiene and regular dental check-ups can prevent costly complications like extensive decay or gum disease down the line.
Recovery and Aftercare: Long-Term Management
Managing dry mouth at night is often an ongoing process, especially if it's due to chronic medical conditions or unavoidable medications. Long-term management focuses on sustained relief, preventing complications, and maintaining optimal oral and general health.
Sustained Symptom Relief
- Consistent Use of Products: Continue using prescribed medications (pilocarpine, cevimeline) and recommended OTC products (saliva substitutes, gels) as directed. Consistency is paramount for sustained relief, particularly before bed.
- Hydration Habits: Make frequent water intake a lifelong habit. Carry a water bottle and sip regularly throughout the day.
- Environmental Control: Continue using a bedroom humidifier, especially during dry seasons or if you sleep with your mouth open.
- Dietary Awareness: Permanently limit or avoid dehydrating beverages (excess caffeine, alcohol) and foods that irritate a dry mouth (spicy, salty, acidic).
Preventing Complications
- Rigorous Oral Hygiene: This is perhaps the most critical aspect of aftercare. With reduced saliva, your teeth are highly vulnerable to decay, and your gums are prone to inflammation and infection.
- Brush at least twice a day with a fluoride toothpaste (preferably prescription-strength).
- Floss daily.
- Use an antibacterial, alcohol-free mouthwash recommended by your dentist.
- Consider interdental brushes or water flossers for thorough cleaning.
- Regular Dental Check-ups: Schedule more frequent visits with your dentist, typically every 3-6 months. These appointments allow your dentist to:
- Monitor for new cavities or gum disease.
- Apply professional fluoride treatments.
- Clean your teeth thoroughly.
- Assess the effectiveness of your dry mouth management plan and make adjustments.
- Monitor for Infections: Be vigilant for signs of oral thrush (white patches, soreness) or other infections. Report them to your dentist immediately for prompt treatment.
Ongoing Medical Management
- Regular Doctor Visits: Continue seeing your physician to manage any underlying medical conditions (diabetes, Sjögren's, sleep apnea) that contribute to dry mouth.
- Medication Review: Periodically review your medication list with both your doctor and dentist. As new medications become available or your health status changes, there may be opportunities to adjust prescriptions to minimize dry mouth side effects.
- Specialist Follow-up: If you're under the care of a specialist (e.g., rheumatologist for Sjögren's, ENT for nasal issues), maintain those follow-up appointments.
Pro Tip: Consider keeping a "dry mouth journal" to track which products or habits provide the most relief, note any new symptoms, or identify potential triggers. This information can be invaluable for your dentist and doctor in fine-tuning your management plan.
Prevention of Dry Mouth at Night
Preventing dry mouth at night involves a combination of healthy habits and proactive measures, especially if you are prone to the condition or are aware of specific risk factors.
- Stay Hydrated Throughout the Day:
- Drink plenty of water consistently. Aim for at least eight 8-ounce glasses daily, more if you are active or in a hot climate.
- Sip water frequently, don't wait until you're thirsty. Keep a water bottle accessible.
- Optimize Bedroom Environment:
- Use a cool-mist humidifier in your bedroom. This adds moisture to the air, reducing evaporation from your mouth and throat, especially if you tend to breathe through your mouth.
- Keep your bedroom temperature comfortable, not too warm or dry.
- Practice Nasal Breathing:
- Consciously try to breathe through your nose during the day.
- If you habitually mouth breathe at night, try strategies like sleeping on your side or using nasal strips.
- Address underlying issues like nasal congestion (allergies, colds) or structural problems (deviated septum) with an ENT specialist.
- Avoid Dry Mouth Triggers:
- Limit Caffeine and Alcohol: These are diuretics and can lead to dehydration. Reduce intake, especially in the hours before bed.
- Quit Tobacco: All forms of tobacco (cigarettes, cigars, smokeless tobacco) severely reduce saliva flow and are detrimental to oral health.
- Reduce Sugary and Acidic Foods/Drinks: These exacerbate the risk of decay when saliva protection is low.
- Avoid Very Dry, Salty, or Spicy Foods: These can further irritate a dry mouth.
- Maintain Excellent Oral Hygiene:
- Brush your teeth twice daily with a fluoride toothpaste.
- Floss daily.
- Use an alcohol-free mouthwash.
- Regular dental check-ups (every 6 months or more frequently if advised) for professional cleanings and early detection of issues.
- Manage Medications and Health Conditions:
- Regularly review your medications with your doctor and dentist. If a medication is causing dry mouth, ask about alternative drugs or dosage adjustments.
- Effectively manage chronic medical conditions like diabetes or autoimmune diseases, as their control can impact saliva production.
- Stimulate Saliva Naturally:
- Chew sugar-free gum or suck on sugar-free candies (preferably with xylitol) to stimulate saliva flow. Do this throughout the day, not just before bed.
- Pro Tip: For persistent dry mouth, your dentist may recommend specific products like oral moisturizers or saliva substitutes for prophylactic use, even before symptoms become severe.
Risks and Complications of Untreated Dry Mouth at Night
While the immediate discomfort of dry mouth at night is significant, the long-term risks and complications of untreated xerostomia are far more serious, directly impacting oral health and potentially systemic well-being.
- Rampant Tooth Decay (Cavities): This is the most prevalent and damaging complication. Saliva neutralizes acids, washes away food particles, and contains minerals for remineralization. Without it, teeth are left defenseless against acid attacks, leading to rapid, widespread decay, often at the gumline and around existing fillings. This can necessitate extensive dental work, including multiple fillings, crowns, root canals, or even extractions.
- Gum Disease (Gingivitis and Periodontitis): Reduced saliva allows bacteria to proliferate and form plaque more aggressively. This leads to inflamed gums (gingivitis), which can progress to periodontitis, a severe infection that damages the soft tissue and bone supporting your teeth, potentially leading to tooth loss.
- Oral Infections: Saliva contains antimicrobial components. Without them, the mouth becomes a breeding ground for opportunistic infections.
- Oral Thrush (Candidiasis): A common fungal infection appearing as white patches on the tongue and inner cheeks, often accompanied by soreness and taste changes.
- Bacterial Infections: Increased risk of bacterial infections in the mouth and throat.
- Difficulty Eating and Swallowing (Dysphagia): Lack of lubrication makes chewing and swallowing food challenging and sometimes painful. This can lead to nutritional deficiencies, weight loss, and avoidance of certain foods.
- Difficulty Speaking (Dysphonia): A dry mouth and throat can make articulation difficult, leading to slurred speech or hoarseness.
- Bad Breath (Halitosis): As bacteria thrive in a dry environment, persistent and often severe bad breath is a common and embarrassing complication.
- Soreness and Cracking of Oral Tissues: The tongue, lips, and corners of the mouth can become dry, cracked, and painful.
- Denture Problems: For denture wearers, dry mouth can lead to poor retention, friction, soreness, and difficulty wearing dentures comfortably.
- Burning Mouth Syndrome: A persistent burning sensation in the mouth, often on the tongue, which can be exacerbated or caused by dry mouth.
- Reduced Quality of Life: The cumulative effect of these issues can significantly impact a person's comfort, confidence, social interactions, and overall quality of life.
Pro Tip: If you notice any of these complications, such as a sudden increase in cavities or persistent soreness, schedule an appointment with your dentist immediately. Early intervention is crucial to mitigate severe damage.
Children / Pediatric Considerations for Dry Mouth
While dry mouth at night is often associated with adults, children can also experience xerostomia, though the causes and presentation might differ. Recognizing and addressing dry mouth in children is critical, as their developing teeth are particularly vulnerable to decay.
Causes of Dry Mouth in Children:
- Mouth Breathing: This is a very common cause in children. It can be due to:
- Nasal Congestion: Allergies, colds, or chronic sinusitis.
- Enlarged Adenoids or Tonsils: These can physically block the nasal airway.
- Deviated Septum: A structural issue in the nose.
- Thumb Sucking/Pacifier Use: Can lead to an open-mouth posture.
- Sleep Apnea: Children can suffer from obstructive sleep apnea, leading to mouth breathing.
- Medications: Similar to adults, certain medications for allergies, ADHD, asthma, or depression can cause dry mouth.
- Dehydration: Children, especially infants and toddlers, can quickly become dehydrated, leading to dry mouth. This is common during illness with fever, vomiting, or diarrhea.
- Systemic Conditions: Less common but possible, conditions like juvenile diabetes or autoimmune disorders (e.g., juvenile Sjögren's Syndrome) can cause dry mouth.
- Cancer Treatment: Children undergoing head and neck radiation or chemotherapy can experience severe dry mouth.

Signs and Symptoms in Children:
Beyond the obvious dry lips and frequent thirst, look for:
- Difficulty eating dry foods: Kids may prefer soft, moist foods.
- Reluctance to talk: Or speech that sounds hoarse or sticky.
- Bad breath: Persistent halitosis.
- Increased cavities: Especially surprising new cavities or cavities progressing rapidly.
- Red, inflamed gums: Or frequent gum bleeding.
- Oral infections: White patches of oral thrush.
- Difficulty sleeping: Due to discomfort or mouth breathing.
Management and Prevention in Children:
- Hydration: Encourage frequent sips of water throughout the day. Keep water by their bedside.
- Address Mouth Breathing:
- Consult your pediatrician or an Ear, Nose, and Throat (ENT) specialist to identify and treat underlying causes like allergies, enlarged tonsils/adenoids, or nasal blockages.
- If sleep apnea is suspected, a sleep study may be recommended.
- Medication Review: Discuss any medications with your pediatrician to see if alternatives or dosage adjustments are possible.
- Sugar-Free Products:
- Offer sugar-free gum (for older children) or sugar-free lozenges/hard candies (xylitol-containing) to stimulate saliva.
- Avoid anything with sugar, as the risk of decay is significantly higher with dry mouth.
- Strict Oral Hygiene:
- Ensure consistent brushing (twice daily) and flossing (daily).
- Use fluoride toothpaste appropriate for their age.
- Pediatric Dentist Guidance: Regular visits to a pediatric dentist are essential. They can monitor for decay, apply fluoride varnishes, and recommend specific dry mouth products safe for children.
- Humidifier: Use a cool-mist humidifier in their bedroom.
- Limit Sugary/Acidic Foods: Avoid juice, soda, and excessive sugary snacks, especially before bed.
- Saliva Substitutes: For severe cases, your pediatric dentist may recommend child-friendly saliva substitutes or oral moisturizers. Always consult a professional before using these products on children.
Pro Tip for Parents: If your child consistently wakes up with a dry mouth, snores, or frequently breathes through their mouth, do not delay in consulting their pediatrician or a pediatric dentist. Early intervention is crucial to protect their developing oral health and address potential systemic issues.
Frequently Asked Questions
What is the main cause of dry mouth at night?
The most common cause of dry mouth at night is certain medications, with over 500 prescription and over-the-counter drugs listing dry mouth as a side effect. Other significant causes include mouth breathing during sleep (often due to nasal congestion or sleep apnea), dehydration, and systemic medical conditions like Sjögren's syndrome or diabetes.
Can dry mouth at night be a sign of something serious?
Yes, persistent dry mouth can be a symptom of serious underlying medical conditions such as Sjögren's syndrome, diabetes, or even neurological disorders. It can also be a significant indicator of obstructive sleep apnea. Furthermore, chronic dry mouth itself leads to severe oral health complications like rampant tooth decay and gum disease, which can impact overall health.
How can I get rid of dry mouth at night naturally?
Natural remedies include staying well-hydrated throughout the day, using a cool-mist humidifier in your bedroom, avoiding caffeine and alcohol before bed, and breathing through your nose (addressing nasal congestion if present). Chewing sugar-free gum or sucking on sugar-free lozenges (especially those with xylitol) can also stimulate saliva production.
What foods or drinks should I avoid if I have dry mouth?
You should avoid very dry, salty, or spicy foods that can further irritate a dry mouth. It's also wise to limit or avoid highly acidic drinks (like sodas and fruit juices), sugary snacks, caffeine, and alcohol, as these can either dehydrate you, irritate your oral tissues, or accelerate tooth decay in a dry mouth environment.
Are there any specific toothpastes or mouthwashes for dry mouth?
Yes, many brands offer toothpastes and mouthwashes specifically formulated for dry mouth. Look for products that are alcohol-free and contain ingredients like xylitol or fluoride. Your dentist may also recommend a prescription-strength fluoride toothpaste or gel to help protect your teeth from decay.
How much does dry mouth treatment cost?
Costs vary widely depending on the treatment. Over-the-counter saliva substitutes and gels typically cost $5-$25 per month. Prescription medications like pilocarpine or cevimeline can range from $30-$150 per month (often covered by medical insurance). Dental check-ups, cleanings, and any necessary treatments for complications like cavities will incur additional costs, usually partially covered by dental insurance.
Does insurance cover dry mouth treatments?
Dental insurance typically covers preventative care (exams, cleanings) and restorative treatments (fillings) for complications. Medical insurance often covers diagnostic tests for underlying conditions and prescription medications for dry mouth. Coverage for specific OTC dry mouth products is rare, but you can use HSA/FSA funds.
How long does it take for dry mouth treatment to work?
Relief from over-the-counter products like sprays and gels is often immediate but temporary. Prescription medications designed to stimulate saliva might take a few days to a few weeks to show their full effect. Consistent application of treatments and lifestyle changes is crucial for sustained, long-term improvement.
Can dry mouth cause a burning sensation in my mouth?
Yes, a persistent burning sensation in the mouth, often on the tongue, is a condition known as burning mouth syndrome, which can be caused or exacerbated by dry mouth. The lack of saliva leads to irritation and increased sensitivity of the oral tissues.
When should I see a dentist for dry mouth?
If your dry mouth is persistent, interferes with your sleep, eating, or speaking, or if you notice any associated complications like new cavities, gum inflammation, or oral infections (e.g., white patches), you should see a dentist promptly. They can help diagnose the cause and recommend appropriate treatment to prevent further damage.
When to See a Dentist
While occasional dry mouth might be a temporary inconvenience, persistent dry mouth at night warrants professional attention. Knowing when to consult a dentist or physician is crucial for protecting your oral health and addressing potential underlying medical conditions.
You should schedule a routine appointment with your dentist if you experience:
- Chronic dry mouth symptoms: If your dry mouth lasts for several weeks or months, even after trying basic home remedies like increasing water intake.
- Worsening symptoms: If your dry mouth is becoming more severe, impacting your sleep, ability to eat, or speak clearly.
- Difficulty wearing dentures: If your dentures become uncomfortable or slip due to lack of moisture.
- Concerns about medication side effects: If you suspect a medication is causing your dry mouth, your dentist can advise you on discussing alternatives with your prescribing doctor.
You should seek more urgent dental or medical attention (within a few days) if you notice:
- Rapid increase in cavities: Especially new cavities forming quickly or around the gumline, which is a hallmark of dry mouth-related decay.
- Signs of gum disease: Bleeding gums, swollen gums, or persistent bad breath that doesn't improve with regular brushing.
- Oral infections: White patches on your tongue or inner cheeks (suggestive of oral thrush), or any persistent sores or unusual lesions in your mouth.
- Significant difficulty swallowing or eating: Leading to weight loss or nutritional concerns.
- Unexplained hoarseness or persistent sore throat: These can be related to chronic dryness and irritation.
Consider seeking immediate medical attention or emergency care if:
- Sudden onset of severe dry mouth accompanied by other acute symptoms: Such as fever, severe pain, or difficulty breathing, as this could indicate a serious systemic issue or infection.
- You suspect severe dehydration: With symptoms like extreme thirst, infrequent urination, dizziness, or confusion.
Your dentist is often the first point of contact for dry mouth, as they can assess your oral health directly, perform salivary flow tests, and guide you on initial management. They can also refer you to a medical doctor or specialist if an underlying systemic cause is suspected. Delaying treatment for chronic dry mouth can lead to irreversible damage to your teeth and gums, making early intervention vital.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026