Dry Mouth With Cpap: Complete Guide
Key Takeaways
- When you commit to using a Continuous Positive Airway Pressure (CPAP) machine, a life-changing treatment for sleep apnea, you anticipate better sleep and improved health. However, many individuals quickly discover an unwelcome side effect: dry mouth with CPAP. This isn't just an annoyance; it ca
When you commit to using a Continuous Positive Airway Pressure (CPAP) machine, a life-changing treatment for sleep apnea, you anticipate better sleep and improved health. However, many individuals quickly discover an unwelcome side effect: dry mouth with CPAP. This isn't just an annoyance; it can significantly impact your comfort, adherence to therapy, and overall oral health. In fact, studies suggest that up to 40-60% of CPAP users experience dry mouth, a condition known medically as xerostomia, which can lead to a cascade of dental problems if left unaddressed. Understanding why this happens, what signs to look for, and the comprehensive solutions available is crucial for maintaining your health and ensuring your CPAP therapy remains effective.
This in-depth guide from SmilePedia.net will explore the intricate relationship between CPAP use and dry mouth. We'll delve into the underlying causes, common symptoms, and a wide array of effective strategies and treatments, including the role of humidifiers, proper mask fit, and even alternative solutions like mouth guards for sleep apnea. Our goal is to equip you with the knowledge and practical advice to overcome this common challenge, improve your CPAP adherence, and safeguard your dental well-being.
Key Takeaways:
- Prevalence: Dry mouth affects 40-60% of CPAP users, significantly impacting comfort and therapy adherence.
- Primary Causes: Mouth breathing (often due to an ill-fitting mask or nasal congestion), insufficient humidification, and certain medications are common culprits.
- Key Solutions: Optimizing CPAP humidifier settings (often an integrated feature), ensuring a proper mask seal, and addressing nasal congestion are first-line strategies.
- Oral Appliances: Custom mouth guards for sleep apnea (oral appliance therapy) can be an effective alternative for mild to moderate cases, eliminating CPAP-related dry mouth, with costs ranging from $1,800 to $5,000.
- Mouth Taping: For persistent mouth breathing, gentle mouth taping can encourage nasal breathing, costing as little as $5-$20 for a roll of medical tape.
- Oral Health Impact: Chronic dry mouth increases risks for cavities, gum disease, and oral infections; regular dental check-ups are essential.
- Treatment Timeline: Adjustments to CPAP settings or mask types can offer relief within days to weeks, while dental oral appliances may take 4-8 weeks from consultation to final fitting.
What It Is: Understanding Dry Mouth with CPAP
Dry mouth, or xerostomia, is the subjective sensation of dryness in the mouth, often caused by a reduction in saliva flow. When experienced specifically in conjunction with Continuous Positive Airway Pressure (CPAP) therapy, it arises from the unique mechanics of the treatment. CPAP machines deliver a continuous stream of pressurized air through a mask worn over the nose or mouth during sleep. While this air keeps the airway open and prevents apneic events, it can also have a drying effect on the delicate mucous membranes of the mouth and throat.
The purpose of saliva is far more than just keeping your mouth moist; it plays a critical role in digestion, taste, speaking, and most importantly, oral health. Saliva helps wash away food particles, neutralize acids produced by bacteria, and contains enzymes and antibodies that fight infection and prevent tooth decay. When salivary flow is reduced, the mouth's natural protective mechanisms are compromised, leading to a host of potential problems beyond mere discomfort.
For CPAP users, dry mouth is a common complaint that can range from mild morning dryness to severe discomfort, often leading to cracked lips, a sore throat, and difficulty swallowing. It's a significant barrier to consistent CPAP use, as many individuals find the discomfort intolerable enough to abandon their therapy, thereby negating the health benefits of treating their sleep apnea. Addressing dry mouth with CPAP is not just about comfort; it's about optimizing treatment adherence and protecting your long-term oral and systemic health.
Causes: Why Dry Mouth Happens with CPAP
Several factors can contribute to or exacerbate dry mouth while using a CPAP machine. Understanding these causes is the first step toward finding an effective solution.
1. Mouth Breathing
This is arguably the most common culprit. If you breathe through your mouth while using CPAP, the constant stream of pressurized air passing over your oral tissues can quickly evaporate saliva, leading to significant dryness.
- Improper Mask Fit: A mask that leaks, especially around the mouth or jaw, can allow air to escape and contribute to mouth breathing. Even a slight leak can be enough.
- Nasal Congestion: If your nose is blocked due to allergies, a cold, deviated septum, or chronic sinusitis, you'll naturally resort to mouth breathing, even with a nasal or nasal pillow CPAP mask. The brain prioritizes oxygen intake, forcing you to breathe through the path of least resistance.
- Open Mouth Sleeping: Some individuals are habitual mouth breathers during sleep, regardless of CPAP use. The CPAP air simply intensifies the drying effect.
2. Inadequate Humidification
Most modern CPAP machines come with an integrated heated humidifier, designed to add moisture to the pressurized air before it reaches your airway.
- Low Humidifier Settings: If the humidifier is set too low for your environment (e.g., dry climate, winter, or air-conditioned room), the air may still be too dry.
- No Humidifier Used: Some older CPAP models or travel CPAPs may not include a humidifier, or users might opt not to use it, especially if they are unaware of its importance.
- Empty Water Chamber: For humidifiers to work, they need distilled water. Forgetting to fill the chamber or letting it run dry can render it ineffective.
3. Mask Type
The type of CPAP mask you use can influence dry mouth.
- Nasal Masks/Pillows: If you use a nasal mask or nasal pillows, but habitually open your mouth during sleep, the air can escape through your mouth, leading to dryness. This is often referred to as "mouth leak."
- Full Face Masks: While full face masks cover both the nose and mouth, making them ideal for mouth breathers, they can still contribute to dryness if the mask seal is poor, or if humidification is insufficient. The larger surface area exposed to the air stream might also play a role if not properly humidified.
4. Medications
Various prescription and over-the-counter medications can cause dry mouth as a side effect, regardless of CPAP use. Common culprits include:
- Antihistamines
- Decongestants
- Antidepressants
- Antianxiety medications
- Blood pressure medications
- Muscle relaxants
If you're taking any of these, CPAP therapy might exacerbate an existing dry mouth condition.
5. Medical Conditions
Certain medical conditions can reduce saliva production:
- Sjögren's Syndrome: An autoimmune disorder characterized by dry eyes and dry mouth.
- Diabetes: Poorly controlled diabetes can affect salivary glands.
- Radiation Therapy: Head and neck radiation can permanently damage salivary glands.
- Nerve Damage: Damage to nerves that stimulate salivary glands.
6. Lifestyle Factors
- Dehydration: Not drinking enough water throughout the day.
- Alcohol and Caffeine: These can have diuretic effects, contributing to overall dehydration.
- Smoking: Tobacco use can irritate oral tissues and reduce saliva flow.
Signs and Symptoms of Dry Mouth with CPAP
Recognizing the symptoms of dry mouth is important, not just for comfort but for alerting you to potential oral health issues.
- Waking up with a dry, sticky, or parched feeling in your mouth and throat: This is the most obvious sign.
- Difficulty swallowing, chewing, or speaking: A lack of saliva makes these basic functions challenging.
- Sore throat or hoarseness: The constant dryness can irritate the throat.
- Cracked lips or corners of the mouth (cheilosis): Dryness can lead to skin breakdown.
- Bad breath (halitosis): Saliva helps wash away odor-causing bacteria; without it, bacteria can proliferate.
- Changes in taste sensation: Food may taste different or bland.
- Increased thirst: A natural response to dryness.
- Red, raw, or fissured tongue: The tongue may appear dry and less smooth.
- Increased incidence of cavities (dental caries): This is a serious long-term consequence as saliva's protective effects are diminished.
- Gum inflammation (gingivitis) or gum disease (periodontitis): Lack of saliva allows bacteria to thrive, increasing the risk of gum problems.
- Oral infections: Fungal infections, like oral thrush (candidiasis), are more common in dry mouths.
If you experience these symptoms, especially if they are persistent or worsening, it's crucial to investigate the underlying cause and seek appropriate treatment.
Treatment Options for Dry Mouth with CPAP
Addressing dry mouth while using CPAP often involves a multi-pronged approach, targeting the specific causes.
1. Optimizing CPAP Equipment and Settings
- Heated Humidifier:
- Increase Settings: Gradually increase the humidity level on your CPAP machine. Most machines allow you to adjust both the humidity level and the heated tubing temperature. Experiment to find a comfortable balance.
- Use Distilled Water: Always use distilled water in your humidifier to prevent mineral buildup and bacterial growth.
- Check Water Chamber: Ensure the water chamber is filled before bed and doesn't run dry overnight.
- Pro Tip: In very dry climates or during winter, you might need a higher humidity setting than in more temperate conditions.
- Heated Tubing: Many modern CPAP machines offer heated tubing, which prevents condensation (rainout) in the hose and ensures the humidified air reaches your mask at the desired temperature. This is essential for effective humidification, especially at higher settings.
- Mask Fit and Type:
- Check for Leaks: Perform a mask leak test before bed. A poorly fitting mask allows air to escape, contributing to dryness. Adjust straps, try different cushion sizes, or consult your CPAP provider for a re-fitting.
- Consider a Full Face Mask: If you're a chronic mouth breather or experience significant mouth leaks with a nasal mask, a full face mask (covering both nose and mouth) might be a better option as it delivers air directly to both airways.
- Chinstrap: For those using nasal masks who find their mouth opens during sleep, a chinstrap can help keep the jaw closed, encouraging nasal breathing. This simple device can be very effective in preventing "mouth leak" from a nasal mask.
2. Addressing Nasal Congestion
If you struggle with nasal breathing, resolving nasal issues is paramount.
- Nasal Sprays/Rinses: Saline nasal sprays or rinses (like a neti pot) can clear congestion before bed.
- Decongestants: Over-the-counter decongestants can provide temporary relief, but prolonged use can cause rebound congestion. Consult your doctor for long-term solutions.
- Allergy Management: If allergies are the cause, antihistamines or nasal corticosteroids prescribed by a doctor can help manage symptoms.
- Medical Evaluation: For persistent congestion, a visit to an Ear, Nose, and Throat (ENT) specialist may be necessary to rule out structural issues (e.g., deviated septum, polyps) that might require surgical correction.
3. Oral Solutions and Habits
- Oral Moisturizers: Over-the-counter products like oral gels, sprays, or rinses designed for dry mouth can provide temporary relief. Look for products containing xylitol.
- Xylitol Products: Xylitol-sweetened gums, lozenges, or mints can stimulate saliva flow and help prevent cavities. Chew gum for 5-10 minutes before bed.
- Hydration: Drink plenty of water throughout the day. Keep a glass of water by your bedside.
- Avoid Irritants: Limit caffeine, alcohol, and tobacco, as these can exacerbate dry mouth.
- Proper Oral Hygiene: Regular brushing (twice daily) and flossing (once daily) are even more critical when experiencing dry mouth to prevent cavities and gum disease. Use fluoride toothpaste. The American Dental Association (ADA) strongly recommends fluoride for cavity prevention.
- Mouth Taping: For persistent mouth breathing, particularly with nasal masks, gently taping your mouth closed can encourage nasal breathing. Use a small piece of porous medical tape or specially designed sleep tape (available from $5 to $20 for a roll/pack). This should only be attempted if your nasal passages are clear. Pro Tip: Start with a small piece of tape vertically over the center of your lips to get used to it. Ensure you can easily remove it if needed.
4. Alternative Sleep Apnea Treatments
While CPAP is highly effective, if dry mouth severely impacts your adherence, discussing alternatives with your sleep specialist is vital.
- Oral Appliance Therapy (OAT): Custom-made mouth guards for sleep apnea are devices worn in the mouth during sleep. They work by gently repositioning the jaw and/or tongue to keep the airway open. OAT is primarily recommended for mild to moderate obstructive sleep apnea (OSA) or for those who cannot tolerate CPAP.
- Pros: Highly effective for many, portable, no dry air issues, can significantly improve sleep quality without CPAP side effects.
- Cons: Not suitable for severe OSA or central sleep apnea, can cause jaw discomfort or changes in bite over time (usually reversible), requires custom fitting by a qualified dentist specializing in sleep medicine.
- Cost: The cost for a custom oral appliance typically ranges from $1,800 to $5,000 in the US, depending on the type of appliance, complexity, and geographic location. Insurance often covers a portion if diagnosed with OSA.
- Positional Therapy: For individuals whose apnea is worse when sleeping on their back, devices that encourage side sleeping can be helpful.
- Surgical Options: In some cases, surgical procedures (e.g., uvulopalatopharyngoplasty (UPPP), genial advancement, nasal surgery) can address anatomical obstructions, but these are generally considered after other treatments have failed.
- Weight Loss: For overweight or obese individuals, significant weight loss can reduce the severity of OSA, and in some cases, resolve it entirely.
Comparison of Dry Mouth Solutions with CPAP
| Solution / Approach | Mechanism | Pros | Cons | Estimated Cost (US) |
|---|---|---|---|---|
| CPAP Humidifier Optimization | Adds moisture to CPAP air | Immediate relief, integrated, no additional devices | May require trial & error, water chamber refills | Included with CPAP machine, distilled water ($1-$2/gallon) |
| Mask Fit/Type Adjustment | Prevents air leaks, enables nasal breathing | Directly addresses common cause, part of existing therapy | May require multiple mask trials, can be frustrating | New mask cushions ($30-$100), new mask ($100-$300) |
| Chinstrap | Keeps mouth closed with nasal mask | Simple, inexpensive, effective for mouth breathers | Can be uncomfortable, may not work for all | $15-$40 |
| Mouth Taping | Encourages nasal breathing, reduces mouth leak | Very inexpensive, simple | Requires clear nasal passages, can be unusual feeling | Medical tape ($5-$20/roll) |
| Nasal Care (Sprays/Rinses) | Clears nasal passages for better airflow | Reduces reliance on mouth breathing | Temporary relief, consistent use needed | Saline spray ($10-$20), Neti Pot ($15-$30) |
| Oral Appliances (Mouth Guards for Sleep Apnea) | Repositions jaw to open airway (alternative to CPAP) | No CPAP-related dry mouth, portable, comfortable | Not for severe OSA, potential jaw discomfort, custom fit required | $1,800 - $5,000 (dental consults may be separate) |
| Xylitol Products | Stimulates saliva, fights bacteria | Natural, accessible, also prevents cavities | Temporary relief, not a primary solution | Gum/lozenges ($5-$15/pack) |
| Oral Moisturizers | Provides temporary moisture | Immediate comfort, easy to use | Temporary, doesn't address underlying cause | Gels/sprays ($10-$30) |
Step-by-Step Process for Addressing Dry Mouth with CPAP
-
Assess Your Current Situation:
- Identify Symptoms: When do you experience dry mouth? How severe is it?
- Check Your Mask: Does your mask fit snugly without being too tight? Do you notice air leaks?
- Humidifier Status: Is your humidifier full of distilled water? What are its current settings (humidity level, heated tube temperature)?
- Nasal Patency: Can you comfortably breathe through your nose with your mouth closed, both awake and before sleep?
- Medication Review: Are you taking any medications known to cause dry mouth? Discuss this with your doctor.
-
Initial Adjustments (First 1-2 Weeks):
- Optimize Humidifier: Gradually increase your CPAP machine's humidifier setting. If you have heated tubing, ensure it's on and adjust its temperature as well.
- Mask Check and Adjustment: Re-fit your mask. If you suspect leaks, try tightening straps slightly, or consider a different cushion size. Watch online tutorials for proper mask fitting for your specific model.
- Nasal Hygiene: Incorporate saline nasal rinses or sprays into your bedtime routine to clear nasal passages.
-
Intermediate Strategies (If Dry Mouth Persists, Weeks 2-4):
- Consider a Chinstrap: If using a nasal mask and you mouth breathe, a chinstrap can help keep your mouth closed.
- Try Mouth Taping: If nasal breathing is clear and consistent, carefully try medical mouth tape to encourage nasal breathing.
- Explore Oral Moisturizers/Xylitol: Use over-the-counter dry mouth products for symptomatic relief.
- Review Mask Type: If you're using a nasal mask and still experiencing significant mouth leaks or mouth breathing despite other efforts, consider trying a full face mask. Consult your sleep specialist or CPAP supplier for advice on trying different mask types.
-
Professional Consultation (If Symptoms Remain, After 4 Weeks):
- Consult Your Sleep Doctor: Discuss persistent dry mouth. They can review your CPAP data (mask leaks, AHI), rule out other medical conditions, and advise on medication adjustments or advanced CPAP settings.
- Visit Your Dentist: Inform your dentist about your CPAP use and dry mouth. They can assess your oral health for signs of decay or gum disease and recommend professional fluoride treatments or prescription dry mouth remedies. If CPAP intolerance is high due to dry mouth, discuss mouth guards for sleep apnea (oral appliance therapy) as an alternative with a dentist specializing in sleep medicine.
- Consider an ENT Specialist: If chronic nasal congestion is the primary issue, an ENT can diagnose and treat underlying conditions like a deviated septum or chronic sinusitis.
Cost and Insurance for Dry Mouth Solutions
The cost of addressing dry mouth with CPAP varies widely depending on the chosen solution, whether it's an adjustment to your existing therapy or an alternative treatment.
CPAP-Related Adjustments
- CPAP Humidifier & Heated Tubing: Usually included with the initial CPAP machine purchase. If bought separately, a humidifier attachment can range from $150-$300, and heated tubing from $50-$100.
- Mask Cushions/Seals: These need regular replacement every 1-3 months. Costs range from $30-$100 per cushion/seal.
- New CPAP Mask: A complete new mask can cost between $100-$300.
- Chinstrap: Inexpensive, typically $15-$40.
- Mouth Tape: Very low cost, $5-$20 for a roll or pack.
- Distilled Water: About $1-$2 per gallon, used nightly for humidifiers.
Insurance Coverage: Most health insurance plans, including Medicare and private plans, typically cover CPAP machines and replacement supplies (masks, tubing, cushions) as Durable Medical Equipment (DME) if medically necessary and prescribed for sleep apnea. You'll likely pay a deductible and co-insurance (e.g., 20% of the cost) until you meet your out-of-pocket maximum. Some plans might require you to rent the machine for a period before owning it. Always verify coverage with your specific provider.
Dental and Medical Solutions
- Oral Appliances (Mouth Guards for Sleep Apnea):
- Consultation with a Sleep Dentist: Initial consultation may range from $150-$350.
- Custom Oral Appliance: The appliance itself typically costs between $1,800 and $5,000. This includes impressions, custom fabrication, multiple fitting appointments, and follow-up adjustments.
- Insurance Coverage: Many medical insurance plans, recognizing OSA as a medical condition, will cover a significant portion of oral appliance therapy if it's prescribed by a sleep physician and fabricated by a qualified dentist. Coverage is generally not under dental insurance but under medical insurance as DME. Medicare also covers oral appliances for OSA. You'll be responsible for deductibles and co-pays.
- Over-the-Counter Oral Moisturizers/Xylitol Products: $10-$30 per product, generally not covered by insurance.
- Prescription Dry Mouth Medications (e.g., pilocarpine, cevimeline): If medically necessary due to systemic conditions, these may be covered by prescription drug plans, with standard co-pays.
- ENT Specialist Consultation: $150-$500 depending on the complexity and if diagnostic procedures are performed. Covered by medical insurance, subject to deductibles and co-pays.
- Dental Check-ups and Fluoride Treatments: Routine dental check-ups are typically covered by dental insurance with co-pays. Professional fluoride treatments range from $30-$70 and may or may not be covered depending on the plan.
Cost-Saving Tips
- Verify Insurance: Always contact your medical and dental insurance providers directly to understand your specific benefits, deductibles, co-pays, and approved durable medical equipment (DME) suppliers.
- Shop Around for Supplies: For CPAP accessories not covered, compare prices from different DME providers or online retailers.
- Manufacturer Coupons: Check for coupons or patient assistance programs for prescription medications.
- Dental School Clinics: For oral appliance therapy, some university dental school clinics offer services at a reduced cost, often with highly experienced supervising faculty.
- Payment Plans: Many dental offices and medical providers offer in-house payment plans or work with third-party financing options like CareCredit.
Recovery and Aftercare for Dry Mouth with CPAP
Addressing dry mouth isn't a one-time fix; it often requires ongoing management and vigilance.
- Consistent Hydration: Make a habit of drinking water throughout the day, not just before bed.
- Oral Hygiene: Maintain exemplary oral hygiene. Brush twice daily with a fluoride toothpaste, floss daily, and consider an antimicrobial mouthwash (alcohol-free). The ADA emphasizes fluoride's role in strengthening enamel, which is especially important with reduced saliva.
- Regular Dental Check-ups: Schedule more frequent dental visits (e.g., every 4-6 months instead of 6-12 months) if dry mouth is severe or persistent. Your dentist can monitor for cavities, gum disease, and provide professional fluoride applications.
- CPAP Maintenance: Regularly clean your CPAP mask, tubing, and humidifier water chamber to prevent bacterial growth and ensure optimal performance. Replace supplies as recommended by the manufacturer.
- Monitor Symptoms: Pay attention to your symptoms. If dry mouth returns or worsens, re-evaluate your CPAP settings, mask fit, and general health habits.
- Follow-up with Specialists: If you've sought help from a sleep doctor, ENT, or sleep dentist, adhere to their follow-up schedules to ensure treatments are effective and to address any new concerns.
Prevention of Dry Mouth with CPAP
Proactive measures can significantly reduce the likelihood and severity of dry mouth with CPAP.
- Optimal Humidification from Day One: Don't wait for dry mouth to start. Begin CPAP therapy with the heated humidifier engaged and adjust settings as needed for comfort, especially in dry environments.
- Ensure Proper Mask Fit: Work closely with your CPAP provider to find a mask that fits perfectly and creates a good seal from the start. A proper fit not only prevents dry mouth but also improves overall CPAP effectiveness.
- Address Nasal Issues Proactively: If you have chronic allergies or congestion, seek treatment before starting CPAP, or at least concurrently. Regular use of saline rinses can also be a good preventive measure.
- Stay Hydrated: Develop a habit of consistent water intake throughout the day.
- Good Oral Hygiene: Maintain excellent oral health habits, including regular brushing, flossing, and dental check-ups, to bolster your mouth's natural defenses.
- Regular CPAP Maintenance: Clean your equipment diligently and replace parts (masks, filters, tubing) according to manufacturer guidelines to ensure optimal performance and hygiene.
- Review Medications: Discuss potential dry mouth side effects with your doctor when starting new medications.
- Consider Early Intervention for Mouth Breathing: If you know you are a mouth breather during sleep, discuss solutions like a chinstrap or even gentle mouth taping with your sleep specialist or CPAP provider early on, especially if you're using a nasal mask.
Risks and Complications of Untreated Dry Mouth
Ignoring persistent dry mouth, whether or not it's related to CPAP, carries significant risks, particularly for your oral health.
- Increased Risk of Dental Caries (Cavities): Saliva is your mouth's natural defense against acid attacks and decay. Without adequate saliva, teeth are much more vulnerable to cavities, which can progress rapidly. This is a primary concern highlighted by the ADA for individuals with xerostomia.
- Gum Disease (Gingivitis and Periodontitis): Reduced saliva allows plaque and bacteria to accumulate more easily, leading to inflammation of the gums (gingivitis) and, if untreated, more severe gum disease (periodontitis), which can result in tooth loss.
- Oral Infections: Saliva contains antimicrobial properties. A dry mouth is a breeding ground for bacteria and fungi. Oral thrush (candidiasis) is a common fungal infection that thrives in dry oral environments.
- Difficulty Eating and Speaking: Chronic dryness can make chewing, swallowing, and speaking comfortably very challenging, impacting quality of life.
- Bad Breath (Halitosis): Without saliva to wash away food particles and bacteria, foul odors can develop.
- Sore Throat and Hoarseness: Persistent dryness and irritation of the throat tissues.
- Reduced CPAP Adherence: Perhaps the most critical complication in the context of sleep apnea is the abandonment of CPAP therapy due to discomfort, leading to untreated sleep apnea and its associated health risks (cardiovascular disease, stroke, diabetes, accidents).
- Tooth Sensitivity: Exposed dentin due to gum recession or enamel erosion can lead to increased tooth sensitivity.
- Changes in Taste: The ability to taste can be diminished or altered.
Children / Pediatric Considerations
Sleep apnea can affect children, and some may require CPAP therapy. While dry mouth is less commonly discussed as a primary concern in pediatric CPAP users compared to adults, it is still a potential side effect and warrants attention.
- Causes in Children: Similar to adults, mouth breathing (often due to enlarged tonsils and adenoids, allergies, or nasal obstruction) and inadequate humidification are key causes. Pediatric masks and settings must be carefully chosen and adjusted.
- Symptoms in Children: Children may not articulate dry mouth as clearly as adults. Look for signs like increased thirst, frequent waking for water, chapped lips, difficulty eating certain foods, or increased fussiness around brushing teeth.
- Oral Health Impact: Children's teeth are still developing, and the protective role of saliva is crucial. Chronic dry mouth can accelerate tooth decay, especially in developing primary (baby) teeth and newly erupted permanent teeth.
- Treatment Approach:
- Prioritize Nasal Breathing: For children, addressing the root cause of nasal obstruction is often paramount. This may involve allergy management or, frequently, adenotonsillectomy (removal of tonsils and adenoids), which can often resolve pediatric OSA and negate the need for CPAP.
- Proper Mask Fit: Pediatric CPAP masks are specifically designed for smaller faces and require careful fitting by a pediatric sleep specialist or CPAP technician to ensure a good seal and prevent leaks.
- Humidification: Ensure the CPAP's heated humidifier is used and adjusted to appropriate levels for the child's comfort and environment.
- Oral Hygiene: Emphasize excellent oral hygiene with fluoride toothpaste and regular dental check-ups. Pediatric dentists can offer fluoride varnishes and sealants as preventive measures.
- Xylitol: Xylitol-containing products (sugar-free gum for older children, xylitol lollipops or rinses for younger ones) can be beneficial, always under parental supervision.
- Mouth Guards for Sleep Apnea (Pediatric): While oral appliances are generally used for adults, specific orthodontic appliances can sometimes be used in children to expand the palate or advance the jaw, addressing anatomical issues contributing to OSA. These are typically managed by a pediatric orthodontist or sleep dentist. Mouth tape is generally not recommended for children due to potential safety concerns and difficulty in communication regarding discomfort or breathing issues.
- Parental Role: Parents play a critical role in monitoring their child's CPAP use, observing for signs of dry mouth, ensuring proper hygiene, and communicating regularly with their child's sleep specialist and pediatric dentist.
Frequently Asked Questions
What does "dry mouth with CPAP" feel like?
You might wake up with a parched or sticky feeling in your mouth, a scratchy or sore throat, or a persistent urge to drink water. Your lips may feel chapped, and you might notice difficulty speaking or swallowing easily.
Can dry mouth from CPAP lead to cavities?
Yes, absolutely. Saliva is your mouth's natural defense against tooth decay by neutralizing acids and washing away food particles. When dry mouth reduces saliva flow, your teeth are much more vulnerable to cavities, gum disease, and other oral infections.
Is it normal to get dry mouth when I first start CPAP therapy?
It can be common, especially as you adjust to the machine and mask. However, it's not something you should simply tolerate. Persistent dry mouth indicates an issue with your CPAP setup, mask fit, or an underlying medical condition that needs to be addressed.
What's the difference between a nasal mask and a full face mask for dry mouth?
A nasal mask covers only your nose. If you open your mouth during sleep while using a nasal mask, air can escape, causing dry mouth. A full face mask covers both your nose and mouth, making it suitable for mouth breathers, but still requires proper humidification and a good seal to prevent dryness.
Does mouth tape help with sleep apnea itself, or just dry mouth?
Mouth tape primarily helps with dry mouth by encouraging nasal breathing and preventing mouth leaks from nasal CPAP masks. While proper nasal breathing is beneficial, mouth tape is not a direct treatment for sleep apnea; it's a complementary strategy to improve CPAP adherence and comfort. It should only be used if your nasal passages are clear.
How much do mouth guards for sleep apnea cost, and are they covered by insurance?
Custom oral appliances (mouth guards for sleep apnea) typically cost between $1,800 and $5,000 in the US. Many medical insurance plans, including Medicare, cover a significant portion of this cost as Durable Medical Equipment (DME) if prescribed by a sleep physician for diagnosed sleep apnea, rather than under dental insurance.
How long does it take for dry mouth to improve once I make changes?
Improvements can often be noticed within a few nights to a week after adjusting your humidifier settings, improving mask fit, or addressing nasal congestion. If you switch to an oral appliance, relief from CPAP-related dry mouth is usually immediate upon successful use. Persistent issues warrant a professional consultation.
Can switching to a different type of humidifier help?
Most modern CPAP machines have integrated heated humidifiers that are very effective. If you have an older machine without one, adding a heated humidifier is highly recommended. Ensure it is properly maintained with distilled water and settings are optimized.
Should I stop using my CPAP if I get dry mouth?
No, do not stop your CPAP therapy without consulting your sleep doctor. Untreated sleep apnea poses significant health risks. Instead, work with your CPAP provider, sleep specialist, and dentist to troubleshoot and resolve the dry mouth issue so you can continue to benefit from your prescribed therapy.
Are there any specific toothpastes or mouthwashes recommended for dry mouth?
Yes, look for toothpastes and mouthwashes specifically formulated for dry mouth (often labeled "for dry mouth relief"). These are typically alcohol-free and contain ingredients like xylitol or fluoride to help moisturize and protect your teeth. Your dentist may also recommend prescription-strength fluoride toothpaste.
When to See a Dentist or Doctor
While many dry mouth issues can be resolved with adjustments to your CPAP setup and home remedies, certain situations warrant professional medical or dental attention.
- Persistent Symptoms: If dry mouth symptoms persist for more than a few weeks despite trying various self-help strategies (humidifier adjustments, mask fit, nasal care).
- New or Worsening Oral Health Problems: If you notice new cavities, increased tooth sensitivity, bleeding gums, persistent bad breath, or any signs of oral infection (e.g., white patches on your tongue or cheeks, which could indicate thrush).
- Difficulty Adhering to CPAP: If dry mouth is severely impacting your ability to use your CPAP machine consistently, leading you to skip nights or remove the mask early. This indicates a need for your sleep specialist to review your therapy.
- Chronic Nasal Congestion: If you consistently struggle to breathe through your nose, even after using saline rinses or over-the-counter decongestants, consult an Ear, Nose, and Throat (ENT) specialist.
- Suspected Medical Condition: If you have other symptoms that suggest an underlying medical condition might be contributing to your dry mouth (e.g., changes in vision, joint pain, unexplained fatigue), discuss this with your primary care physician.
- Considering Alternatives to CPAP: If CPAP intolerance (due to dry mouth or other issues) is high, schedule an appointment with your sleep physician to discuss alternative treatment options like mouth guards for sleep apnea (oral appliance therapy) or surgical interventions. Your sleep physician can refer you to a qualified sleep dentist if appropriate.
Remember, early intervention can prevent minor discomfort from escalating into significant oral health problems or leading to the abandonment of crucial sleep apnea therapy. Your dental health is an integral part of your overall well-being, and addressing dry mouth promptly is a vital step in maintaining it.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
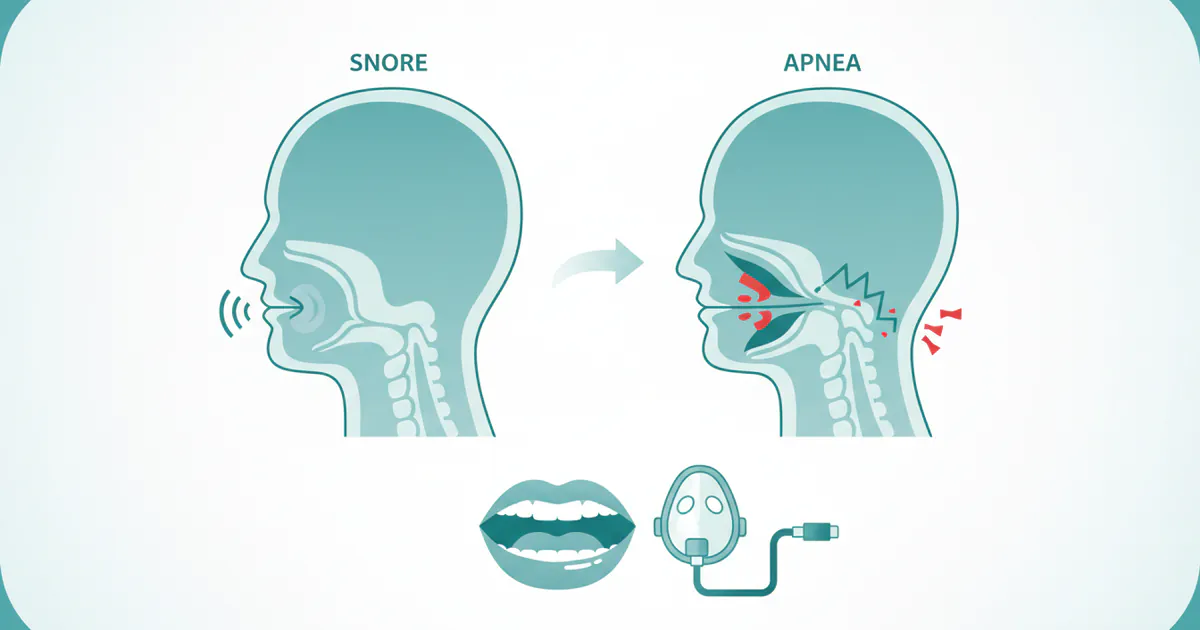
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026